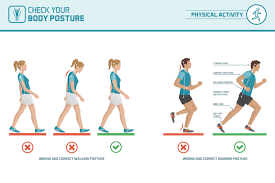
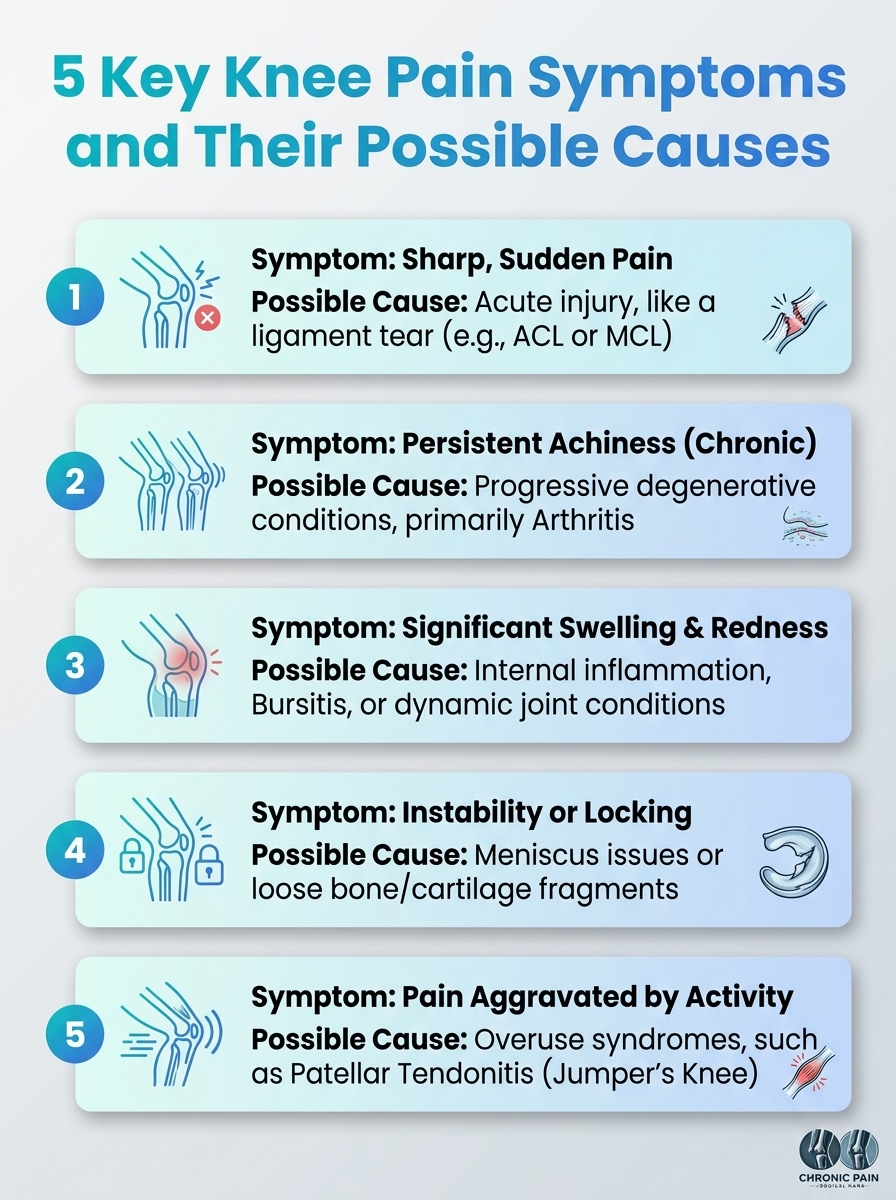
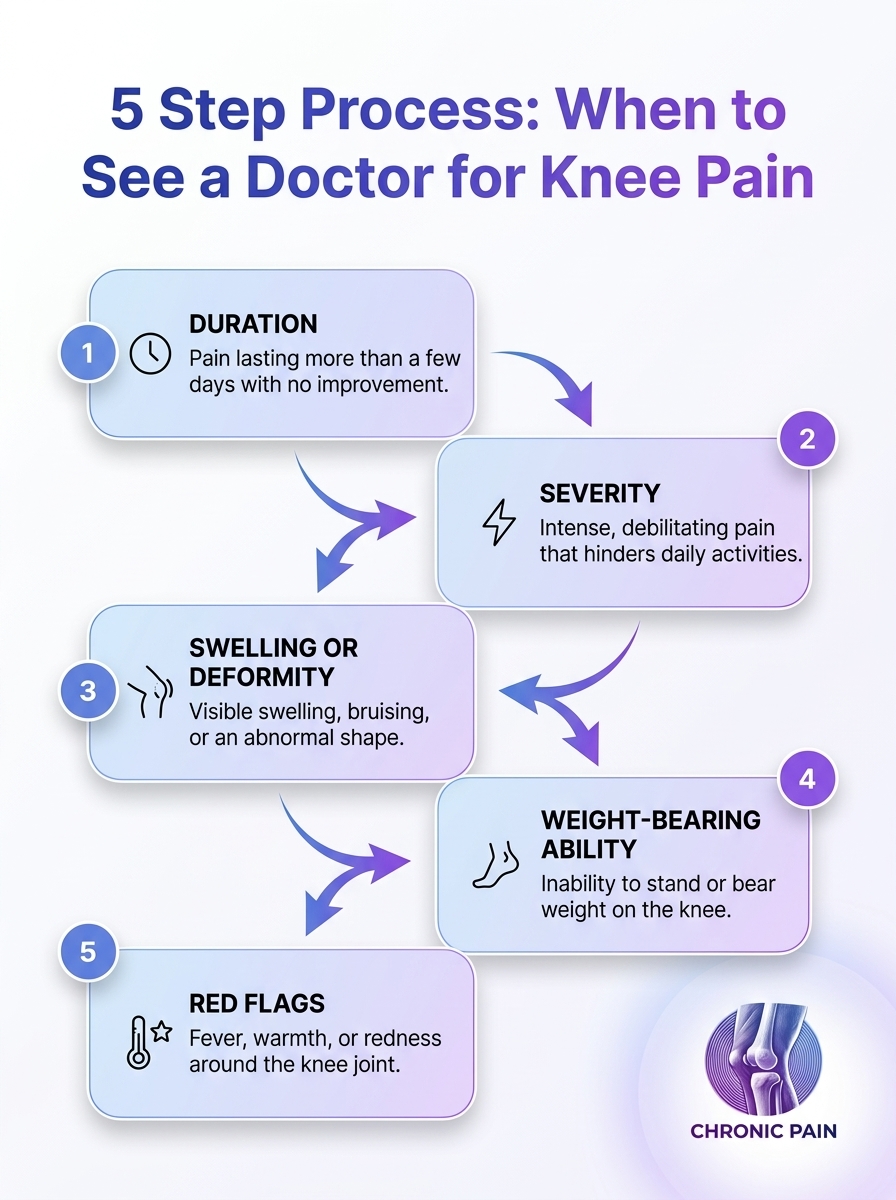
Walking with osteoarthritis knee pain can transform a simple daily activity into a challenging ordeal. Your knee joint bears significant pressure with every step. Finding the best knee support for osteoarthritis makes walking comfortable again.
Millions of people experience arthritis knee pain that limits their mobility. The right knee brace designed for osteoarthritis provides stability and compression. This support reduces pain during walking activities.
This comprehensive guide explores everything you need to know about knee support options. We cover different types, essential features, and how to choose the right fit. You will discover practical solutions for managing your condition while staying active.
Find Your Perfect Knee Support Match
Take our quick 60-second assessment to discover which knee support type matches your osteoarthritis severity and walking needs. Get personalized recommendations based on your specific condition.
Understanding Osteoarthritis and Knee Pain During Walking
Osteoarthritis affects the knee joint by breaking down protective cartilage over time. This degeneration causes bones to rub together during movement. Walking becomes painful as the cushioning between bones diminishes.
The condition creates inflammation around the knee area. Swelling increases pressure on surrounding tissue and nerves. Each step you take while walking puts stress on an already compromised joint.
Your body weight multiplies the force on your knee during walking activities. A 150-pound person generates approximately 450 pounds of pressure per step. This repetitive stress accelerates cartilage breakdown and intensifies pain.
How Knee Pain Affects Your Walking Pattern
Pain changes how you walk naturally. You might shift weight away from the affected knee unconsciously. This altered gait pattern creates problems in other joints over time.
Your muscles work harder to compensate for knee instability. This extra effort leads to fatigue and additional discomfort. The muscle strain can extend to your hips and lower back.
Limited range of motion restricts your stride length. Shorter steps reduce your walking speed and efficiency. These changes make daily activities more challenging and time-consuming.
Common Walking Symptoms
- Sharp pain with weight-bearing steps
- Stiffness after sitting or resting
- Grinding sensation during movement
- Swelling that worsens throughout the day
- Reduced walking distance tolerance
Impact on Daily Life
- Difficulty climbing stairs or inclines
- Challenges with grocery shopping
- Reduced participation in social activities
- Increased dependence on others
- Loss of confidence in mobility
Why Walking Remains Important Despite Pain
Movement keeps your knee joint healthy despite arthritis. Walking lubricates the joint and maintains cartilage nutrition. Complete inactivity actually accelerates joint deterioration.
Regular walking strengthens muscles around your knee. Strong muscles provide better support and stability. This muscle support reduces stress on damaged cartilage.
Physical activity helps manage your body weight effectively. Maintaining a healthy weight decreases pressure on knee joints. Every pound lost removes four pounds of pressure from your knees.
Types of Knee Supports for Osteoarthritis While Walking
Different knee support designs serve specific purposes for arthritis management. Understanding each type helps you select the most appropriate option. Your choice depends on pain severity and activity requirements.
Knee Braces for Maximum Support
Knee braces provide the highest level of support for osteoarthritis. These devices feature rigid structures with hinges or stays. A knee brace designed for arthritis redistributes weight away from damaged areas.
Unloader braces specifically target one side of your knee joint. They shift pressure from the affected compartment to healthier areas. This mechanism delivers significant pain relief during walking activities.
Hinged knee braces offer stability without completely restricting movement. The hinges allow natural bending while preventing harmful sideways motion. This design protects your joint during the healing process.
Wraparound braces feature adjustable straps for customized compression levels. You can modify the fit throughout the day as swelling changes. This flexibility makes them practical for extended wear during walking.
Important: Unloader braces work best for unicompartmental osteoarthritis affecting only one side of your knee. Consult healthcare professionals before using specialized braces for your specific condition.
Hinged Knee Braces
Provide maximum stability with controlled motion. Metal or composite hinges support your knee joint during movement. Ideal for moderate to severe arthritis pain.
- Bilateral support for both sides
- Prevents harmful lateral movement
- Allows natural flexion and extension
- Durable construction for long-term use
Unloader Knee Braces
Specifically designed to shift weight from damaged cartilage. Creates space in affected compartment during walking. Best for single-compartment osteoarthritis.
- Reduces pressure on worn cartilage
- Significant pain relief for targeted areas
- Customizable angle adjustment
- Prescription often recommended
Wraparound Braces
Easy-to-use design with customizable compression. Adjustable straps accommodate swelling changes. Suitable for mild to moderate arthritis knee pain.
- Simple application without stepping through
- Adjustable throughout the day
- Good for fluctuating swelling
- More affordable option
Knee Sleeves for Compression and Warmth
Knee sleeves offer compression therapy for arthritis management. These elastic garments slide over your knee like a sock. A knee sleeve provides consistent pressure around the entire joint.
Compression improves blood circulation in the affected area. Better circulation reduces inflammation and promotes healing. This therapy accelerates your body’s natural recovery process.
The fabric generates warmth around your knee joint. Heat soothes stiff muscles and improves flexibility. Many people experience reduced pain during walking with this gentle warmth.
Sleeves fit discreetly under regular clothing during daily activities. You can wear them throughout the day without drawing attention. This convenience encourages consistent use for better results.
Benefits of Compression Therapy
Compression sleeves work through several therapeutic mechanisms. The pressure stimulates proprioception, improving your joint awareness. Better awareness leads to more controlled movements and reduced injury risk.
The graduated compression design provides varying pressure levels. Tighter compression at specific points targets problem areas. This strategic pressure distribution optimizes pain relief and support.
Moisture-wicking materials keep your skin dry during extended wear. Breathable fabrics prevent overheating and discomfort. These features make sleeves suitable for all-day use.
Knee Sleeve Advantages
- Lightweight and comfortable for extended wear
- Improves circulation and reduces swelling
- Provides warmth for stiff joints
- Discreet under clothing
- Easy to put on and remove
- Affordable compared to rigid braces
- Machine washable for easy care
Knee Sleeve Limitations
- Limited structural support for severe cases
- May roll down during vigorous activity
- Compression can feel restrictive initially
- Less effective for instability issues
- Requires proper sizing for effectiveness
- Can cause skin irritation in some users
Knee Bands and Straps for Targeted Support
Knee bands provide focused pressure on specific problem areas. These narrow straps wrap around your knee or below the kneecap. The targeted compression addresses particular pain points effectively.
Patellar tracking bands help align your kneecap during movement. Proper alignment reduces friction and grinding sensations. This correction minimizes pain during walking activities.
Infrapatellar straps sit just below your kneecap. They reduce tension on the patellar tendon and surrounding tissue. This relief helps with pain concentrated around the kneecap area.
Bands offer minimal bulk while delivering therapeutic benefits. You can wear them alone or combine them with other support. This versatility makes them useful for various arthritis knee situations.
When to Use Knee Bands
Knee bands work best for specific osteoarthritis presentations. Consider bands when your pain localizes to the kneecap region. They effectively address anterior knee pain during walking.
Athletes with arthritis often prefer bands for continued activity. The minimal design allows greater freedom of movement. You maintain natural knee function while receiving targeted support.
Bands serve as supplementary support alongside other treatments. Combine them with knee sleeves for enhanced therapy. This layered approach addresses multiple aspects of your condition.
Combination Support Systems
Some knee support products combine multiple design elements. Hybrid braces integrate rigid support with compression benefits. These systems offer comprehensive therapy for complex needs.
A brace designed with both hinges and compression panels provides versatility. The rigid components deliver stability during walking. The compression zones reduce swelling and improve circulation simultaneously.
Modular systems allow you to customize your support level. Add or remove components based on daily requirements. This flexibility adapts to changing symptoms and activity levels.
Essential Features to Look for in Knee Support for Walking
Selecting the right knee support requires understanding key design features. Specific characteristics determine effectiveness for osteoarthritis management. These features directly impact your comfort and pain relief during walking.
Compression Level and Distribution
Appropriate compression reduces swelling without restricting circulation. Graduated compression provides varying pressure across different areas. The tightest compression should target the most affected regions.
Excessive compression causes discomfort and potential circulation problems. Insufficient pressure fails to deliver therapeutic benefits. Finding the right balance maximizes pain relief and comfort.
Look for adjustable compression in knee brace designs. Straps and closures should allow pressure modification. This adjustability accommodates swelling fluctuations throughout your day.
Material Quality and Breathability
Breathable materials prevent moisture buildup during extended wear. Moisture-wicking fabrics keep your skin dry and comfortable. Good ventilation reduces the risk of skin irritation and rashes.
Neoprene provides excellent compression and warmth retention. However, this material can trap heat and moisture. Consider perforated neoprene or alternative fabrics for better breathability.
Antimicrobial treatments resist odor and bacterial growth. These treatments maintain hygiene during daily use. Regular washing becomes easier with quality, durable materials.
| Material Type | Breathability | Compression | Durability | Best For |
| Neoprene | Low to Medium | High | Excellent | Maximum support and warmth |
| Elastic Blend | High | Medium | Good | All-day comfort |
| Mesh Fabric | Excellent | Low to Medium | Fair | Hot weather use |
| Compression Knit | Medium to High | Medium to High | Very Good | Balanced performance |
Stability and Support Structures
Rigid support elements provide stability for unstable knee joints. Side stays prevent excessive lateral movement during walking. This protection reduces stress on damaged cartilage and ligaments.
Hinged mechanisms allow controlled flexion and extension. Quality hinges move smoothly through your natural range of motion. Poor hinge design creates friction and limits mobility.
Patellar support features stabilize your kneecap position. Open patella designs reduce pressure on the kneecap. Closed designs offer more comprehensive compression around this area.
Comfort Features for Extended Wear
Padded edges prevent chafing and pressure sores during walking. Strategic padding placement protects sensitive areas around your knee. Comfort features encourage consistent use for better results.
Seamless construction eliminates irritation points against your skin. Flat-lock stitching prevents rubbing during movement. These details matter significantly during all-day wear.
Non-slip silicone grips keep the support in proper position. The brace should stay in place without constant adjustment. Secure positioning ensures consistent therapeutic benefits.
Anti-Migration Technology
Quality knee supports incorporate multiple features to prevent slipping. Silicone bands grip your skin gently but effectively. These strips are strategically placed at the top and bottom edges.
Tapered designs conform to your leg’s natural shape. The anatomical fit reduces movement during activities. Your support stays positioned correctly throughout your walking routine.
Properly fitted supports require minimal readjustment during wear. Frequent repositioning indicates poor fit or inadequate grip. Invest in products with proven anti-slip technology.
Ease of Application and Removal
Simple designs encourage regular use for consistent therapy. Complicated closures frustrate users and reduce compliance. Look for intuitive systems you can manage independently.
Pull-on sleeves work well for people with good hand strength. Wraparound designs suit those with limited dexterity or flexibility. Consider your physical capabilities when selecting a style.
Quick-release mechanisms allow easy removal when needed. You should be able to apply and remove your support without assistance. Independence in management promotes consistent use.
Compare Top-Rated Knee Supports for Walking
Access our comprehensive comparison tool featuring the highest-rated knee braces for osteoarthritis. Filter by support level, material preferences, and price range to find your ideal match.
Top Recommendations: Best Knee Support for Osteoarthritis While Walking
These carefully selected knee supports represent the best options for arthritis management. Each recommendation addresses specific needs and severity levels. Your optimal choice depends on individual circumstances and preferences.
Best Overall: Medical-Grade Unloader Knee Brace
This premium unloader brace specifically targets unicompartmental osteoarthritis. The three-point pressure system shifts weight from damaged cartilage. Users report significant pain reduction during walking activities.
Adjustable hinge settings allow customization for your specific needs. The brace accommodates various degrees of knee alignment correction. This flexibility ensures optimal pressure redistribution for maximum relief.
Lightweight aircraft-grade aluminum provides strength without bulk. The streamlined design fits comfortably under most clothing. You can wear this brace throughout your daily activities.
Key Features
- Medial or lateral compartment offloading
- Adjustable correction angles (0-6 degrees)
- Breathable moisture-wicking liner
- Dual-pivot hinge system
- Anti-migration technology
- Hypoallergenic materials
Best For
Moderate to severe single-compartment osteoarthritis affecting medial or lateral knee areas. Ideal for active individuals seeking maximum pain relief during walking and daily activities.
“After three months of struggling with severe medial knee pain, this unloader brace changed my life. I can now walk my dog for 30 minutes without limping. The pain reduction is remarkable.”
Best Value: Compression Knee Sleeve with Gel Pad
This affordable knee sleeve delivers excellent compression therapy for mild to moderate arthritis. The integrated gel pad cushions your patella during movement. Graduated compression reduces swelling while improving circulation.
Medical-grade compression fabric provides 20-30 mmHg pressure. This therapeutic range effectively manages inflammation and pain. The fabric maintains compression strength through repeated washing.
The sleeve design allows easy application without assistance. Simply pull it on like a sock for instant support. The seamless construction prevents irritation during extended wear.
Advantages
- Exceptional value for price point
- Lightweight and breathable design
- Machine washable for easy care
- Discreet under clothing
- Provides all-day comfort
- Gel pad protects kneecap
Limitations
- Limited support for severe cases
- May roll slightly during vigorous activity
- Sizing requires careful measurement
- Less durable than rigid braces
Ideal Candidates
Perfect for individuals with mild to moderate osteoarthritis seeking affordable daily support. Excellent choice for preventive care and early-stage arthritis management during walking activities.
Best for Stability: Hinged Knee Brace with Dual Support
This robust brace combines bilateral hinges with adjustable compression straps. The dual-hinge design provides exceptional lateral stability during walking. Metal stays prevent unwanted side-to-side movement that stresses damaged cartilage.
Open patella design reduces pressure on your kneecap. The cutout allows the patella to track naturally during movement. This feature addresses both arthritis pain and patellofemoral issues simultaneously.
Four adjustable straps allow precise compression control. Modify tightness at different points for customized support. The wraparound design facilitates easy application and removal.
Technical Specifications
- Bilateral polycentric hinges
- Range of motion: 0-120 degrees
- Four-way adjustable straps
- Open patella stabilizer ring
- Removable medial/lateral stays
- Neoprene blend with perforations
- Weight: 14 oz
Performance Highlights
Exceptional performance for individuals with knee instability from arthritis. The combination of compression and rigid support addresses multiple symptoms. Users report improved confidence during walking and standing activities.
Professional Insight: This brace works particularly well for osteoarthritis patients with concurrent ligament laxity. The bilateral support compensates for weakened stabilizing structures around the knee joint.
Best for Active Lifestyles: Sport-Specific Arthritis Knee Brace
Designed for arthritis patients who refuse to give up active pursuits. This brace balances support with freedom of movement. The low-profile design suits running, hiking, and recreational sports.
Advanced moisture-wicking technology keeps your skin dry during exercise. Mesh panels provide strategic ventilation at high-heat areas. Antimicrobial treatment prevents odor during intense activities.
Flexible composite stays offer support without the weight of metal. These materials bend with your knee during dynamic movements. You maintain natural biomechanics while receiving therapeutic benefits.
Walking & Hiking
Excellent shock absorption for trail walking. Provides stability on uneven terrain. Compression reduces fatigue during long distances.
Light Running
Supports jogging and run-walk intervals. Reduces impact stress on damaged cartilage. Improves proprioception during running.
Cycling
Low-profile fit works under cycling gear. Maintains proper patellar tracking. Provides compression without restricting pedaling.
Who Should Choose This Brace
Perfect for active individuals with mild to moderate arthritis who want to maintain their fitness routines. Not recommended for severe instability or advanced osteoarthritis requiring maximum support.
Best for Night Use: Therapeutic Warming Knee Support
This specialized sleeve provides therapeutic heat during rest periods. The thermal fabric retains body heat effectively overnight. Many users experience reduced morning stiffness after consistent use.
The gentle compression promotes circulation while you sleep. Better blood flow supports the healing process during rest. This therapy complements daytime support strategies.
Ultra-soft interior lining prevents skin irritation during extended wear. The comfortable design allows natural sleep positions. You won’t wake up from brace discomfort.
Benefits of Heat Therapy
Heat increases blood flow to your knee joint tissues. Enhanced circulation delivers nutrients essential for cartilage health. Warmth also relaxes muscles surrounding the joint.
The therapeutic temperature range reduces pain signals. Your brain processes fewer discomfort messages during rest. This effect contributes to better sleep quality.
Consistent overnight use shows cumulative benefits over time. Many users notice improved morning mobility after several weeks. The therapy supports your body’s natural healing process.
Usage Guidelines
Apply the sleeve before bed for optimal results. Ensure proper positioning over your entire knee joint. The support should feel snug but not restrictive.
Combine with your daytime support routine for comprehensive care. This layered approach addresses symptoms around the clock. Consistent use produces the best outcomes.
Monitor your skin for any irritation signs. Remove the sleeve if you experience discomfort or excessive heat. Most users tolerate overnight wear without issues.
Get Personalized Knee Support Recommendations
Speak with our certified orthopedic specialists who understand osteoarthritis challenges. Receive expert guidance on selecting the perfect knee support for your specific walking needs and arthritis severity.
How to Choose Knee Support Based on Osteoarthritis Severity
Your osteoarthritis severity determines appropriate support requirements. Understanding your condition stage guides effective product selection. The right match between severity and support maximizes pain relief.
Mild Osteoarthritis Support Needs
Early-stage arthritis presents with occasional pain and minimal swelling. You experience discomfort primarily after extended activity. Joint damage remains relatively limited at this stage.
Compression sleeves work effectively for mild cases. The gentle pressure reduces inflammation and provides proprioceptive feedback. This awareness helps you move more carefully.
Preventive support slows progression to more severe stages. Consistent use during activities protects vulnerable cartilage. Early intervention yields the best long-term results.
Mild Stage Characteristics
- Pain occurs occasionally, usually after activity
- Minor swelling that resolves with rest
- Slight stiffness in the morning
- Full range of motion mostly preserved
- X-rays show minimal joint space narrowing
- Daily activities remain largely unaffected
Recommended Support Options
- Compression knee sleeves with 15-20 mmHg pressure
- Lightweight elastic supports for activity
- Patellar stabilizing bands for specific pain
- Thermal sleeves for morning stiffness
Moderate Osteoarthritis Support Requirements
Moderate arthritis causes more frequent pain and noticeable swelling. Walking becomes uncomfortable even during short distances. Your knee may feel unstable on uneven surfaces.
Hybrid designs combining compression with structural support work best. Look for braces with some rigid elements and adjustable straps. These features address multiple symptoms simultaneously.
Increased support helps maintain your activity level despite progression. Proper bracing prevents further damage from instability. You can continue walking with appropriate assistance.
Moderate Stage Indicators
- Regular pain during and after walking
- Persistent swelling requiring management
- Morning stiffness lasting 30+ minutes
- Grinding or clicking sensations
- Some limitation in range of motion
- Difficulty with stairs and inclines
- X-rays show clear joint space reduction
Optimal Support Features
- Adjustable compression levels
- Removable stays for customization
- Open or closed patella designs
- Side stabilizers for lateral support
- Moisture-wicking materials
- Easy-adjust strap systems
Effective Choices
- Wraparound braces with stays
- Hinged supports with compression
- Dual-strap stabilizing braces
- Moderate-duty sleeve with gel pads
- Hybrid compression-rigid designs
Less Effective
- Simple elastic sleeves alone
- Single-strap supports
- Very lightweight designs
- Bands without additional support
- Non-adjustable compression
Severe Osteoarthritis Support Solutions
Advanced arthritis causes constant pain limiting daily function. Significant joint damage appears on imaging studies. Walking short distances becomes extremely challenging.
Maximum support braces become necessary at this stage. Unloader braces or heavy-duty hinged designs provide essential assistance. These devices significantly reduce pain during necessary movement.
Medical consultation becomes critical for severe cases. Healthcare professionals may recommend custom-fitted braces. Prescription devices offer superior fit and effectiveness.
Medical Attention Required: Severe osteoarthritis may require interventions beyond supportive bracing. Consult with orthopedic specialists about comprehensive treatment plans including possible surgical options.
Severe Stage Characteristics
- Constant or near-constant pain at rest and during activity
- Significant swelling and inflammation
- Severe morning stiffness lasting hours
- Marked range of motion limitations
- Visible joint deformity or malalignment
- Major difficulty with weight-bearing activities
- X-rays show extensive cartilage loss and bone changes
Essential Support Specifications
- Maximum stability with bilateral hinges
- Unloading capabilities for compartment relief
- Custom-fitting options preferred
- Professional consultation recommended
- Prescription-grade materials and construction
- Multiple adjustment mechanisms
- Superior durability for long-term use
Progression Monitoring and Adjustment
Osteoarthritis severity can change over time requiring support modifications. Regular assessment ensures your brace continues meeting your needs. Adjust your support strategy as symptoms evolve.
Track your pain levels and functional limitations weekly. Notice changes in swelling patterns and stiffness duration. These observations guide timely support upgrades.
Work with healthcare providers to monitor disease progression. Professional imaging reveals changes not apparent through symptoms alone. This information informs optimal support selection.
| Severity Level | Primary Symptoms | Recommended Support Type | Key Features Needed |
| Mild | Occasional pain, minimal swelling, full motion | Compression sleeve or light elastic support | 15-20 mmHg compression, breathable material |
| Moderate | Frequent pain, regular swelling, some limitation | Hybrid brace with stays or hinged support | Adjustable compression, lateral stability, open patella |
| Severe | Constant pain, significant swelling, major limitation | Unloader brace or heavy-duty hinged brace | Maximum stability, offloading capability, custom fit |
| Post-Surgical | Recovery phase pain, healing tissue, restricted motion | ROM-limiting brace or post-op specific design | Controlled range of motion, superior stability, medical-grade |
Proper Fit and Usage Tips for Maximum Effectiveness
Correct fitting determines your knee support effectiveness and comfort. An improperly fitted brace provides inadequate relief and may cause problems. Learning proper application techniques ensures optimal benefits.
Measuring Your Knee for Correct Sizing
Accurate measurements prevent ordering the wrong size support. Most manufacturers require specific circumference measurements. Take measurements while standing with your leg straight.
Measure around your knee joint at the kneecap center. Record this measurement in inches or centimeters. Some braces also require thigh and calf circumferences.
Measure at the recommended time of day for accuracy. Morning measurements differ from evening due to swelling. Follow manufacturer guidelines for measurement timing.
Measurement Instructions
- Stand upright with weight evenly distributed on both legs
- Keep your knee straight but not locked
- Use a flexible measuring tape for accuracy
- Measure directly on skin, not over clothing
- Take measurements at specified locations:
- Knee center (over kneecap)
- 4 inches above kneecap for thigh
- 4 inches below kneecap for calf
- Record all measurements before comparing to size charts
- Measure both knees even if only one needs support
Pro Tip: If your measurements fall between sizes, consider your symptoms. Choose the smaller size for mild support needs and the larger size for more severe swelling issues.
Application Techniques for Different Support Types
Each knee support style requires specific application methods. Proper technique ensures the device functions as designed. Incorrect application reduces effectiveness and comfort.
Applying Pull-On Sleeves
Turn the sleeve inside out to the halfway point. Step into the sleeve with your foot, positioning it around your ankle. Pull the sleeve up your leg gradually while keeping it centered.
Avoid bunching the fabric as you pull upward. Smooth out any wrinkles that form during application. Position the sleeve so reinforcement elements align properly with your knee.
The top and bottom edges should lie flat against your skin. Silicone grips should contact your skin without rolling. Adjust positioning until the support feels evenly distributed.
Applying Wraparound Braces
Open all straps completely before application. Position the brace behind your knee with hinges aligned to joint line. Wrap the brace around your leg, overlapping edges as designed.
Secure the primary strap first to anchor the brace. Work from bottom to top when fastening remaining straps. This sequence prevents the brace from sliding during application.
Adjust each strap to achieve appropriate compression. The brace should feel snug but not restrict circulation. You should insert two fingers comfortably under any strap.
Strap Tightening Guidelines
- Bottom straps: Snug to prevent downward migration
- Middle straps: Moderate compression for support
- Top straps: Secure but allow muscle movement
- Never overtighten any single strap
- Check circulation after application
- Readjust as swelling changes throughout day
Wearing Duration and Schedule
Your wearing schedule depends on support type and symptom severity. Build tolerance gradually when starting new support. Extended initial wear can cause skin irritation or discomfort.
Start with 1-2 hours of wear during light activity. Increase duration by 30 minutes daily as comfort allows. Most users reach full-day wear within one to two weeks.
Remove your support periodically to check skin condition. Look for redness, irritation, or excessive moisture. Brief removal periods allow your skin to breathe.
Daytime Wearing Schedule
Wear your support during all walking and standing activities. Apply it before getting out of bed if morning stiffness occurs. Keep it on during errands, work, and exercise.
Remove the support during extended sitting periods if comfortable. Your knee experiences less stress while seated. However, keep it on if sitting causes pain.
Plan to wear support for 6-12 hours daily for moderate arthritis. Severe cases may require longer wearing times. Listen to your body and adjust accordingly.
Nighttime Considerations
Most rigid braces should be removed for sleeping. They restrict natural movement during rest. Sleeping with hard structures can cause discomfort.
Compression sleeves designed for night use offer an alternative. These provide therapeutic warmth and gentle support. They address nighttime pain without limiting sleep positions.
Consult healthcare providers about overnight wear recommendations. Post-surgical situations may require continuous use. Follow professional guidance for your specific case.
Maintenance and Care Instructions
Regular cleaning extends your knee support lifespan and prevents odor. Proper maintenance also protects your skin from irritation. Follow manufacturer care instructions for best results.
Hand washing works best for most knee supports. Use mild detergent and lukewarm water for cleaning. Harsh chemicals damage elastic fibers and support materials.
Air dry your support completely between uses. Avoid direct heat sources like radiators or dryers. High temperatures degrade elastic properties and can warp rigid components.
Cleaning and Maintenance Checklist
- Hand wash after every 2-3 uses or daily with heavy perspiration
- Use mild, fragrance-free detergent only
- Rinse thoroughly to remove all soap residue
- Gently squeeze out excess water without wringing
- Air dry completely before storing or reusing
- Inspect hinges and stays regularly for wear
- Check straps and closures for secure attachment
- Replace supports showing significant wear or damage
- Store in cool, dry location away from direct sunlight
Common Fitting Problems and Solutions
Even properly sized supports can present fitting challenges. Identifying and resolving these issues improves comfort and effectiveness. Most problems have simple solutions.
| Problem | Possible Cause | Solution |
| Brace slides down during walking | Insufficient top grip or too large | Tighten top straps, check sizing, ensure silicone grips contact skin |
| Excessive pressure behind knee | Incorrect positioning or too tight | Reposition brace centered on knee, loosen middle straps slightly |
| Numbness or tingling | Straps too tight restricting circulation | Loosen all straps immediately, check for proper fit, consult specialist |
| Skin irritation or rash | Material sensitivity or moisture buildup | Try hypoallergenic liner, ensure support is dry, reduce wearing time |
| Support feels bulky under clothing | Design incompatible with clothing style | Consider lower-profile design, wear looser pants, try sleeve alternative |
| Hinges dig into skin | Misalignment with natural knee joint | Reposition to align hinges with knee joint line, add padding if needed |
Signs Your Support Needs Replacement
Knee supports don’t last forever despite proper care. Worn components lose effectiveness and may cause problems. Recognize replacement indicators for continued benefit.
Elastic materials stretch out over time reducing compression. If your support feels loose despite proper fastening, replacement time approaches. Lost compression means lost therapeutic benefit.
Visible damage to hinges, stays, or fabric compromises function. Frayed straps won’t hold securely. Bent or broken rigid elements fail to provide intended support.
Replace When You Notice:
- Persistent sliding despite proper adjustment
- Visible fabric tears or excessive pilling
- Broken or bent hinges and stays
- Velcro that no longer grips securely
- Elastic that remains stretched when removed
- Persistent odor despite thorough cleaning
- Increased pain during use
Typical Replacement Timeline:
- Compression sleeves: 3-6 months with daily use
- Wraparound braces: 6-12 months
- Hinged braces: 12-24 months
- Premium unloader braces: 2-3 years
- Earlier replacement needed with heavy use
- Quality products last longer than budget options
Download Free Knee Support Fitting Guide
Get our comprehensive PDF guide with detailed measurement instructions, fitting tips, and troubleshooting advice. Includes printable measurement charts and visual application guides for all support types.
Additional Management Strategies for Osteoarthritis While Walking
Knee support works best as part of comprehensive arthritis management. Combining multiple strategies provides superior results. Your holistic approach addresses various aspects of the condition.
Strengthening Exercises for Knee Support
Strong muscles around your knee joint provide natural support. Regular strengthening reduces stress on damaged cartilage. Exercise complements mechanical bracing effectively.
Quadriceps muscles on your thigh front are particularly important. These muscles control knee movement and absorb shock. Hamstring strength balances quad function.
Low-impact exercises protect your joint during strengthening. Avoid high-impact activities that increase pain. Consistency matters more than intensity for arthritis exercise.
Straight Leg Raises
Lie on your back with one knee bent. Keep the other leg straight and lift it to bent knee height. Hold for 5 seconds and lower slowly.
- Strengthens quadriceps without knee stress
- Perform 10-15 repetitions per leg
- Complete 2-3 sets daily
Wall Squats
Stand with your back against a wall. Slide down into a partial squat position. Hold for 10 seconds then return to standing.
- Builds quad and glute strength
- Start with shallow squats
- Progress depth as strength improves
Hamstring Curls
Stand holding a chair for balance. Bend one knee bringing heel toward buttock. Lower slowly and repeat.
- Strengthens back of thigh
- Balances quadriceps development
- Add ankle weights for progression
Exercise Guidelines for Arthritis
Start any new exercise program gradually and gently. Pain during exercise indicates too much intensity. Discomfort should decrease, not increase, with regular activity.
Warm up before strengthening exercises with light movement. Walking slowly or gentle cycling prepares your joints. Cool down afterward with stretching.
Work with physical therapists for personalized exercise programs. Professional guidance ensures proper form and appropriate progression. Incorrect technique can worsen symptoms.
Exercise Timing: Perform strengthening exercises when pain levels are lowest. Many people find morning or early afternoon optimal. Avoid exercising during symptom flares.
Proper Footwear for Walking with Osteoarthritis
Appropriate shoes significantly impact knee stress during walking. Good footwear absorbs shock and promotes proper alignment. Your shoe choice complements knee support benefits.
Look for shoes with excellent cushioning in the heel and forefoot. Extra padding reduces impact forces transmitted to your knee. This shock absorption decreases pain during walking.
Stability features prevent excessive foot motion that stresses knees. Firm heel counters and supportive midsoles control pronation. Proper foot control improves overall leg alignment.
Essential Shoe Features
- Thick, shock-absorbing midsole
- Firm heel counter for stability
- Adequate toe box room
- Lightweight construction
- Flexible forefoot for natural roll
- Removable insole for orthotics
- Non-slip outsole for safety
- Low to moderate heel height
Shoes to Avoid
- High heels that increase knee pressure
- Completely flat shoes without arch support
- Worn-out shoes with compressed cushioning
- Narrow toe boxes that affect gait
- Heavy boots that fatigue muscles
- Flip-flops lacking any support
- Fashion shoes prioritizing style over function
Weight Management for Reduced Knee Stress
Excess body weight dramatically increases knee joint pressure. Losing weight reduces pain and slows arthritis progression. Even modest weight loss yields significant benefits.
Each pound of body weight generates approximately four pounds of knee pressure. Losing 10 pounds removes 40 pounds of stress per step. This reduction provides substantial relief during walking.
Combine healthy eating with appropriate physical activity. Focus on nutrient-dense foods supporting joint health. Avoid crash diets that cause muscle loss.
Joint-Friendly Nutrition Guidelines
Foods to Emphasize
- Fatty fish rich in omega-3s
- Colorful fruits and vegetables
- Nuts and seeds
- Olive oil and healthy fats
- Whole grains
- Lean proteins
- Green tea
Foods to Limit
- Processed foods with additives
- Refined sugars and carbohydrates
- Excessive red meat
- Trans fats and fried foods
- High-sodium items
- Alcohol in excess
Walking Technique Modifications
Adjusting your walking pattern reduces knee joint stress. Small technique changes make significant differences. Proper mechanics complement your knee support.
Shorten your stride length to decrease impact forces. Longer steps increase pressure on your knee during landing. Smaller steps distribute forces more evenly.
Maintain a steady, moderate pace during walking. Rushing increases impact and muscle fatigue. Consistent speed allows better movement control.
Beneficial Techniques
- Shorter, controlled strides
- Upright posture with engaged core
- Heel-to-toe rolling motion
- Relaxed shoulders and arms
- Steady, moderate pace
- Level, smooth surfaces when possible
- Walking poles for additional support
Harmful Habits
- Overstriding with long steps
- Forward-leaning posture
- Hard heel strikes
- Tense muscles and locked joints
- Rushing or irregular pace
- Walking on uneven terrain unnecessarily
- Ignoring pain signals
Complementary Therapies and Treatments
Various treatments work alongside knee support for comprehensive care. Multiple approaches address different aspects of osteoarthritis. Discuss options with healthcare providers.
Physical Therapy
Professional physical therapy optimizes your recovery and function. Therapists design personalized exercise programs for your needs. Manual therapy techniques reduce pain and improve mobility.
Regular physical therapy sessions accelerate your healing process. Therapists monitor progress and adjust treatments accordingly. They teach proper body mechanics for daily activities.
Heat and Cold Therapy
Temperature therapy provides pain relief and reduces inflammation. Apply ice after activities to control swelling. Use heat before movement to improve flexibility.
Ice therapy constricts blood vessels reducing inflammation and pain. Apply for 15-20 minutes several times daily. Use a barrier between ice and skin.
Heat increases circulation promoting healing and relaxation. Warm compresses or heating pads soothe stiff joints. Apply heat for 15-20 minutes before activity.
When to Use Ice
- After walking or physical activity
- During acute pain flares
- When swelling increases
- After accidental injury
- For sharp, intense pain
When to Use Heat
- Before morning activity
- For muscle tension and stiffness
- During chronic, dull pain
- Before stretching exercises
- When joints feel tight
Over-the-Counter Pain Management
Appropriate medications complement physical treatments effectively. Nonsteroidal anti-inflammatory drugs reduce pain and swelling. Acetaminophen provides pain relief without anti-inflammatory effects.
Topical pain relievers offer localized relief without systemic effects. Creams and gels containing menthol or capsaicin ease discomfort. Apply directly to your knee before walking.
Always consult healthcare providers before starting new medications. Some drugs interact with existing prescriptions. Professional guidance ensures safe, effective use.
Medication Safety: Never exceed recommended dosages of over-the-counter medications. Long-term NSAID use can cause serious side effects. Discuss ongoing pain management with your doctor.
Rest and Recovery Balance
Appropriate rest prevents overuse while maintaining function. Balance activity with adequate recovery time. Too much rest weakens muscles; too much activity increases damage.
Listen to your body’s signals during and after walking. Increased pain lasting more than two hours indicates excessive activity. Adjust your routine to prevent symptom escalation.
Plan rest days into your weekly schedule. Recovery allows tissue repair and inflammation reduction. Active recovery with gentle movement often works better than complete rest.
Create Your Personalized Arthritis Management Plan
Work with our specialized team to develop a comprehensive treatment strategy combining knee support, exercise, and lifestyle modifications. Schedule a free consultation to start your journey toward better mobility and reduced pain.
Frequently Asked Questions About Knee Support for Osteoarthritis
Can I wear a knee brace all day for osteoarthritis?
Most knee braces designed for osteoarthritis are safe for all-day wear. Build up wearing time gradually over 1-2 weeks. Remove your brace periodically to check skin condition and allow it to breathe.
Compression sleeves typically tolerate extended wear better than rigid braces. Heavy-duty hinged braces may feel uncomfortable during prolonged sitting. Remove rigid supports during extended rest periods unless instructed otherwise by healthcare providers.
Monitor your skin for redness, irritation, or excessive moisture. These signs indicate you need breaks from wearing your support. Proper fit minimizes complications during extended use.
How tight should my knee support be?
Your knee support should feel snug but not restrict circulation. You should be able to insert two fingers comfortably under any strap or edge. The support should stay in place during movement without constant adjustment.
Proper compression feels like a firm handshake around your knee. Too loose provides inadequate support and slides during activity. Too tight causes numbness, tingling, or skin color changes.
Adjust tightness as swelling fluctuates throughout the day. Morning application may require looser settings than afternoon. Check fit regularly and modify as needed for comfort and effectiveness.
Will a knee brace cure my osteoarthritis?
Knee braces do not cure osteoarthritis as the condition involves irreversible cartilage damage. However, appropriate support significantly reduces pain and improves function. Braces may slow progression by reducing harmful stress on damaged areas.
Think of knee support as a management tool rather than a cure. The brace helps you maintain activity levels and quality of life. Combined with other treatments, supports optimize your long-term outcomes.
Some research suggests unloader braces may preserve remaining cartilage. By redistributing pressure away from damaged areas, these devices potentially delay further deterioration. Consistent use provides the best protective benefits.
Can I exercise while wearing a knee brace?
Yes, most knee braces are designed to support you during physical activity. Exercise while wearing appropriate support often reduces pain and improves confidence. Choose braces specifically rated for your intended activities.
Low-impact exercises like walking, swimming, and cycling work well with most supports. High-impact activities may require specialized sport braces. Some compression sleeves are designed specifically for running or athletics.
Ensure your brace stays properly positioned during exercise. Excessive movement indicates poor fit or inadequate support for that activity. You may need different supports for various exercise types.
How do I know if I need an unloader brace versus a regular support?
Unloader braces specifically address unicompartmental osteoarthritis affecting only one side of your knee. X-rays or MRI imaging confirm if damage is isolated to medial or lateral compartments. These specialized braces work best for single-sided arthritis.
Regular supports provide general compression and stability for diffuse arthritis. If both sides of your knee joint show damage, standard braces are more appropriate. Unloader braces won’t help with patellofemoral arthritis affecting the kneecap area.
Consult with orthopedic specialists before investing in unloader braces. These devices are expensive and require proper fitting. Professional assessment ensures you select the most effective option for your specific condition.
Should I wear my knee support to bed?
Most rigid knee braces should be removed for sleeping unless specifically instructed otherwise. Hard structures restrict natural movement during rest and can disrupt sleep quality. Your knee needs freedom to find comfortable positions overnight.
Compression sleeves designed for nighttime use offer an alternative for overnight support. These provide therapeutic warmth and gentle compression without restricting movement. Many users experience reduced morning stiffness with overnight sleeves.
Post-surgical situations may require continuous brace wear including during sleep. Always follow your surgeon’s specific instructions. Nighttime immobilization serves specific purposes during the healing process.
How often should I replace my knee support?
Compression sleeves typically need replacement every 3-6 months with daily use. The elastic fibers lose compression strength over time. Replace sooner if the sleeve feels loose or shows visible wear.
Wraparound braces last 6-12 months depending on usage intensity. Hinged braces with quality construction may last 12-24 months. Premium unloader braces can remain effective for 2-3 years with proper care.
Replace your support immediately if you notice broken hinges, torn fabric, or failed closures. Damaged supports don’t provide intended benefits and may cause injury. Proper maintenance extends lifespan but all supports eventually wear out.
Can knee supports prevent osteoarthritis from getting worse?
Appropriate knee support may slow osteoarthritis progression by reducing harmful stress. Unloader braces show promise for preserving cartilage in affected compartments. Consistent use during activities provides the best protective effects.
Supports work best as part of comprehensive management including exercise and weight control. No single intervention stops arthritis progression completely. Multiple strategies together optimize your long-term outcomes.
Early intervention with appropriate support yields better results. Starting support when arthritis is mild may preserve function longer. However, even advanced cases benefit from proper bracing for symptom management.
Do I need a prescription for a knee brace?
Over-the-counter knee supports don’t require prescriptions for purchase. You can buy compression sleeves and basic braces directly. These options work well for mild to moderate arthritis management.
Specialized unloader braces often require prescriptions for insurance coverage. Custom-fitted devices need professional assessment and measurement. Prescription braces typically cost more but offer superior effectiveness for specific conditions.
Some insurance plans cover knee supports with proper medical documentation. Check your benefits and requirements. A prescription may be necessary for reimbursement even for non-custom braces.
What’s the difference between a knee brace and a knee sleeve?
Knee braces feature rigid or semi-rigid structures providing maximum support and stability. They include components like hinges, stays, or frames. Braces restrict certain movements while allowing controlled motion.
Knee sleeves are elastic garments providing compression without rigid elements. They offer flexibility and comfort for all-day wear. Sleeves improve circulation and proprioception rather than limiting movement.
Choose braces for instability or severe pain requiring structural support. Select sleeves for mild symptoms, swelling management, or preventive care. Some people use both types for different activities or stages of their condition.
Taking the Next Step Toward Better Mobility
Finding the best knee support for osteoarthritis transforms your walking experience. The right support reduces pain and improves your mobility. You can maintain an active lifestyle despite arthritis challenges.
This comprehensive guide provided essential information for informed decisions. You learned about different support types and their specific benefits. Understanding features and proper fitting ensures optimal results.
Remember that knee support works best within a holistic management approach. Combine mechanical support with exercise, proper footwear, and healthy lifestyle choices. This multi-faceted strategy addresses various aspects of osteoarthritis.
Your Action Plan
Start by assessing your current arthritis severity and symptoms. Identify which support type matches your specific needs. Consider consulting healthcare professionals for personalized recommendations.
Invest in quality products designed specifically for osteoarthritis management. Proper support represents an investment in your long-term mobility and comfort. Choose products from reputable manufacturers with proven effectiveness.
Commit to consistent use of your chosen knee support. Regular wear during walking activities provides cumulative benefits. Combine support with recommended exercises and lifestyle modifications.
Immediate Steps
- Measure your knee accurately for proper sizing
- Research products matching your severity level
- Read user reviews and ratings
- Consider trying different types if possible
- Schedule consultation with specialists if needed
- Start with gradual wearing schedule
Long-Term Commitment
- Maintain regular exercise routine
- Monitor and manage body weight
- Attend follow-up appointments
- Track symptom changes and improvements
- Adjust support as condition evolves
- Stay informed about new treatment options
Living Well with Osteoarthritis
Osteoarthritis doesn’t have to limit your enjoyment of walking. Proper support and comprehensive management restore function and reduce pain. Many people maintain active, fulfilling lives with appropriate interventions.
Your journey toward better mobility starts with informed choices. The knowledge gained from this guide empowers you to select optimal solutions. Take control of your arthritis management today.
Walking remains one of the best activities for joint health and overall wellness. Don’t let arthritis pain keep you sedentary. With the right knee support and management strategies, you can continue enjoying this beneficial activity.
Remember: Every person’s osteoarthritis experience is unique. What works perfectly for one individual may not suit another. Be patient in finding your optimal combination of support, treatment, and lifestyle modifications. Progress may be gradual, but consistent effort yields meaningful improvements in your quality of life.
Start Your Journey to Pain-Free Walking Today
Don’t let osteoarthritis knee pain control your life any longer. Our specialized team is ready to help you find the perfect knee support solution and develop a comprehensive management plan tailored to your unique needs.
Get Expert Guidance
Schedule a free consultation with our certified orthopedic specialists. We’ll assess your condition, discuss your goals, and recommend the best knee support options for your specific situation.
- Personalized product recommendations
- Professional fitting assistance
- Comprehensive management strategies
- Ongoing support and follow-up
Take the first step toward better mobility and reduced pain. Your journey to improved quality of life starts with the right knee support.