Are you experiencing knee pain or instability due to patellar malalignment? This condition can significantly impact daily activities and athletic performance. Effective management is crucial to alleviate symptoms and prevent further complications.
Patellar maltracking taping techniques offer a practical solution by providing stabilization and support to the knee. By applying specific knee taping techniques, individuals can experience relief from pain and improved knee function.
Key Takeaways
- Understanding the causes of patellar malalignment is crucial for effective management.
- Taping techniques can provide immediate relief from knee pain and instability.
- Proper application of patellar tracking tape is essential for optimal results.
- Combining taping with physical therapy can enhance recovery.
- Knee taping techniques can be adapted for various activities and lifestyles.
Understanding Patellar Maltracking
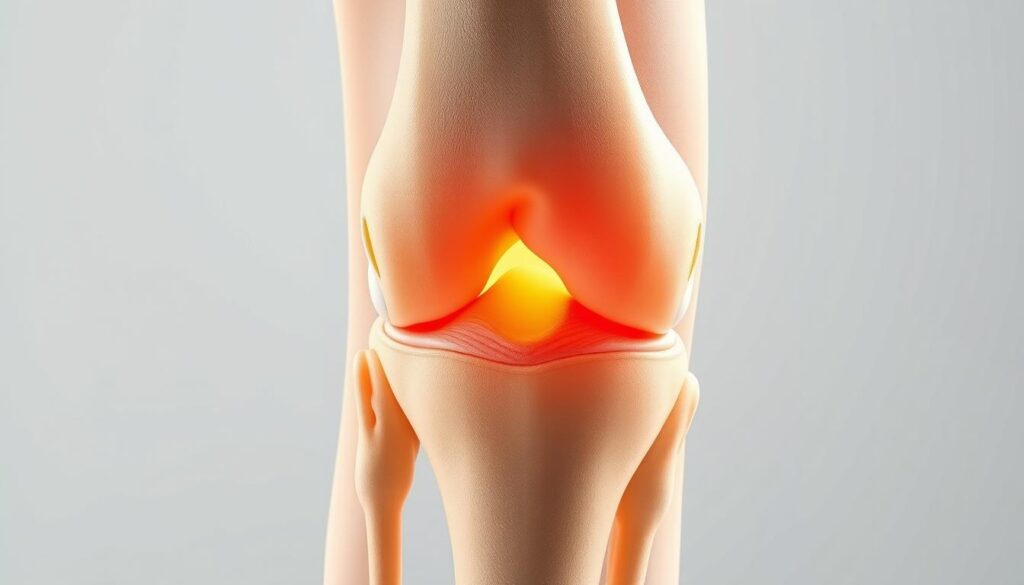
Understanding patellar maltracking is crucial for diagnosing and treating knee-related issues. Patellar maltracking refers to the abnormal movement of the patella (kneecap) within the femoral trochlear groove. This condition can lead to various knee problems, including pain and discomfort, especially during activities that stress the knee.
What is Patellar Maltracking?
Patellar maltracking occurs when the patella does not move smoothly within its groove. This can be due to several factors, including structural issues, muscle imbalance, and ligament damage. When the patella does not track correctly, it can cause friction and irritation, leading to pain and potentially more severe knee problems over time.
Causes of Patellar Maltracking
The causes of patellar maltracking are multifaceted. Structural problems in the legs, such as abnormal pronation or supination of the foot, can affect the alignment of the patella. Additionally, muscle imbalance around the knee, particularly weakness in the quadriceps or tightness in the iliotibial tract, can contribute to maltracking. Ligament damage or laxity around the patella can also play a significant role.
Activities that involve repetitive knee movements, such as running or jumping, can exacerbate these issues. Therefore, individuals engaged in sports or activities that stress the knee are more prone to experiencing patellar maltracking.
Symptoms to Look For
Identifying the symptoms of patellar maltracking is essential for early diagnosis and treatment. Common symptoms include knee pain, especially during activities like climbing stairs, squatting, or jumping. Tenderness around the patella and a grinding or clicking sensation when moving the knee are also indicative of patellar maltracking. In some cases, individuals may experience a feeling of the knee giving way or instability.
Recognizing these symptoms early can help in implementing appropriate treatments, such as patellar tracking exercises or taping for knee alignment, to alleviate discomfort and prevent further complications.
The Role of Taping in Treatment
Taping plays a crucial role in the treatment of patellar maltracking by providing support and realigning the patella. This non-invasive technique is used alongside other therapies to enhance treatment outcomes.
Benefits of Taping Techniques
Taping techniques offer several benefits for individuals suffering from patellar maltracking. The primary advantages include pain reduction, improved patellar alignment, and enhanced knee function. By providing external support, taping helps to stabilize the patella, thereby reducing the strain on the surrounding soft tissues.
The benefits of taping can be summarized in the following table:
| Benefit | Description |
|---|---|
| Pain Reduction | Taping helps to realign the patella, reducing pain caused by malalignment. |
| Improved Patellar Alignment | By providing external support, taping aids in correcting patellar malalignment. |
| Enhanced Knee Function | Taping supports the patella, improving overall knee function and stability. |
How Taping Supports the Patella
Taping supports the patella by mechanically stabilizing it, ensuring it tracks correctly within the femoral trochlear groove. This is particularly important during activities that exacerbate patellar maltracking symptoms, such as running or squatting.
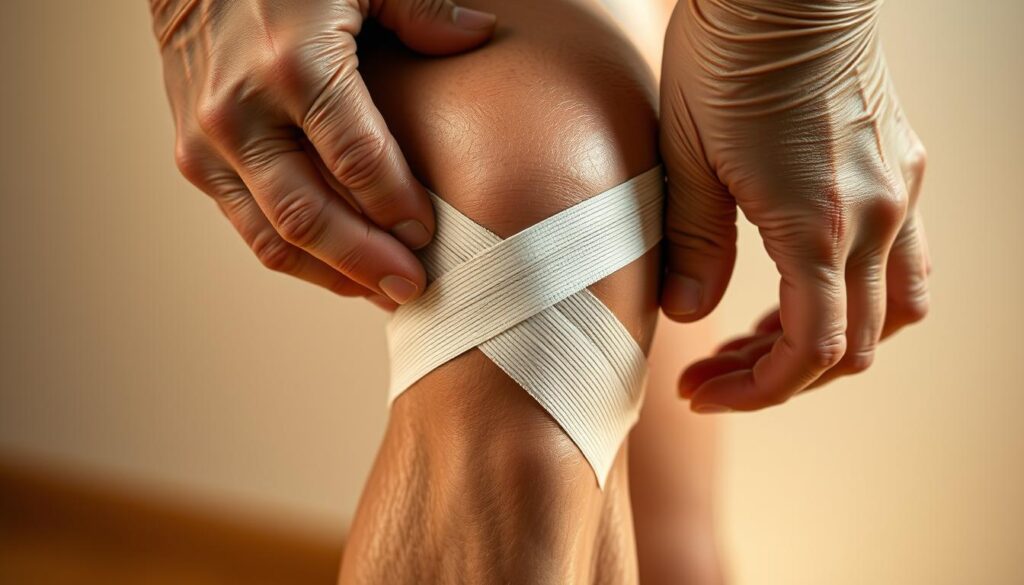
The application of patellar instability tape or knee taping techniques can significantly improve patellar tracking. By doing so, taping reduces the risk of further injury and alleviates pain, making it a valuable component of a comprehensive treatment plan for patellar malalignment.
Types of Taping Techniques
For individuals suffering from patellar maltracking, various taping techniques can provide relief and support. Taping is a versatile treatment method that can be tailored to the specific needs of the patient.
McConnell Taping
McConnell taping is a technique that focuses on correcting the alignment of the patella. It involves the application of tape to pull the patella into a more correct position, thereby alleviating pain and improving knee function.
Kinesiology Taping
Kinesiology taping is another method used to support the patella and surrounding tissues. This technique involves applying tape to the knee in a specific manner to provide support without restricting movement.
Traditional Athletic Taping
Traditional athletic taping provides rigid support to the knee, limiting excessive movement that could exacerbate patellar maltracking. This method is often used in conjunction with other treatments.
The following table summarizes the key differences between the taping techniques:
| Taping Technique | Primary Benefit | Application |
|---|---|---|
| McConnell Taping | Corrects patellar alignment | Used for patellar realignment |
| Kinesiology Taping | Provides support without restricting movement | Used for support and pain relief |
| Traditional Athletic Taping | Offers rigid support | Used for stability during activities |
Preparation for Taping
Proper preparation is the foundation of successful taping for patellar malalignment. Before applying any tape, it’s essential to ensure that the knee is properly assessed, the skin is prepared, and the right type of tape is selected.
Assessing the Knee Joint
Assessing the knee joint is a critical step in determining the most effective taping technique. This involves evaluating the alignment of the patella, checking for any swelling or inflammation, and assessing the range of motion. A thorough assessment helps in identifying the specific needs of the individual, allowing for a more tailored approach to taping.
The assessment should be conducted by a healthcare professional who can accurately diagnose the issue and recommend the appropriate taping technique. Key aspects to assess include patellar position, knee stability, and pain levels.
Cleaning the Skin
Cleaning the skin before applying tape is vital for ensuring that the tape adheres properly. Dirt, oils, and lotions can interfere with the adhesive, causing the tape to peel off prematurely. The skin should be cleaned with soap and water, and then dried thoroughly.
It’s also recommended to remove any hair from the area where the tape will be applied, as this can help improve adhesion and reduce discomfort when removing the tape.
Selecting the Right Tape
Selecting the right type of tape is crucial for effective taping. Different types of tape offer varying levels of support and flexibility. For example, rigid tape is often used for more support, while kinesiology tape provides flexibility and elasticity.
- Rigid Tape: Provides strong support and is often used for more severe cases of patellar malalignment.
- Kinesiology Tape: Offers flexibility and can be used for a range of activities without restricting movement.
- Cohesive Tape: Sticks to itself but not to skin, making it a good option for wrapping around the knee without causing irritation.
By carefully assessing the knee joint, cleaning the skin, and selecting the appropriate tape, individuals can ensure that their taping technique is effective in addressing patellar malalignment.
Step-by-Step Guide to Taping Techniques
For individuals dealing with patellar maltracking, mastering taping techniques can be a game-changer. Taping provides the necessary support to the patella, helping to alleviate symptoms associated with patellar maltracking.
There are several taping techniques, but this section will focus on two of the most commonly used methods: McConnell taping and kinesiology taping. Understanding the steps involved in each technique is crucial for effective application.
McConnell Taping Steps
McConnell taping is a technique that involves applying tape to the patella to correct its alignment and movement. Here are the steps to follow:
- Prepare the skin: Ensure the skin is clean and dry.
- Apply the base strip: Place a piece of tape along the medial (inner) border of the patella.
- Correct the patella: Gently move the patella into the correct position.
- Secure with additional strips: Apply additional strips of tape to secure the patella in place.
Kinesiology Taping Steps
Kinesiology taping involves applying a specific type of tape that is designed to stretch and move with the body. The steps for kinesiology taping are as follows:
- Measure and cut the tape: Measure the length of tape needed and cut it accordingly.
- Apply the tape: Place the tape on the skin, starting from the center and working outwards.
- Stretch the tape: Gently stretch the tape to the desired tension.
- Secure the ends: Ensure the ends of the tape are securely attached to the skin.
By following these steps, individuals can effectively use McConnell taping and kinesiology taping to manage patellar maltracking. It’s essential to practice these techniques to ensure they are applied correctly.
Maintaining Proper Tape Position
The effectiveness of patellar tracking tape largely depends on its correct placement. Proper positioning ensures that the tape provides the necessary support to the patella, facilitating correct alignment and reducing discomfort.
Maintaining the correct position of the tape is crucial for its effectiveness. If the tape is not applied correctly, it can lead to reduced efficacy or even skin irritation. Therefore, understanding the importance of alignment and being aware of common mistakes to avoid are essential for effective taping.
Importance of Alignment
Correct alignment is vital when applying patellar realignment taping. The tape should be positioned in a way that it supports the patella and promotes proper tracking. Misalignment can lead to inadequate support, potentially worsening the condition.
“Proper taping techniques can significantly improve patellar alignment, reducing pain and discomfort associated with maltracking.”
A well-aligned tape application not only enhances the therapeutic effect but also minimizes the risk of complications. It is essential to assess the knee joint thoroughly before applying the tape to determine the most appropriate alignment.
| Alignment Aspect | Importance | Consequence of Misalignment |
|---|---|---|
| Patellar Positioning | Ensures proper tracking | Increased pain and discomfort |
| Tape Tension | Affects support and comfort | Skin irritation or reduced efficacy |
| Application Technique | Influences overall effectiveness | Inadequate support or complications |
Common Mistakes to Avoid
Several common mistakes can compromise the effectiveness of taping for knee alignment. These include applying the tape too tightly, which can cause skin irritation, and incorrect positioning, which can fail to provide adequate support.
- Applying tape with excessive tension
- Failing to clean the skin before application
- Not assessing the knee joint properly
By being aware of these potential pitfalls, individuals can take steps to ensure that their taping technique is both safe and effective. Regular monitoring and adjustments as needed can help maintain optimal tape position and overall therapeutic benefit.
![]()
Taping for Different Activity Levels
Different activity levels require adjustments in taping techniques to effectively manage patellar instability. Whether an individual is engaging in high-impact sports or performing everyday tasks, the application of knee taping techniques can be tailored to provide the necessary support.
The key to effective taping is understanding the specific demands of the activity and how they impact the knee joint. For instance, athletes involved in high-impact activities require taping that not only supports the patella but also withstands the rigors of their sport.
Athletes and High-Impact Activities
Athletes participating in sports such as basketball, soccer, or tennis can benefit from patellar instability tape that is designed to provide additional support during high-impact movements. The taping technique used for these athletes may involve more rigid tape or a specific application method to ensure the patella remains in alignment during intense activity.
- Use of rigid tape for added support
- Specific application techniques to enhance patellar stability
- Consideration of the sport’s specific demands on the knee
Research on the effectiveness of taping for patellar malalignment in athletes can be found in various studies, including those published in medical journals such as PMC.
Everyday Activities and Taping
For individuals who are not athletes but still experience patellar maltracking during everyday activities, the taping technique can be adjusted to provide comfort and support without restricting movement. Taping for patellar malalignment in these cases focuses on providing a balance between support and flexibility.
The tape used for everyday activities may be less rigid, allowing for a full range of motion while still offering the necessary patellar support. This approach helps individuals manage their condition effectively while going about their daily routines.
Frequency and Duration of Taping
To maximize the benefits of patellar maltracking taping techniques, it’s essential to know the right duration and frequency of application. The goal is to balance continuous support for the patella with the need to maintain skin health.
Effective taping for knee alignment requires understanding how long to keep the tape on. Generally, the tape should be left on for several days, but this can vary based on individual skin types and activity levels. It’s crucial to monitor skin condition closely to avoid irritation or other adverse effects.
How Long to Keep the Tape On
The duration for which the tape is left on can depend on several factors, including the type of tape used, individual skin sensitivity, and the specific activity level of the person. For most people, leaving the tape on for 3 to 5 days is a good starting point. However, it’s essential to inspect the skin daily for any signs of irritation, even if the tape is still securely in place.
When to Reapply the Tape
Reapplying the tape should be done based on the condition of the skin and the tape’s adherence. If the tape starts to peel off or loses its effectiveness, it’s time to reapply. Reapplication should also be considered if there’s significant skin irritation, as this could be a sign that the tape needs to be removed or replaced with a different type.
![]()
For individuals using taping as part of their patellar tracking correction regimen, understanding the balance between support and skin health is key. As one expert notes,
“The key to successful taping is not just the technique, but also how well you manage the skin and tape interface.”
By carefully managing the frequency and duration of taping, individuals can maximize the benefits of patellar maltracking taping techniques while minimizing potential drawbacks.
Caring for Your Skin
To avoid skin complications, it’s vital to understand how to care for your skin while using taping for patellar malalignment. Proper skin care is essential when using knee taping techniques to prevent irritation and ensure the skin remains healthy.
Preventing Skin Irritation
Preventing skin irritation begins with preparing your skin before applying patellar tracking tape. Ensure your skin is clean and dry. Remove any oils, lotions, or dirt that might interfere with the tape’s adhesive. It’s also advisable to shave the area if you have excessive hair to ensure better adhesion and easier removal.
Another crucial step is to check for any signs of skin irritation or allergic reactions to the tape. If you experience redness, itching, or any discomfort, consider using a hypoallergenic tape or consulting a healthcare professional for advice.
Tips for Safe Removal of Tape
Removing knee taping techniques tape requires care to avoid causing skin irritation or injury. Start by gently peeling back the edge of the tape, working slowly across the skin. Avoid pulling the tape off quickly or at a sharp angle, as this can cause skin tears or irritation.
If the tape is stubborn, you can use a small amount of oil or adhesive remover to help loosen it. Gently massage the oil into the adhesive before attempting to remove the tape again. After removal, clean the area with soap and water to remove any remaining adhesive residue.
By following these guidelines, you can minimize the risk of skin complications when using taping for patellar malalignment or other knee taping techniques. Proper care and caution will help ensure that you can benefit from these techniques without adverse effects on your skin.
Combining Taping with Other Treatments
Combining taping with other therapeutic approaches can enhance the management of patellar maltracking. A comprehensive treatment plan often involves a multi-faceted approach, incorporating various therapies to achieve optimal results.
Physical Therapy Options
Physical therapy plays a crucial role in the treatment of patellar maltracking. Techniques such as manual therapy, including mobilization and manipulation, can help improve patellar alignment and reduce discomfort. Additionally, physical therapists can provide personalized exercise programs to strengthen the surrounding muscles, thereby enhancing patellar stability.
Some of the physical therapy options include:
- Patellar mobilization to improve tracking and reduce pain
- Strengthening exercises for the quadriceps and hip muscles
- Stretching exercises to improve flexibility
Strengthening Exercises
Strengthening the muscles around the knee, particularly the quadriceps and hip muscles, is essential for improving patellar tracking and stability. Exercises such as squats, lunges, and leg press can be beneficial. It’s also important to focus on exercises that strengthen the hip muscles, as weak hip muscles can contribute to patellar maltracking.
| Exercise | Muscle Group | Benefit |
|---|---|---|
| Squats | Quadriceps, Hamstrings, Glutes | Improves overall lower limb strength and stability |
| Lunges | Quadriceps, Hamstrings, Glutes | Enhances balance and strengthens the muscles around the knee |
| Leg Press | Quadriceps, Hamstrings | Strengthens the quadriceps and hamstrings, supporting patellar stability |
As noted by a physical therapy expert,
“A well-structured exercise program is crucial for patients with patellar maltracking. Strengthening the surrounding muscles can significantly improve patellar tracking and reduce symptoms.”
By combining taping techniques with physical therapy and strengthening exercises, individuals with patellar maltracking can experience improved knee function and reduced pain. This comprehensive approach addresses the condition from multiple angles, providing a more effective management strategy.
Assessing the Effectiveness of Taping
The effectiveness of taping techniques for patellar maltracking can be evaluated by monitoring changes in symptoms and pain levels. This assessment is crucial for understanding whether the taping is providing the desired support and correction to the patella.
Monitoring Symptoms and Pain Levels
To effectively monitor symptoms, it’s essential to keep a record of pain levels and any changes in knee function. This can be done using a pain diary or a mobile app designed for tracking symptoms. Key areas to monitor include:
- Pain levels during daily activities
- Swelling or inflammation around the knee
- Instability or feeling of the patella slipping
- Difficulty in bending or straightening the knee
By closely monitoring these symptoms, individuals can determine if the taping is effective in providing relief and supporting the patella. For more information on the benefits of taping, research studies such as those found on PubMed Central can offer valuable insights.
When to Consult a Professional
If symptoms persist or worsen despite taping, it’s crucial to consult a healthcare professional for further evaluation. A professional can assess the knee joint and provide guidance on adjusting the taping technique or recommend alternative treatments. Signs that necessitate professional consultation include:
- Increased pain or swelling
- No improvement in symptoms after consistent taping
- Difficulty walking or performing daily activities
Consulting a professional ensures that the taping technique is correctly applied and that any underlying issues are addressed. This proactive approach can lead to more effective management of patellar maltracking.
Conclusion and Next Steps
Effective management of patellar maltracking involves a combination of proper diagnosis, treatment, and ongoing care. By understanding and applying the appropriate knee taping techniques, individuals can experience significant relief from symptoms associated with patellar maltracking.
Key Takeaways
The techniques discussed, including McConnell taping and kinesiology taping, offer valuable methods for patellar realignment taping. These methods help in stabilizing the patella and reducing discomfort. It’s essential to remember that the effectiveness of patellar tracking tape depends on proper application and maintenance.
Ongoing Management
For long-term relief and to prevent the recurrence of patellar maltracking symptoms, it’s crucial to continue practicing the taping techniques as needed and to incorporate strengthening exercises into your routine. Consulting with a healthcare professional can provide personalized guidance tailored to your specific condition and needs.
FAQ
What is patellar maltracking, and how does it affect the knee?
Patellar maltracking refers to the abnormal movement of the patella (kneecap) within the femoral trochlear groove, leading to knee pain, instability, and potentially, further injury. It can be caused by structural issues, muscle imbalance, or ligament damage.
How do taping techniques help in managing patellar maltracking?
Taping techniques, such as McConnell taping and kinesiology taping, help realign the patella, reduce pain, and provide support to the knee, making them a valuable treatment option for managing patellar maltracking.
What are the different types of taping techniques used for patellar maltracking?
The different types of taping techniques used include McConnell taping, kinesiology taping, and traditional athletic taping, each with its specific applications and benefits.
How do I prepare my knee for taping?
To prepare for taping, assess the knee joint, clean the skin thoroughly, and choose the right tape for your specific needs, ensuring a proper and effective taping application.
Can taping be used for different activity levels, such as high-impact activities or everyday tasks?
Yes, taping can be adjusted based on the individual’s activity level, providing support for both high-impact activities and everyday tasks, helping to manage patellar maltracking in various contexts.
How often should I reapply the tape, and how long can I keep it on?
The frequency and duration of taping depend on individual needs, balancing the need for continuous support with skin health considerations; it’s essential to follow guidelines for reapplication and removal.
How can I prevent skin irritation when using taping techniques?
To prevent skin irritation, ensure the skin is clean and dry before applying tape, avoid using tape with harsh adhesives, and follow proper removal techniques to maintain skin health.
Can taping be used in conjunction with other treatments, such as physical therapy or strengthening exercises?
Yes, taping can be effectively combined with other treatments, including physical therapy options and strengthening exercises, to provide a comprehensive approach to managing patellar maltracking.
How do I assess the effectiveness of taping in managing my patellar maltracking?
To assess the effectiveness of taping, monitor your symptoms and pain levels, and consult a healthcare professional if you experience persistent or worsening symptoms, or if you need further guidance on adjusting your taping technique.
What are some common mistakes to avoid when applying tape for patellar maltracking?
Common mistakes to avoid include incorrect alignment, applying too much tension, or not removing the tape properly, which can lead to reduced effectiveness or skin irritation.
Are there specific exercises that can be done in conjunction with taping to help manage patellar maltracking?
Yes, strengthening exercises targeting the muscles around the knee, such as the quadriceps and hip stabilizers, can be beneficial when used alongside taping techniques to help manage patellar maltracking.