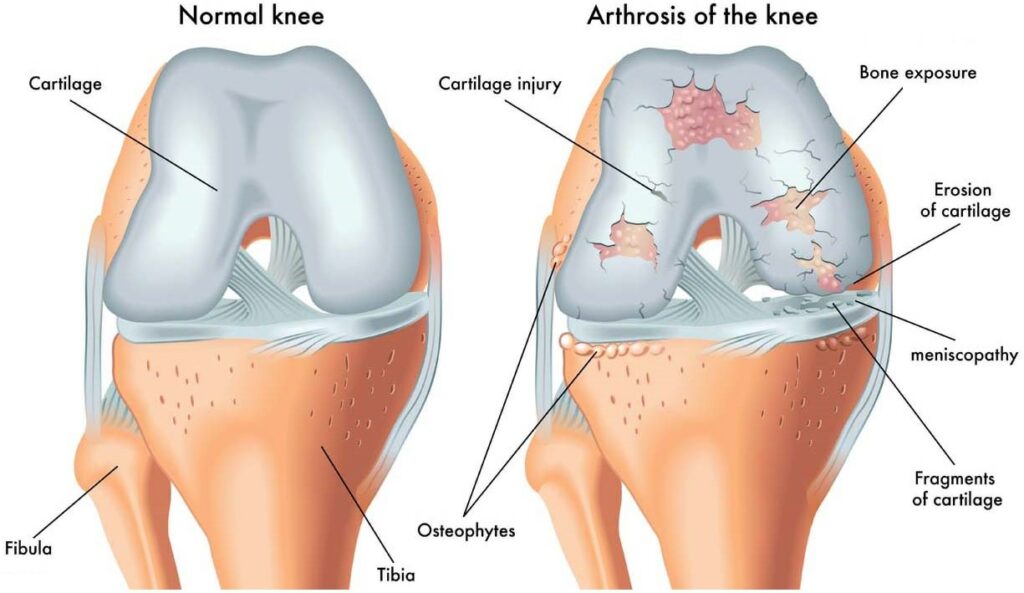
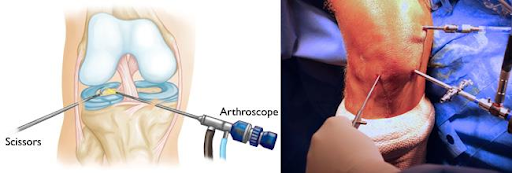
The knee joint is a complex and vital structure that plays a crucial role in supporting the body and facilitating movement. Understanding the functions of the knee bones is essential for comprehending the biomechanics and stability of the knee joint. In this article, we will explore the structure of the knee joint, the biomechanics of knee movement, and the importance of knee joint stability in detail.
Key Takeaways
- The knee joint is composed of the femur, tibia, and patella, each serving distinct functions in movement and weight-bearing.
- Flexion and extension are the primary movements of the knee joint, while rotational movements are also possible.
- The ligaments and tendons of the knee play a crucial role in providing stability and support during movement.
- The menisci contribute to knee joint stability by distributing forces and absorbing shock, while muscles surrounding the knee joint provide dynamic stability.
- Understanding the functions of knee bones is essential for comprehending the biomechanics and stability of the knee joint.
The Structure of the Knee Joint
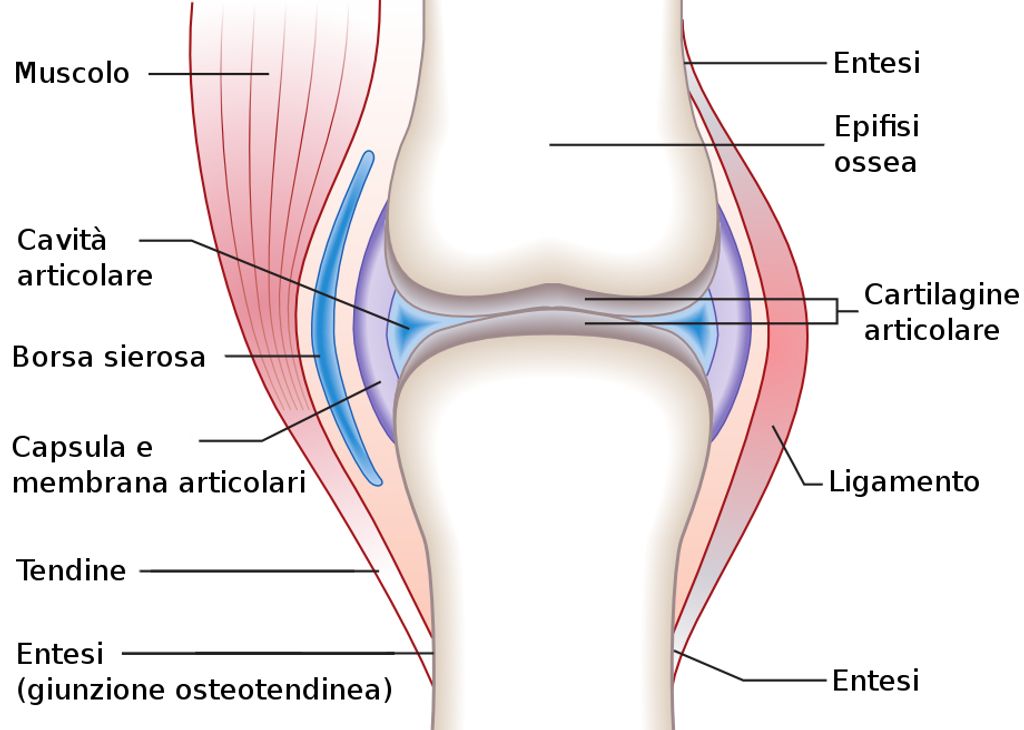
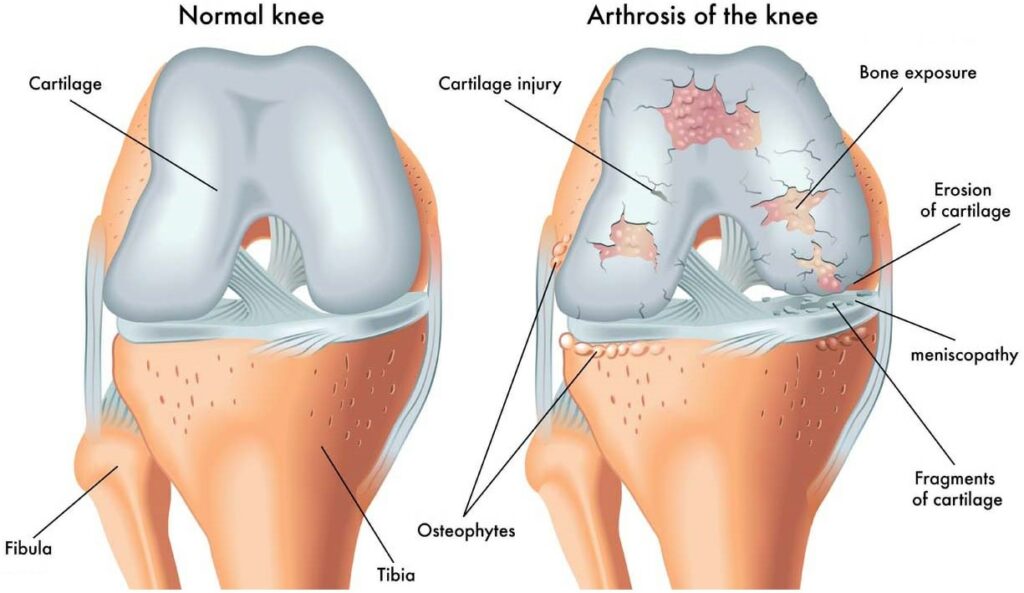
Anatomy of the Femur and Tibia
In our exploration of knee anatomy, we encounter the femur and tibia, the two principal bones that form the knee joint. The femur, or thigh bone, is the longest and strongest bone in the human body, anchoring the muscles that power movement. Its distal end articulates with the tibia, creating the hinge that is central to knee function.
The tibia, commonly referred to as the shinbone, supports the body’s weight and aligns with the femur to facilitate movement. At its proximal end, the tibia expands to form the tibial plateau, a critical load-bearing area that interfaces with the femur.
Understanding the relationship between these bones is fundamental to grasping knee mechanics. Here’s a quick overview of their attributes:
- Femur: Longest bone, supports thigh muscles
- Tibia: Weight-bearing bone, forms tibial plateau
Tip: Regular exercise can help maintain the strength and integrity of the bones, reducing the risk of injury to the knee joint.
Function of the Patella
We often overlook the critical role the patella, or kneecap, plays in our knee joint’s function. This small bone, nestled within the quadriceps tendon, serves as a fulcrum to increase the leverage of the tendon. This, in turn, enhances the force of the quadriceps muscle as it extends the knee.
The patella also protects the knee joint by providing a hard surface that deflects compressive forces away from the femoral condyles during activities like jumping or running. It’s essential for the proper tracking of the knee as it bends and straightens.
- Proper patellar function is crucial for maintaining knee health and preventing injury. Here’s a simple list of the patella’s functions:
- Increases leverage of the quadriceps tendon
- Enhances force of quadriceps muscle during knee extension
- Protects knee joint from compressive forces
- Assists in proper tracking of the knee during movement
Tip: Regular strengthening exercises for the quadriceps can help maintain the patella’s alignment and prevent knee pain.
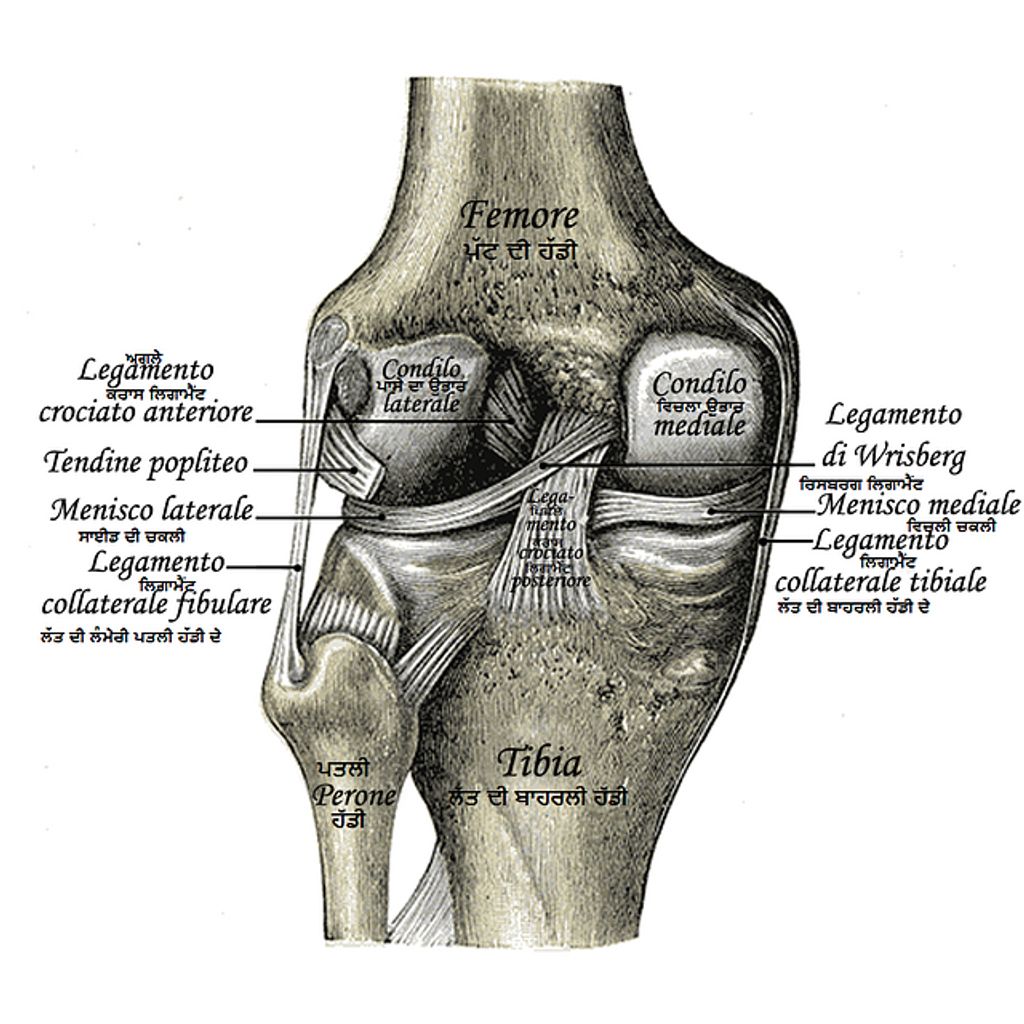
Ligaments and Tendons of the Knee
In our exploration of knee anatomy, we recognize the critical role of ligaments and tendons. These fibrous structures work in concert to provide stability and facilitate movement. Ligaments, such as the anterior cruciate ligament (ACL) and the posterior cruciate ligament (PCL), are key to preventing excessive forward and backward motion of the tibia. On the other hand, the medial and lateral collateral ligaments (MCL and LCL) resist sideways motion, ensuring our knees do not buckle during lateral stress.
Tendons, notably the patellar tendon, connect muscles to bones, allowing us to execute the powerful actions required for walking, running, and jumping. The quadriceps tendon, which merges into the patellar tendon, is a prime example of this functional synergy.
We must not overlook the importance of these structures in maintaining knee health. A well-coordinated interplay between ligaments and tendons is essential for the knee’s full range of motion and its ability to withstand the stresses of daily activities.
Tip: Regular exercise and proper stretching can help maintain the strength and flexibility of knee ligaments and tendons, potentially reducing the risk of injury.
Biomechanics of Knee Movement
Flexion and Extension
In knee biomechanics, flexion and extension are fundamental movements that allow for the bending and straightening of the knee joint. These movements are crucial for various activities, including walking, running, and jumping. The range of motion in flexion and extension is influenced by the interaction of the femur and tibia, as well as the surrounding ligaments and tendons. Understanding the biomechanics of flexion and extension is essential for assessing knee function and diagnosing related injuries or conditions.
Rotational Movements of the Knee
After exploring the dynamics of knee flexion, extension, and rotational movements, we turn our attention to the critical aspect of knee joint stability. Stability is paramount for both everyday activities and high-impact sports, and it is largely influenced by the menisci and surrounding muscles.
The menisci, two crescent-shaped cartilages, play a vital role in absorbing shock and distributing load across the knee joint. They also aid in the complex coordination required for rotational stability. Without the menisci, the femur and tibia would bear excessive stress, leading to rapid joint deterioration.
Muscles contribute significantly to knee stability. The quadriceps and hamstrings, in particular, provide the necessary tension and support to prevent unwanted movements. Strengthening these muscles through targeted exercises can enhance knee stability and reduce the risk of injury.
Tip: Consistent muscle-strengthening routines are essential for maintaining knee joint stability, especially for individuals engaged in sports that involve twisting or pivoting motions.
Knee Joint Stability
Role of Menisci in Knee Stability
The role of the menisci in knee stability is crucial for distributing weight and reducing friction within the joint. Menisci also contribute to shock absorption and provide stability during rotational movements. Additionally, the menisci help in lubricating the joint and nourishing the articular cartilage.
- It is important to note that the menisci have a significant impact on the overall function and longevity of the knee joint.
- Proper care and rehabilitation after meniscus injuries are essential for maintaining knee stability and preventing further damage.
It is advisable to consult a healthcare professional for personalized guidance on maintaining meniscal health and knee stability.
Importance of Muscles in Knee Stability
In our exploration of knee anatomy, we’ve seen how bones, ligaments, and menisci contribute to knee stability. However, the role of muscles is paramount. Muscles around the knee work in concert to provide the necessary strength and stability for daily activities and athletic endeavors. The quadriceps and hamstrings are the primary muscle groups that stabilize the knee joint. The quadriceps, located at the front of the thigh, are responsible for extending the knee, while the hamstrings, at the back, facilitate knee flexion.
The synergy between these muscle groups is crucial. When the quadriceps contract, the hamstrings must relax, and vice versa. This coordinated action ensures smooth movement and protects the joint from undue stress. Additionally, the calf muscles support the knee by controlling movements of the lower leg.
Tip: Regular strengthening exercises can significantly enhance knee stability and prevent injuries.
To illustrate the importance of muscle strength, consider the following table showing the relationship between muscle strength and knee stability:
| Muscle Group | Function in Knee Stability |
|---|---|
| Quadriceps | Extension and stabilization |
| Hamstrings | Flexion and stabilization |
| Calf Muscles | Support and movement control |
Maintaining muscle strength is not only crucial for knee stability but also for recovery from injuries such as an ACL tear. Post-surgery rehabilitation often focuses on rebuilding muscle strength to support the knee and facilitate a return to normal function.
Conclusion
In conclusion, a thorough understanding of the anatomy and functions of the knee bones is essential for comprehending the complexities of knee mechanics and addressing various knee-related issues. This knowledge serves as a foundation for medical professionals, researchers, and individuals seeking to enhance their understanding of the intricate structures that support the human body.
Frequently Asked Questions
What are the main bones in the knee joint?
The main bones in the knee joint are the femur, tibia, and patella.
What is the function of the patella?
The patella acts as a fulcrum for the quadriceps muscles and protects the knee joint.
How do ligaments and tendons contribute to knee stability?
Ligaments and tendons provide support and stability to the knee joint by connecting bones and muscles.
What is the range of motion of the knee joint?
The knee joint has a range of motion that includes flexion, extension, and rotational movements.
What is the role of menisci in knee stability?
The menisci act as shock absorbers and help distribute weight in the knee joint, contributing to stability.
How do muscles contribute to knee stability?
Muscles play a crucial role in knee stability by providing dynamic support and controlling movement.