Are inflammatory conditions affecting your knee joint causing discomfort and limiting your mobility? Knee synovitis is characterized by inflammation of the synovial membrane surrounding the knee joint, leading to pain and swelling.
Understanding the causes and symptoms of this condition is crucial in finding effective relief. Holistic approaches can play a significant role in managing knee synovitis by reducing inflammation and promoting overall joint health.
Key Takeaways
- Understanding knee synovitis and its impact on joint health
- The role of holistic approaches in managing the condition
- Importance of reducing inflammation for symptom relief
- Promoting overall well-being through natural treatments
- Exploring alternative remedies for knee synovitis
Understanding Knee Synovitis
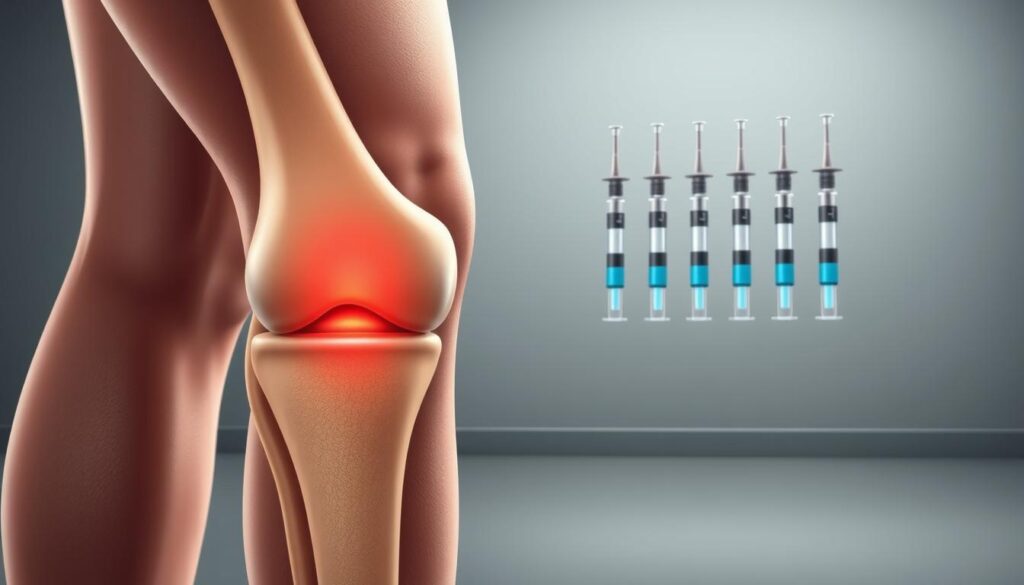
Understanding the intricacies of knee synovitis is crucial for effective management and relief. Knee synovitis refers to the inflammation of the synovial membrane, a condition that can significantly impact the quality of life for those affected.
What is Knee Synovitis?
Knee synovitis is characterized by the inflammation of the synovial membrane, which surrounds the knee joint. This condition can lead to pain, swelling, and stiffness in the knee. Rheumatoid arthritis, a chronic autoimmune disorder, is a common cause of knee synovitis.
The synovial membrane plays a vital role in maintaining the health of the knee joint by producing synovial fluid, which lubricates the joint and supplies nutrients to the cartilage. When this membrane becomes inflamed, it can lead to an overproduction of synovial fluid, causing swelling and pain.
Symptoms to Look Out For
The symptoms of knee synovitis can vary but typically include:
- Joint pain and tenderness
- Swelling and redness around the knee
- Warmth or heat around the affected joint
- Stiffness, especially after periods of rest
- Reduced range of motion
Recognizing these symptoms early is crucial for timely intervention and management.
“Early diagnosis and treatment of knee synovitis can significantly improve outcomes and reduce the risk of long-term damage.”
Causes of Knee Synovitis
The causes of knee synovitis are multifactorial, involving both genetic and environmental factors. Rheumatoid arthritis is a primary cause, where the body’s immune system mistakenly attacks the lining of the joints, leading to inflammation.
| Cause | Description |
|---|---|
| Rheumatoid Arthritis | A chronic autoimmune disorder that causes the immune system to attack the joint lining. |
| Genetic Factors | Genetic predisposition can increase the risk of developing knee synovitis. |
| Environmental Triggers | Factors such as infections or injuries can trigger the onset of knee synovitis in susceptible individuals. |
Understanding these causes is essential for developing effective treatment plans.
Natural Remedies for Knee Synovitis
Natural approaches offer a promising solution for individuals dealing with knee synovitis. By incorporating various natural remedies, individuals can potentially reduce inflammation and improve their overall joint health.
Introduction to Natural Remedies
Natural remedies encompass a broad range of treatments, including dietary changes, herbal supplements, and other holistic practices. These remedies aim to address the root causes of knee synovitis, providing relief from symptoms and improving quality of life.
Some of the most effective natural remedies include anti-inflammatory herbs and dietary adjustments. For instance, certain foods have anti-inflammatory properties that can help reduce knee swelling.

Importance of Natural Approaches
Adopting natural approaches can be beneficial for several reasons. Firstly, natural remedies often have fewer side effects compared to conventional medications, making them a safer option for long-term use.
“The use of natural remedies can complement traditional treatments, offering a more holistic approach to managing knee synovitis.”
Furthermore, natural remedies can be tailored to individual needs, allowing for a more personalized treatment plan. This can include dietary changes, such as incorporating foods rich in omega-3 fatty acids, which are known for their anti-inflammatory properties.
| Remedy | Description | Benefits |
|---|---|---|
| Turmeric | Contains curcumin, a compound with anti-inflammatory properties | Reduces inflammation and pain |
| Ginger | Has anti-inflammatory compounds called gingerols | Helps reduce pain and inflammation |
| Omega-3 Fatty Acids | Found in fish oil, these fatty acids reduce inflammation | Improves joint health and reduces symptoms |
By exploring these natural remedies, individuals can take a proactive approach to managing knee synovitis and improving their overall well-being.
Dietary Changes for Relief
A well-planned diet is essential for reducing inflammation associated with knee synovitis. Dietary changes play a significant role in managing the condition, and making informed food choices can help alleviate symptoms.
Incorporating the right foods into your diet can help mitigate knee synovitis symptoms. Certain nutrients have anti-inflammatory properties that can reduce inflammation and promote joint health.
Foods to Include
Foods rich in omega-3 fatty acids, such as salmon and sardines, are known for their anti-inflammatory effects. Additionally, consuming foods high in antioxidants like berries, leafy greens, and other fruits and vegetables can help reduce oxidative stress and inflammation.
Other beneficial foods include:
- Turmeric: Contains curcumin, which has potent anti-inflammatory and antioxidant properties.
- Ginger: Has anti-inflammatory compounds like gingerol, which can help reduce pain and inflammation.
- Green tea: Rich in antioxidants and has been shown to have anti-inflammatory effects.
Foods to Avoid
Just as some foods can help alleviate knee synovitis symptoms, others can exacerbate them. It’s essential to limit or avoid foods that promote inflammation.
Some foods to avoid include:
- Processed meats: High in advanced glycation end (AGE) products, which can stimulate inflammation.
- Sugary drinks and foods: Can lead to increased inflammation due to their high sugar content.
- Refined carbohydrates: Can cause a spike in blood sugar and insulin resistance, leading to increased inflammation.
For more detailed information on foods to avoid, especially in the context of knee osteoarthritis, you can visit this resource.
| Food Category | Beneficial Foods | Foods to Avoid |
|---|---|---|
| Protein Sources | Fatty fish (salmon, sardines), nuts, and seeds | Processed meats (hot dogs, sausages) |
| Fruits and Vegetables | Berries, leafy greens, turmeric, and ginger | Nightshade vegetables (for some individuals) |
| Beverages | Green tea, water | Sugary drinks (soda, sports drinks) |
Top Essential Oils for Relief
In the quest for knee synovitis relief, essential oils such as peppermint, lavender, and eucalyptus have gained significant attention due to their anti-inflammatory and pain-relieving properties.
These essential oils can be used in various ways to alleviate knee pain and inflammation, offering a holistic approach to managing synovitis symptoms.

Peppermint Oil
Peppermint oil is known for its cooling effect, which can help reduce pain and inflammation associated with knee synovitis.
It contains menthol, which has a natural analgesic effect, providing relief from pain.
Lavender Oil
Lavender oil is renowned for its calming properties, which can help reduce stress and promote relaxation, indirectly alleviating knee synovitis symptoms.
Its anti-inflammatory properties can also contribute to reducing swelling and pain in the knee.
Eucalyptus Oil
Eucalyptus oil has potent anti-inflammatory effects that can help manage knee synovitis by reducing inflammation and easing pain.
It is also known for its decongestant properties, which can help improve circulation, further aiding in the healing process.
By incorporating these essential oils into your daily routine, you can explore a natural and holistic approach to managing knee synovitis symptoms.
The Role of Physical Activity
Engaging in physical activity is a crucial aspect of managing knee synovitis naturally. Regular exercise can help maintain joint mobility, reduce stiffness, and alleviate pain associated with knee synovitis. According to the Arthritis Foundation, exercise is vital for maintaining healthy joints and overall well-being.
Gentle Exercises to Try
Gentle exercises are recommended for individuals with knee synovitis as they help improve joint mobility without causing further irritation. Some beneficial exercises include:
- Straight leg raises: Lift your leg straight out in front of you while lying on your back.
- Quad sets: Tighten your quadriceps muscles by straightening your knee.
- Short arc movements: Perform gentle, short movements of the knee, such as slight bends or straightens.
These exercises can be done regularly to help maintain flexibility and strength around the knee.
Importance of Stretching
Stretching is another critical component of managing knee synovitis. It helps improve flexibility, reduce stiffness, and promote healing. As noted by healthcare professionals,
“Regular stretching can significantly reduce knee pain and improve function in individuals with knee synovitis.”
Incorporating stretching exercises into your daily routine can lead to noticeable improvements in knee mobility and overall comfort.
In conclusion, physical activity, including gentle exercises and stretching, plays a vital role in managing knee synovitis. By incorporating these activities into your daily routine, you can improve joint mobility, reduce pain, and enhance your overall quality of life. As emphasized by experts, maintaining an active lifestyle is crucial for long-term knee health.
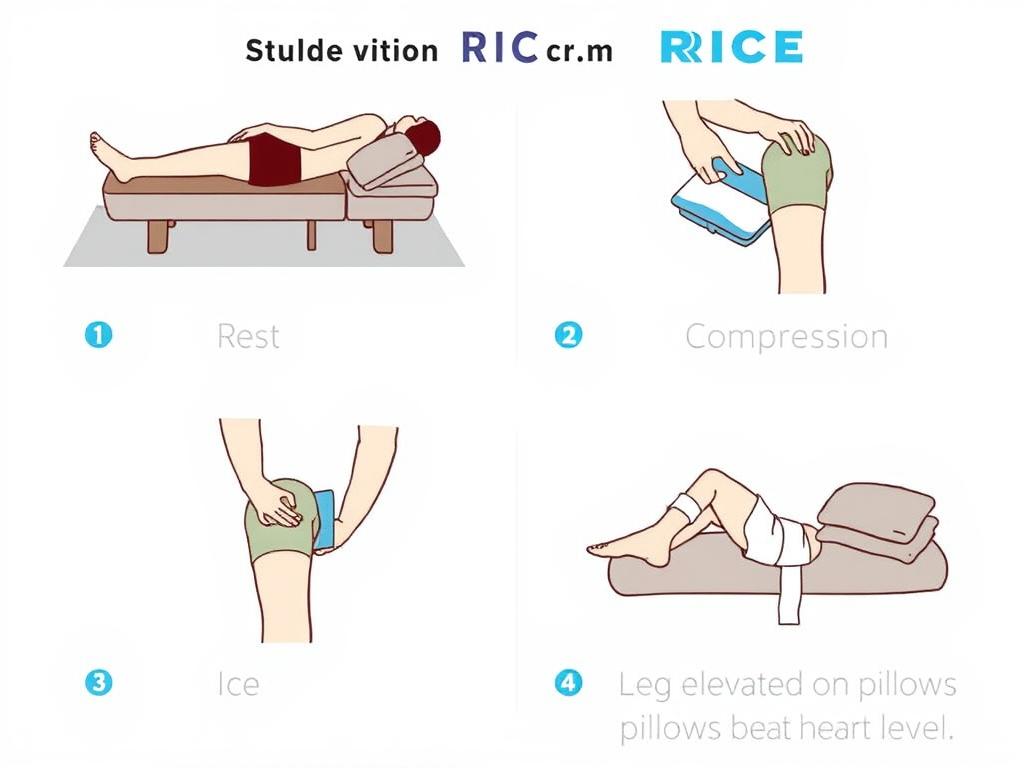
Using Hot and Cold Therapy
Both heat and cold therapies have been recognized for their potential in easing knee synovitis symptoms. Hot and cold therapy can provide relief by reducing pain and inflammation, making it a valuable addition to a treatment plan.
Benefits of Heat Therapy
Heat therapy is known for its ability to relax muscles and increase blood flow to the affected area. This can be particularly beneficial for individuals with knee synovitis, as it helps in reducing stiffness and promoting healing. Applying heat can be done using a warm bath, a heating pad, or even a warm cloth.
Key benefits of heat therapy include:
- Relaxation of muscles around the knee
- Increased blood flow to promote healing
- Reduction in stiffness and pain
Benefits of Cold Therapy
Cold therapy, on the other hand, is effective in reducing inflammation and numbing pain. It works by constricting blood vessels and reducing metabolic rate, which can help in minimizing swelling. Cold therapy can be applied using an ice pack or a cold compress.
Key benefits of cold therapy include:
- Reduction in inflammation and swelling
- Numbing of pain
- Constriction of blood vessels to reduce bruising
To effectively use hot and cold therapy, it’s essential to understand when to apply each. Generally, cold therapy is recommended during acute phases of inflammation, while heat therapy is more beneficial during the chronic phase or after activity.
| Therapy Type | Benefits | Application Method |
|---|---|---|
| Heat Therapy | Relaxes muscles, increases blood flow, reduces stiffness | Warm bath, heating pad, warm cloth |
| Cold Therapy | Reduces inflammation, numbs pain, constricts blood vessels | Ice pack, cold compress |

Herbal Supplements for Support
For those dealing with knee synovitis, certain herbal supplements may offer relief by targeting inflammation. These natural remedies can complement traditional treatments, providing a holistic approach to managing the condition.
Turmeric
Turmeric, with its active compound curcumin, is renowned for its potent anti-inflammatory and antioxidant properties. Studies have shown that curcumin can significantly reduce joint inflammation and alleviate symptoms associated with knee synovitis.
Benefits of Turmeric: Anti-inflammatory effects, antioxidant properties, potential to improve joint health.
Ginger
Ginger has been used for centuries in traditional medicine for its anti-inflammatory properties. It contains compounds like gingerol, which have been shown to reduce pain and inflammation in the joints, making it a valuable supplement for knee synovitis management.
Ginger’s Role: Reduces pain and inflammation, improves joint mobility.
Boswellia
Boswellia, also known as frankincense, is another herbal supplement that has been found to possess anti-inflammatory properties. It works by inhibiting the production of pro-inflammatory enzymes, thereby reducing inflammation and pain in the knee joint.
Here’s a comparison of these herbal supplements:
| Herbal Supplement | Primary Benefit | Key Compound |
|---|---|---|
| Turmeric | Reduces inflammation | Curcumin |
| Ginger | Reduces pain and inflammation | Gingerol |
| Boswellia | Inhibits pro-inflammatory enzymes | Acetyl-boswellic acids |
Incorporating these herbal supplements into your daily regimen, under the guidance of a healthcare professional, can provide additional support for managing knee synovitis. It’s essential to choose high-quality supplements to maximize their potential benefits.
Alternative Therapies
Alternative therapies offer a complementary approach to traditional treatments for knee synovitis. These therapies focus on treating the whole person, not just the symptoms, and can provide relief and improve quality of life.
“The integration of alternative therapies into a treatment plan can significantly enhance patient outcomes,” notes a study on holistic approaches to arthritis management.
Acupuncture
Acupuncture is an ancient practice that involves inserting thin needles into specific points on the body. It is believed to stimulate healing, reduce pain, and improve function in patients with knee synovitis. Research has shown that acupuncture can be effective in managing chronic pain and inflammation associated with knee synovitis.
Benefits of Acupuncture:
- Reduces pain and inflammation
- Improves joint function
- Enhances overall well-being
Massage Therapy
Massage therapy involves the manipulation of soft tissue to promote relaxation, ease muscle tension, and improve circulation. For knee synovitis, massage can help reduce stiffness, improve range of motion, and promote healing.
Regular massage therapy sessions can lead to significant improvements in symptoms and quality of life for individuals with knee synovitis.
Incorporating alternative therapies like acupuncture and massage therapy into a treatment plan can provide a more comprehensive approach to managing knee synovitis. These therapies not only address the physical aspects of the condition but also contribute to overall well-being.
Lifestyle Modifications
Lifestyle adjustments play a vital role in the holistic management of knee synovitis. By incorporating simple yet effective changes into daily routines, individuals can significantly alleviate their symptoms and improve their quality of life.
Importance of Maintaining a Healthy Weight
Maintaining a healthy weight is crucial for reducing the strain on the knee joint, thereby alleviating some of the pressure that contributes to synovitis symptoms. Excess weight can exacerbate the condition, making weight management a key aspect of knee synovitis management. A healthy diet combined with regular, gentle exercise can help achieve and maintain a healthy weight.
Aiming for a balanced diet rich in fruits, vegetables, whole grains, and lean proteins can support overall health and weight management. Consulting with a healthcare provider or a nutritionist can provide personalized guidance tailored to individual needs.
Mindfulness and Stress Reduction
Mindfulness and stress reduction techniques are valuable tools in managing the psychological aspects of chronic pain associated with knee synovitis. Practices such as meditation, deep breathing exercises, and yoga can help reduce stress levels and improve overall well-being.
Engaging in mindfulness practices can lead to a decrease in pain perception and an improvement in mood. Mindfulness-based stress reduction (MBSR) programs have been shown to be particularly effective in managing chronic pain and improving quality of life.
- Meditation and deep breathing exercises
- Yoga and tai chi
- Progressive muscle relaxation
By incorporating these lifestyle modifications, individuals with knee synovitis can experience significant relief from symptoms and an improvement in their overall quality of life.
When to Seek Professional Help
While natural remedies and lifestyle changes can offer significant relief from knee synovitis, it’s crucial to recognize when professional medical help is necessary. Severe symptoms can indicate a more serious underlying condition that requires immediate attention.
Identifying Severe Symptoms
Recognizing severe symptoms is vital for timely intervention. If you experience intense pain, significant swelling, or difficulty moving the knee, it’s essential to consult a healthcare provider. These symptoms may signal a need for alternative treatments for knee inflammation or other medical interventions.
Collaboration with Healthcare Providers
Working closely with healthcare providers ensures that knee synovitis is managed effectively. They can offer personalized guidance on seeking professional help for knee synovitis, recommend appropriate treatments, and provide knee pain relief strategies tailored to your specific needs.
FAQ
What is knee synovitis and how is it related to rheumatoid arthritis?
Knee synovitis is often associated with rheumatoid arthritis, a condition where the body’s immune system attacks the lining of the joints, leading to inflammation and pain.
What are the symptoms of knee synovitis?
The symptoms of knee synovitis include joint pain, swelling, and stiffness, which can significantly impact daily activities and overall well-being.
How can dietary changes help manage knee synovitis?
Including foods rich in anti-inflammatory properties, such as omega-3 fatty acids, and avoiding pro-inflammatory foods can help alleviate symptoms and support joint health.
What essential oils are beneficial for knee synovitis relief?
Peppermint oil, lavender oil, and eucalyptus oil are particularly beneficial due to their cooling, calming, and anti-inflammatory effects, which can help alleviate knee pain and inflammation.
How does physical activity impact knee synovitis?
Gentle exercises and stretching can help improve joint mobility, reduce stiffness, and alleviate pain, making physical activity a crucial component of managing knee synovitis.
What is the role of hot and cold therapy in managing knee synovitis?
Heat therapy can help relax muscles and increase blood flow, while cold therapy can reduce inflammation and numb pain, providing relief from knee synovitis symptoms.
How can herbal supplements support knee synovitis treatment?
Turmeric, ginger, and boswellia are valuable additions to a treatment plan due to their anti-inflammatory properties, which can help reduce inflammation and alleviate symptoms.
What alternative therapies can complement traditional treatments for knee synovitis?
Acupuncture and massage therapy offer complementary treatments that can enhance overall well-being by stimulating healing, reducing pain, and improving joint mobility.
Why is maintaining a healthy weight important for knee synovitis management?
Maintaining a healthy weight reduces the strain on the knee joint, which can help alleviate symptoms and slow disease progression.
When should I seek professional help for knee synovitis?
Recognizing severe symptoms and collaborating with healthcare providers ensures that knee synovitis is managed effectively, and any underlying conditions are addressed.
What are some holistic approaches for managing knee synovitis?
Holistic approaches include dietary changes, herbal supplements, essential oils, physical activity, hot and cold therapy, and alternative therapies like acupuncture and massage therapy.
Are there any natural treatments for knee synovitis that can be done at home?
Yes, natural treatments such as dietary changes, using essential oils, practicing gentle exercises, and applying hot and cold therapy can be done at home to help manage knee synovitis.
How can joint health supplements support knee synovitis treatment?
Joint health supplements, including those containing omega-3 fatty acids, glucosamine, and chondroitin, can support knee health and alleviate symptoms.