Articles / Effective Remedies for Knee Pain Below Knee Cap Inside
Knee pain under the kneecap can be really uncomfortable and make it hard to move around. It’s important to know what causes this pain and how to treat it. This article will help you understand the reasons behind the pain, home remedies, exercises, diet tips, and medical treatments that can help. Plus, you’ll learn how to prevent knee pain in the future.
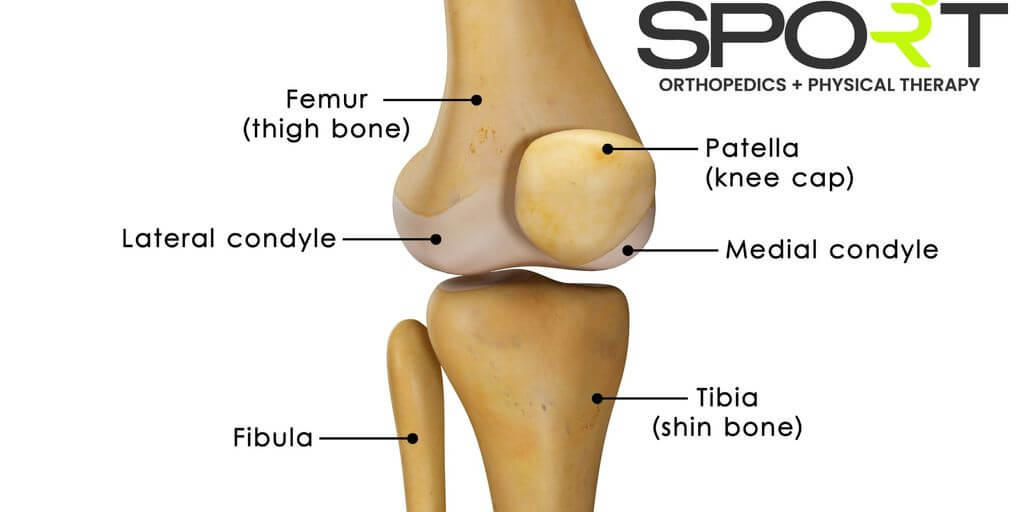
Understanding Knee Pain Below the Knee Cap
Common Causes
Knee pain below the knee cap can be caused by various factors. Overuse injuries are common, especially in athletes. Conditions like patellar tendinitis or bursitis can also lead to discomfort. Sometimes, structural issues such as misalignment of the knee cap can be the culprit.
Symptoms to Watch For
If you experience pain below the knee cap, you might notice swelling, stiffness, or a popping sensation. Tenderness when pressing on the area is also a common symptom. It’s important to monitor these signs to understand the severity of the issue.
When to Seek Medical Help
You should seek medical help if the pain persists despite home remedies or if it worsens over time. Additionally, if you experience severe swelling, inability to bear weight, or if the knee looks deformed, it’s crucial to consult a healthcare professional.
Early diagnosis and treatment can prevent further complications and help you get back to your daily activities sooner.
Home Remedies for Alleviating Knee Pain
Rest and Ice Therapy
Giving your knee enough rest is crucial. Avoid putting too much weight on it and use ice packs to reduce swelling. Apply ice for 15-20 minutes every few hours.
Compression and Elevation
Using a compression bandage can help manage swelling. Make sure it’s snug but not too tight. Elevate your leg on pillows to keep it above heart level, which helps reduce swelling.
Over-the-Counter Pain Relievers
Over-the-counter pain relievers like ibuprofen or acetaminophen can be effective. These medications help reduce pain and inflammation. Always follow the dosage instructions on the package.
Taking care of your knee at home can make a big difference in your recovery. Simple steps like rest, ice, compression, and elevation can help you feel better faster.
Exercises to Strengthen the Knee
Stretching Techniques
Stretching is a great way to keep your knees flexible and reduce pain. Simple stretches like hamstring stretches or calf stretches can make a big difference. Try to stretch every day to keep your muscles loose and your joints healthy.
Strengthening Workouts
Strengthening the muscles around your knee can help support the joint and reduce pain. Exercises like leg lifts, squats, and lunges are very effective. Start with light weights and gradually increase as you get stronger. Remember, consistency is key.
Low-Impact Activities
Low-impact activities are easier on your knees and can still help you stay active. Swimming, cycling, and walking are great options. These activities help you stay fit without putting too much stress on your knees.
Regular exercise can help you manage knee pain and improve your overall health. Make sure to choose activities that you enjoy and can stick with over time.
Diet and Supplements for Joint Health

Anti-Inflammatory Foods
Eating the right foods can help reduce knee pain. Foods rich in omega-3 fatty acids like salmon and walnuts can lower inflammation. Adding fruits and vegetables, especially those high in antioxidants, can also help. Try to avoid processed foods and sugary drinks as they can make inflammation worse.
Essential Vitamins and Minerals
Certain vitamins and minerals are important for joint health. Vitamin D and calcium are crucial for strong bones. Magnesium helps with muscle function and can reduce cramps. Make sure to get enough of these nutrients through your diet or supplements if needed.
Herbal Supplements
Some herbal supplements can help with knee pain. Turmeric, with its active ingredient curcumin, is known for its anti-inflammatory properties. Ginger is another good option. Always talk to your doctor before starting any new supplement to make sure it’s safe for you.
Eating a balanced diet and taking the right supplements can make a big difference in managing knee pain. It’s important to focus on foods and supplements that support joint health and reduce inflammation.
Medical Treatments for Persistent Knee Pain
Physical Therapy
Physical therapy is often the first step in treating ongoing knee pain. A therapist will guide you through exercises to improve strength and flexibility. This can help reduce pain and prevent further injury. Regular sessions can make a big difference in your recovery.
Prescription Medications
When over-the-counter pain relievers aren’t enough, doctors may prescribe stronger medications. These can include anti-inflammatory drugs or painkillers. It’s important to follow your doctor’s instructions to avoid side effects.
Surgical Options
In severe cases, surgery might be needed. Procedures can range from arthroscopy to knee replacement. Your doctor will discuss the best option for you based on your condition. Surgery is usually considered only after other treatments have failed.
Persistent knee pain can be challenging, but there are many medical treatments available to help you find relief.
Preventing Knee Pain in the Future
Proper Footwear
Wearing the right shoes can make a big difference in keeping your knees healthy. Supportive shoes help align your legs and reduce stress on your knees. Avoid high heels and choose shoes with good arch support.
Regular Exercise
Staying active is key to preventing knee pain. Focus on exercises that strengthen the muscles around your knee. This can include activities like walking, swimming, or cycling. Remember to warm up before exercising to avoid injury.
Weight Management
Keeping a healthy weight is important for your knees. Extra weight puts more pressure on your knees, which can lead to pain. Eating a balanced diet and staying active can help you maintain a healthy weight.
Taking care of your knees now can save you from pain later. Simple steps like wearing the right shoes, staying active, and keeping a healthy weight can make a big difference.
Conclusion
In summary, dealing with knee pain below the kneecap can be challenging, but there are many effective remedies to help manage it. From simple exercises and stretches to over-the-counter medications, there are various ways to find relief. It’s important to listen to your body and not push through the pain. If the pain persists, seeking advice from a healthcare professional is a good idea. Remember, taking care of your knees today can prevent bigger problems in the future. Stay active, stay healthy, and take steps to protect your knees.
Key Takeaways
- Understanding the causes of knee pain helps in finding the right treatment.
- Home remedies like rest, ice, and compression can ease knee pain.
- Regular exercises can strengthen the knee and prevent future pain.
- Eating the right foods and taking supplements can improve joint health.
- Seeking medical help is important for persistent or severe knee pain.
Frequently Asked Questions
What are common causes of knee pain below the knee cap?
Knee pain below the knee cap is often caused by overuse, injuries, or conditions like tendinitis and bursitis. Sometimes, it can also be due to arthritis or a dislocated knee cap.
What symptoms should I watch for with knee pain?
Watch for swelling, stiffness, redness, and pain when moving the knee. If you hear popping sounds or feel like your knee might give out, these are also signs to be aware of.
When should I see a doctor for knee pain?
You should see a doctor if the pain is severe, if you can’t put weight on your knee, if it looks deformed, or if you have a fever along with the pain. These could be signs of a more serious problem.
What home remedies can help with knee pain?
Resting your knee, using ice packs, wearing a compression bandage, and keeping your leg elevated can help. Over-the-counter pain relievers like ibuprofen can also reduce pain and swelling.
How can exercises help with knee pain?
Exercises can strengthen the muscles around your knee, improve flexibility, and reduce pain. Stretching, strengthening workouts, and low-impact activities like swimming are good options.
What foods are good for joint health?
Foods that fight inflammation, like fruits, vegetables, and fish, are good for joint health. Vitamins and minerals like Vitamin D and calcium, as well as herbal supplements, can also help keep your joints healthy.