Are athletes destined to suffer from knee pain due to quadriceps tendon injury? Recent studies suggest that there is hope for effective management and recovery.
Eccentric loading has emerged as a key rehabilitation strategy for treating quads tendinopathy. This approach has shown promise in reducing pain and improving function in individuals affected by this condition.
Understanding how to effectively utilize eccentric loading is crucial for athletes and healthcare professionals seeking to address quadriceps tendinopathy.
Key Takeaways
- Effective management of quadriceps tendinopathy is possible with the right rehabilitation strategies.
- Eccentric loading is a key approach in treating quads tendinopathy.
- Proper understanding and application of eccentric loading can significantly improve outcomes.
- Athletes and healthcare professionals can benefit from learning about quads tendinopathy treatment options.
- Reducing pain and improving function are primary goals in managing quadriceps tendon injury.
Understanding Quadriceps Tendinopathy
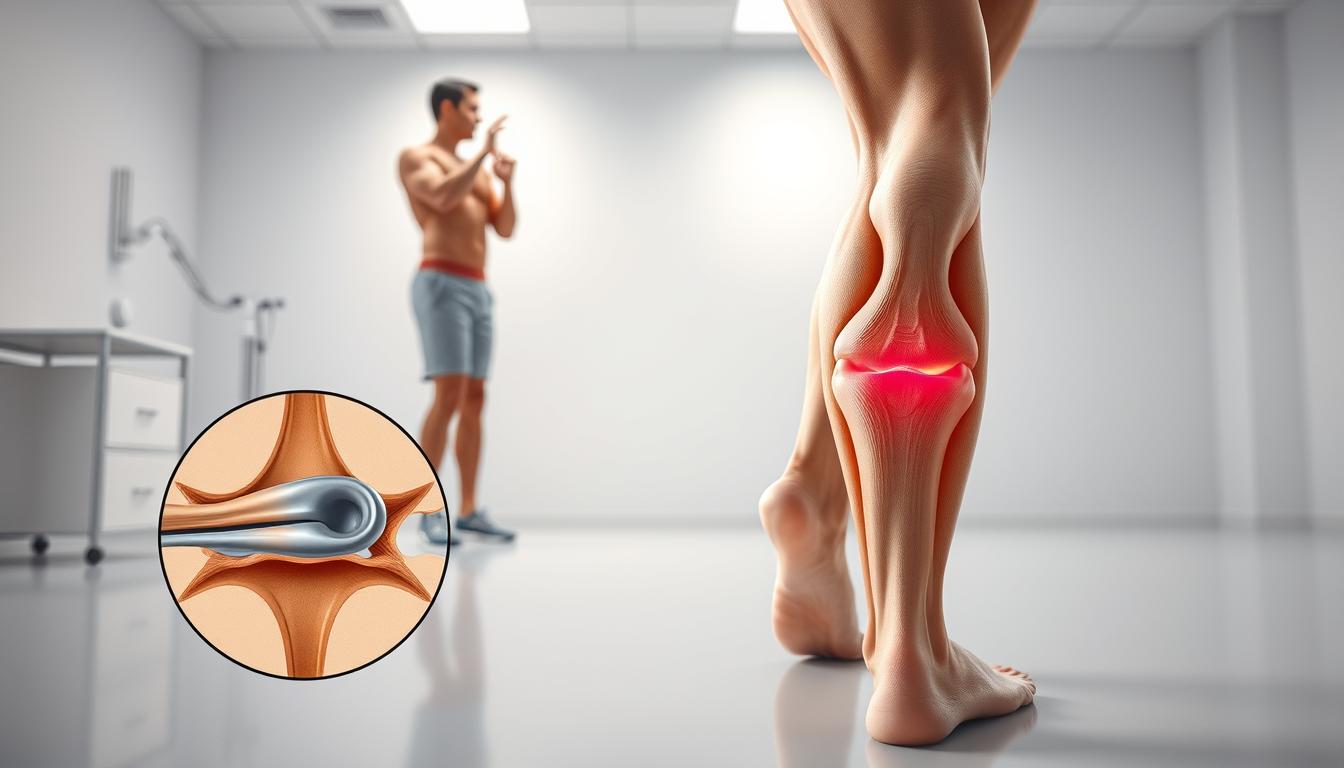
Quadriceps tendinopathy, a common issue among athletes, involves the degeneration and inflammation of the quadriceps tendon. This condition is associated with overuse and is prevalent in sports that involve running and jumping. Understanding its implications is crucial for effective management and treatment.
What is Quadriceps Tendinopathy?
Quadriceps tendinopathy refers to the inflammation and degeneration of the quadriceps tendon, which connects the quadriceps muscles to the kneecap. This condition can significantly impact an individual’s athletic performance and daily activities due to the pain and tenderness it causes.
Causes of Quadriceps Tendinopathy
The primary cause of quadriceps tendinopathy is repetitive strain on the quadriceps tendon, often resulting from overuse in sports or activities that involve frequent jumping and running. Poor training practices, inadequate warm-up routines, and insufficient recovery time can also contribute to the development of this condition.
Symptoms to Watch For
Individuals with quadriceps tendinopathy typically experience pain and tenderness in the knee area, particularly just above the kneecap. The pain can be exacerbated by activities that strain the quadriceps tendon, such as squatting, jumping, or climbing stairs. Early recognition of these symptoms is crucial for timely intervention and effective quads tendinopathy treatment.
The Role of Eccentric Loading
Eccentric loading has emerged as a pivotal rehabilitation technique for addressing quadriceps tendinopathy. This method involves the lengthening of muscles under load, which is particularly beneficial for tendon rehabilitation.
Eccentric loading is characterized by the slow and controlled lengthening of the muscle-tendon unit. This technique is crucial for promoting tendon healing and strength, as supported by various studies, including those found on PubMed Central.
What is Eccentric Loading?
Eccentric loading refers to the process where the quadriceps muscle is subjected to a controlled lengthening under load. This is typically achieved through exercises that involve the slow lowering of the body or a weight, thereby engaging the quadriceps eccentrically.
The eccentric contractions for quad tendinopathy are particularly beneficial as they help in promoting collagen synthesis and improving tendon strength. This is a critical aspect of rehabilitation, as enhanced tendon strength directly correlates with improved functional outcomes and reduced risk of re-injury.
Benefits of Eccentric Loading in Rehabilitation
The benefits of incorporating eccentric strength training for quads into a rehabilitation program are multifaceted. Firstly, it aids in the recovery from quadriceps tendinopathy by enhancing tendon strength and promoting healing.
- Promotes collagen synthesis, thereby aiding in tendon repair.
- Improves tendon strength, reducing the risk of re-injury.
- Enhances functional outcomes by improving muscle-tendon unit function.
By understanding and applying the principles of eccentric loading, individuals suffering from quadriceps tendinopathy can significantly benefit from a well-structured rehabilitation program. This approach not only addresses the symptoms but also targets the underlying causes, leading to a more sustainable recovery.
Initial Treatment Strategies
The first line of defense against quadriceps tendinopathy involves a combination of rest, ice, and pain management. These initial treatment strategies are crucial for reducing pain and inflammation, thereby facilitating the rehabilitation process.
Rest and Ice Application
Rest is essential in the acute phase of quadriceps tendinopathy to prevent further injury. Avoiding activities that aggravate the condition allows the tendon to begin the healing process. Ice application is another critical component, helping to reduce inflammation and pain. Applying ice for 15-20 minutes, several times a day, can significantly alleviate symptoms.
Importance of Pain Management
Effective pain management is vital for ensuring that patients can participate in rehabilitation exercises without undue discomfort. This can involve the use of over-the-counter pain relievers or, in some cases, more advanced pain management strategies under the guidance of a healthcare professional. Pain management is not just about alleviating symptoms; it’s about creating a foundation for successful rehabilitation.
By focusing on rest, ice application, and pain management, individuals with quadriceps tendinopathy can effectively manage their symptoms and progress towards a more comprehensive rehabilitation program, including eccentric loading exercises.
Eccentric Loading Exercises
For individuals suffering from quadriceps tendinopathy, incorporating eccentric loading exercises into their rehabilitation program can be highly beneficial. Eccentric loading is a form of exercise where the muscle lengthens under load, which is particularly effective for strengthening tendons and promoting healing.
Recommended Eccentric Exercises for Quadriceps
Several eccentric exercises are recommended for quadriceps tendinopathy, with one of the most effective being the single-leg decline squat. This exercise specifically targets the quadriceps tendon, promoting strength and resilience.
To perform the single-leg decline squat, start by standing on a decline surface (such as a slant board or a wedge) with one leg. Slowly lower your body down, keeping your back straight and your core engaged, and then return to the starting position with the help of your other leg or a support.

How to Perform Eccentric Exercises Correctly
Performing eccentric exercises correctly is crucial to avoid further injury and ensure the effectiveness of the rehabilitation program. It’s essential to start with lower loads and gradually increase the intensity as your tendon becomes more resilient.
Proper technique involves slow and controlled movements during the lowering phase, avoiding any jerky or bouncy actions. For example, when performing the decline squat, take 3-5 seconds to lower your body down.
“Eccentric exercises, when performed correctly, can significantly reduce pain and improve function in patients with quadriceps tendinopathy.”
It’s also important to be consistent with your exercises, typically performing them 2-3 times a day, and to monitor your progress, adjusting the intensity and volume as needed.
Creating a Rehabilitation Program
Creating a personalized rehabilitation plan is essential for effective quadriceps tendon rehabilitation. A tailored program considers the individual’s specific condition, goals, and progress over time.
Eccentric strength training for quads is a critical component of this rehabilitation. It involves exercises that are designed to strengthen the quadriceps tendon and surrounding muscles.
Setting Realistic Goals
Setting realistic goals is a fundamental aspect of a successful rehabilitation program. Goals should be specific, measurable, achievable, relevant, and time-bound (SMART). For example, a goal might be to return to running within 12 weeks.
Examples of Realistic Goals:
- Reducing pain during daily activities within 6 weeks
- Increasing quadriceps strength by 20% within 8 weeks
- Returning to sports-specific activities within 12 weeks
Monitoring Progress Over Time
Regular monitoring of progress is crucial to adjust the rehabilitation program as needed. This involves tracking pain levels, strength improvements, and functional abilities.
Progress Monitoring Techniques:
| Technique | Description | Frequency |
|---|---|---|
| Pain Assessment | Using a pain scale to rate discomfort | Weekly |
| Strength Testing | Measuring quadriceps strength using dynamometry | Bi-Weekly |
| Functional Tests | Evaluating ability to perform daily and sports-specific activities | Monthly |
By setting realistic goals and continuously monitoring progress, individuals can optimize their rehabilitation outcomes. This structured approach ensures that the rehabilitation program remains effective and relevant to the individual’s changing needs.
The Importance of Professional Guidance
Professional guidance is the cornerstone of a successful recovery from quadriceps tendinopathy. Managing quadriceps tendon pain effectively requires a comprehensive approach that includes proper diagnosis, treatment planning, and rehabilitation. Seeking help from healthcare professionals is crucial in this process.
Quadriceps tendinopathy is a condition that can significantly impact one’s quality of life, especially for athletes or individuals with active lifestyles. The condition involves inflammation and degeneration of the quadriceps tendon, leading to pain and reduced functionality. Early intervention by professionals can prevent further deterioration and facilitate a more effective recovery.
When to See a Physical Therapist?
Knowing when to seek professional help is vital. If you’re experiencing persistent pain or if your symptoms are not improving with basic care, it’s time to consult a physical therapist. They can provide a detailed assessment and create a personalized rehabilitation plan. Physical therapists are trained to manage conditions like quadriceps tendinopathy, helping patients through exercises and manual therapy tailored to their specific needs.
As
“The role of physical therapists in rehabilitation is not just about alleviating pain but also about restoring function and preventing future injuries.”
This holistic approach ensures that patients receive comprehensive care, addressing not just the symptoms but the underlying causes.
Working with Athletic Trainers
Athletic trainers play a significant role in the rehabilitation process, especially for athletes. They are equipped to design and implement rehabilitation programs that are specific to the individual’s sport or activity. Working with an athletic trainer can help ensure that the recovery is tailored to the patient’s specific needs, enhancing the effectiveness of the rehabilitation.
Moreover, athletic trainers can provide valuable insights into preventing recurrence, helping individuals understand how to modify their activities to avoid putting excessive strain on their quadriceps tendon. This guidance is invaluable in managing quadriceps tendon pain and preventing future episodes of tendinopathy.
Lifestyle Modifications for Recovery
Recovering from quadriceps tendinopathy requires more than just exercises; it demands a comprehensive lifestyle adjustment. Lifestyle modifications play a crucial role in enhancing the recovery process and preventing future occurrences.
Nutrition’s Role in Healing
Adequate nutrition is vital for tendon health and recovery. A balanced diet rich in proteins, vitamins, and minerals supports the healing process. Foods high in omega-3 fatty acids, such as salmon, and those rich in antioxidants, like berries, can help reduce inflammation and promote healing.
- Incorporate lean proteins like chicken and turkey to support muscle repair.
- Consume foods rich in vitamin C, such as citrus fruits and leafy greens, to enhance collagen synthesis.
- Include whole grains like brown rice and quinoa for complex carbohydrates.
For more information on exercises that complement nutritional healing, visit our page on effective exercises for patellar tendonitis treatment, which shares valuable insights into rehabilitation exercises that can be adapted for quadriceps tendinopathy.
Importance of Hydration
Proper hydration is equally crucial for tendon health. Adequate fluid intake helps maintain tendon elasticity and facilitates the repair process. It’s recommended to drink plenty of water throughout the day, especially before, during, and after exercise.
- Drink at least 8-10 glasses of water per day.
- Avoid sugary drinks that can lead to inflammation.
- Monitor urine color to ensure it’s pale yellow, indicating proper hydration.
By combining a balanced diet with proper hydration, individuals can significantly enhance their recovery from quadriceps tendinopathy and improve overall athletic performance.
Preventing Recurrence of Tendinopathy
Eccentric strength training for quads plays a significant role in preventing the recurrence of quadriceps tendinopathy. By incorporating specific exercises and training modifications into your rehabilitation program, you can significantly reduce the risk of re-injury.
Stretching and Warm-Up Techniques
Proper warm-up and stretching exercises are crucial before engaging in any physical activity. This not only prepares the muscles for the upcoming exertion but also enhances flexibility and reduces the risk of strain. Dynamic stretching, which involves moving your joints through a range of motion while keeping your muscles active, is particularly effective.
Examples of dynamic stretches for the quadriceps include leg swings and lunges. Incorporating these into your warm-up routine can help prevent tendinopathy by improving muscle elasticity and reducing stiffness.

Strengthening Surrounding Muscles
Strengthening the muscles around the knee, particularly the hamstrings, is vital for providing stability and support to the quadriceps tendon. A balanced strength between the quadriceps and hamstrings can help prevent overuse and strain on the tendon.
The following table outlines a simple strengthening program for the hamstrings:
| Exercise | Sets | Repetitions |
|---|---|---|
| Hamstring Curls | 3 | 12-15 |
| Deadlifts | 3 | 8-10 |
| Lunges | 3 | 10-12 per leg |
By integrating these exercises into your rehabilitation program, you can enhance the stability of your knee and reduce the risk of quadriceps tendinopathy recurrence.
Advanced Therapies for Chronic Cases
When conventional treatments fail, advanced therapies can be a viable solution for managing quadriceps tendinopathy. These innovative treatments aim to stimulate healing and reduce pain in chronic cases.
Shockwave Therapy
Shockwave therapy is a non-invasive treatment that uses high-energy shockwaves to stimulate the healing process in tendons. This therapy is particularly beneficial for chronic tendinopathy as it promotes blood flow and tissue repair.
- Stimulates Healing: Enhances the body’s natural healing processes.
- Reduces Pain: Helps in alleviating chronic pain associated with tendinopathy.
- Non-Invasive: Offers a treatment option without the need for surgery.
Platelet-Rich Plasma (PRP) Injections
PRP injections involve using the patient’s own platelet-rich plasma, derived from their blood, to promote tendon healing. This treatment is considered effective for chronic quadriceps tendinopathy.
- Promotes Tissue Repair: PRP contains growth factors that aid in tendon repair.
- Minimally Invasive: Involves injections, which are less invasive than surgical procedures.
- Potential for Pain Relief: Can lead to significant reduction in pain.
Both shockwave therapy and PRP injections represent advanced therapeutic options for managing chronic quadriceps tendinopathy. These treatments can be particularly beneficial for individuals who have not responded to conventional therapies.
Patient Success Stories
Quadriceps tendinopathy rehabilitation through eccentric loading has inspired numerous success stories. Athletes and individuals who were once sidelined by this condition have made remarkable recoveries, returning to their activities with renewed strength and confidence.
Real-Life Experiences with Eccentric Loading
Eccentric loading exercises have been a cornerstone in the rehabilitation of quadriceps tendinopathy for many. The slow and controlled movements involved in eccentric exercises help in strengthening the tendon, promoting healing, and reducing pain. One athlete, a competitive runner, shared her experience of using eccentric loading to overcome quadriceps tendinopathy. She noted significant improvements in her condition after consistently performing eccentric squats and leg press exercises.
Another individual, a recreational basketball player, reported that after six weeks of eccentric loading exercises, he was able to return to his sport without experiencing the debilitating pain that once held him back. These stories underscore the potential of eccentric loading as a effective rehabilitation strategy.
Lessons Learned from Recovery
The journey to recovery from quadriceps tendinopathy through eccentric loading teaches valuable lessons. Patience and consistency are key, as the rehabilitation process can be lengthy. Additionally, the importance of proper technique cannot be overstated, as incorrect form can lead to further injury.
A common theme among success stories is the role of professional guidance. Working with physical therapists or athletic trainers not only ensures that exercises are performed correctly but also provides motivation and support throughout the rehabilitation process.
| Key Factors | Importance | Benefits |
|---|---|---|
| Patience and Consistency | High | Ensures complete rehabilitation |
| Proper Technique | Critical | Prevents further injury |
| Professional Guidance | Essential | Provides motivation and corrects form |
Conclusion: Embracing Eccentric Loading
Eccentric loading has emerged as a highly effective strategy for managing quadriceps tendinopathy, a common issue among athletes. By incorporating eccentric exercises for quad tendonitis into a rehabilitation program, individuals can significantly improve their recovery outcomes.
Key Principles for Effective Recovery
Effective management of quadriceps tendinopathy involves understanding the condition, applying eccentric exercises correctly, and making necessary lifestyle adjustments. Quadriceps tendinopathy recovery exercises should be tailored to the individual’s needs, with a focus on progressive overload and pain management.
Long-Term Health Benefits
Embracing eccentric loading and associated lifestyle modifications can lead to a healthier, more sustainable athletic career. By adopting these practices, athletes can not only recover from quadriceps tendinopathy but also reduce the risk of recurrence, ensuring long-term participation in their chosen sports.
FAQ
What is quadriceps tendinopathy?
Quadriceps tendinopathy refers to the inflammation and degeneration of the quadriceps tendon, often resulting from overuse. It is a common issue among athletes, characterized by pain and dysfunction in the quadriceps tendon.
How does eccentric loading help in managing quadriceps tendinopathy?
Eccentric loading involves the lengthening of muscles under load, which is particularly beneficial for tendon rehabilitation. It helps in promoting collagen synthesis and improving tendon strength, thereby aiding in the recovery from quadriceps tendinopathy.
What are some effective eccentric exercises for quadriceps tendinopathy?
Eccentric exercises, such as the single-leg decline squat, are highly effective for quadriceps tendinopathy. Proper technique is essential to avoid further injury and ensure the tendon is subjected to the appropriate stress for healing.
What is the role of nutrition in the recovery from quadriceps tendinopathy?
Adequate nutrition and hydration are vital for tendon health and recovery. A balanced diet rich in proteins, vitamins, and minerals, along with proper hydration, supports the healing process and overall athletic performance.
How can recurrence of quadriceps tendinopathy be prevented?
Preventing the recurrence of quadriceps tendinopathy involves incorporating stretching and warm-up routines into training. Strengthening the surrounding muscles, such as the hamstrings, also plays a crucial role in providing stability and reducing the risk of re-injury.
What are some advanced therapies for chronic quadriceps tendinopathy?
For cases of quadriceps tendinopathy that are resistant to initial treatments, advanced therapies such as shockwave therapy and PRP injections may be considered. These treatments aim to stimulate healing and reduce pain in chronic tendinopathy.
How can a rehabilitation program be structured for effective recovery?
A well-structured rehabilitation program is key to successful recovery. This involves setting realistic goals, such as return to sport, and regularly monitoring progress to adjust the program as needed.
What is the importance of working with physical therapists and athletic trainers in the recovery process?
Working with physical therapists and athletic trainers can significantly enhance the recovery process. They provide personalized guidance, help in managing pain, and ensure that the rehabilitation program is executed correctly.
What is the significance of eccentric strength training for quadriceps tendinopathy?
Eccentric strength training is crucial for quadriceps tendinopathy as it helps in promoting collagen synthesis and improving tendon strength, thereby aiding in the recovery and reducing the risk of recurrence.
How can athletes manage quadriceps tendon pain effectively?
Managing quadriceps tendon pain involves reducing pain and inflammation. Rest and ice are crucial in the acute phase, alongside pain management strategies to ensure the athlete can continue with rehabilitation exercises.