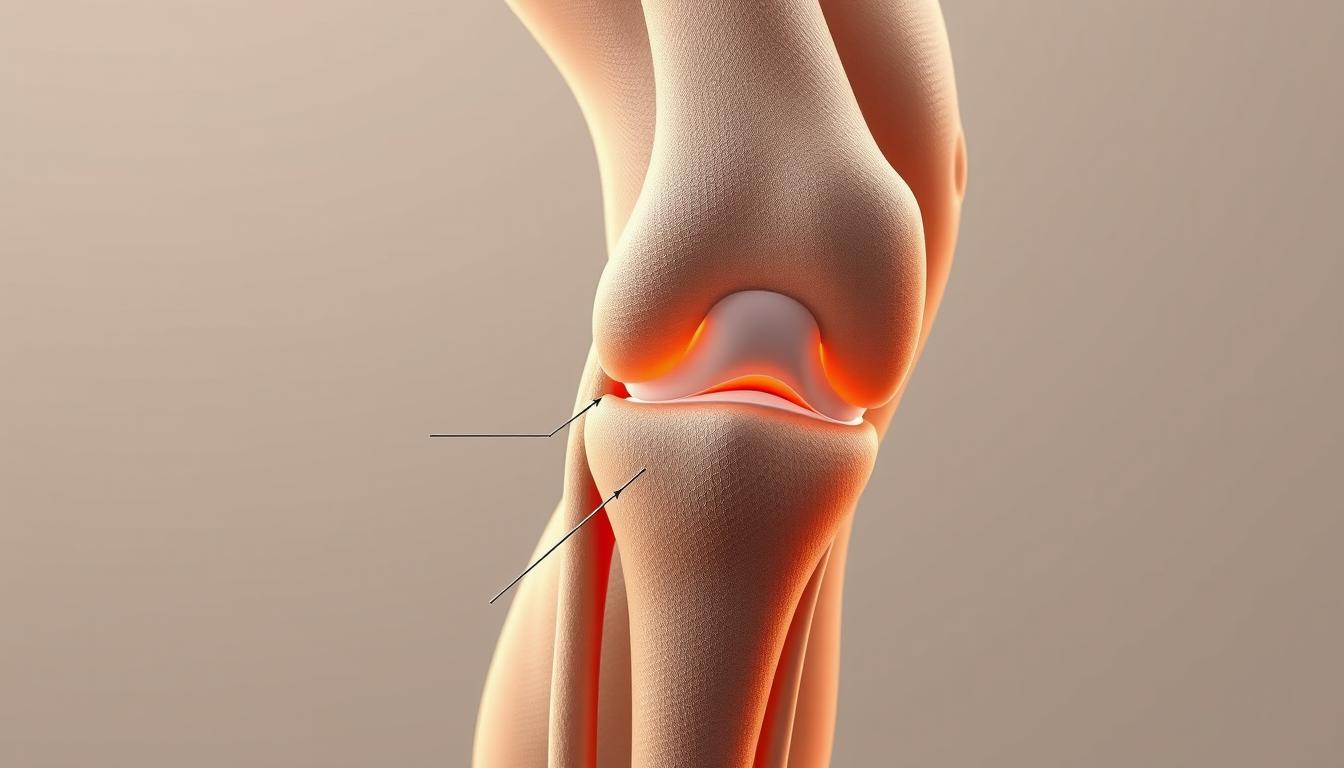
Are knee pain and limited mobility affecting your daily life? You might be suffering from either Pes Anserine Bursitis or an MCL Tear, two distinct knee conditions that require accurate diagnosis and treatment.
Understanding the differences between these conditions is crucial for effective management. While both can cause significant discomfort, their symptoms and treatment approaches differ. Pes Anserine Bursitis involves inflammation of the bursa at the lower knee, leading to pain on the inner aspect of the knee. On the other hand, an MCL Tear involves damage to the medial collateral ligament, a critical ligament that provides stability to the knee.
Regenexx procedures offer a promising solution for treating these knee conditions. This article will delve into the symptoms, diagnosis, and treatment options for Pes Anserine Bursitis and MCL Tear, helping you understand which condition you might be dealing with and how to find relief.
Key Takeaways
- Understanding the differences between Pes Anserine Bursitis and MCL Tear is crucial for effective treatment.
- Pes Anserine Bursitis involves inflammation of the bursa, causing inner knee pain.
- An MCL Tear involves damage to the medial collateral ligament, affecting knee stability.
- Regenexx procedures are a viable treatment option for both conditions.
- Accurate diagnosis is key to managing knee pain and restoring mobility.
Overview of Pes Anserine Bursitis
The pes anserine bursa plays a vital role in knee function, and its inflammation can lead to significant discomfort. Pes anserine bursitis is a condition characterized by the inflammation of this bursa, which is located at the lower inner aspect of the knee.
What is Pes Anserine Bursitis?
Pes anserine bursitis refers to the inflammation of the bursa located between the tibia (shinbone) and the tendons of the sartorius, gracilis, and semitendinosus muscles. This bursa reduces friction between these tendons and the tibia, facilitating smooth knee movement. When this bursa becomes inflamed, it can cause pain and tenderness in the lower inner knee area.
Common Causes and Risk Factors
Several factors contribute to the development of pes anserine bursitis. Overuse or repetitive stress on the knee is a common cause, often seen in athletes or individuals who engage in activities that involve running or cycling. Other risk factors include poor knee alignment, obesity, and previous knee injuries or surgeries. Additionally, conditions like osteoarthritis can increase the risk of developing pes anserine bursitis.
Symptoms of Pes Anserine Bursitis
The primary symptom of pes anserine bursitis is pain on the lower inner aspect of the knee, which can be exacerbated by activities such as climbing stairs, running, or even simple actions like standing up from a seated position. Swelling and tenderness in the affected area are also common. In some cases, the pain can radiate down the leg, mimicking other knee conditions.
Strengthening exercises, such as those targeting the muscles around the knee, can help alleviate symptoms by improving knee stability and reducing pain. Resources like the knee exercise guide can provide valuable information on appropriate exercises.
Overview of MCL Tear
The medial collateral ligament (MCL) is crucial for knee stability, and tears in this ligament can significantly impact mobility and comfort. The MCL is one of the key ligaments that help stabilize the knee joint, and injuries to it are common, especially among athletes.
What is an MCL Tear?
An MCL tear refers to a partial or complete rupture of the medial collateral ligament, which connects the femur (thigh bone) to the tibia (shin bone) in the knee. This ligament is vital for providing stability to the knee, especially during movements that involve bending or twisting.
Causes of MCL Tears
MCL tear causes can vary, but they often result from direct blows to the knee, such as those experienced during contact sports like football or soccer. Other causes include sudden twisting or bending movements that put excessive stress on the MCL. Athletes participating in sports that involve cutting, pivoting, or sudden changes in direction are at a higher risk of sustaining an MCL tear.
Symptoms of an MCL Tear
The MCL tear symptoms can range from mild to severe, depending on the extent of the injury. Common symptoms include pain and tenderness along the inside of the knee, swelling, and instability or a feeling of the knee giving way. In some cases, individuals may hear a popping sound at the time of injury.
For those diagnosed with an MCL tear, treatment options vary. While traditional treatments often involve rest, physical therapy, or in severe cases, surgery, some patients may benefit from innovative procedures like those offered by Regenexx. Regenexx procedures provide a non-surgical alternative, utilizing the body’s natural healing processes to repair damaged ligaments.
Similarities Between Pes Anserine Bursitis and MCL Tear
Understanding the similarities between Pes Anserine Bursitis and MCL tears is crucial for accurate diagnosis and effective treatment. Both conditions affect the knee and can cause significant pain and discomfort, making it essential to identify their commonalities.
Common Symptoms
One of the primary similarities between Pes Anserine Bursitis and MCL tears is the presence of common symptoms. Both conditions can cause knee pain, swelling, and stiffness. The pain associated with Pes Anserine Bursitis is typically located on the lower inner aspect of the knee, while MCL tears can cause pain along the medial (inner) aspect of the knee. Despite these differences in pain location, both conditions can result in significant discomfort and limited mobility.
Another common symptom is swelling. In both conditions, swelling can occur due to inflammation. For Pes Anserine Bursitis, the swelling is usually localized to the area around the pes anserine bursa, whereas MCL tears can cause more widespread swelling along the medial aspect of the knee.
Similar Risk Factors
Both Pes Anserine Bursitis and MCL tears share similar risk factors. Sports injuries are a common risk factor for both conditions, particularly in sports that involve running, jumping, or quick changes of direction. Activities that stress the knee joint, such as football, soccer, and basketball, increase the risk of developing either condition.
Additionally, overuse and repetitive strain on the knee can contribute to the development of Pes Anserine Bursitis. Similarly, MCL tears can occur due to repetitive stress or acute injuries. Other risk factors include poor training habits, inadequate warm-up or cool-down exercises, and biomechanical issues such as overpronation or flat feet.
Key Differences in Symptoms
Understanding the distinct symptoms of Pes Anserine Bursitis and MCL tears is crucial for accurate diagnosis. While both conditions can cause knee pain and discomfort, their symptom profiles have distinct characteristics that can guide healthcare professionals toward the correct diagnosis.
Pain Location Comparisons
One of the primary differences between Pes Anserine Bursitis and MCL tears lies in the location of the pain. Pes Anserine Bursitis typically causes pain on the lower inner aspect of the knee, approximately 2-3 inches below the joint line. This pain is often described as sharp and tender to the touch. In contrast, an MCL tear usually results in pain along the medial (inner) aspect of the knee, often directly over the ligament. The pain from an MCL tear can be more diffuse and may be associated with a feeling of instability.
Variations in Swelling and Stiffness
Swelling and stiffness are common symptoms in both conditions, but their presentation can vary. Pes Anserine Bursitis often results in localized swelling and tenderness over the pes anserine area, with stiffness being more pronounced after periods of rest or inactivity. An MCL tear, on the other hand, may cause more generalized swelling along the medial aspect of the knee, potentially accompanied by bruising. The stiffness associated with an MCL tear can be significant, especially in the acute phase, and may be accompanied by a feeling of knee instability.
Recognizing these differences in symptom presentation is essential for healthcare providers to make an accurate diagnosis and develop an appropriate treatment plan. By understanding the unique characteristics of each condition, patients can receive targeted care that addresses their specific needs.
Diagnostic Procedures
Understanding the diagnostic procedures for pes anserine bursitis and MCL tears is essential for proper treatment. Accurate diagnosis is crucial for developing an effective treatment plan, as both conditions affect the knee but require different approaches.
Physical Examination Techniques
A thorough physical examination is the first step in diagnosing both pes anserine bursitis and MCL tears. Healthcare professionals use various techniques to assess knee function and identify the source of pain. For pes anserine bursitis, tenderness over the pes anserine area, typically located about 2 inches below the joint line on the medial aspect of the knee, is a key indicator. In contrast, MCL tears are diagnosed by assessing knee stability, particularly in the medial (inner) aspect of the knee.
Specific physical examination maneuvers include the valgus stress test for MCL tears, which checks for medial knee instability. For pes anserine bursitis, palpation (feeling with the fingers) over the pes anserine bursa can elicit tenderness.
Imaging Tests for Accurate Diagnosis
While physical examination provides valuable insights, imaging tests are often necessary to confirm the diagnosis. For both conditions, MRI (Magnetic Resonance Imaging) is a preferred imaging modality due to its ability to visualize soft tissue injuries, including ligament tears and bursitis.
An MRI can help differentiate between pes anserine bursitis and MCL tears by showing inflammation of the bursa or ligamentous injury, respectively. In some cases, an ultrasound may also be used, particularly to evaluate the pes anserine bursa.
The choice of imaging test depends on the clinical presentation and the healthcare provider’s suspicion of the underlying condition. Advanced diagnostic techniques, as mentioned on the Regenexx website, may also include other specialized tests to further evaluate knee conditions.
Treatment Options for Pes Anserine Bursitis
The treatment of pes anserine bursitis is multifaceted, incorporating both non-surgical methods and surgical options tailored to the severity of the condition.
Conservative management is typically the first line of treatment for pes anserine bursitis. This approach includes a variety of strategies aimed at reducing inflammation, alleviating pain, and improving function.
Conservative Treatment Strategies
Conservative treatment strategies for pes anserine bursitis include:
- Physical therapy to strengthen the surrounding muscles and improve flexibility
- Non-steroidal anti-inflammatory drugs (NSAIDs) to reduce pain and inflammation
- Corticosteroid injections to decrease inflammation
- Rest and activity modification to avoid exacerbating the condition
Additionally, innovative treatments such as Regenexx procedures, which are non-surgical and utilize the body’s own healing mechanisms, are gaining recognition. According to the Regenexx website, these procedures offer a promising alternative for patients seeking to avoid surgery.
“Regenerative medicine offers a new paradigm in the treatment of pes anserine bursitis, providing patients with options that are less invasive than traditional surgery.”
Surgical Options for Severe Cases
In cases where conservative management fails to provide adequate relief, surgical intervention may be considered. Surgical options can include:
| Treatment Approach | Description | Indications |
|---|---|---|
| Bursectomy | Surgical removal of the inflamed bursa | Chronic bursitis not responsive to conservative treatment |
| Tendon repair or reconstruction | Addressing any underlying tendon issues contributing to bursitis | Presence of significant tendon damage or degeneration |
The choice between conservative and surgical treatments depends on the severity of symptoms, the patient’s overall health, and the effectiveness of initial treatments. A healthcare professional can provide guidance on the most appropriate treatment plan.
Treatment Options for MCL Tear
The treatment of MCL tears involves a multifaceted approach, considering the severity of the injury and the patient’s overall health. Effective management strategies are crucial for optimal recovery and preventing further complications.
Non-Surgical Approaches
For many patients, non-surgical treatments are the first line of defense against MCL tears. These include bracing to provide stability to the knee, physical therapy to strengthen the surrounding muscles, and pain management through medication. Bracing is particularly useful as it helps in reducing the stress on the MCL, allowing it to heal.
Physical therapy plays a critical role in the rehabilitation process, focusing on improving knee mobility and strength. A well-structured physical therapy program can significantly enhance recovery outcomes.
Rehabilitation and Recovery
The rehabilitation phase is crucial for regaining knee function and preventing future injuries. A comprehensive rehabilitation program includes exercises tailored to improve strength, flexibility, and range of motion. Regenexx procedures, which involve the use of platelet-rich plasma (PRP) therapy, have emerged as a promising treatment option for MCL tears, potentially reducing the need for surgical intervention.
According to the Regenexx website, their procedures can be an effective treatment for MCL tears by promoting healing and tissue repair. Incorporating such advanced therapies into the treatment plan can offer patients a more conservative yet effective alternative to surgery.
Rehabilitation and recovery also involve a gradual return to activity, ensuring that the knee is adequately prepared to handle the stresses of normal and sports-specific activities. Monitoring progress and adjusting the treatment plan as necessary are key components of successful rehabilitation.
In conclusion, the treatment of MCL tears requires a tailored approach, considering the severity of the tear and the individual patient’s needs. By combining non-surgical approaches with advanced therapies like Regenexx procedures, patients can achieve optimal recovery and return to their normal activities.
When to Seek Medical Attention
Recognizing the warning signs for both pes anserine bursitis and MCL tears is vital for effective treatment. If you’re experiencing knee pain or other symptoms, it’s essential to know when to seek medical help.
Warning Signs for Both Conditions
Both pes anserine bursitis and MCL tears can present with significant knee pain and discomfort. Key warning signs that necessitate medical evaluation include:
- Severe pain or swelling
- Instability or buckling of the knee
- Difficulty walking or bearing weight
- Pain that persists or worsens over time
| Symptom | Pes Anserine Bursitis | MCL Tear |
|---|---|---|
| Severe Pain | Common, especially with movement | Often severe, especially after injury |
| Swelling | Localized to the pes anserine area | Can be more widespread around the knee |
| Instability | Less common | More common due to ligament damage |

Importance of Early Diagnosis
Early diagnosis is crucial for effective treatment of both pes anserine bursitis and MCL tears. According to the Regenexx website, seeking medical attention for knee injuries is vital to prevent further complications. An early and accurate diagnosis can lead to more targeted and effective treatment strategies, improving outcomes and reducing the risk of long-term damage.
For instance, early intervention for MCL tears can involve non-surgical approaches such as physical therapy and bracing, potentially avoiding the need for surgery. Similarly, pes anserine bursitis can often be managed with conservative treatments, including rest, ice, and anti-inflammatory medications, if addressed promptly.
Preventative Measures
Preventing knee injuries such as Pes Anserine Bursitis and MCL tears requires a comprehensive approach that includes exercises and lifestyle adjustments. By understanding the causes and implementing effective prevention strategies, individuals can significantly reduce their risk of developing these conditions.
Tips to Avoid Pes Anserine Bursitis
Pes Anserine Bursitis is often caused by overuse, poor training techniques, and inadequate warm-up routines. To avoid this condition, it’s essential to incorporate exercises that strengthen the knee and improve flexibility.
Some effective exercises include:
- Hamstring stretches: Tight hamstrings can contribute to Pes Anserine Bursitis, so regular stretching is crucial.
- Quadriceps strengthening: Strengthening the quadriceps helps stabilize the knee and reduce strain on the Pes Anserine bursa.
- Knee flexion exercises: Gentle knee flexion exercises can help maintain or improve range of motion.
According to the knee exercise guide website, incorporating these exercises into a regular routine can help prevent knee injuries, including Pes Anserine Bursitis.
How to Prevent MCL Tears
MCL tears are commonly caused by direct blows to the knee, sudden stops, or quick changes in direction. Preventing MCL tears involves a combination of strengthening exercises, proper training techniques, and equipment adjustments.
| Prevention Strategy | Description | Benefit |
|---|---|---|
| Strengthening knee ligaments | Exercises that strengthen the muscles around the knee | Improved knee stability |
| Proper training techniques | Avoiding sudden changes in direction or speed | Reduced risk of sudden knee injuries |
| Equipment adjustments | Ensuring proper footwear and knee support | Minimized risk of knee injuries from external factors |
By understanding the causes of MCL tears and implementing these prevention strategies, individuals can significantly reduce their risk of injury.
Conclusion: Making the Right Diagnosis
The complexity of knee injuries necessitates a professional evaluation to differentiate between Pes anserine bursitis and MCL tears. Both conditions present unique challenges and require distinct treatment approaches.
Importance of Professional Evaluation
A professional evaluation is crucial for an accurate diagnosis. As emphasized by the Regenexx website, a thorough assessment by a healthcare professional is vital for determining the appropriate treatment plan. This is because both Pes anserine bursitis and MCL tears can present with similar symptoms, making self-diagnosis challenging.
Key benefits of professional evaluation include:
- Accurate diagnosis through comprehensive examination
- Tailored treatment plans based on individual needs
- Prevention of further injury through appropriate management
Recap of Key Differences
To summarize, the key differences between Pes anserine bursitis and MCL tears lie in their symptoms, causes, and treatment options. Pes anserine bursitis is characterized by inflammation of the bursa around the knee, often causing pain on the lower inner aspect of the knee. In contrast, an MCL tear involves damage to the medial collateral ligament, typically resulting from a direct blow to the knee.
- Location of pain: Pes anserine bursitis pain is typically on the lower inner knee, while MCL tear pain is often more widespread along the medial aspect.
- Causes: Pes anserine bursitis is often due to overuse or repetitive stress, whereas MCL tears are commonly caused by direct trauma.
- Treatment approaches: While both may involve conservative management, severe MCL tears may require surgical intervention.
Resources for Further Information
For those seeking more information on pes anserine bursitis vs MCL tear, several reliable resources are available. Understanding the differences between these two conditions is crucial for proper diagnosis and treatment.
Reliable Online Resources
Websites like Regenexx offer valuable insights into knee injuries, including pes anserine bursitis and MCL tears. The knee exercise guide is another useful resource for individuals looking to manage or prevent these conditions through exercise.
Publications and Books
Several books and publications provide in-depth information on knee injuries. Readers can explore medical journals and orthopedic books that cover topics related to pes anserine bursitis and MCL tears, enhancing their understanding of these conditions.
FAQ
What is pes anserine bursitis?
Pes anserine bursitis is a condition that causes pain on the lower inner aspect of the knee, often due to inflammation of the bursa located in this area.
What are the symptoms of pes anserine bursitis?
Symptoms include pain, swelling, and tenderness on the lower inner aspect of the knee, which can worsen with activities like climbing stairs or running.
What is an MCL tear?
An MCL (Medial Collateral Ligament) tear is an injury to one of the ligaments that connect the bones of the knee together, often caused by a blow to the outer knee.
How do I know if I have an MCL tear or pes anserine bursitis?
Accurate diagnosis requires a medical professional’s evaluation, including physical examination and potentially imaging tests like an MRI, to distinguish between the two conditions based on symptoms and severity.
Can strengthening exercises help manage pes anserine bursitis?
Yes, strengthening exercises, such as those targeting the muscles around the knee, can help improve knee stability and reduce pain associated with pes anserine bursitis.
What are the treatment options for pes anserine bursitis?
Treatment options include conservative strategies like physical therapy, non-surgical Regenexx procedures, and in severe cases, surgical intervention.
How are MCL tears treated?
Treatment for MCL tears often involves non-surgical approaches such as bracing and physical therapy, with Regenexx procedures being a potential treatment option, and in more severe cases, surgical repair.
Can pes anserine bursitis and MCL tears be prevented?
Yes, preventative measures include exercises that strengthen the knee, improve flexibility, and avoid overuse or direct trauma to the knee area.
When should I seek medical attention for knee pain?
It’s advisable to seek medical attention if you experience severe pain, instability, or if symptoms persist or worsen over time, as early diagnosis is crucial for effective treatment.
Are there any resources available for more information on pes anserine bursitis and MCL tears?
Yes, resources include websites like Regenexx and knee exercise guides, as well as medical organizations and publications that provide detailed information on knee injuries and their management.
What diagnostic procedures are used to identify pes anserine bursitis and MCL tears?
Diagnostic procedures include physical examination techniques and imaging tests such as MRI to accurately diagnose and differentiate between pes anserine bursitis and MCL tears.
What are the similarities between pes anserine bursitis and MCL tears?
Both conditions share common symptoms like knee pain and swelling, and similar risk factors such as sports injuries, making a thorough diagnosis crucial.