Knee Pain Symptoms and Causes: A Comprehensive Guide
Knee pain can be a bothersome issue that affects people of all ages. It may result from a number of factors, such as injuries like torn cartilage or ruptured ligaments, or medical conditions like arthritis, gout, and infections. Understanding the causes and symptoms of knee pain is essential for seeking timely and appropriate treatment to alleviate discomfort and prevent complications.
In this article, we will explore the various factors that contribute to knee pain and gain insights into different treatment approaches. We will also discuss risk factors and preventive measures to help maintain healthy knees and maintain overall well-being.
patellofemoral pain syndrome:
Understanding Patellofemoral Pain Syndrome
| Category | Details |
|---|---|
| Definition | Pain between the kneecap (patella) and thighbone (femur) due to abnormal biomechanical forces |
| Common Causes | – Kneecap maltracking/dysfunction<br>- Overuse from sports<br>- Tight quadriceps, IT band, calves <br>- Weak hip and gluteal stabilizers |
| Contributing Factors | – High Q-angle anatomy<br>- Poor movement patterns<br>- Sudden load increases without adaptation |
| Affected Populations | – Athletes <br>- Young active adults<br>- Older adults with kneecap arthritis |
| Conservative Treatment | – Taping/bracing to improve tracking <br>- Targeted stretching & strengthening <br>- Movement pattern retraining |
| Surgical Options | – Lateral release to loosen tight tissues<br>- Patellar reshaping procedures<br>- Kneecap cartilage resurfacing |
Key components of PFPS involve abnormal kneecap gliding, overloading tissue capacities through sports, and anatomical vulnerabilities. Conservative rehabilitation aims to correct the imbalances, while surgery is occasionally utilized for refractory cases to realign structures or halt arthritis progression.
Key Takeaways
- Knee pain can be caused by injuries or medical conditions like arthritis and gout.
- Timely diagnosis and treatment can alleviate discomfort and prevent complications.
- Understanding risk factors and preventive measures helps maintain healthy knees.
Overview
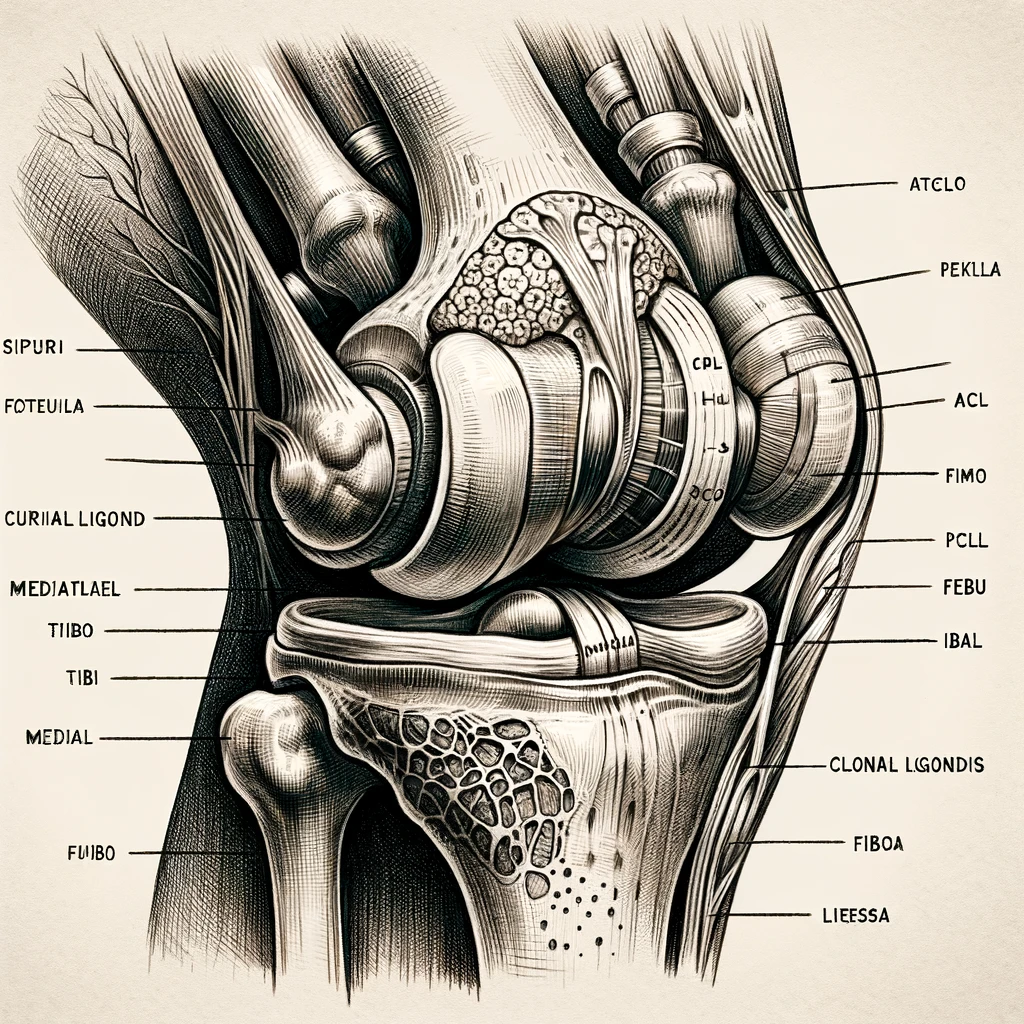
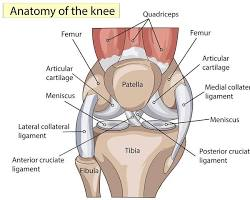
Knee pain is highly prevalent and affects individuals of all age groups. It can stem from injuries such as torn cartilage or ruptured ligaments or be a result of medical conditions like arthritis, gout, and infections. Fortunately, most minor knee pain cases can be managed through self-care measures, while more severe cases may benefit from physical therapy, knee braces, or even surgical intervention. Our discussion will dive deeper into the complexities of knee pain, exploring muscles, joints, ligaments, tendons, and bones (tibia, patella, and femur) involved in the knee joint.
Symptoms
Recognizing the Signs
Knee pain can manifest in various ways depending on the underlying issue. Some common symptoms accompanying knee pain are:
- Swelling and stiffness
- Redness and a warm sensation
- Weakness or instability
- Audible popping or crunching sounds
- Difficulty fully straightening the knee
Seeking Medical Attention
We encourage you to consult your doctor if you experience any of the following:
- Inability to bear weight on your knee or a feeling of instability
- Significant swelling of the knee
- Limited extension or flexing of the knee
- Visible deformities in your leg or knee
- Fever, accompanied by redness, pain, and swelling in the knee
- Severe knee pain associated with an injury
From Mayo Clinic to Your Inbox
We’re excited to provide you with the latest research advancements, health tips, current health topics, and advice on managing your health straight to your inbox. Sign up for free and stay informed with information tailored to your needs.
By signing up, we combine your email and website usage information with other details we have about you, ensuring the most relevant and helpful content is delivered to you. For Mayo Clinic patients, rest assured that your protected health information is treated with utmost care and used according to our privacy practices.
Remember, you have the option to opt-out of our email communications at any time by simply clicking the unsubscribe link provided in the email.
Causes of Knee Pain
Injuries Affecting the Knee
Knee injuries can involve various structures around the knee joint, such as ligaments, tendons, bursae, bones, and cartilage. Some common knee injuries are:
- ACL injury: A tear in the anterior cruciate ligament, which connects the shinbone to the thighbone, often occurs in sports that require sudden directional changes like basketball or soccer.
- Fractures: Knee bones, including the kneecap, may break due to falls or vehicle accidents. Osteoporosis can also lead to knee fractures from minor missteps.
- Torn meniscus: The meniscus, the cartilage cushioning between the shinbone and thighbone, may tear if the knee is suddenly twisted while bearing weight.
- Knee bursitis: Injuries may cause inflammation in the knee bursae, the fluid-filled sacs that enable smooth movement between tendons, ligaments, and the knee joint.
- Patellar tendinitis: This refers to the irritation and inflammation of tendons attaching muscles to bones, particularly the patellar tendon connecting the kneecap and shinbone. It often occurs in runners, skiers, cyclists, and people involved in jumping sports.
Mechanical Issues
Mechanical problems causing knee pain include:
- Loose body: Detached bone or cartilage fragments floating in the joint space can obstruct knee joint movement, akin to a pencil caught in a hinge.
- Iliotibial band syndrome: Tightening of the iliotibial band, which extends from the hip to the outer knee, can cause rubbing against the thighbone. Distance runners and cyclists are prone to this condition.
- Dislocated kneecap: The kneecap can slip out of place, typically to the knee’s outside. In some instances, the dislocation remains visible.
- Hip or foot pain: Compensating for pain in the hips or feet by changing one’s gait can place extra stress on the knee joint, leading to pain.
Forms of Arthritis
Various types of arthritis can cause knee pain:
- Osteoarthritis: This wear-and-tear condition results from the knee cartilage’s deterioration due to use and age.
- Rheumatoid arthritis: An autoimmune disease potentially affecting any joint, including the knees. This chronic condition’s severity may fluctuate.
- Gout: Occurs when uric acid crystals accumulate in the joint, typically affecting the big toe but also the knee.
- Pseudogout: Often mistaken for gout, this condition stems from calcium-containing crystals in the joint fluid. The knee is the most frequently affected joint.
- Septic arthritis: An infection in the knee joint may lead to swelling, pain, redness, and fever. It can quickly damage the knee cartilage, requiring urgent medical attention.
Additional Issues
Patellofemoral pain syndrome (PFPS) refers to discomfort between the kneecap (patella) and underlying thighbone (femur). It involves abnormal forces transmitted through the patellofemoral joint which is the articulation between these two structures. PFPS commonly affects certain populations, especially athletes who overloaded their knees through repetitive overuse from sports.
The main culprit causing PFPS is maltracking or dysfunction of the kneecap as it glides up and down in a groove on the femur during knee bending. This maltracking indicates a biomechanical imbalance, often from tight muscles or anatomical misalignment pulling the cap sideways. This leads to increased pressures on the back of the patella and the adjacent cartilage, triggering pain.
PFPS frequently develops in young active adults, particularly females, who have naturally higher “Q angles” – an anatomical measurement of kneecap positioning. It also occurs in some older adults for whom the cartilage under the kneecap has worn away significantly due to arthritis, causing bone-on-bone grinding. These groups appear predisposed towards developing knee pain from the aftermath of abnormal patellofemoral mechanics.
Besides overuse from sports and vulnerable anatomy, other PFPS triggers involve sudden increases in loading too quickly. The muscles stabilizing the patella require adaptations to control loads safely. When demands exceed abilities, the kneecap tracking suffers. Additionally, poor movement patterns such as unbalanced squatting or jumping/landing with knock knees induces patellofemoral compression. Often tight quadriceps, IT bands and calves paired with weak hips/glutes contributes to dysfunction.
Several targeted interventions aim at conservatively realigning the patella, strengthening deficient stabilizers, restoring ideal tracking and alleviating compression forces causing PFPS. Using braces, taping, customized exercise corrections and gait pattern retraining are common initial tactics under therapist guidance to calm pain and prevents recurrences. In some cases of refractory PFPS or significant arthritis, surgical options to release or reshape overtightened tissues or resurface damaged articulations provide longer term solutions.