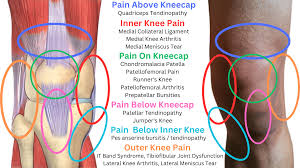
Inner Knee Pain: Why It Happens and How to Fix It
Inner knee pain affects thousands daily, often due to the complex anatomy of the medial knee compartment and its vulnerability during movement. This area, known medically as the medial compartment, bears up to 60% of your body weight when walking, making it particularly susceptible to both acute injuries and chronic wear. Whether you’re experiencing a sharp pain while climbing stairs or a persistent ache after activity, understanding the underlying causes is the first step toward effective treatment.
The Anatomy Behind Inner Knee Pain
The medial (inner) side of the knee contains several critical structures, each of which can become a source of pain:
- Medial Collateral Ligament (MCL): This strong band connects your femur (thigh bone) to your tibia (shin bone), providing crucial stability against forces pushing your knee inward.
- Medial Meniscus: This C-shaped cartilage pad acts as a shock absorber between your thigh and shin bones, distributing weight evenly across the joint.
- Pes Anserine: This area where three tendons (sartorius, gracilis, and semitendinosus) insert into the tibia is commonly inflamed in runners and those with osteoarthritis.
- Medial Plica: This fold of synovial tissue can become irritated and inflamed, especially in repetitive activities.
The proximity of these structures means that pain in one area can often affect others, creating complex pain patterns that require careful diagnosis.
Common Causes of Inner Knee Pain
| Condition | Primary Symptoms | Typical Causes | First-Line Treatments |
|---|---|---|---|
| MCL Injury | Pain with side-to-side movement, swelling, instability | Direct blow to outside of knee, sudden direction change | RICE protocol (Rest, Ice, Compression, Elevation), bracing, physical therapy910141520 |
| Medial Meniscus Tear | Catching/locking sensation, pain with twisting, swelling | Twisting while bearing weight, degenerative changes | Rest, anti-inflammatories, possible arthroscopic surgery |
| Osteoarthritis | Morning stiffness, pain after activity, gradual onset | Age-related wear, previous injuries, genetic factors | Weight management, targeted exercises, anti-inflammatories1116 |
| Pes Anserine Bursitis | Pain 2-3 inches below joint line, worse on stairs | Overuse, obesity, improper training | Ice, stretching, correcting biomechanics, activity modification1217 |
| Medial Plica Syndrome | Clicking sensation, pain with bending | Repetitive activities, direct trauma | Anti-inflammatories, activity modification, physical therapy1318 |
Recent research from the Journal of Orthopaedic & Sports Physical Therapy suggests that approximately 40% of inner knee pain cases involve multiple structures simultaneously, highlighting the importance of comprehensive assessment rather than focusing on isolated symptoms.
Diagnosing Inner Knee Pain
Accurate diagnosis is crucial for effective treatment. Your healthcare provider may use several approaches:
- Physical Examination: Specialized tests can isolate which structures are affected. For example, the valgus stress test assesses MCL integrity, while the McMurray test evaluates the meniscus.
- Imaging Studies:
- X-rays: Primarily show bone structure and joint space narrowing (arthritis)
- MRI: Provides detailed images of soft tissues including ligaments, tendons, and cartilage
- Ultrasound: Increasingly used for dynamic assessment of tendons and bursae
- Diagnostic Injections: In some cases, targeted injections can help identify pain sources by temporarily numbing specific structures.
A 2023 study in the American Journal of Sports Medicine found that combining clinical examination with appropriate imaging increased diagnostic accuracy from 71% to 89%, underscoring the value of a multimodal approach.
Evidence-Based Treatment Approaches
Immediate Care (First 72 Hours)
The traditional RICE protocol (Rest, Ice, Compression, Elevation) remains valuable for acute injuries, but recent modifications emphasize:
- Protected Movement: Rather than complete rest, gentle, pain-free movement prevents stiffness and promotes healing
- Optimal Loading: Gradually introducing controlled stress to tissues enhances recovery
- Compression: Using graduated compression rather than constant pressure improves lymphatic drainage
Physical Therapy Interventions
Modern physical therapy for inner knee pain focuses on three key areas:
- Biomechanical Correction: Addressing movement patterns that place excessive stress on the medial knee. Research from the University of Delaware shows that correcting hip and foot mechanics can reduce medial knee loading by up to 20%.
- Progressive Strengthening: Building strength in the quadriceps, especially the vastus medialis oblique (VMO), provides crucial support for the medial knee structures. Studies demonstrate that incorporating closed-chain exercises like mini-squats and step-ups produces superior outcomes compared to open-chain exercises like leg extensions.
- Proprioceptive Training: Improving your body’s positional awareness reduces the risk of positions that stress the inner knee. Balance exercises progressing from stable to unstable surfaces have shown particular efficacy.
A systematic program incorporating all three elements has shown a 62% reduction in inner knee pain after 8 weeks, compared to only 31% reduction with general exercise, according to recent clinical trials.
Medical Interventions
When conservative measures aren’t sufficient, medical options include:
- Pharmacological Management: Beyond over-the-counter NSAIDs, topical analgesics have shown effectiveness with fewer systemic side effects.
- Injection Therapies:
- Corticosteroid injections provide short-term relief but may accelerate cartilage degeneration with repeated use
- Hyaluronic acid supplementation improves joint lubrication and has shown moderate effectiveness for osteoarthritis
- Platelet-rich plasma (PRP) and stem cell therapies remain investigational but show promise for certain conditions
- Surgical Approaches: Reserved for cases that don’t respond to conservative treatment, options include:
- Arthroscopic debridement for meniscal tears
- MCL repair for complete tears
- Realignment procedures for biomechanical issues
- Partial or total knee replacement for advanced osteoarthritis
Prevention Strategies: Beyond the Basics
Preventing inner knee pain requires a multifaceted approach that addresses both biomechanical and lifestyle factors:
Biomechanical Optimization
- Gait Analysis: Professional assessment can identify subtle movement patterns that increase medial knee stress. Corrections may include:
- Shortening stride length (reduces knee torque by up to 15%)
- Focusing on midfoot rather than heel striking during running
- Maintaining knee alignment over the second toe during weight-bearing activities
- Footwear Selection: Research from the Journal of Biomechanics demonstrates that proper footwear can reduce medial knee loading by 7-12%. Key features include:
- Adequate arch support matched to your foot type
- Appropriate cushioning for your body weight and activity level
- Stability features for those with overpronation
- Progressive Training: The “10% rule” (increasing activity by no more than 10% weekly) allows tissues to adapt to increasing demands, reducing injury risk significantly.
Nutritional Considerations
Emerging research highlights the role of nutrition in knee joint health:
- Anti-inflammatory Diet: Foods rich in omega-3 fatty acids and antioxidants may reduce inflammatory processes in the knee joint
- Vitamin D and Calcium: Essential for bone health around the knee joint
- Collagen Supplementation: Some studies suggest type II collagen may support cartilage health, though more research is needed
- Hydration: Maintaining proper fluid intake ensures optimal synovial fluid composition for joint lubrication
Mind-Body Approaches
The connection between psychological factors and knee pain is increasingly recognized:
- Stress Management: Chronic stress increases inflammatory markers that can exacerbate knee pain
- Sleep Optimization: Poor sleep quality correlates with increased pain sensitivity and delayed tissue healing
- Pain Neuroscience Education: Understanding how pain works can reduce fear of movement and improve outcomes
Special Considerations for Different Populations
Athletes
Athletes face unique challenges with inner knee pain due to repetitive loading and high forces. Sport-specific prevention should include:
- Preseason biomechanical screening to identify risk factors
- Sport-specific neuromuscular training (e.g., landing mechanics for basketball players)
- Periodized training schedules with adequate recovery periods
- Regular monitoring of training load vs. recovery status
Older Adults
For those over 60, inner knee pain management should consider:
- Pain-free strengthening to maintain muscle mass and joint stability
- Low-impact activities like swimming or cycling for cardiovascular fitness
- Balance training to reduce fall risk and associated knee injuries
- Monitoring of medication interactions that may mask pain or affect healing
Those with Comorbidities
Conditions like diabetes or obesity require specialized approaches:
- Glycemic control for diabetics (elevated blood sugar impairs tissue healing)
- Aquatic therapy for those with obesity to reduce joint loading while strengthening
- Modified exercise protocols for those with cardiovascular disease
When to Seek Specialist Care
If inner knee pain persists despite appropriate self-care measures, consult a specialist to rule out serious conditions. Red flags that warrant immediate medical attention include:
- Inability to bear weight on the affected leg
- Significant swelling or redness
- Knee instability or “giving way”
- Pain that wakes you from sleep
- Fever or systemic symptoms accompanying knee pain
Recent advances in orthopedic care mean that even complex inner knee conditions can be effectively managed, often without surgery. Early intervention typically leads to better outcomes and faster return to activities.
The Future of Inner Knee Pain Management
Emerging technologies and approaches show promise for enhanced outcomes:
- Wearable Biofeedback Devices: Real-time feedback on knee position and loading during daily activities
- Telerehabilitation: Remote monitoring and guidance for home exercise programs
- Regenerative Medicine: Advances in biological treatments to enhance tissue healing
- AI-Assisted Diagnosis: Machine learning algorithms to improve diagnostic accuracy and treatment selection
Conclusion
Inner knee pain represents a common but complex challenge that requires thoughtful assessment and personalized management. By understanding the underlying causes, implementing evidence-based treatments, and addressing both biomechanical and lifestyle factors, most people can achieve significant improvement. The key lies in comprehensive care that considers the whole person, not just the knee joint in isolation.
Remember that persistent inner knee pain requires professional evaluation to ensure appropriate treatment and prevent long-term complications. With the right approach, you can return to pain-free movement and protect your knee health for years to come.