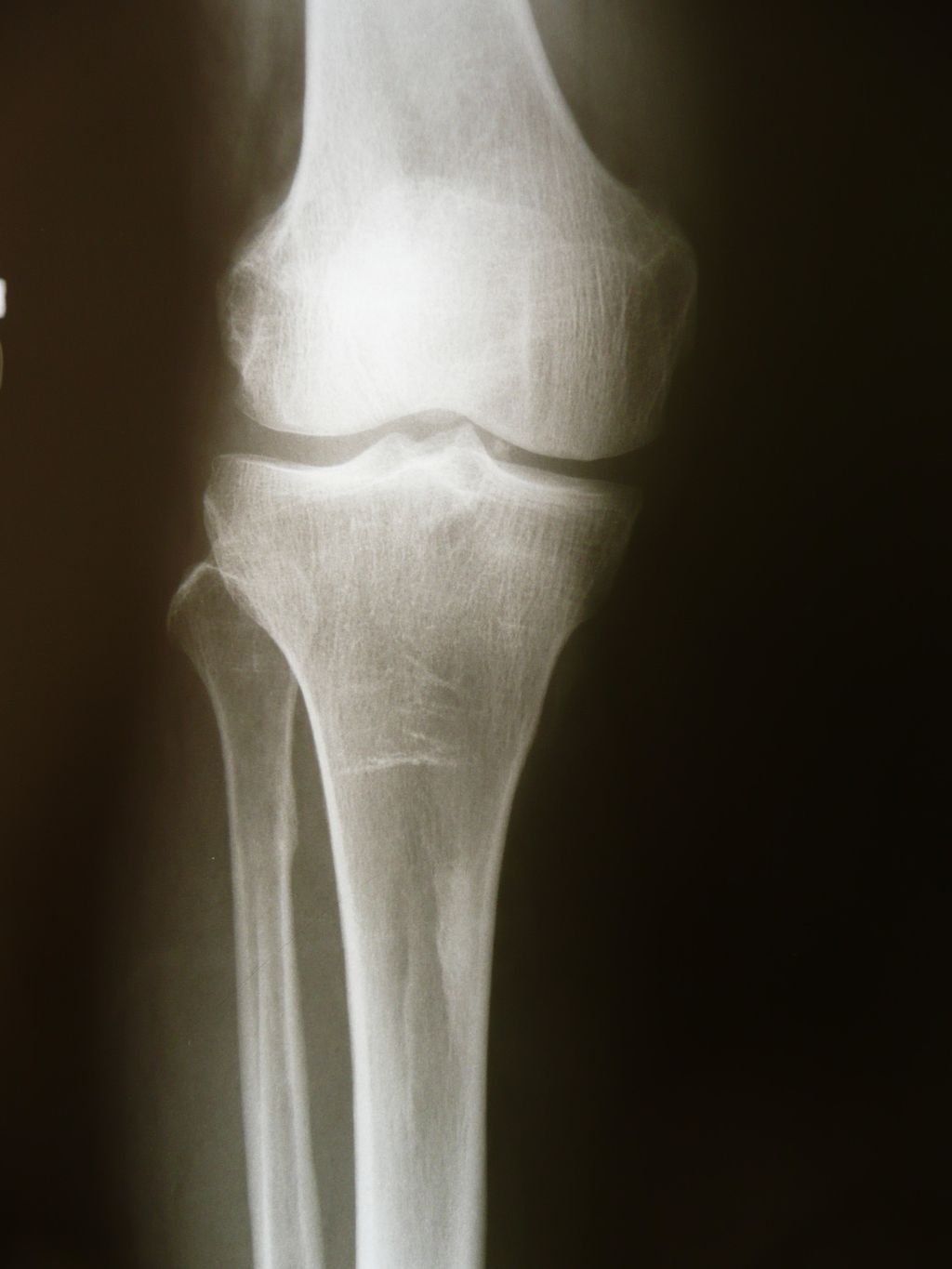
At some point in our lives, many of us may experience knee pain or discomfort. This can be attributed to various factors, one of which is knee osteoarthritis. Understanding the causes of knee osteoarthritis is crucial in order to better manage and prevent its progression.
Knee osteoarthritis is primarily caused by the degeneration of the knee joint, specifically the articular cartilage. This degeneration happens gradually and is often characterized by wear and tear. It can be further divided into two types: primary and secondary knee osteoarthritis.
Primary knee osteoarthritis refers to articular degeneration without any known underlying reason. On the other hand, secondary knee osteoarthritis is caused by factors such as abnormal concentration of force across the knee joint or abnormal articular cartilage, which can be seen in conditions like rheumatoid arthritis.
The contributing factors of knee osteoarthritis can vary from individual to individual. However, some common risk factors include knee cartilage wear and tear, previous injuries or trauma to the knee, joint deformities, and certain metabolic diseases. Additionally, age, genetics, and gender can also contribute to the development of knee osteoarthritis.
Identifying these risk factors and understanding the triggers and contributing factors of knee osteoarthritis can help us make informed decisions about prevention, management, and treatment options. It is important to note that while there are no proven disease-modifying agents for knee osteoarthritis, various conservative measures and surgical interventions are available to alleviate symptoms and improve quality of life for those affected.
In the following sections, we will delve deeper into the etiology, risk factors, pathophysiology, epidemiology, and clinical symptoms of knee osteoarthritis, providing a comprehensive understanding of this common degenerative joint disease.
Etiology of Knee Osteoarthritis
Knee osteoarthritis, a prevalent degenerative joint disease, can be categorized into two types: primary and secondary. Primary knee osteoarthritis occurs when articular cartilage degenerates without a known cause. It is commonly associated with age-related wear and tear on the knee joint. On the other hand, secondary knee osteoarthritis is caused by specific factors such as post-traumatic injuries, congenital or limb malformations, abnormal joint forces, or certain diseases like rheumatoid arthritis. Understanding the etiology of knee osteoarthritis is crucial for developing effective management strategies.
Primary knee osteoarthritis is characterized by articular cartilage degeneration without any apparent underlying reason. It is often associated with factors such as advancing age, obesity, and genetic predisposition. The gradual breakdown of cartilage results in joint pain, stiffness, and limited mobility.
Secondary knee osteoarthritis, on the other hand, is caused by identifiable factors that contribute to the deterioration of the knee joint. These factors include trauma, such as sports injuries or accidents, congenital or limb malformations, abnormal forces exerted on the joint, and certain chronic conditions like rheumatoid arthritis.
Regardless of the type, knee osteoarthritis leads to articular cartilage degradation and eventually affects the overall function of the knee joint. By understanding the etiology of knee osteoarthritis, healthcare professionals can tailor treatment plans and interventions to address the specific underlying causes and improve patient outcomes.
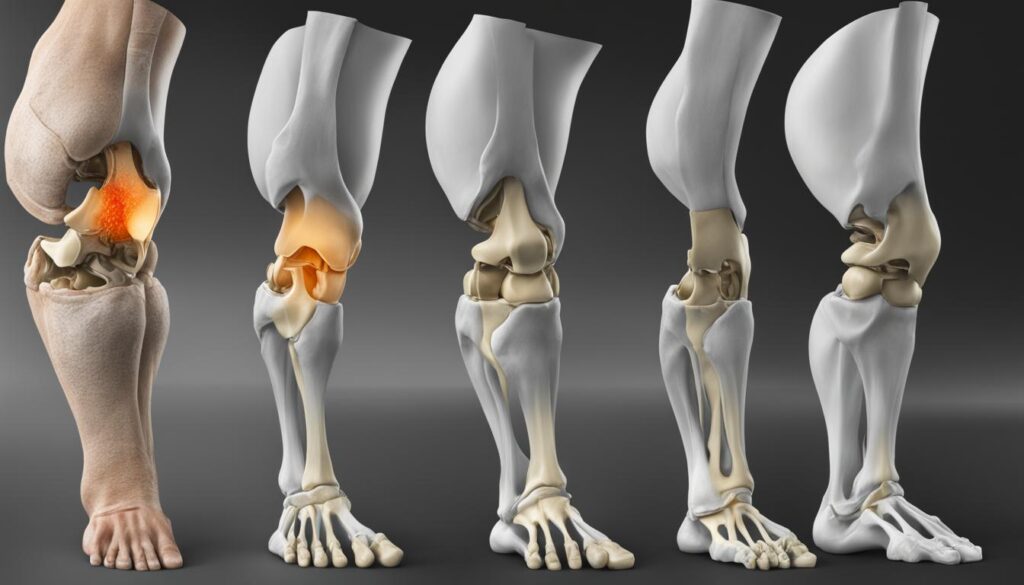
Risk Factors for Knee Osteoarthritis
Various risk factors contribute to the development of knee osteoarthritis. It’s important to understand these risk factors to prevent and intervene early in the progression of the disease.
Modifiable Risk Factors
- Articular Trauma: Injuries to the knee joint, such as ligament tears or fractures, can increase the risk of developing knee osteoarthritis later in life.
- Occupation-related Factors: Prolonged standing and repetitive knee bending, which are common in occupations that require heavy physical labor, can contribute to knee joint degeneration.
- Muscle Weakness or Imbalance: Weak or imbalanced muscles around the knee can lead to abnormal joint forces and increased stress on the knee joint, increasing the risk of osteoarthritis.
- Weight: Excess weight puts additional stress on the knee joint, accelerating the wear and tear of articular cartilage and increasing the risk of knee osteoarthritis.
- Metabolic Syndrome: Conditions such as obesity, high blood pressure, insulin resistance, and abnormal blood lipid levels that make up metabolic syndrome can contribute to the development of knee osteoarthritis.
Non-modifiable Risk Factors
- Gender: Females are more commonly affected by knee osteoarthritis compared to males.
- Age: Advanced age increases the risk of knee osteoarthritis due to the natural wear and tear of articular cartilage over time.
- Genetics: Certain genetic factors can predispose individuals to develop knee osteoarthritis, including inherited abnormalities in the structure of the joint or cartilage.
- Race: Some ethnicities, such as African Americans, have a higher prevalence of knee osteoarthritis compared to other populations.
In addition to these risk factors, factors such as previous joint injuries, repeated stress on the joint, bone deformities, and certain metabolic diseases can also increase the risk of knee osteoarthritis. By identifying and understanding these risk factors, healthcare professionals can implement preventive measures and early intervention strategies to minimize the impact of knee osteoarthritis.

Epidemiology of Knee Osteoarthritis
Knee osteoarthritis is a highly prevalent condition, making it the most common type of arthritis affecting individuals worldwide. With the global population aging and increasing rates of obesity, the prevalence of knee osteoarthritis is expected to rise in the coming years.
Demographically, the prevalence of symptomatic knee osteoarthritis is influenced by both gender and age. Studies have shown that approximately 13% of women and 10% of men aged 60 and older experience symptomatic knee osteoarthritis. Among individuals older than 70, the prevalence can be as high as 40%. These statistics highlight the significant impact of knee osteoarthritis in the older population.
In terms of incidence, knee osteoarthritis affects a considerable number of individuals each year. The incidence of symptomatic knee osteoarthritis is estimated to be around 240 cases per 100,000 people annually. However, it is important to note that not all individuals with radiographic evidence of knee osteoarthritis will experience symptomatic manifestations of the disease.
Understanding the epidemiology of knee osteoarthritis is crucial for healthcare professionals in terms of resource allocation, management strategies, and public health interventions. By comprehending the prevalence, incidence, and demographics of knee osteoarthritis, we can better address the needs of individuals affected by this condition and work towards improving their quality of life.
Pathophysiology of Knee Osteoarthritis
The pathophysiology of knee osteoarthritis involves the progressive degradation of articular cartilage. In healthy cartilage, there is a delicate balance between collagen, proteoglycans, and chondrocytes. However, in osteoarthritis, this equilibrium is disrupted, leading to the loss of cartilage integrity.
Matrix metalloproteases (MMPs) play a crucial role in the degradation of the cartilage matrix. These enzymes are overexpressed in osteoarthritis, resulting in the breakdown of collagen and proteoglycans. As a result, the cartilage becomes thinner and less resistant to mechanical stress.
In response to the cartilage damage, chondrocytes, the cells responsible for maintaining and repairing cartilage, attempt to counteract the matrix degradation. They secrete tissue inhibitors of MMPs (TIMPs) to inhibit the activity of MMPs, and they increase the synthesis of proteoglycans. However, these reparative processes are insufficient to fully restore the damaged cartilage.
The progressive degradation of articular cartilage in knee osteoarthritis ultimately leads to the development of fissures, cracks, and erosion. The loss of cartilage cushioning between the bones results in increased friction and can cause pain, stiffness, and swelling in the knee joint.
While knee osteoarthritis is commonly associated with aging, it is important to recognize that it is a distinct disease characterized by specific biochemical changes in the cartilage. Understanding the pathophysiology of knee osteoarthritis is essential for developing targeted treatments and interventions that can slow down or prevent the progression of the disease.
Clinical Symptoms of Knee Osteoarthritis
The clinical symptoms of knee osteoarthritis can vary among individuals, but they typically include:
- Gradual onset knee pain: Many individuals with knee osteoarthritis experience gradual onset pain, which may start as a mild discomfort and progress over time.
- Increased pain with activity: Knee pain often worsens with activities such as walking, climbing stairs, or prolonged standing.
- Knee stiffness: Stiffness is a common symptom of knee osteoarthritis, especially after periods of rest or inactivity.
- Knee swelling: Some individuals may notice swelling around the knee joint, which can be accompanied by warmth or redness.
- Pain after prolonged periods of sitting or resting: After sitting or resting for an extended period, individuals with knee osteoarthritis may experience pain or stiffness when they first stand up and start moving.
- Pain that worsens over time: The pain associated with knee osteoarthritis tends to progress gradually, worsening over time if left untreated.
These clinical symptoms can significantly impact an individual’s functional capacity and quality of life. Recognizing and understanding the symptoms of knee osteoarthritis is crucial for timely diagnosis and appropriate management.
| Symptoms | Description |
|---|---|
| Gradual onset knee pain | Slowly developing pain in the knee joint |
| Increased pain with activity | Pain worsens during movement or weight-bearing activities |
| Knee stiffness | Feeling of tightness or limited range of motion in the knee |
| Knee swelling | Swelling or fluid accumulation around the knee joint |
| Pain after prolonged periods of sitting or resting | Pain or stiffness when standing up after periods of inactivity |
| Pain that worsens over time | Pain becomes more severe and persistent as knee osteoarthritis progresses |
Conclusion
Knee osteoarthritis is a prevalent degenerative joint disease characterized by the progressive loss of articular cartilage. The causes of knee osteoarthritis can be classified into primary and secondary factors, with wear and tear playing a significant role. Various risk factors, both modifiable and non-modifiable, contribute to the development of knee osteoarthritis. Understanding these factors is crucial for implementing appropriate prevention and early intervention strategies.
The pathophysiology of knee osteoarthritis involves the disruption of cartilage equilibrium, leading to the degradation of collagen and proteoglycans. This process occurs due to the overexpression of matrix metalloproteases, resulting in cracking, fissuring, and erosion of the articular cartilage. Clinically, knee osteoarthritis presents with symptoms such as knee pain, stiffness, swelling, and functional limitations. Recognizing and understanding these symptoms is essential for timely diagnosis and effective management.
In conclusion, knee osteoarthritis is a complex condition influenced by various causes, risk factors, and pathophysiological changes in the joint. By comprehending the underlying factors and recognizing the clinical manifestations, healthcare professionals can develop targeted treatment plans to enhance patients’ quality of life. Continuous research and education in the field of knee osteoarthritis are crucial for advancing the understanding and management of this prevalent joint disease.
FAQ
What are the causes of knee osteoarthritis?
Knee osteoarthritis is primarily caused by wear and tear and progressive loss of articular cartilage. It can be categorized into primary, which has no known underlying cause, and secondary, which is caused by factors like abnormal joint forces or diseases.
What are the risk factors for knee osteoarthritis?
Risk factors for knee osteoarthritis include modifiable factors like articular trauma, occupation-related factors, muscle weakness or imbalance, weight, and metabolic syndrome. Non-modifiable factors include gender, age, genetics, race, joint injuries, repeated stress on the joint, bone deformities, and certain metabolic diseases.
What is the prevalence of knee osteoarthritis?
The prevalence of symptomatic knee osteoarthritis varies by gender and age. Approximately 13% of women and 10% of men aged 60 and older experience symptomatic knee osteoarthritis. Among individuals older than 70, the prevalence can be as high as 40%. The incidence of symptomatic knee osteoarthritis is around 240 cases per 100,000 people per year.
What is the pathophysiology of knee osteoarthritis?
Knee osteoarthritis is characterized by the progressive degradation of articular cartilage. The equilibrium between collagen, proteoglycans, and chondrocytes is disrupted, leading to the overexpression of matrix metalloproteases (MMPs) and the loss of collagen and proteoglycans. Chondrocytes attempt to repair the damage but are unable to fully restore the cartilage, resulting in its degradation.
What are the clinical symptoms of knee osteoarthritis?
Clinical symptoms of knee osteoarthritis include gradual onset knee pain, increased pain with activity, knee stiffness, knee swelling, pain after prolonged periods of sitting or resting, and pain that worsens over time.