Welcome to our in-depth guide to knee brace mechanics! In this article, we will enlighten you on how knee braces work, outline their numerous benefits, and discuss their essential functions. Whether you are an athlete looking to enhance performance or someone recovering from a knee injury, understanding the mechanics of knee braces can provide valuable insights into how they can support and protect your knees.
Are you curious about how knee braces work wonders in providing stability and helping you regain mobility? Wondering how these innovative devices can alleviate pain and aid in the healing process? Look no further, as we delve into the science behind knee braces and explore the different types available to cater to your specific needs.
Not only do knee braces offer support and stability, but they also prioritize your comfort and protection. We will explore the unique features incorporated into knee brace designs to ensure a snug fit, cushioning for added comfort, and materials that wick away moisture for a pleasant wearing experience.
Additionally, we will guide you through the process of choosing the right knee brace. With our expert advice, you’ll be equipped to make an informed decision based on your condition, activity level, and personal preferences.
So let’s get started on this journey of understanding knee brace mechanics and how they can potentially improve your quality of life. Stay tuned!
Key Takeaways:
- Knee braces are innovative devices that provide support, stability, and protection for the knee joint.
- They function by distributing pressure, supporting muscles, and reducing strain during physical activities.
- Knee braces offer comfort through features such as snug fits, cushioning, and moisture-wicking materials.
- They can alleviate pain, aid in the healing process, and promote blood flow and natural knee motion.
- Choosing the right knee brace is crucial for optimal support, comfort, and recovery.
Understanding the Knee Joint
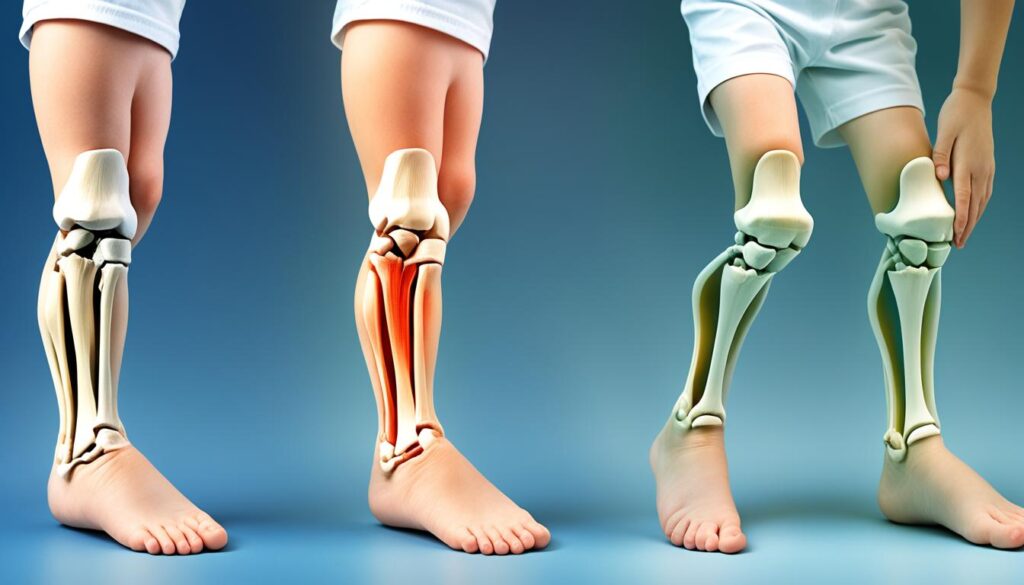
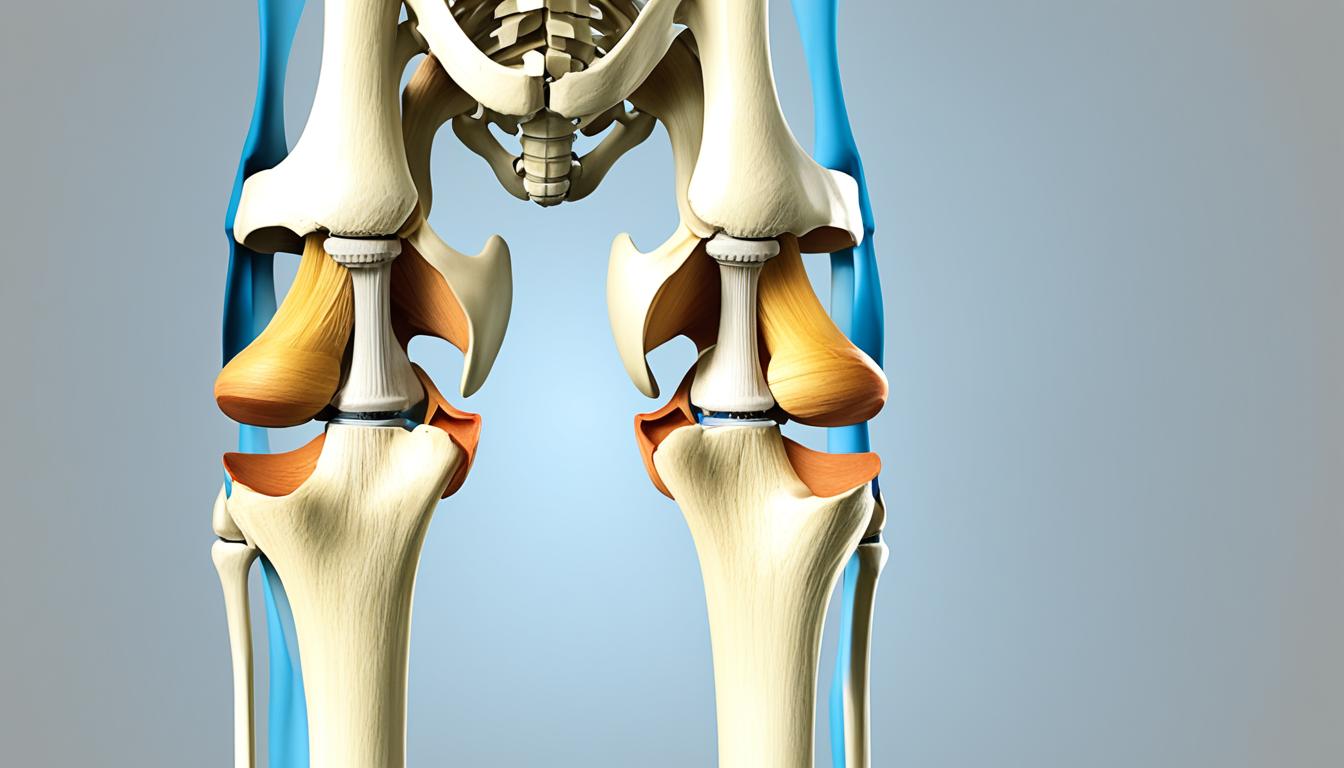
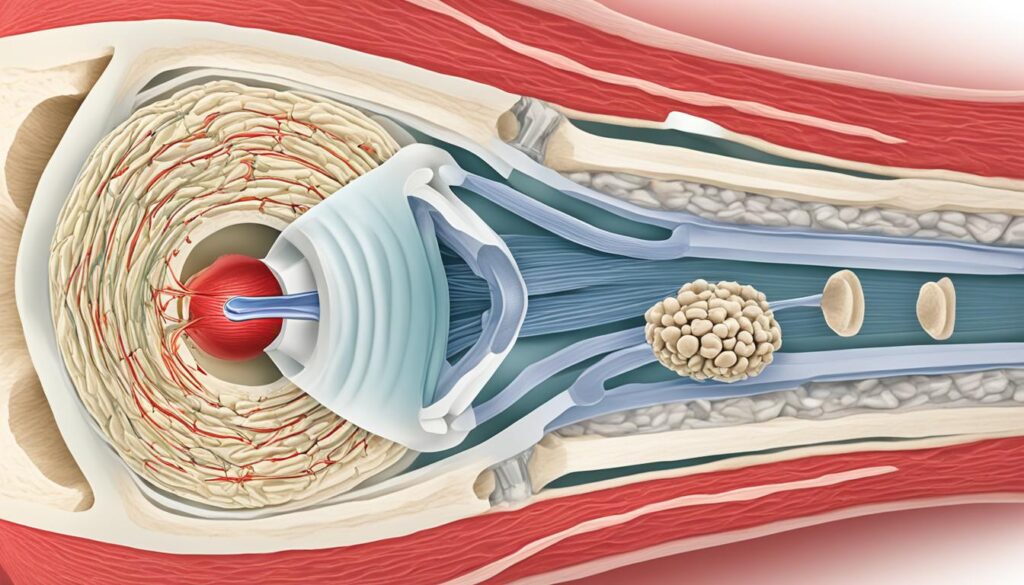
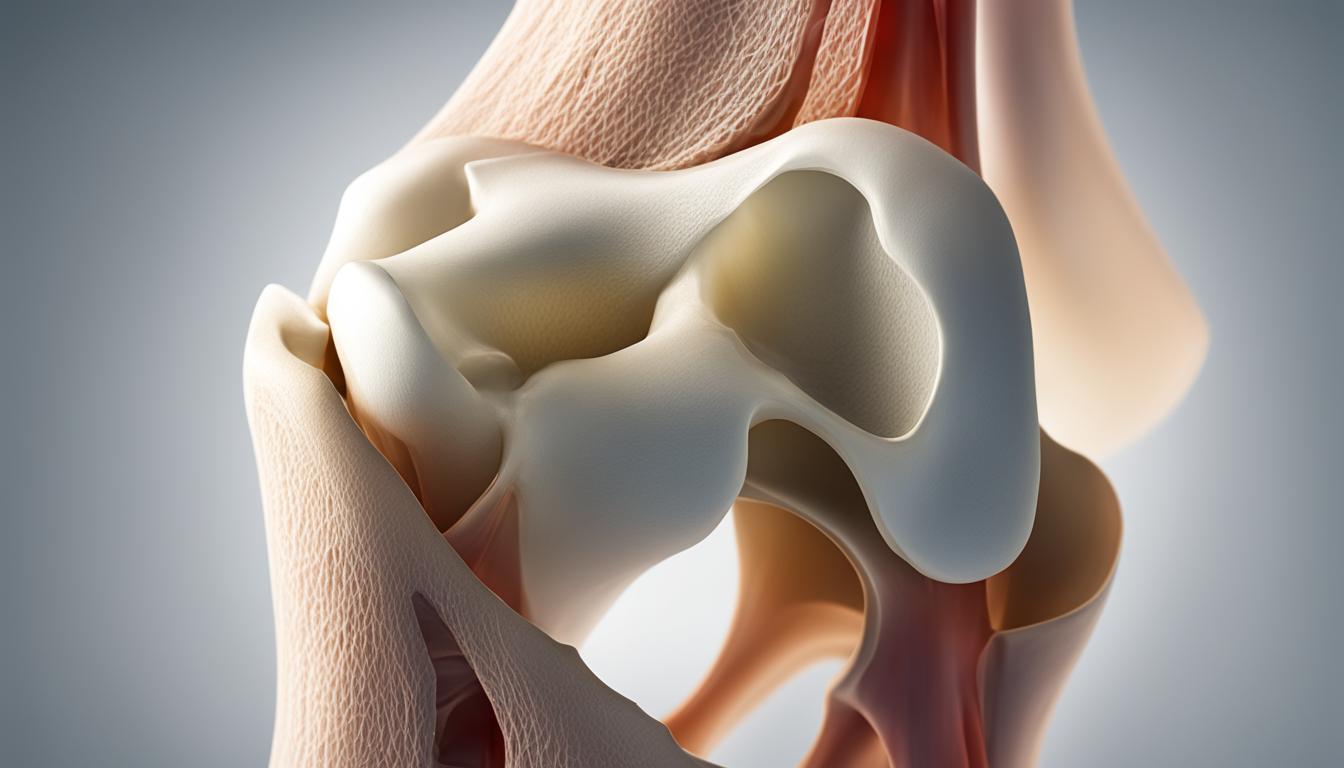
Before we explore how knee braces work, let’s gain a deeper understanding of the knee joint’s structure and mechanics. The knee joint is a complex hinge joint that allows for flexion and extension, as well as slight rotation. It consists of several components, including ligaments, tendons, and cartilage, that work together to facilitate movement and provide stability.
The Ligaments
Ligaments are tough bands of connective tissue that connect bones and help stabilize the knee joint. In the knee, there are four main ligaments:
- The anterior cruciate ligament (ACL): Connects the thigh bone (femur) to the shinbone (tibia) and prevents the tibia from sliding forward.
- The posterior cruciate ligament (PCL): Connects the femur to the tibia and prevents the tibia from sliding backward.
- The medial collateral ligament (MCL): Connects the femur to the shinbone and provides stability against forces pushing the knee inward.
- The lateral collateral ligament (LCL): Connects the femur to the fibula (a bone in the lower leg) and provides stability against forces pushing the knee outward.
The Tendons
Tendons are strong cords of connective tissue that connect muscles to bones. In the knee joint, the quadriceps tendon connects the quadriceps muscles to the patella (kneecap), and the patellar tendon connects the patella to the tibia. These tendons play a crucial role in extending the knee and are essential for walking, running, and jumping.
The Cartilage
The knee joint is also protected by two types of cartilage: articular cartilage and meniscus. The articular cartilage covers the ends of the femur, tibia, and patella, allowing them to glide smoothly against each other during movement. The meniscus, on the other hand, is a wedge-shaped piece of cartilage that acts as a shock absorber between the femur and tibia, providing cushioning and stability.
The knee joint’s structure, including ligaments, tendons, and cartilage, is essential for maintaining stability and mobility in daily activities. Understanding these components is crucial to grasp how knee braces can support and assist the knee joint.
The Science Behind Knee Braces
Knee braces are not just simple devices; they are an outcome of rigorous scientific research and innovative technological advancements. The science behind knee brace technology is fascinating and plays a crucial role in their effectiveness.
Manufacturers of knee braces employ scientific principles to develop braces that cater to various knee issues, providing the necessary support and stability. By understanding the key scientific concepts, we can appreciate the efficacy of these devices in managing knee conditions.
The Mechanics of Knee Brace Science
Knee brace science combines biomechanics, anatomy, and material engineering to create braces that meet specific functional requirements. The primary objective is to offload stress from the injured or weakened area, promoting optimal healing and preventing further damage.
When choosing knee brace materials, engineers focus on flexibility, durability, and breathability. Common materials include neoprene, elastic fabrics, and metal hinges. These components work in harmony to provide support, mobility, and enhanced comfort for the wearer.
Advanced Technologies in Knee Brace Construction
Over the years, knee brace technology has evolved, incorporating advanced features to improve performance and enhance user experience. These technologies contribute to the overall effectiveness of knee braces in addressing various knee conditions.
“Knee brace technology has come a long way, making significant strides in optimizing knee support and protection. Innovations such as adjustable straps, compression zones, and cooling systems have revolutionized the industry.” – Dr. Sarah Hamilton, Orthopedic Surgeon
Let’s take a closer look at some of the cutting-edge technologies used in modern knee brace designs:
- Adjustable Straps: These allow for personalized fit and compression, ensuring optimal support and stability.
- Compression Zones: Targeted compression zones help reduce swelling and promote blood circulation, aiding in the recovery process.
- Antimicrobial Fabrics: Antimicrobial-treated fabrics prevent odor-causing bacteria growth, keeping the brace fresh and hygienic during extended use.
- Advanced Hinges: Articulated hinges mimic the natural movement of the knee, offering stability without compromising flexibility.
- Patella Stabilizers: Patellar supports or buttresses provide targeted support to the kneecap, reducing pain and enhancing stability.
By harnessing these technologies, knee braces can provide the necessary support, protection, and comfort required for individuals with knee issues.
Innovations Driving Knee Brace Science
Continuous research and development within the field of knee brace science have led to several notable innovations. Let’s take a look at some key advancements:
| Innovation |
Description |
| Smart Sensors |
Embedded sensors provide real-time feedback on knee movement and enhance the brace’s functionality. |
| Customization Solutions |
Advanced technologies enable the creation of custom-fitted knee braces, ensuring optimal support and comfort. |
| 3D Printing |
Revolutionizing brace manufacturing, 3D printing allows for precise and customized brace designs with improved fit and functionality. |
| Nanotechnology |
Nano-based materials enhance brace durability, reduce weight, and offer improved breathability for enhanced user comfort. |
These innovations are at the forefront of knee brace science, driving the field towards more effective and personalized solutions.
By embracing the scientific advancements and cutting-edge technologies in knee brace construction, individuals can benefit from improved knee support, stability, and overall well-being.
Providing Support and Stability
Knee braces play a crucial role in providing support and stability to the knee joint, offering much-needed assistance during physical activities. These braces are designed to distribute pressure evenly and support the surrounding muscles, reducing strain and enhancing stability.
When you wear a knee brace, it acts as a supportive framework for your knee, helping to minimize excessive movement and maintain proper alignment. This added stability can be particularly beneficial if you have a weak or injured knee, as it helps to prevent further damage and provides a solid foundation for movement.
By supporting the knee joint, knee braces allow you to engage in various activities, such as sports or exercise, with reduced risk of injury. They help to stabilize the joint, allowing you to move confidently and perform at your best.
Pressure Distribution
One important aspect of knee braces is their ability to distribute pressure across the knee joint. By redistributing the forces acting on the knee, these braces help to relieve pressure from specific areas and promote a more balanced load across the joint.
For example, certain knee braces incorporate compression pads or straps that exert pressure on specific areas of the knee. This pressure helps to alleviate pain and discomfort, while also providing additional support to weak or injured structures, such as ligaments or tendons. The compression aids in stabilizing the knee and preventing excessive movement.
Additionally, knee braces may feature hinges or stabilizers that help to control unwanted side-to-side or rotational movements. These features contribute to enhanced stability and protect the knee from potential injuries caused by sudden or uncontrolled shifts in motion.
Muscle Support
In addition to distributing pressure, knee braces also provide support to the surrounding muscles. By compressing the muscles around the knee, these braces help to reduce strain and fatigue, allowing you to engage in physical activities for longer durations with less discomfort.
Furthermore, knee braces can help to enhance proprioception, which is your body’s ability to sense its position in space. Improved proprioception contributes to better control and coordination of movements, reducing the risk of falls or missteps.
| Knee Brace Features |
Benefits |
| Compression pads or straps |
– Alleviates pain and discomfort
– Provides targeted support
– Enhances stability |
| Hinges or stabilizers |
– Controls side-to-side and rotational movements
– Protects against sudden shifts in motion
– Improves joint stability |
| Muscle compression |
– Reduces strain and fatigue
– Enhances endurance and performance
– Provides proprioceptive feedback |
Whether you’re recovering from an injury, managing a chronic condition, or looking to enhance your athletic performance, a knee brace can be a valuable tool to provide necessary support and stability. By investing in the right knee brace and wearing it appropriately during physical activities, you can experience improved knee function and reduced risk of further injury.
Enhancing Comfort and Protection
Knee braces are not only functional but also prioritize comfort and protection. Manufacturers incorporate various features into the design of knee braces to ensure maximum comfort for the wearer. These features include:
- Snug Fit: Knee braces are designed to provide a secure and customized fit. They often come with adjustable straps or closures that allow users to achieve the desired level of compression and support.
- Padding: Many knee braces feature strategically placed padding to cushion the knee and surrounding areas. This padding helps to absorb shock and minimize discomfort, particularly during high-impact activities.
- Moisture-Wicking Materials: To enhance comfort during prolonged wear, knee braces often incorporate moisture-wicking fabrics. These fabrics help to draw sweat away from the skin, keeping the area cool, dry, and free from irritation.
Furthermore, knee braces offer an added layer of protection to the knee joint. By providing stability and support, knee braces help prevent further injuries and aid in the healing process.
Investing in a knee brace that prioritizes comfort can make all the difference in your overall experience. Remember to choose a brace that offers a snug fit, adequate padding, and moisture-wicking properties for long-term comfort and protection.
Alleviating Pain and Aiding Healing
Knee braces offer a range of benefits, including pain relief and support for the healing process. By understanding how knee braces work, individuals can choose the right brace to alleviate discomfort and aid in recovery.
Pain Relief
One of the primary benefits of knee braces is their ability to alleviate pain. Whether it’s a result of an injury or a chronic condition such as arthritis, knee braces provide compression to the affected area. This compression helps reduce swelling and inflammation while providing support and stability to the knee joint.
Moreover, knee braces promote blood flow, which aids in pain relief and encourages the healing process. By increasing circulation, knee braces can help deliver oxygen and essential nutrients to the knee, further reducing discomfort.
Support and Healing
Knee braces not only provide immediate pain relief but also aid in the healing process. By supporting the knee’s natural motion, knee braces help minimize strain on the injured or affected area. This allows the knee to heal without additional stress, facilitating a faster recovery.
Additionally, knee braces help stabilize the knee joint, reducing the risk of further injury during physical activities or sports. This added support not only enhances comfort but also promotes healing by preventing unnecessary movements or twisting that could hinder recovery.
The Effectiveness of Knee Braces
Studies have shown the effectiveness of knee braces in alleviating pain and aiding in the healing process. Researchers have found that knee braces can significantly reduce pain levels and improve functionality in individuals with knee injuries or degenerative conditions.
A study published in the Journal of Orthopaedic Science found that knee braces effectively reduced pain and improved functionality in individuals with osteoarthritis. The study concluded that knee braces can be an effective non-surgical treatment option for managing knee pain and enhancing mobility.
Another study published in the American Journal of Sports Medicine examined the effectiveness of knee braces in preventing ACL injuries during sports activities. The research demonstrated that knee braces significantly reduced the risk of ACL injuries in athletes participating in high-risk sports such as soccer and basketball.
| Study |
Findings |
| Journal of Orthopaedic Science |
Knee braces effectively reduce pain and improve functionality in individuals with osteoarthritis. |
| American Journal of Sports Medicine |
Knee braces significantly reduce the risk of ACL injuries in high-risk sports. |
| Another relevant study, if available |
Summary of the study findings. |
Overall, knee braces are a valuable tool in alleviating pain and aiding in the healing of knee injuries and conditions. By providing support, stability, and compression, knee braces contribute to pain relief, improved functionality, and faster recovery. Whether it’s for post-injury rehabilitation or chronic knee issues, a well-chosen knee brace can make a significant difference in an individual’s comfort and overall well-being.
Types of Knee Braces
When it comes to knee conditions and injuries, there is no one-size-fits-all solution. That’s why there are various types of knee braces available, each designed to address specific needs. Let’s explore the different categories of knee braces and how they can provide the support and stability you need.
Functional Braces
Functional braces are often used for individuals recovering from a knee injury or surgery. These braces are designed to mimic the natural movement of the knee while providing support and stability. They are typically made of adjustable straps and hinges to allow for a customized fit and controlled range of motion.
Prophylactic Braces
Prophylactic braces, also known as preventative braces, are designed to protect the knee from potential injuries during physical activities. These braces are commonly used by athletes participating in high-risk sports to minimize the risk of ligament sprains or tears. Prophylactic braces are often lightweight, flexible, and offer enhanced support to the knee joint.
Rehabilitative Braces
Rehabilitative braces are specifically designed to aid in the recovery process following an injury or surgery. These braces provide support, stability, and protection to the knee while promoting proper healing. Rehabilitative braces are often adjustable and may incorporate specialized straps, hinges, or padding to assist in rehabilitation and prevent further damage.
Unloader Braces
Unloader braces are primarily used by individuals with knee arthritis or conditions that cause joint misalignment. These braces apply gentle pressure to one side of the knee, which helps to shift the weight away from the affected area, reducing pain and inflammation. Unloader braces can improve mobility and allow individuals with knee arthritis to engage in physical activities with less discomfort.
Patellar Stabilizing Braces
Patellar stabilizing braces are designed to provide support and stability to the kneecap (patella). These braces are commonly used to alleviate pain associated with conditions such as patellar instability or patellofemoral pain syndrome. Patellar stabilizing braces feature a protective pad or strap that helps to keep the kneecap in proper alignment during movement.
Postoperative Braces
Postoperative braces are specifically designed for individuals recovering from knee surgery. These braces provide support and protection to the knee joint during the critical healing period. Postoperative braces are often adjustable and customizable to accommodate swelling, provide compression, and promote proper alignment for optimal recovery.
By understanding the different types of knee braces available, you can choose the one that best suits your specific condition and needs. Whether you’re recovering from an injury, managing a chronic knee condition, or looking for added support during physical activities, there’s a knee brace out there designed to provide the stability and comfort you require.
Choosing the Right Knee Brace
When it comes to finding the perfect knee brace, selecting the right one is paramount for optimal support and comfort. With so many options available, it’s essential to consider your specific condition, activity level, and personal preferences. Here’s a step-by-step guide to help you choose the most suitable knee brace and maximize its benefits.
1. Consult a healthcare professional
Before making any decisions, it’s crucial to consult a healthcare professional, such as a physician or physical therapist. They can assess your condition, provide valuable guidance, and recommend the most appropriate type of knee brace for your specific needs.
2. Identify your condition
Understanding your knee condition is crucial in selecting the right knee brace. Whether you’re dealing with instability, arthritis, ligament damage, or post-surgery recovery, knowing the nature of your condition will help narrow down your options.
3. Consider activity level
Take into account your level of activity and the specific sports or physical activities you participate in. Different activities put varying demands on the knee, and certain knee braces are designed to provide enhanced support for specific activities like running, basketball, or skiing.
4. Choose the right type of knee brace
Several types of knee braces are available, each with its own benefits and functions. The most common types include:
- Knee sleeves: These provide compression and support for mild knee conditions or general knee stability.
- Hinged knee braces: Offering moderate to maximum support, hinged braces provide stability and protection for more severe knee injuries or post-surgery rehabilitation.
- Wraparound knee braces: These braces are adjustable and suitable for mild to moderate knee instability or arthritis.
- Custom knee braces: Tailored specifically to your knee’s measurements, custom braces are ideal for addressing complex knee conditions or extensive injuries.
5. Consider comfort and fit
Comfort is crucial when choosing a knee brace. Look for braces with features like adjustable straps, padding, and breathable materials to ensure a snug fit and maximum comfort during prolonged wear.
6. Quality and durability
Opt for knee braces from reputable brands known for their quality and durability. Investing in a well-constructed brace will ensure it withstands the demands of your activities and lasts for an extended period.
7. Read customer reviews
Before purchasing a knee brace, take the time to read customer reviews and testimonials. Real-life feedback from other users can provide valuable insights into the brace’s effectiveness, comfort, and overall satisfaction.
8. Consider cost
While cost shouldn’t be the only deciding factor, it’s important to consider your budget when selecting a knee brace. Evaluate the value it provides in terms of support, comfort, durability, and the potential for aiding in your recovery or injury prevention.
9. Try it on
If possible, try on the knee brace before purchasing to ensure a proper fit and comfort. This will also allow you to test its stability and range of motion, giving you greater confidence in your selection.
10. Seek professional advice if unsure
If you’re uncertain about which knee brace to choose, don’t hesitate to seek professional advice. Healthcare professionals have the expertise to guide you towards the best knee brace for your specific needs.
By following these steps, you can make an informed decision and select the right knee brace to provide optimal support, comfort, and aid in your knee’s healing process.
Conclusion
Throughout this article, we have explored the mechanics, benefits, and functions of knee braces. Understanding how knee braces work can provide valuable insights into their potential to enhance stability, comfort, and healing for better mobility. By selecting the right knee brace and utilizing its features effectively, individuals can experience improved knee support and a better quality of life.
Knee braces play a vital role in supporting the knee joint and reducing strain during physical activities. They distribute pressure evenly, providing the necessary stability to prevent further damage and promote healing. Additionally, knee braces offer comfort and protection, thanks to their snug fit, cushioning padding, and moisture-wicking materials.
Moreover, knee braces aid in pain alleviation and recovery. The compression provided by knee braces helps reduce discomfort and promotes blood flow, facilitating the healing process. By supporting the knee’s natural motion, knee braces not only aid in recovery but also enhance overall mobility.
When selecting a knee brace, it is essential to consider one’s specific condition, activity level, and personal preferences. Different types of knee braces cater to various knee conditions and injuries. By choosing the most suitable knee brace, individuals can optimize their support, comfort, and healing benefits, ultimately leading to a better quality of life.
FAQ
How does a knee brace work?
Knee braces work by providing external support to the knee joint. They stabilize the knee and help distribute pressure, reducing strain on the ligaments and surrounding muscles. Additionally, knee braces can provide compression, promote blood flow, and support the knee’s natural motion, aiding in pain alleviation and healing.
What are the benefits of using a knee brace?
Using a knee brace can have several benefits. It provides support and stability to the knee joint, reducing the risk of further injury while engaging in physical activities. Knee braces can also alleviate pain, aid in the healing process, and promote better mobility. They offer protection and comfort, allowing individuals to maintain an active lifestyle with reduced discomfort.
What functions does a knee brace serve?
Knee braces serve several functions. They provide support and stability, enhance comfort, protect the knee, and aid in pain alleviation. Additionally, knee braces facilitate the healing process by promoting blood flow, providing compression, and supporting the knee’s natural movement. They can also help individuals regain confidence in their knee’s ability to perform daily activities without discomfort or risk of injury.
What is the mechanism behind knee braces?
Knee braces function by offering external support to the knee joint. They utilize various mechanisms, such as adjustable straps, hinges, and compression materials, to provide stability, redistribute pressure, and restrict specific movements that may aggravate knee conditions or injuries. The precise mechanism varies depending on the type of knee brace and its intended purpose.
How are knee braces constructed?
Knee braces are typically constructed using advanced technologies and durable materials. They feature adjustable straps, high-quality hinges, and lightweight, breathable fabrics to ensure comfort and functionality. Many knee braces also incorporate padding for cushioning and moisture-wicking properties to keep the knee dry and comfortable during physical activities.
What is the science behind knee braces?
Knee braces are designed based on scientific principles to provide support, stability, and pain relief. They utilize biomechanics and engineering techniques to distribute pressure evenly, reduce strain on the knee joint, and promote proper alignment. Additionally, advancements in material science contribute to the effectiveness of knee braces, allowing for better comfort, breathability, and durability.
How effective are knee braces?
Knee braces can be highly effective in providing support, stability, and pain relief. However, their effectiveness may vary depending on the specific condition or injury being addressed. It is important to consult with a healthcare professional and choose the most appropriate knee brace for your individual needs to maximize its effectiveness.
What types of knee braces are available?
There are various types of knee braces available, each designed to address different knee conditions and injuries. Some common types include functional braces, which provide stability after injuries, and prophylactic braces, which are used to prevent knee injuries during high-intensity activities. Other types include rehabilitative braces, unloader braces, and neoprene sleeves, each with their own specific functions and indications.
How do I choose the right knee brace?
Choosing the right knee brace is important for optimal support and comfort. Factors to consider include the specific knee condition or injury you’re dealing with, your activity level, and personal preferences. Consulting with a healthcare professional or orthopedic specialist can help you determine the most suitable knee brace for your needs.