Understanding knee pain symptoms and causes is the first step toward taking back control of your life, and the urgency is real. More than 50% of individuals as young as 33 years old already show early signs of knee joint damage on MRI scans, often before any symptoms appear at all. If your knee is giving you trouble, you are not alone, and more importantly, you deserve clear answers about what is happening inside that joint.
Key Takeaways
| Question | Quick Answer |
|---|---|
| What are the most common knee pain symptoms? | Swelling, stiffness, sharp or dull aching, popping sensations, warmth, and instability when bearing weight. |
| What causes knee pain? | The most common causes include ligament injuries, meniscus tears, osteoarthritis, tendinitis, and traumatic impact injuries. |
| Can knee hurt without an obvious injury? | Yes. Overuse, arthritis, nutritional deficiencies, and misalignment can all cause significant knee pain without a single traumatic event. |
| When should I see a doctor for knee pain? | Seek care if you experience severe swelling, inability to bear weight, a “popping” sound at injury, or pain that lasts more than a few days. |
| Is knee pain a sign of arthritis? | It can be. Knee pain with morning stiffness, grinding sensations, and gradual worsening over time is a common arthritis pattern. |
| Can knee pain symptoms be treated without surgery? | Absolutely. Physical therapy, compression support, exercise, and lifestyle changes resolve the majority of cases without going near an operating room. |
| What is the best starting resource for knee pain? | Our ultimate guide to understanding and managing knee pain covers causes, treatments, and prevention all in one place. |
What Is Knee Pain? Understanding the Basics
The knee is the largest joint in the human body, and it takes an enormous amount of punishment every single day. Every time you walk, climb stairs, sit down, or stand back up, your knee absorbs forces that can equal multiple times your body weight.
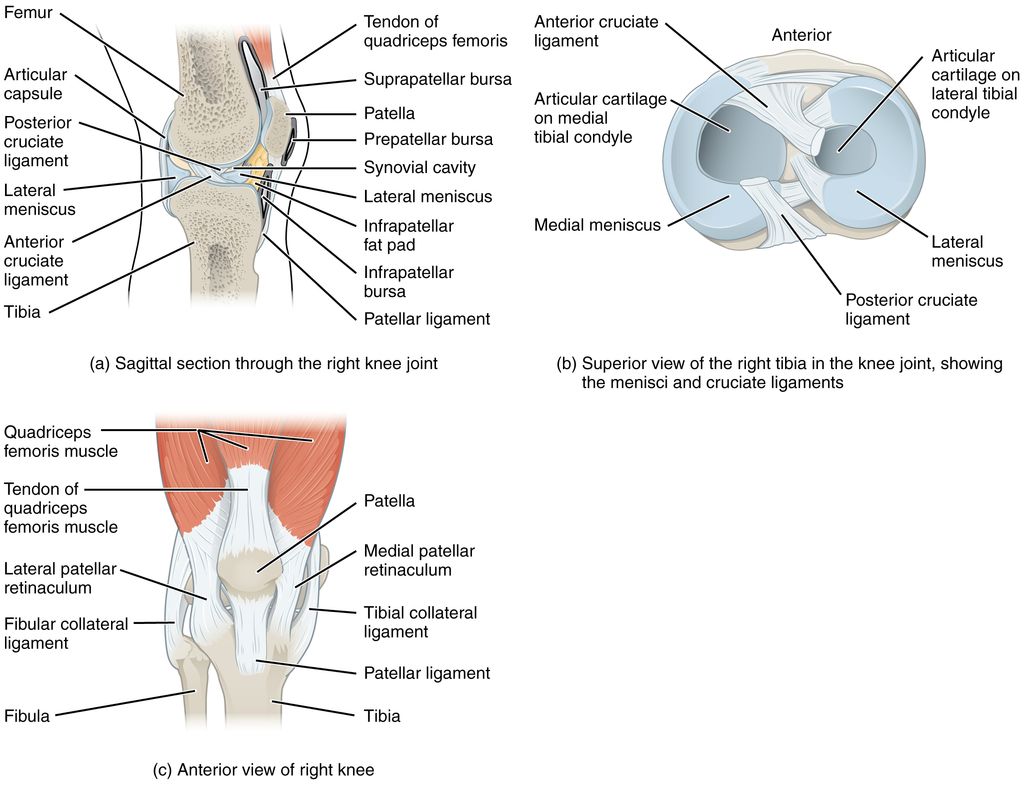
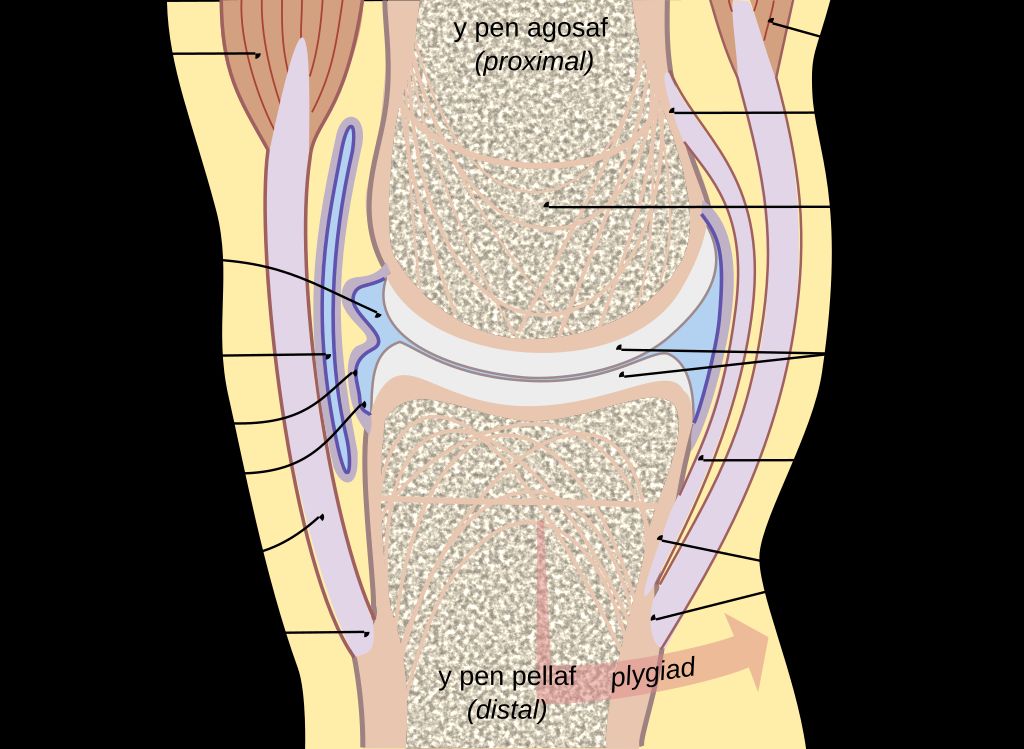
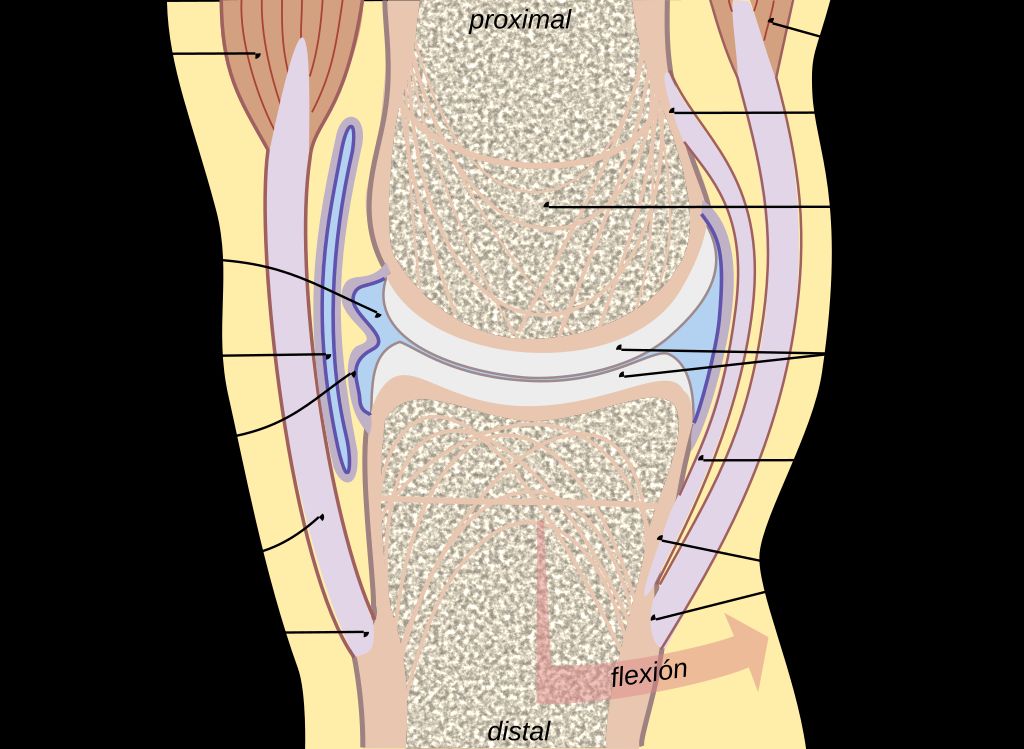
It is no surprise then that knee pain is one of the most reported musculoskeletal complaints seen by healthcare providers in 2026. The joint is a complex network of bones, cartilage, ligaments, tendons, and fluid-filled sacs (called bursae), and any one of these structures can become injured or inflamed.
When we talk about knee pain symptoms and causes, we are really talking about a wide spectrum of conditions. Some people feel a sharp, stabbing sensation on the inside of the knee. Others experience a dull, grinding ache that never quite goes away.
Understanding what type of pain you have, and where it is located, can go a long way toward figuring out what is actually wrong. That is exactly what this guide is for.
Common Knee Pain Symptoms and Causes: The Warning Signs
Recognizing the warning signs early is critical. Your body is always trying to communicate with you, and knee pain symptoms are its way of waving a red flag before things get worse.
Here are the most important symptoms to pay attention to:
-
Swelling and puffiness around the joint – This usually signals inflammation or fluid build-up.
-
Stiffness, especially in the morning – A telltale sign of arthritis-related changes inside the joint.
-
Warmth and redness – Indicates active inflammation, possibly from an infection or inflammatory arthritis.
-
A grinding, clicking, or popping sensation – Often associated with cartilage wear or a torn meniscus.
-
Instability or “giving way” – The feeling that your knee might buckle under you, often linked to ligament damage.
-
Sharp, localized pain – Pain in a very specific spot that worsens with certain movements.
-
Dull, aching pain – A constant background ache that is often linked to overuse or arthritis.
-
Pain behind the kneecap – Commonly caused by patellofemoral syndrome or chondromalacia.
-
Pain when climbing stairs or squatting – A classic pattern in patella-related conditions.
-
Inability to fully straighten or bend the knee – Can indicate a torn meniscus or severe swelling.
It is worth noting that the location of your pain matters enormously. Pain on the inner side of the knee often points to a different problem than pain on the outer side or directly under the kneecap.
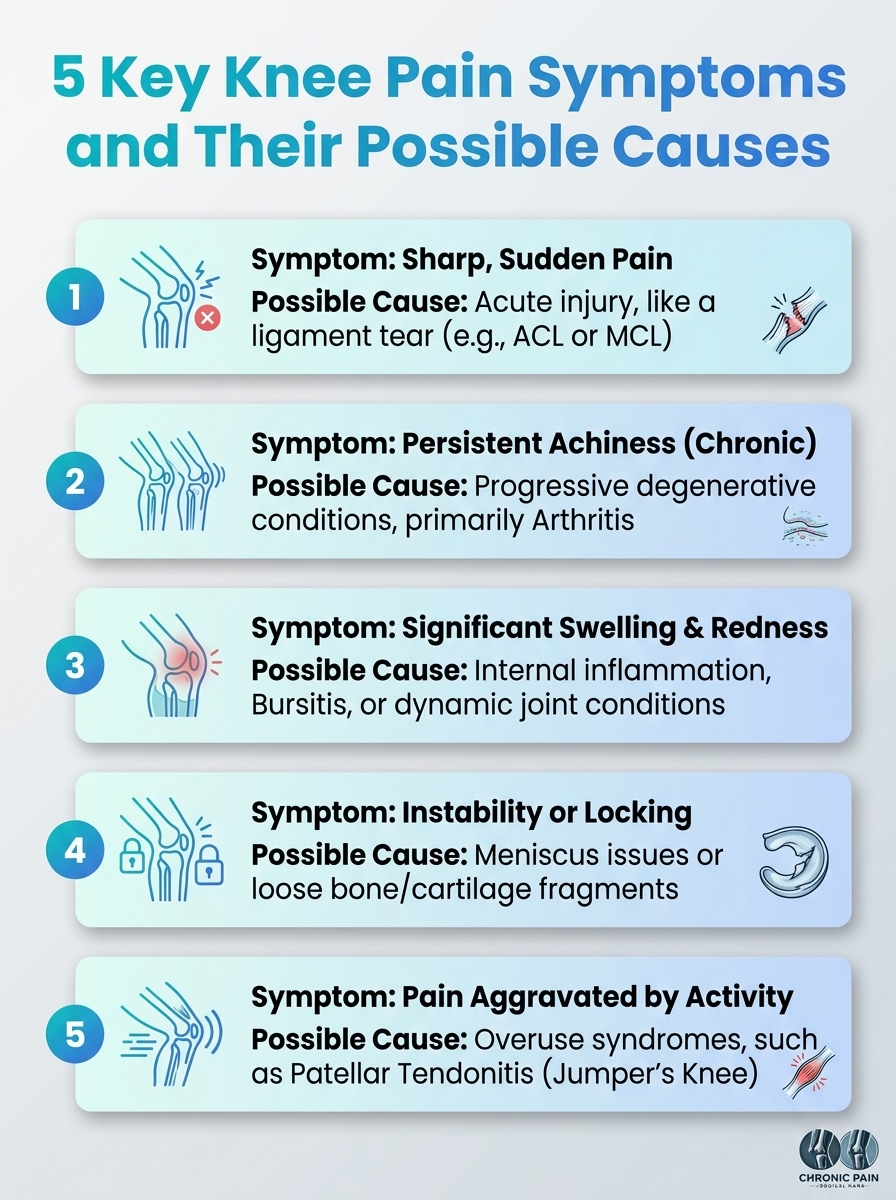
Shows the five main knee pain symptoms and their possible causes. A quick reference for understanding when to seek care.
The Top Causes of Knee Pain: Injuries, Overuse, and Disease
Knee pain symptoms and causes fall into three broad categories: acute injuries, chronic overuse conditions, and systemic diseases like arthritis. Understanding which category applies to you is the foundation of any effective treatment plan.
Acute injuries happen suddenly. You twist your knee on the basketball court, take a hard fall, or absorb a direct blow. These injuries often produce immediate, intense pain alongside rapid swelling.
Overuse conditions develop gradually. They creep up on you after weeks or months of repetitive activity, poor biomechanics, or inadequate recovery time. The pain starts mild, then gets harder and harder to ignore.
Systemic diseases like osteoarthritis and rheumatoid arthritis cause progressive joint damage. They are not caused by a single event but rather by long-term biological and structural processes inside the joint.
For a deeper look at traumatic events that cause immediate joint damage, visit our dedicated page on traumatic knee injuries to understand what happens to the joint during high-impact incidents.
Did You Know?
Losing just 1 pound of body weight results in a 4-pound reduction in pressure on the knee joint during daily activities.
Source: World Health Organization
Ligament Injuries: A Leading Cause of Knee Hurt
Ligament injuries are among the most common and most painful causes of acute knee hurt. The knee has four main ligaments that hold the joint together, and tearing any one of them can be devastating.
The Anterior Cruciate Ligament (ACL) is the most commonly torn ligament in the knee. ACL tears often happen during sports that involve sudden stops, changes of direction, or landing from a jump. The hallmark symptom is a loud “pop” at the moment of injury, followed immediately by intense pain and rapid swelling.

The Posterior Cruciate Ligament (PCL) is less commonly injured but equally disruptive. PCL injuries typically occur from a direct blow to the front of the knee, such as hitting the dashboard in a car accident.
Other ligaments, including the medial collateral ligament (MCL) and lateral collateral ligament (LCL), can also be sprained or torn, causing significant instability and pain along the sides of the knee.
-
Learn more about ACL injuries and the right knee brace support for your recovery.
-
Understand PCL knee injuries and how they differ from ACL damage.
-
Explore a full overview of ligament knee injuries and what causes them.

Meniscus Tears and Cartilage Damage: Key Knee Pain Symptoms and Causes
Between the bones of your knee, two C-shaped pads of cartilage called menisci act as shock absorbers. When these tear, the result is significant pain, swelling, and often a locking or catching sensation inside the joint.
Meniscus tears are extremely common, affecting athletes and non-athletes alike. A sudden twisting motion with the foot planted is a classic mechanism of injury. But meniscus tears also occur gradually in older adults as the cartilage becomes more brittle and less resilient over time.
Cartilage damage beneath the kneecap, a condition known as chondromalacia patella, is another source of chronic knee pain. It produces a characteristic dull ache under and around the kneecap, which tends to worsen when you sit for long periods, climb stairs, or squat.
-
Get detailed information on torn meniscus injuries, including symptoms and recovery options.
-
Understand chondromalacia patella and what is really happening to the cartilage under your kneecap.
Arthritis and Knee Pain Symptoms and Causes: What You Need to Know
Arthritis is one of the leading long-term causes of knee pain symptoms and causes, and it comes in more than one form. The two most relevant types for the knee are osteoarthritis and rheumatoid arthritis.
Osteoarthritis (OA) is by far the more common of the two. It occurs when the protective cartilage inside the knee joint gradually wears down, allowing bone to grind against bone. The hallmark symptoms include:
-
A deep, aching pain that worsens with activity and eases with rest
-
Morning stiffness that loosens up after 20 to 30 minutes of movement
-
Grating or grinding sensations inside the joint
-
Gradual loss of range of motion
-
Visible swelling and a feeling of warmth around the joint
Rheumatoid Arthritis (RA) is an autoimmune disease, meaning the body’s immune system attacks the joint lining. RA typically affects both knees simultaneously and is accompanied by systemic symptoms like fatigue and fever.
In 2026, osteoarthritis remains one of the most undertreated conditions globally, largely because many people assume their knee hurt is simply “part of getting older.” It is not something you have to accept without taking action.

When Knee Hurt Becomes Daily: Overuse and Tendon-Related Causes
Not all knee pain symptoms and causes involve a dramatic injury. Some of the most persistent and frustrating cases of knee hurt come from overuse, repetitive strain, and tendon problems that build up silently over time.
The most common overuse conditions affecting the knee include:
| Condition | Main Symptom | Who It Affects Most |
|---|---|---|
| Runner’s Knee (Patellofemoral Syndrome) | Aching pain around and under the kneecap | Runners, cyclists, hikers |
| Jumper’s Knee (Patellar Tendinitis) | Sharp pain just below the kneecap | Basketball players, volleyball players |
| IT Band Syndrome | Burning pain on the outer knee | Long-distance runners, cyclists |
| Bursitis | Swelling and tenderness at the front of the knee | People who kneel frequently |
| Pes Anserine Bursitis | Pain and swelling on the inner side of the knee | People with obesity, OA patients |
These conditions respond very well to targeted exercise, compression support, and changes in training habits. They do not require surgery, and they are very manageable once properly identified.
Risk Factors That Make Knee Pain Symptoms Worse
Certain factors significantly increase your likelihood of developing knee pain or worsening symptoms that are already present. Knowing your personal risk factors gives you the power to make changes before things escalate.
-
Excess body weight. Every extra pound of body weight translates to several additional pounds of pressure on the knee joint during walking. This accelerates cartilage wear dramatically.
-
Age. Cartilage naturally becomes less resilient over time, making older adults more susceptible to degenerative knee pain symptoms and causes.
-
Previous knee injury. A prior ACL tear, fracture, or meniscus injury significantly raises the risk of future problems, including osteoarthritis.
-
Muscle weakness. Weak quadriceps and hamstrings force the knee to absorb more impact than it should, increasing wear and tear.
-
Improper footwear. High heels increase peak pressure on the knee joint by approximately 26%, accelerating degeneration over years of use.
-
Sedentary lifestyle. Lack of movement stiffens the joint and weakens the surrounding muscles that normally provide crucial support.
-
High-impact sports participation. Repetitive jumping, pivoting, and heavy loading stress the joint structures beyond their natural capacity.
-
Vitamin D deficiency. Research in 2026 continues to link low Vitamin D levels to increased knee pain severity and joint inflammation.
How Knee Pain Is Diagnosed: Tests and Physical Examination
Getting the right diagnosis is non-negotiable if you want to treat your knee pain correctly. There is no such thing as a one-size-fits-all approach, and what works for a meniscus tear is completely different from what works for arthritis.
A thorough diagnosis typically includes several key steps:
-
Physical Examination. A clinician will visually inspect the knee for swelling, bruising, and deformity. They will gently press around the joint to identify tender spots and test your range of motion.
-
Special Orthopedic Tests. Specific maneuvers (like the Lachman test for ACL integrity or McMurray’s test for meniscus tears) help pinpoint which structures are damaged.
-
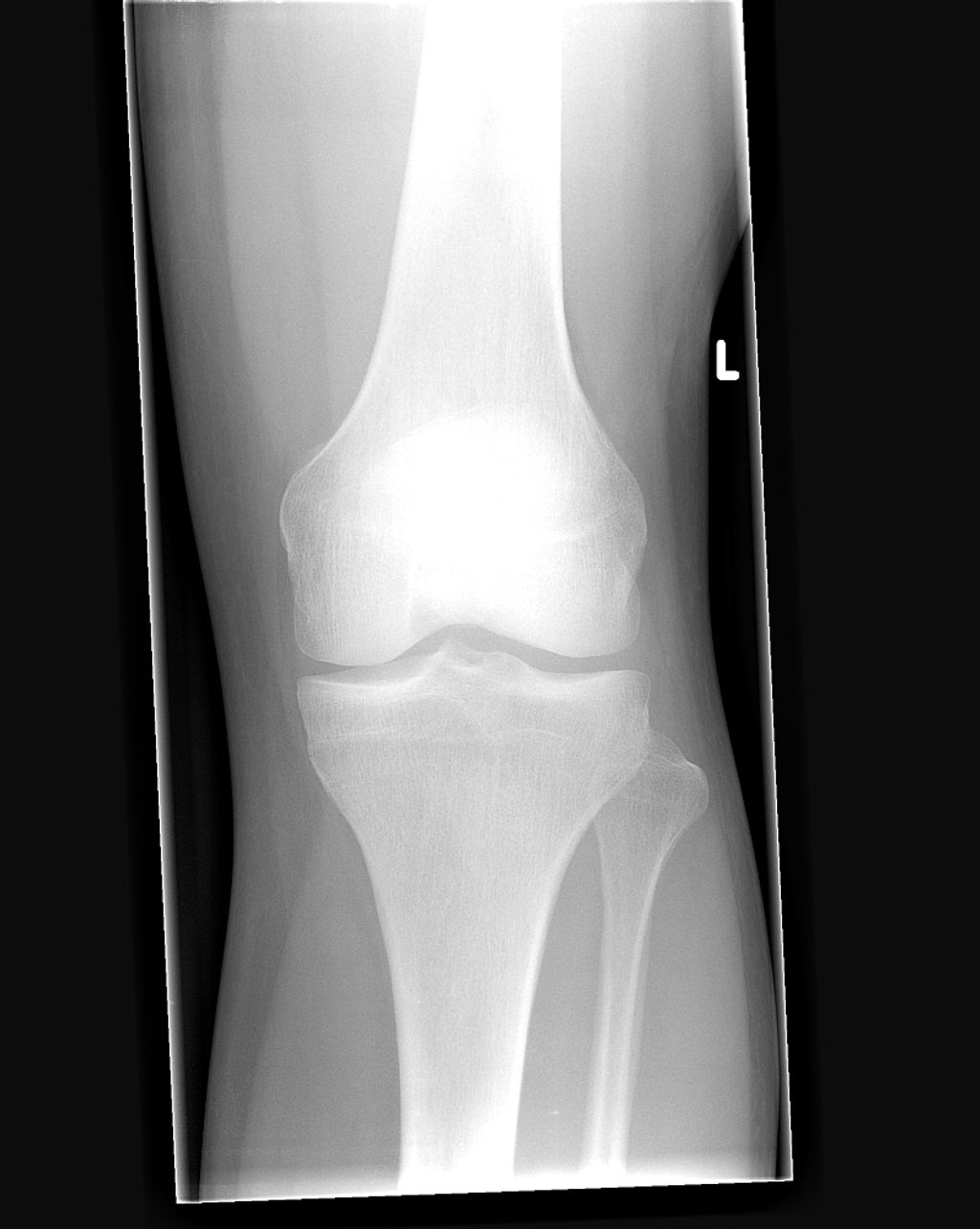
X-rays. Excellent for identifying bone fractures, joint space narrowing (a sign of cartilage loss), and bone spurs associated with osteoarthritis.
-
MRI Scans. The gold standard for visualizing soft tissue damage, including ligament tears, meniscus injuries, and cartilage defects that do not show up on X-ray.
-
Ultrasound. Useful for assessing tendons, bursae, and soft tissue in real-time, particularly for tendinitis and bursitis diagnoses.
-
Blood Tests. Ordered when an inflammatory or autoimmune cause (such as rheumatoid arthritis or gout) is suspected.
A new blood biomarker test can even predict the development of knee osteoarthritis up to 8 years before it is visible on an X-ray, with 85% accuracy. Early diagnosis means early action, and early action saves knees.
Treatment and Relief for Knee Pain Symptoms and Causes
The good news is this: the majority of knee pain symptoms and causes respond well to conservative, non-surgical treatment. You do not have to jump straight to the operating table, and in most cases, doing so would be premature.
Here is what the evidence actually supports in 2026:
Conservative (Non-Surgical) Treatments
-
RICE Protocol (Rest, Ice, Compression, Elevation). The foundational first-response treatment for acute injuries and flare-ups.
-
Physical Therapy. Targeted strengthening and mobility exercises that rebuild the support system around the knee. This is one of the most powerful tools available for long-term relief.
-
Compression Sleeves and Knee Braces. Provide external support, reduce swelling, and improve proprioception (your joint’s awareness of its own position). An excellent adjunct to any treatment plan.
-
Weight Management. Even modest reductions in body weight produce dramatic reductions in joint load and knee pain severity.
-
Anti-inflammatory Medications. Short-term use of NSAIDs can reduce pain and swelling, allowing you to participate in rehabilitation exercises more effectively.
-
Corticosteroid or Hyaluronic Acid Injections. For moderate-to-severe osteoarthritis, these injections can provide months of meaningful relief.
Surgical Options (When Truly Necessary)
-
Arthroscopy. A minimally invasive procedure used to repair or trim torn meniscus tissue and address certain cartilage defects.
-
ACL Reconstruction. A surgical procedure to rebuild a completely torn anterior cruciate ligament, typically using a tissue graft.
-
Total Knee Replacement. Reserved for severe, end-stage osteoarthritis that has not responded to all other treatments.
Did You Know?
Physical therapy can reduce the need for knee surgery by 40% in patients with degenerative knee conditions.
Source: WifiTalents 2026
Think about that number for a moment. Four out of ten people scheduled for knee surgery could potentially avoid the operating room entirely with the right rehabilitation program. That is not a small statistic. That is a life-changing one.
Preventing Knee Pain: Protecting Your Joints for the Long Term
Prevention is always more effective than treatment when it comes to joint health. The steps you take today directly influence how your knee feels five, ten, and twenty years from now.
Here are the most evidence-supported prevention strategies for 2026:
-
Maintain a healthy body weight. Reducing excess load is the single most impactful thing most people can do for their knee joints.
-
Strengthen the muscles around the knee. The quadriceps, hamstrings, hip abductors, and calf muscles all play a role in protecting the joint.
-
Warm up before exercise. A proper warm-up increases blood flow to joint structures and prepares tissues for loading.
-
Choose appropriate footwear. Supportive, low-heeled shoes reduce mechanical stress on the knee during every step.
-
Listen to your body. Pain during exercise is a signal, not a challenge to push through. Rest and modify activity when pain flares.
-
Use compression support proactively. For people with a history of knee hurt or high activity levels, a well-fitted knee sleeve during exercise provides valuable proprioceptive feedback and reduces swelling.
-
Address nutritional gaps. Adequate Vitamin D, calcium, and anti-inflammatory nutrients support joint tissue health from the inside out.
For a complete, resource-rich guide to every aspect of managing your joint health, we highly recommend reading through our comprehensive guide to understanding, managing, and overcoming knee pain.
Conclusion: Taking Control of Knee Pain Symptoms and Causes
Knee pain symptoms and causes are not a mystery. They follow patterns. They respond to evidence-based treatment. And they are far more manageable than most people realize, even when they have been hurting for years.
Whether your knee pain comes from a torn ligament, worn-down cartilage, arthritis, or years of repetitive strain, understanding what is happening inside your joint is the most empowering first step you can take. Knowledge turns confusion into a clear action plan.
The key facts to carry forward are straightforward. Recognize your symptoms early. Understand which cause category fits your experience. Take conservative treatment seriously before considering surgical options. And protect your joint proactively with the right support, movement habits, and body weight management.
Your knee does an extraordinary amount of work every single day. It deserves the same level of attention and care. Stop accepting pain as inevitable, and start treating it as the solvable problem it actually is.
“Getting out of bed should not feel like a workout. Understanding the cause of your knee pain is the first step to making sure it does not have to.”
Explore our full library of condition-specific resources below to find the information most relevant to your exact situation: