Do you know how many people walk around with a torn meniscus without knowing they have a tear?
💥About 5% of young people and up to 67% of older people have asymptomatic (non-painful) meniscus tears! 💥
How is that possible?
Depending on the type of injury and how it is treated, the symptoms of a meniscus tear may resolve within days to weeks or months; and you may not even know the tear exists!
The initial injury may not even have been severe enough to warrant a visit to an orthopedist or ordering an X-ray or MRI, especially if the knee only hurt for a few days before the pain went away.
Here’s what you need to know about meniscus injuries so they don’t hinder your favorite activities…
Where is the meniscus?
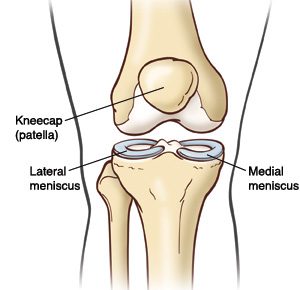
The meniscus is a “C”-shaped disk made of cartilage that is located in the knee, between the shin bone and the femur. It sits on the weight-bearing surface of the tibia, or tibia, in the joint capsule.
There are two menisci, one on the lateral (outside) of the knee and one on the medial (inside). A healthy meniscus provides space, cushion and lubrication to the joint so that the knee can bend, straighten and bear weight comfortably.
The meniscus is located deep in the knee, along with the anterior cruciate ligament (ACL) and the posterior cruciate ligament (PCL). Due to their deep location, the menisci do not have a very good blood supply, so certain areas are not likely to heal from an injury.
💥 🤯 However, the fact that the meniscus does not heal properly on its own does not mean that a tear always needs to be repaired!
What does the meniscus do and why is it so important?
Shock absorption: The meniscus acts as a shock absorber for shocks that occur during daily activities, such as walking, running, jumping and sports. As we move, force travels through the foot and through the shin bone to the knee, where the meniscus absorbs and disperses that force through the knee, so the impact is spread out and not concentrated in one area.
Stability: The meniscus also acts as a wedge that supports the front and back of your knee, keeping the knee from going beyond a certain range of motion, such as hyperextension, which puts you at risk for other injuries.
How does the meniscus become injured?
The meniscus is most commonly injured during twisting of the knee when the foot is planted on the ground. Rotational stress or “shearing” can cause the femur and tibia to rotate beyond what the meniscus can handle, resulting in a tear in the cartilage.
Meniscal tears are common in athletes who exert a large amount of force on one leg and twist their body in a different direction, such as football 🏈, soccer ⚽️, lacrosse 🥍, tennis 🎾, or basketball 🏀. Field and field athletes often put their feet down to stop and change direction; and in a split second the knee rotates with enough force to cause a meniscus tear.
Snow sports, such as skiing ⛷ and snowboarding 🏂, also carry a high risk of meniscus injuries. The edge of a ski or board can unexpectedly hit the snow, causing a sudden rotation of the leg. The long lever arm can quickly generate a high-speed rotational force, strong enough to cause meniscus injury.
Meniscal tears occur in people of all ages, including athletes and non-athletes. In middle-aged and older adults, meniscus tears can occur due to wear and tear on the knee joint. As the body ages, degeneration of the cartilage tissue occurs as the joints are exposed to force for years.
Osteoarthritis, a condition in which cartilage wears away over time, is common in older adults and is often accompanied by a torn meniscus. A meniscus tear earlier in life can also make the knee more susceptible to earlier-onset osteoarthritis. That’s why it’s so important to learn the right moves and exercises to protect your knees!
I have a meniscus tear. What now?
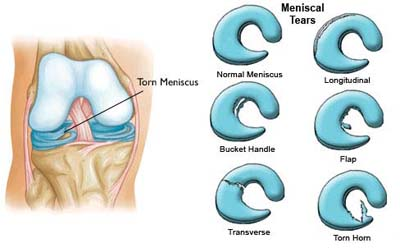
Depending on the type of meniscus tear, you may experience symptoms such as pain, swelling, locking, or locking of the knee. Although a meniscal injury cannot be detected on X-rays, it can be diagnosed through a careful examination or an MRI.
Most meniscal tears are initially treated conservatively (without surgery); although an orthopedic doctor may recommend surgery if symptoms persist and daily activities are limited.
Meniscectomy: The most common surgery for a meniscus tear is called a menisectomy, in which the surgeon removes the torn piece of cartilage and cleans up the surrounding ragged tissue. Although it is a surgical procedure, recovery after a meniscectomy is relatively short. Most people can resume daily activities within a few weeks and exercise within a few months.
It is important to add that everyone responds to surgery differently; and a ‘minor’ surgery for one person may be a more stressful experience and longer rehabilitation for someone else.
Meniscus repair: An alternative surgery is a meniscus repair, which is performed when the orthopedic surgeon believes the torn cartilage structure can be sewn together, saving cartilage to prevent osteoarthritis in the future. This procedure is typically performed more in younger people to preserve the cartilage rather than remove it. Recovery from a meniscus repair takes longer than a menisectomy and involves close monitoring of range of motion, weight bearing, and activity progression during rehabilitation.
Non-surgical treatment A meniscus tear is very common and results in great results in most cases! A diagnosis of a meniscus tear does NOT mean that surgery is always necessary!
Although a meniscus tear will not heal itself, you can strengthen the knee and improve movement patterns to disperse forces and reduce stress at the site of the tear, which will help resolve symptoms.
💪 With the right exercises and learning to move properly, most meniscus tears can be treated conservatively WITHOUT surgical intervention.
💥It’s important to remember that you are not your MRI result; and a meniscus tear should not determine the rest of your life.
How can you treat a meniscus injury without surgery?
A meniscus injury must be properly guided through the healing phases. Pain and inflammation are likely to be early symptoms, while stiffness and weakness may be the main complaints after a few weeks. Dealing with injuries with “PEACE & LOVE” is a good reference for dealing with acute injuries.
To return to normal activities, follow the guidance of your physical therapist, who will develop a care plan for strengthening, balance training, improving mobility, and returning to exercise.
👉Doing the right exercises with good form and consistency will significantly increase your ability to recover from a meniscus tear and prevent future injuries.
If you’re ready to start strengthening at home, ACL Strong has courses that include all the necessary components of exercise and movement to train your body and brain to protect your knees now and for the long term.
Whether you have a torn meniscus or not, doing the right exercises the right way will keep your knees strong and stable, so you’ll be less prone to further injury and better equipped to maintain an active lifestyle for as long as you want. to lead!
You can LIVE with a torn meniscus….
And you can also PREVENT them!