Knee joint replacement surgery is a complex procedure that aims to alleviate pain and improve mobility in individuals with severe knee joint conditions. This surgical intervention involves replacing damaged or worn-out parts of the knee joint with artificial components, allowing patients to regain function and quality of life. Understanding the anatomy of the knee joint, indications for surgery, surgical techniques, and rehabilitation process is crucial for both patients and healthcare professionals. In this article, we will explore key insights into knee joint replacement surgery, covering essential information for those considering or involved in the process.
Key Takeaways
- Understanding the anatomy of the knee joint is essential for comprehending the impact of knee joint conditions.
- Degenerative joint disease, rheumatoid arthritis, and post-traumatic arthritis are common indications for knee joint replacement surgery.
- Total knee replacement, partial knee replacement, and minimally invasive knee replacement are the primary surgical techniques for knee joint replacement.
- Rehabilitation after knee joint replacement involves physical therapy, home care, and adherence to an expected recovery timeline.
- Successful knee joint replacement surgery can significantly improve mobility and quality of life for individuals with severe knee joint conditions.
Anatomy of the Knee Joint

Structure of the Knee Joint
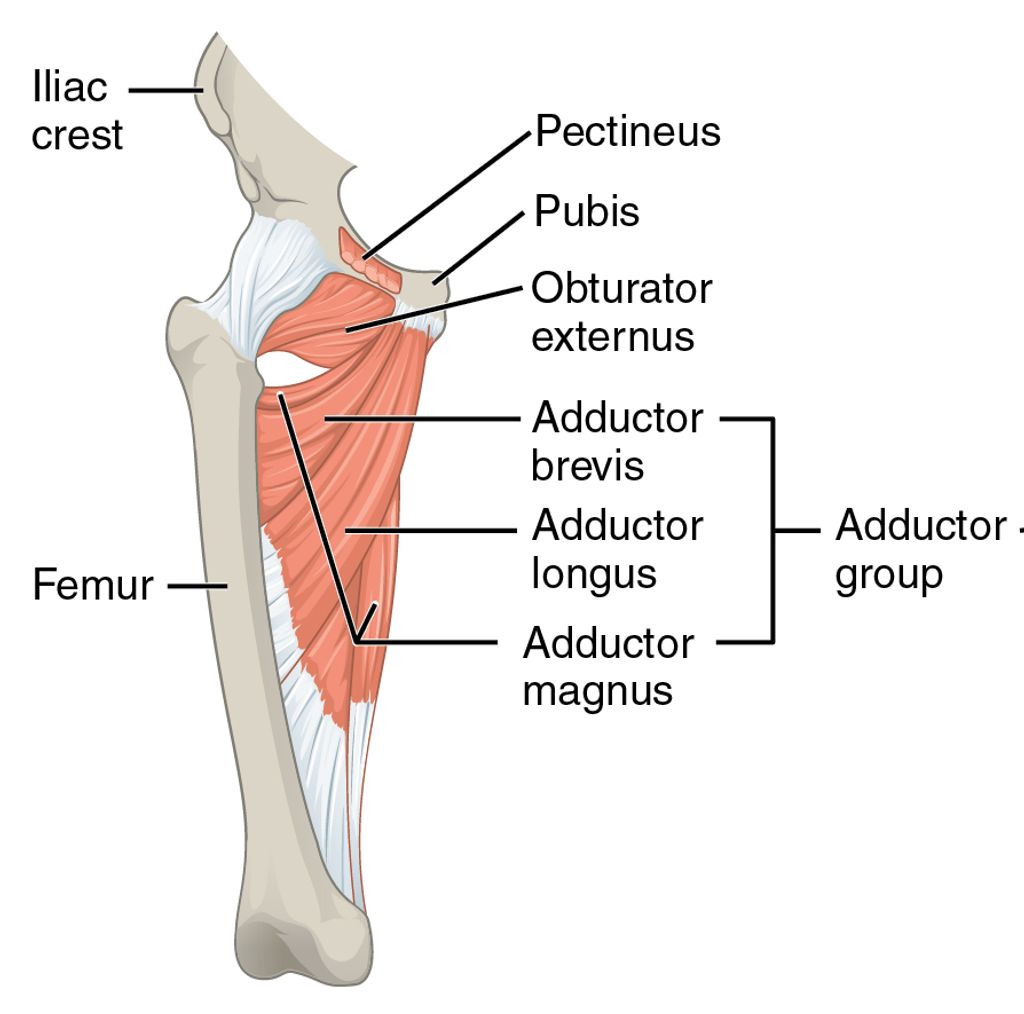
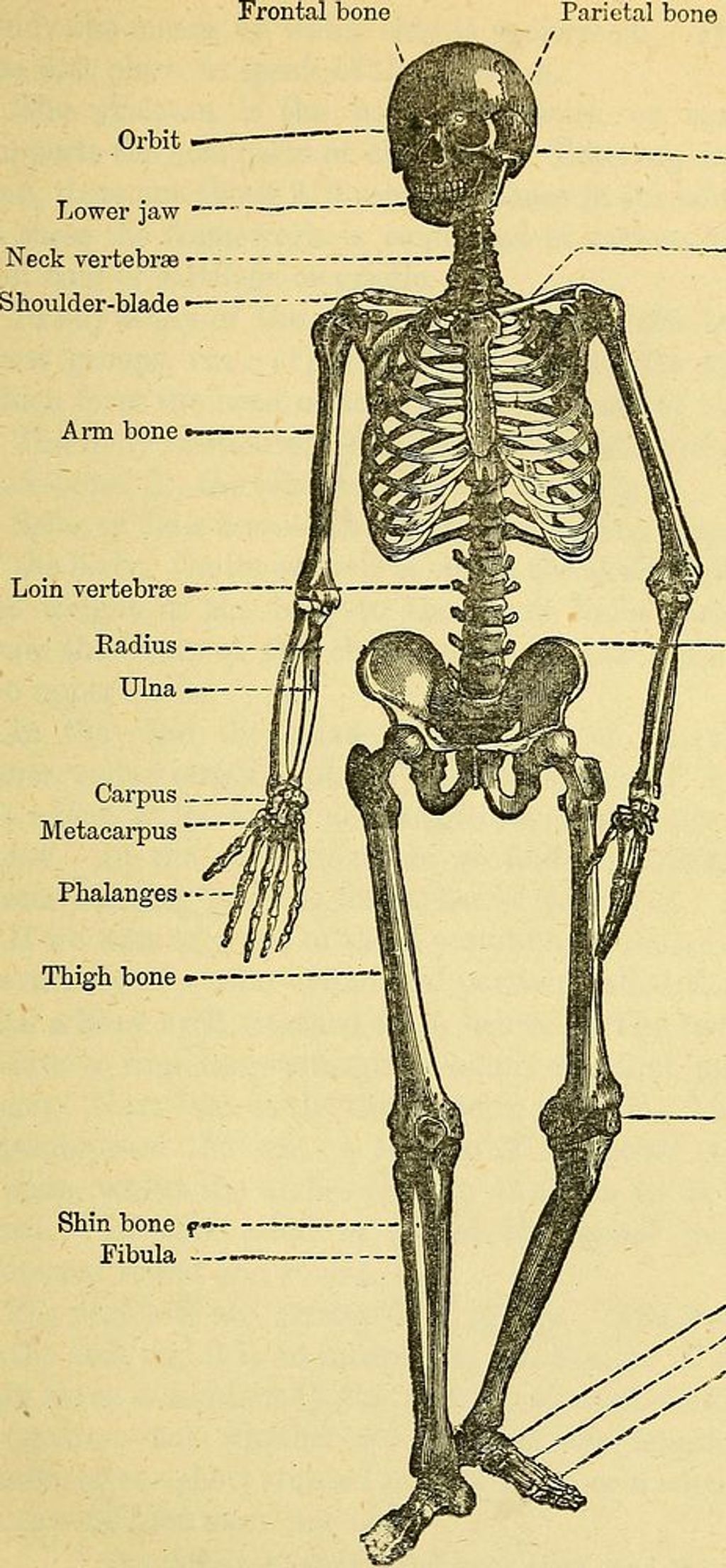
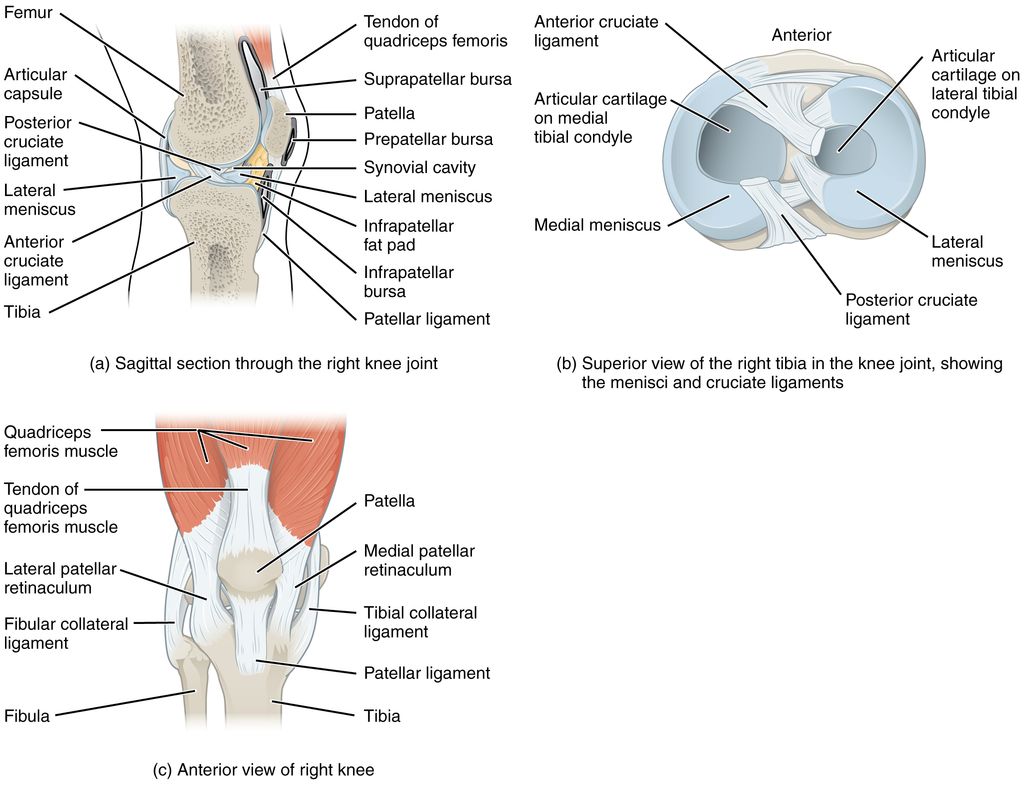
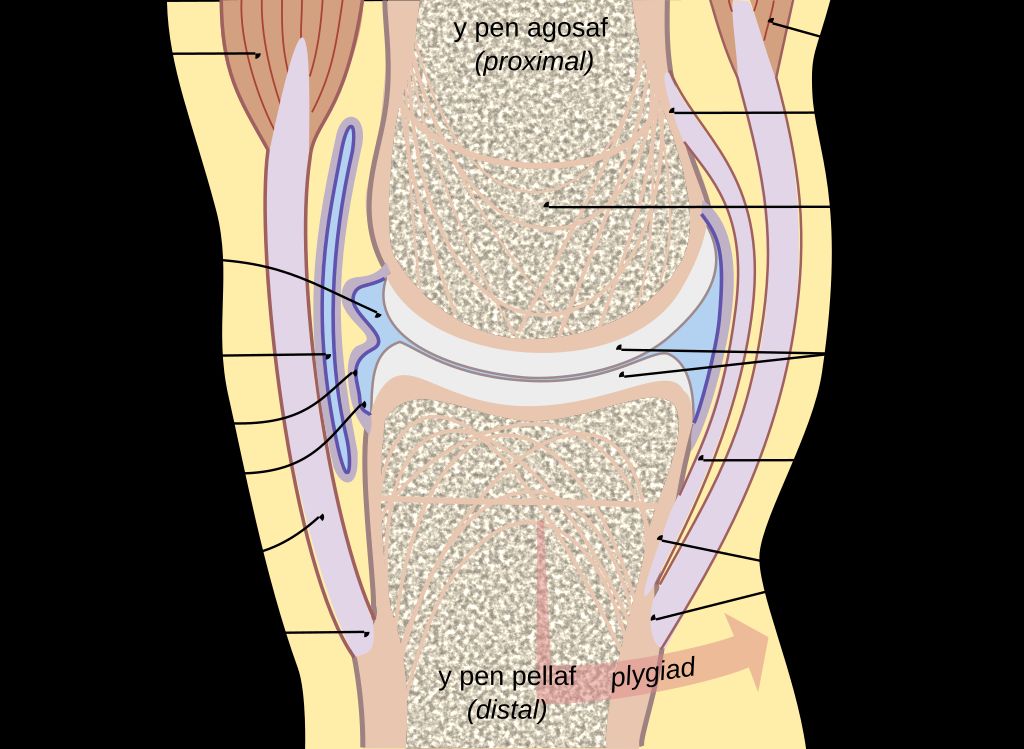
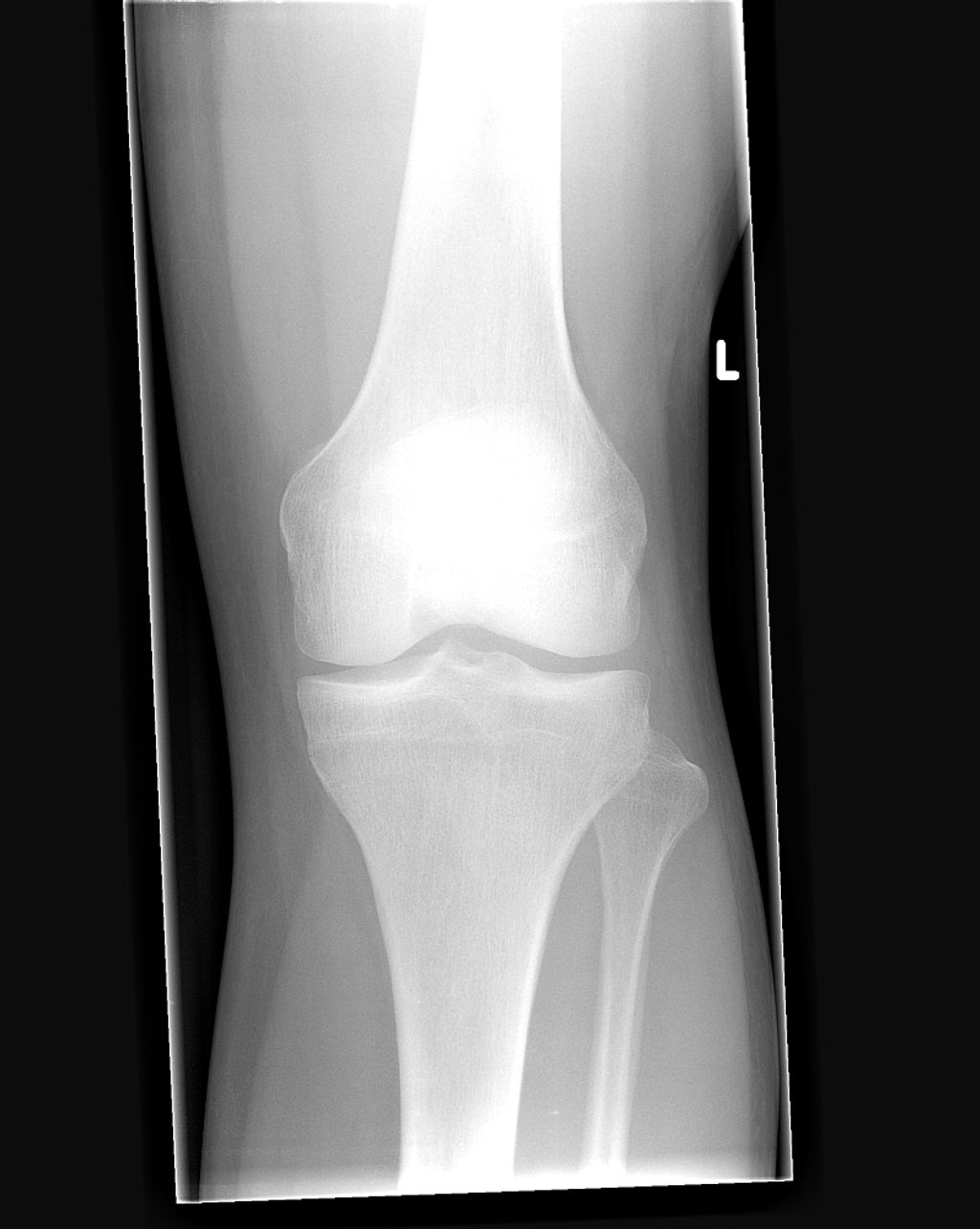
We often take for granted the complex engineering of our knee joints, which are pivotal for our mobility. The knee joint is primarily composed of three bones: the femur, tibia, and patella. These bones are connected by ligaments that provide stability and tendons that attach muscles to the bones, enabling movement.
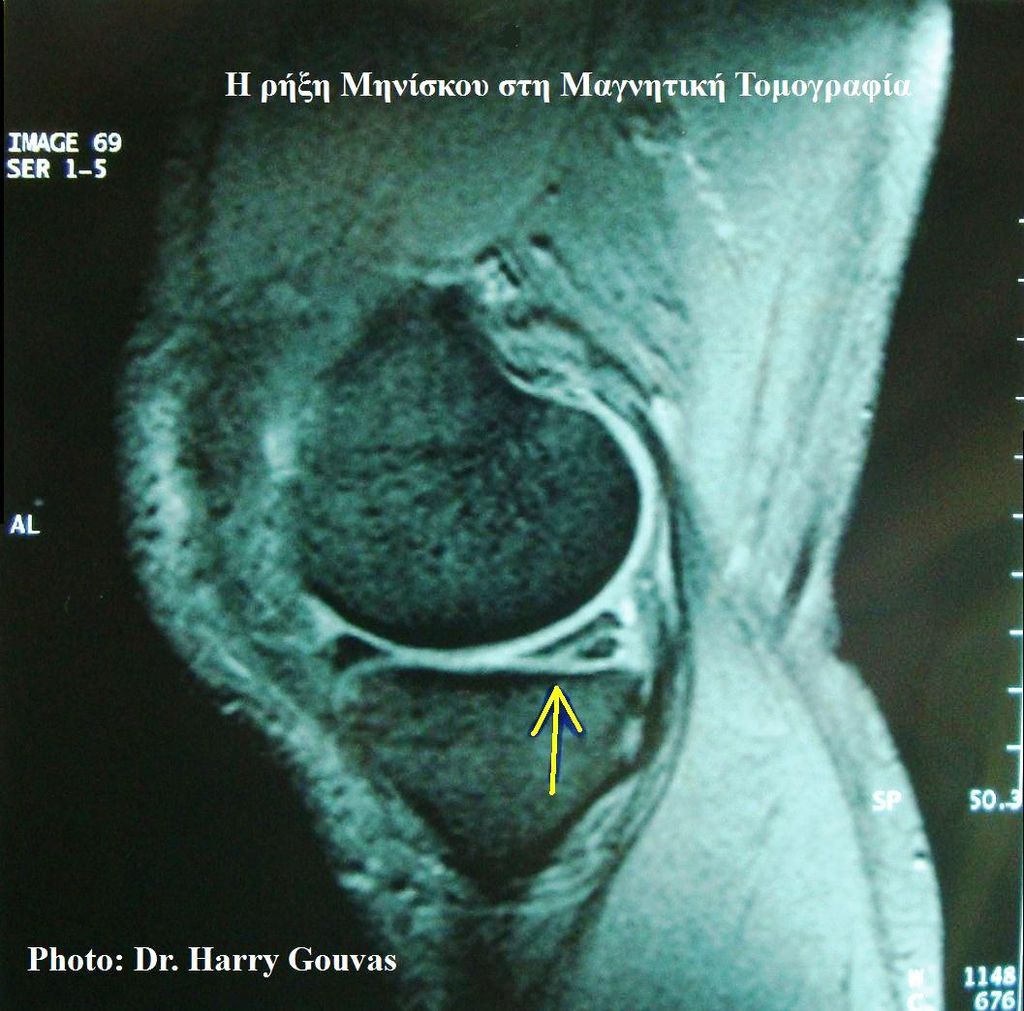
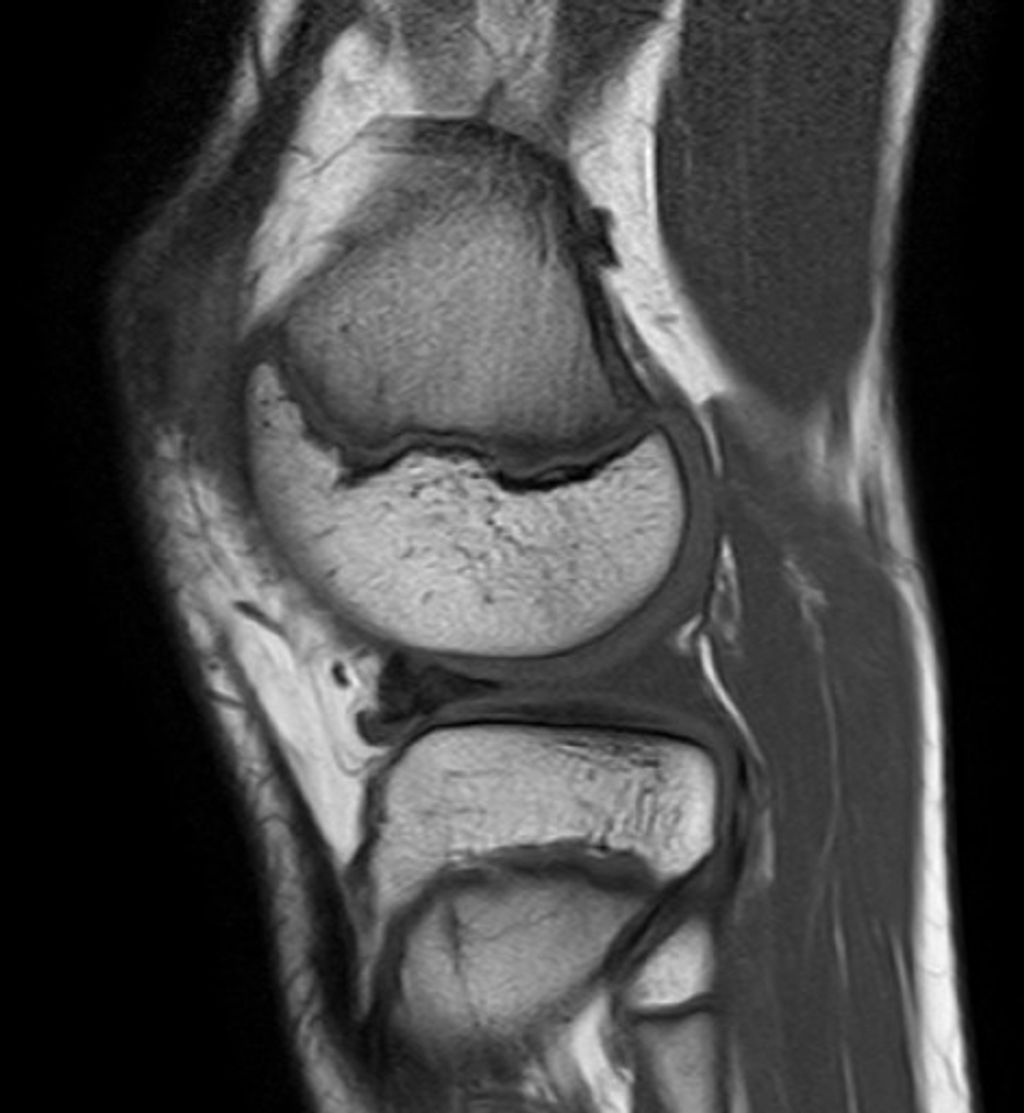
The knee joint is encapsulated in a synovial membrane, which secretes synovial fluid for lubrication, reducing friction during movement. The menisci, two C-shaped pieces of cartilage, act as shock absorbers and ensure smooth articulation between the femur and tibia.
- Proper alignment and balance of these structures are crucial for the knee’s function. Any misalignment can lead to pain and dysfunction. Here’s a simple breakdown of the key components:
- Femur: Thigh bone, articulates with the tibia and patella
- Tibia: Shin bone, supports the weight of the body
- Patella: Kneecap, protects the knee joint
- Ligaments: Connect bones and provide stability
- Tendons: Connect muscles to bones, facilitating movement
- Menisci: Cartilage that cushions and stabilizes the joint
- Synovial membrane: Produces fluid for lubrication
Remember, maintaining the health of each component is essential for the overall function of the knee joint. Regular exercise and weight management can help preserve knee joint integrity and function.
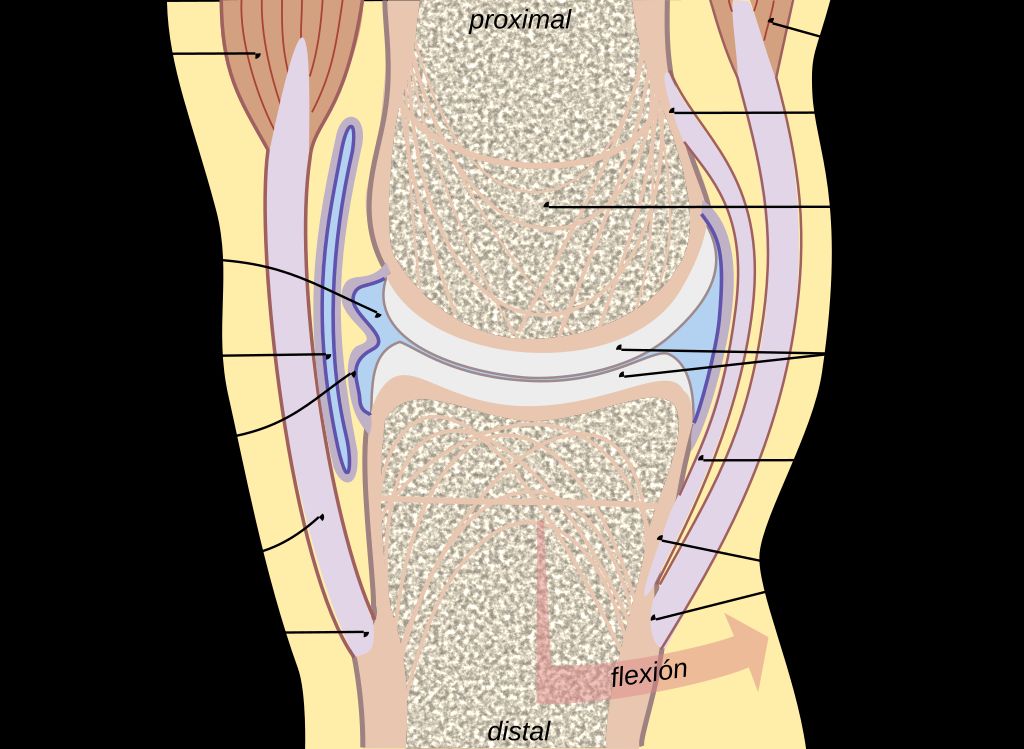
Function of the Knee Joint
The function of the knee joint is crucial for our mobility and stability. It allows us to perform activities such as walking, running, and jumping. The knee joint also plays a role in absorbing shock and providing support for the body. Maintaining healthy knee function is essential for overall quality of life.
| Function | Description |
|---|---|
| Flexion | Bending of the knee joint |
| Extension | Straightening of the knee joint |
| Rotation | Internal and external rotation |
It is important to note that proper knee function is necessary for a wide range of daily activities. Engaging in exercises that promote knee strength and flexibility can contribute to improved joint function and overall well-being.
Indications for Knee Joint Replacement Surgery

Degenerative Joint Disease
Degenerative joint disease, also known as osteoarthritis, is the most common reason for knee joint replacement surgery. It is characterized by the breakdown of cartilage in the joint, leading to pain, stiffness, and reduced mobility. Early intervention is crucial in managing degenerative joint disease, as it can prevent further damage to the knee joint. Patients with degenerative joint disease often experience relief from pain and improved function after knee joint replacement surgery. Here is a brief overview of the success rates for knee joint replacement surgery:
| Success Rate | Percentage |
|---|---|
| 1 year | 90% |
| 5 years | 80% |
| 10 years | 70% |
It’s important to note that individual results may vary, and consulting with a healthcare professional is essential for personalized guidance and care. Patients should also be aware of the potential risks and complications associated with knee joint replacement surgery, which can be discussed in detail with their healthcare provider.
Rheumatoid Arthritis
Rheumatoid arthritis is a chronic, systemic autoimmune condition that affects the joints, including the knees. It can lead to significant pain, swelling, and stiffness, impacting our ability to perform daily activities. In some cases, medication and other conservative treatments may not provide sufficient relief, leading to the consideration of knee joint replacement surgery. Patients with rheumatoid arthritis may experience improved joint function, reduced pain, and enhanced quality of life following knee replacement surgery. However, it’s important to carefully consider the potential risks and benefits, as well as the long-term management of the condition post-surgery.
Post-Traumatic Arthritis
In our exploration of knee joint replacement surgery, we recognize that post-traumatic arthritis is a significant factor necessitating this procedure. Following a severe injury to the knee, such as a fracture or ligament damage, the joint may develop arthritis over time. This condition is characterized by the gradual deterioration of the cartilage that cushions the ends of the bones in the joint.
The symptoms of post-traumatic arthritis include pain, swelling, and a decreased range of motion, which can severely impact daily activities. We often see patients who have exhausted other treatment options, such as anti-inflammatory medications or corticosteroid injections, before considering surgery.
Key considerations for patients with post-traumatic arthritis contemplating knee replacement surgery include:
- The extent of joint damage
- The patient’s age and activity level
- The presence of other medical conditions
Tip: It’s crucial for patients to have realistic expectations about the outcomes of knee replacement surgery and to understand that rehabilitation is an integral part of the recovery process.
Surgical Techniques for Knee Joint Replacement

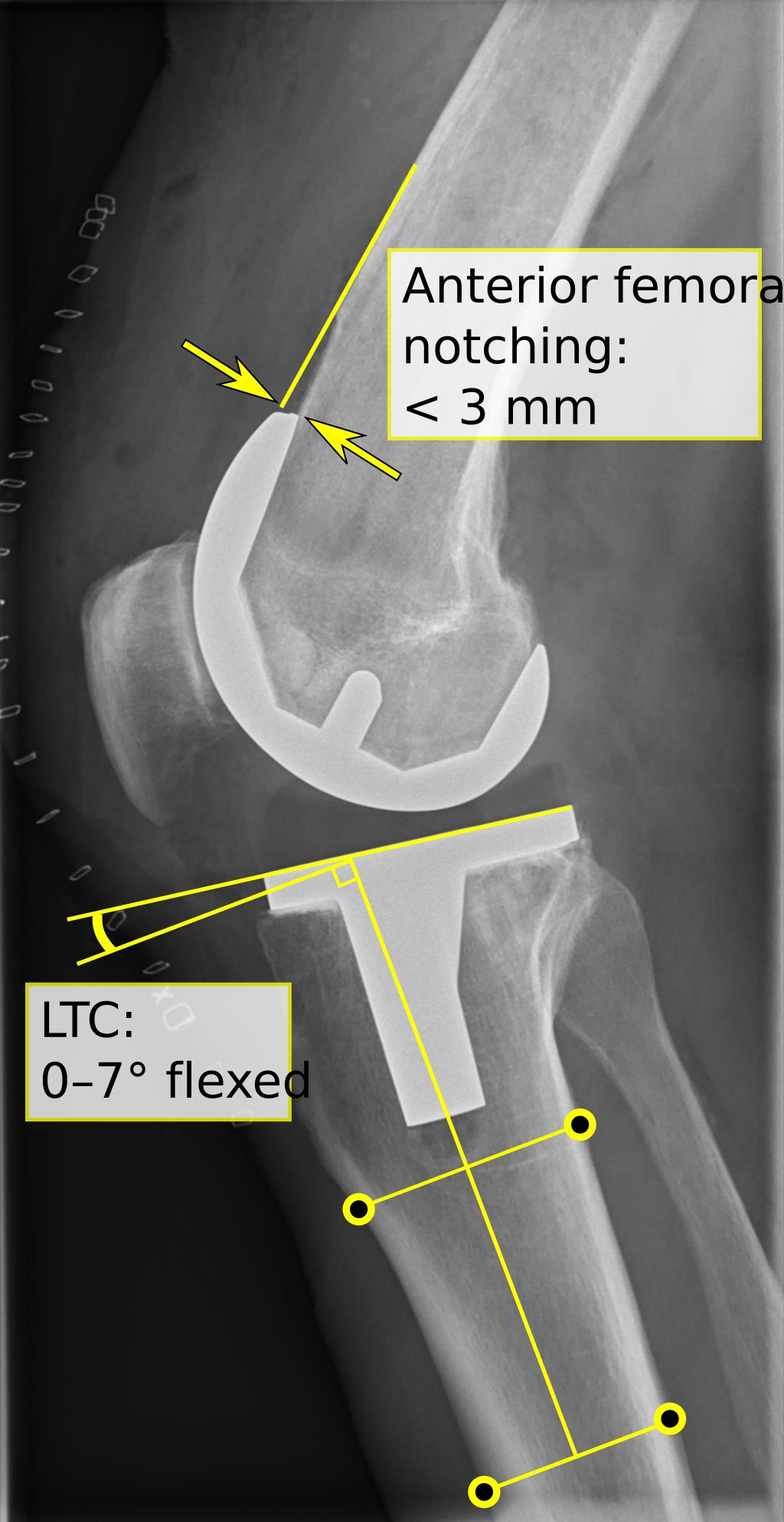
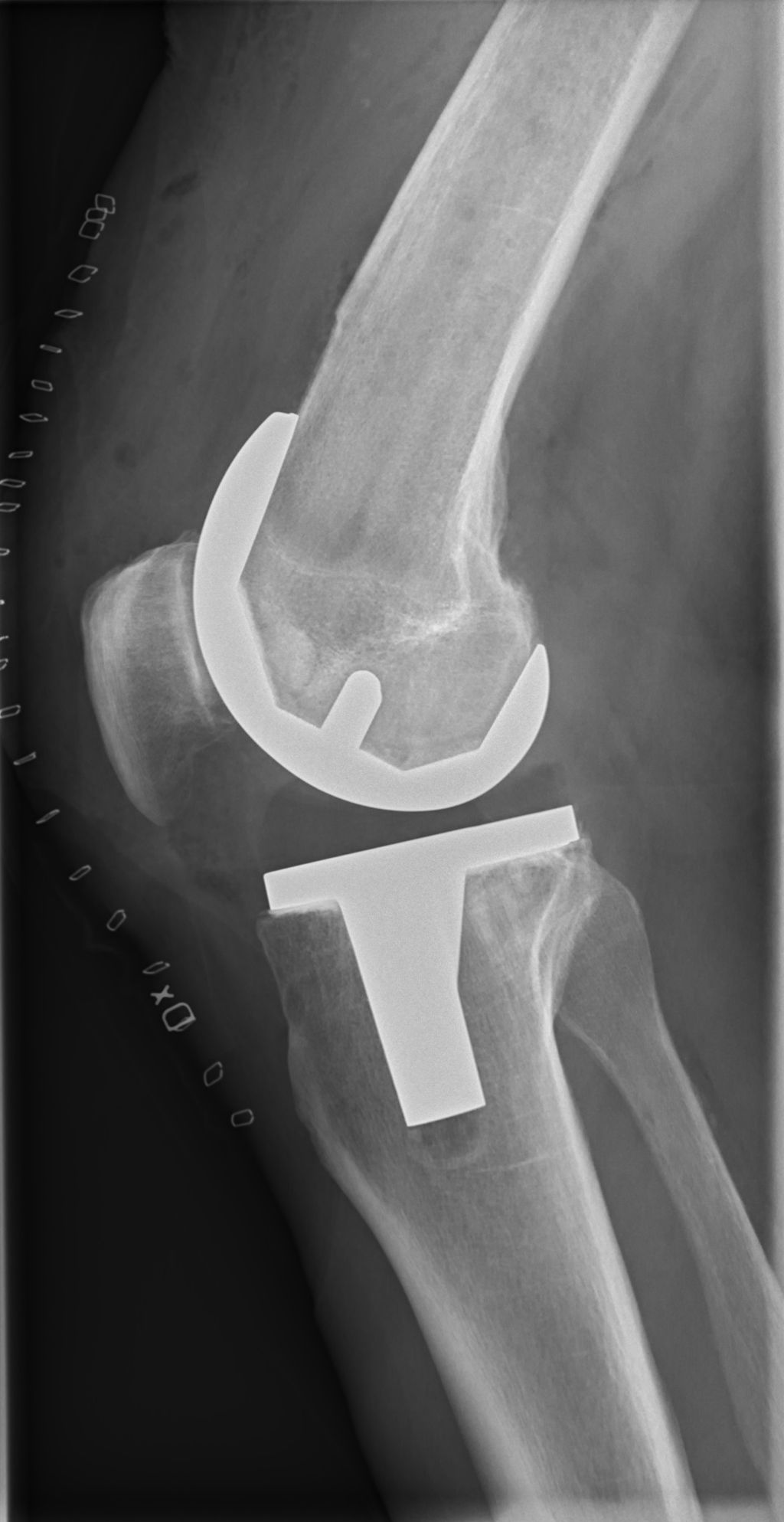
Total Knee Replacement
After undergoing a Total Knee Replacement, the rehabilitation process is crucial for a successful recovery. Our team emphasizes the importance of physical therapy and home care in the post-surgery period. Here’s a brief overview of the expected recovery timeline:
Partial Knee Replacement
In our exploration of knee joint replacement options, we recognize that partial knee replacement surgery is a viable choice for patients whose arthritis is confined to a single compartment of the knee. Unlike total knee replacement, this procedure involves replacing only the damaged area of the knee, preserving as much of the natural knee structure as possible.
Partial knee replacement offers several advantages, including a quicker recovery time and less blood loss during surgery. Patients often report a more natural knee feeling post-operation due to the retention of undamaged knee components.
The following list outlines the typical steps involved in a partial knee replacement procedure:
- Anesthesia is administered.
- A small incision is made in the knee area.
- Damaged cartilage and bone are removed from the knee.
- Implants are positioned to resurface the damaged knee compartment.
- The knee is tested for proper movement and alignment.
- The incision is closed, and the recovery process begins.
Tip: It’s crucial for patients to follow their surgeon’s advice on post-operative care to ensure the best possible outcome.
Minimally Invasive Knee Replacement
After undergoing a Minimally Invasive Knee Replacement, my team and I focus on providing personalized care to ensure a smooth recovery process. We emphasize the importance of early mobilization and pain management to facilitate a quicker return to normal activities. Our approach involves a combination of physical therapy, home exercises, and regular follow-up appointments to monitor progress and address any concerns.
Additionally, we track patient outcomes using the following data:
| Metric | Outcome |
|---|---|
| Range of Motion | Excellent improvement in flexion and extension |
| Pain Level | Significant reduction in post-operative pain |
| Hospital Stay | Shortened duration of hospitalization |
Our experience has shown that this comprehensive approach leads to favorable outcomes and high patient satisfaction. As a team, we are committed to providing the best possible care and support throughout the recovery journey.
Tip: Encouraging early ambulation and adherence to prescribed exercises can significantly contribute to a successful recovery after minimally invasive knee replacement surgery.
Rehabilitation and Recovery After Knee Joint Replacement

Physical Therapy
Physical therapy plays a crucial role in our recovery journey after knee joint replacement surgery. It is a comprehensive program that focuses on improving our strength, flexibility, and range of motion. Through tailored exercises and activities, physical therapy helps us regain functionality and mobility in our knee joint. Additionally, it is important to note that physical therapy is not limited to post-surgery recovery; it benefits individuals of all ages and activity levels, aiming to improve overall well-being. Here is a brief overview of the key components of physical therapy:
Home Care
After completing the phase of Home Care, we transition to the next stage of rehabilitation. This phase focuses on regaining strength, flexibility, and mobility in the knee joint. Our team will guide you through a personalized exercise program tailored to your specific needs and progress. Additionally, we will monitor your progress closely to ensure that any setbacks are addressed promptly and effectively. It’s important to remember that setbacks are a natural part of the recovery process, and with the right strategies, one can overcome them quickly and emerge stronger. Our goal is to support you in achieving a successful and sustainable recovery.
Expected Recovery Timeline
After undergoing knee joint replacement surgery, recovery is a crucial phase that requires patience and dedication. Our rehabilitation program focuses on restoring strength, flexibility, and mobility to the knee joint. Physical therapy plays a key role in this process, with personalized exercises and techniques tailored to each patient’s needs. Additionally, home care is an essential aspect of recovery, involving proper wound care, medication management, and assistance with daily activities. It’s important to note that the expected recovery timeline varies for each individual, depending on factors such as overall health, adherence to rehabilitation protocols, and post-operative complications. Patients are encouraged to follow the guidance of their healthcare team and adhere to the prescribed rehabilitation plan for optimal outcomes.
Conclusion
In conclusion, the insights gained from this article shed light on the intricate nature of knee joint replacement surgery. The complexity of the procedure, coupled with the potential for improved mobility and quality of life for patients, underscores the significance of ongoing research and advancements in this field. As medical knowledge and technology continue to evolve, it is imperative to prioritize the well-being and long-term outcomes of individuals undergoing knee joint replacement surgery.
Frequently Asked Questions
What is the recovery time for knee joint replacement surgery?
The recovery time for knee joint replacement surgery varies, but most patients can expect to resume normal activities within 3 to 6 months.
Is knee joint replacement surgery painful?
Patients may experience some pain and discomfort after surgery, but this can be managed with medication and proper rehabilitation.
How long does a knee joint replacement surgery take?
The duration of knee joint replacement surgery typically ranges from 1 to 2 hours, depending on the complexity of the procedure.
What are the potential risks and complications of knee joint replacement surgery?
Potential risks and complications include infection, blood clots, implant loosening, and nerve damage, among others. Your surgeon will discuss these in detail before the surgery.
Can I return to sports and physical activities after knee joint replacement surgery?
Many patients are able to return to low-impact sports and physical activities after knee joint replacement surgery, but high-impact activities may be limited.
How long does a knee joint replacement implant last?
The lifespan of a knee joint replacement implant varies, but most implants last between 15 to 20 years. Revision surgery may be required after this time period.