Hot knees can be a discomforting and sometimes painful experience for many individuals. Understanding the causes and finding effective solutions is essential for managing this issue. In this article, we will explore the anatomy of the knee joint, identify the causes of hot knees, discuss diagnostic methods, and explore various treatment approaches.
Key Takeaways
- Understanding the anatomy of the knee joint is crucial for identifying and addressing issues related to hot knees.
- Inflammatory conditions, overuse, and environmental factors are common causes of hot knees and should be addressed through appropriate measures.
- Diagnostic methods such as physical examination, imaging techniques, and laboratory tests are essential for accurately diagnosing the underlying issues related to hot knees.
- Treatment approaches for hot knees may include medication and pain management, physical therapy, and lifestyle modifications for long-term relief.
- Seeking professional medical advice and guidance is crucial for effectively managing hot knees and preventing further complications.
Understanding the Anatomy of the Knee Joint
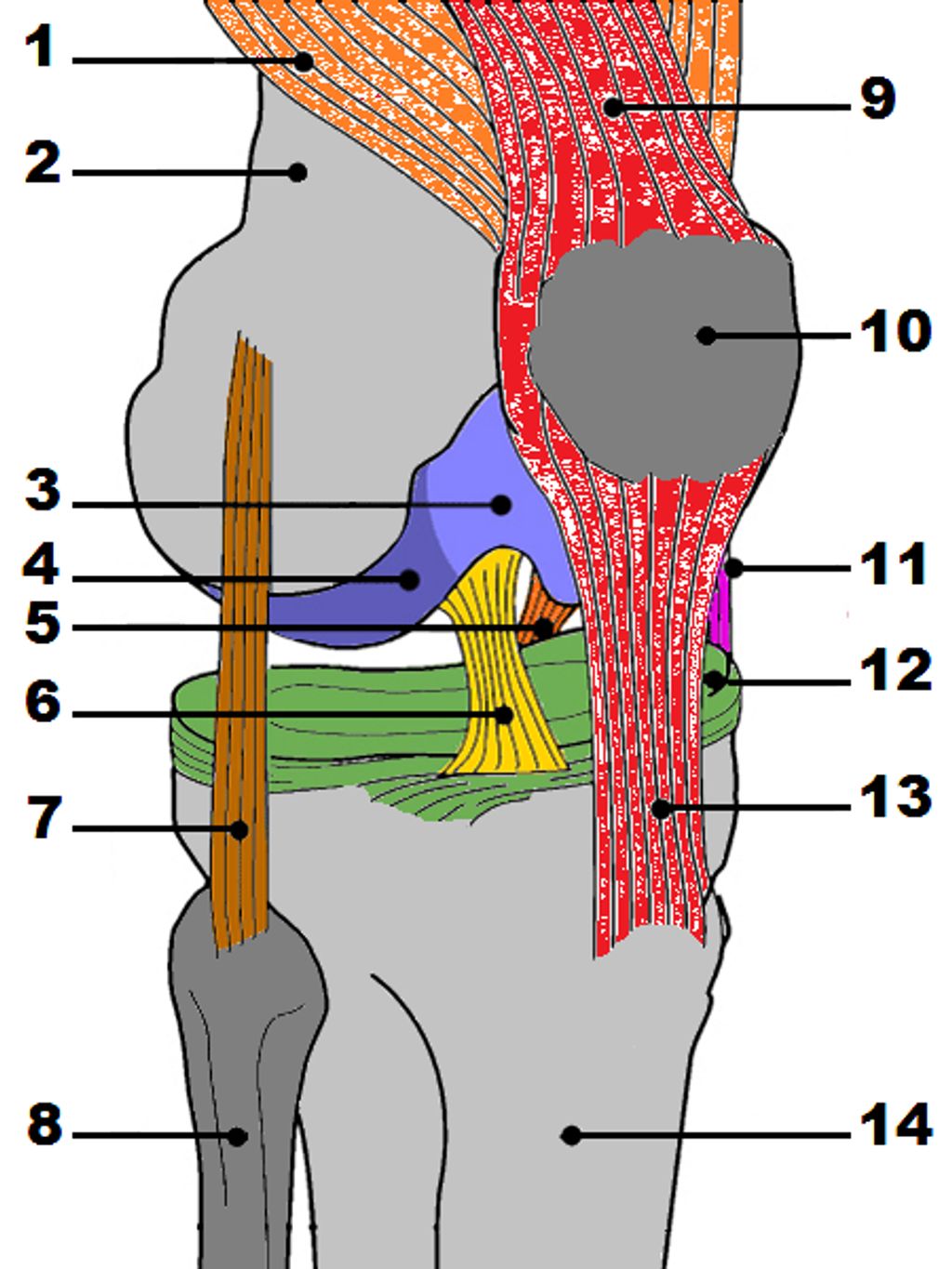
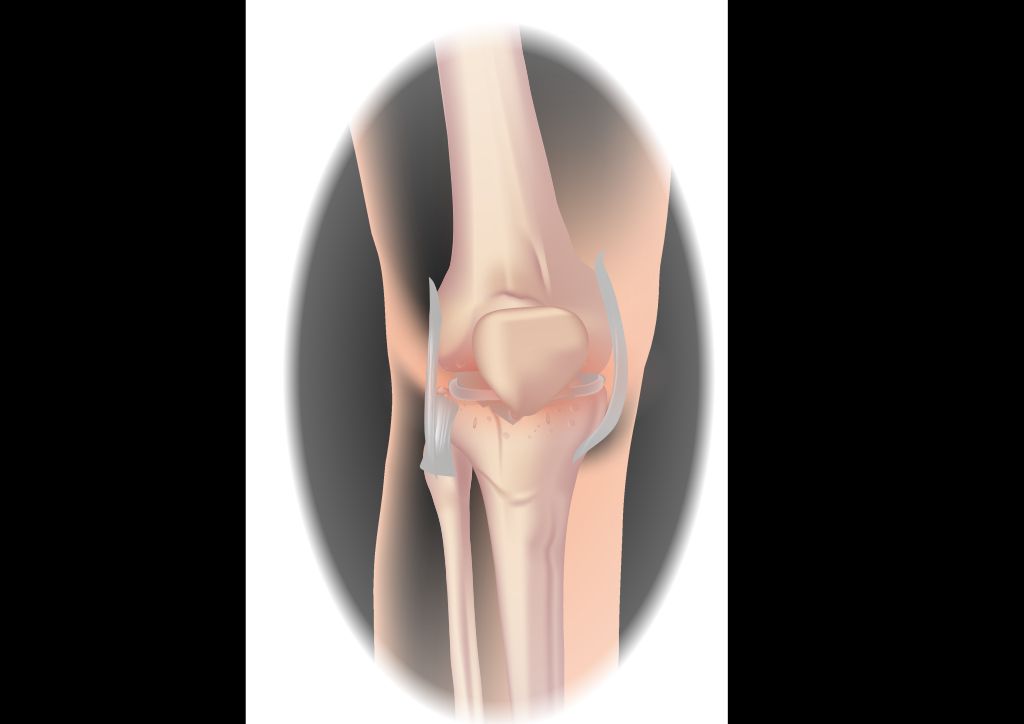
The Structure of the Knee Joint
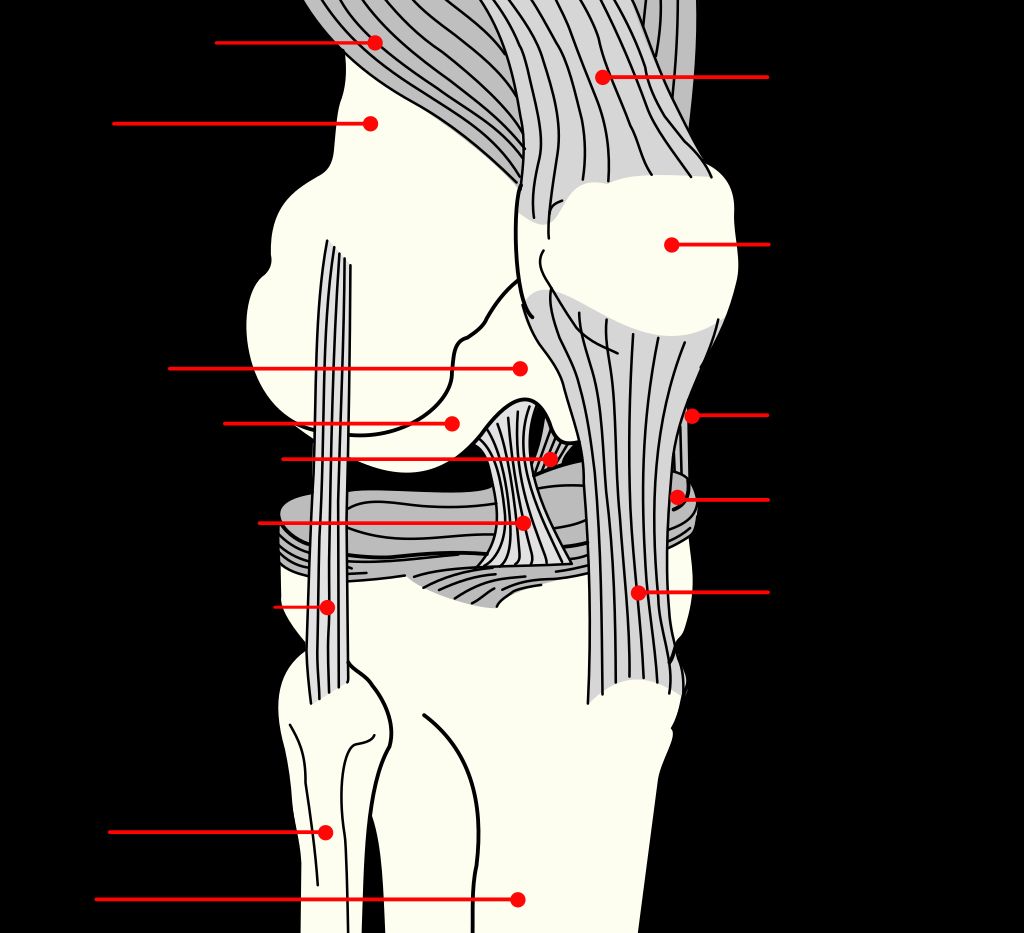
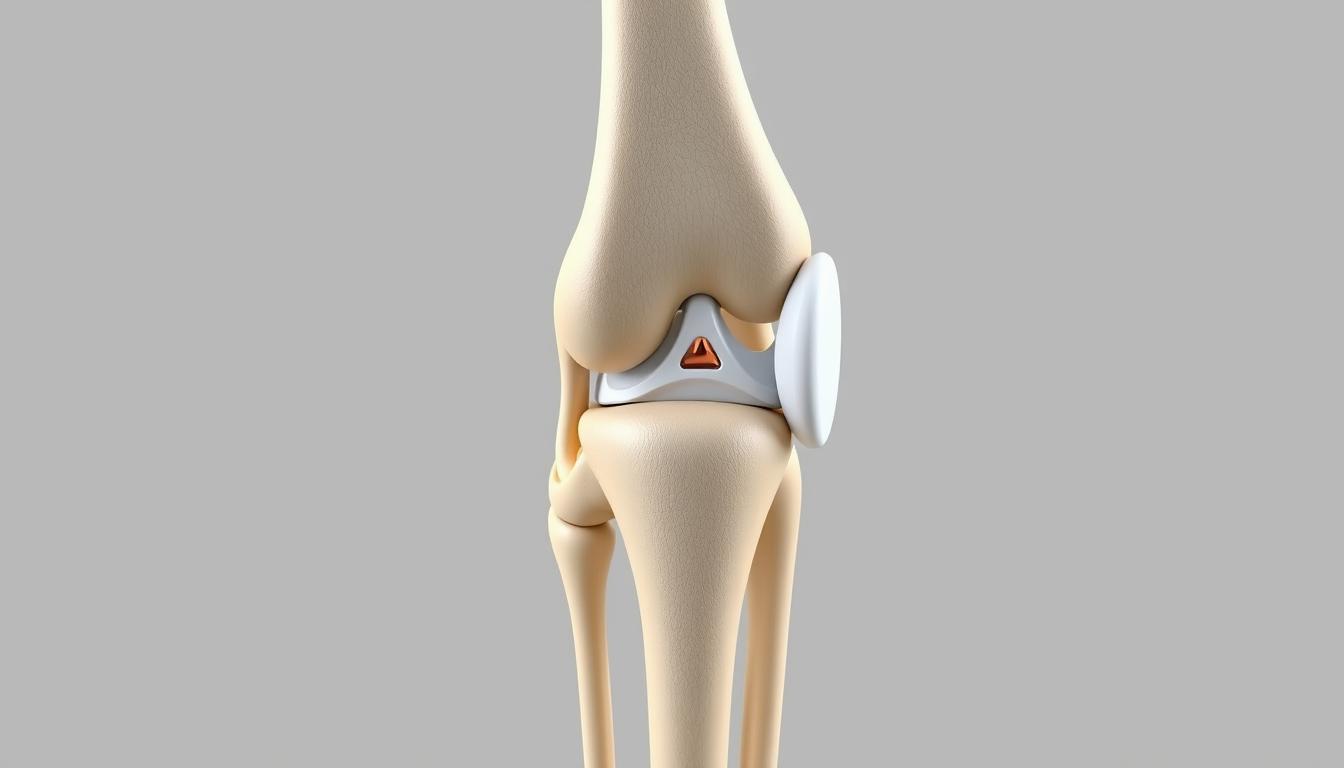
We often take for granted the intricate design of our knee joints, which are pivotal for movement and stability. The knee joint is a complex hinge that connects the thigh bone (femur) to the shin bone (tibia), with the kneecap (patella) sitting in front to provide protection and aid in movement.
Within the joint, there are several key components that ensure its functionality: cartilage provides a smooth surface for movement, ligaments connect bones and provide stability, and tendons attach muscles to bones, enabling motion. Menisci, two C-shaped pieces of cartilage, act as shock absorbers and help distribute weight evenly across the joint.
Tip: Regularly engaging in knee-strengthening exercises can help maintain the health and longevity of these critical structures.
Understanding the anatomy of the knee is essential for identifying the root causes of hot knees. Each component plays a significant role, and damage or inflammation to any part can lead to discomfort and heat sensation in the knee area.
Functions of the Knee Joint
The knee joint is a complex structure that plays a crucial role in supporting our body weight and facilitating movement. It consists of several components, including the femur, tibia, and patella, which work together to provide stability and flexibility. Additionally, the knee joint is surrounded by a network of ligaments and tendons that help maintain its integrity and function. Understanding the intricate anatomy of the knee joint is essential for comprehending its biomechanical properties and the potential sources of discomfort or pain.
Common Issues Affecting the Knee Joint
We often encounter a range of issues that can affect the knee joint, leading to discomfort and a sensation of heat. Among these, arthritis stands out as a prevalent condition, causing inflammation and pain. Other common problems include ligament injuries, such as ACL tears, and meniscal damage, which can result from both acute trauma and chronic wear.
Patellofemoral pain syndrome (PFPS), also known as runner’s knee, is another issue that frequently brings patients to our clinic. This condition is characterized by pain around the kneecap and is often linked to overuse or misalignment.
Here’s a brief overview of the common knee issues we see:
- Arthritis, particularly osteoarthritis and rheumatoid arthritis
- Ligament injuries, including ACL and MCL tears
- Meniscal tears
- Patellofemoral pain syndrome (PFPS)
- Bursitis, an inflammation of the fluid-filled sacs that cushion the knee
Tip: Maintaining a healthy weight and regular exercise can help prevent some of these common knee issues. However, it’s crucial to listen to your body and avoid overexerting the knee joint.
Identifying the Causes of Hot Knees

Inflammatory Conditions
We often encounter patients who report a sensation of heat in their knees, a condition that can be attributed to various inflammatory processes. Inflammation is the body’s natural response to injury or disease, and in the context of the knee, it can be a sign of underlying issues that require attention.
One common inflammatory condition that leads to hot knees is osteoarthritis, a degenerative joint disease that affects the cartilage and can cause significant discomfort. Other conditions such as rheumatoid arthritis, gout, and infections like septic arthritis also contribute to inflammation and a feeling of warmth in the knee joint.
- Recognizing the symptoms early is crucial for effective management and treatment. Here’s a brief list of symptoms associated with inflammatory knee conditions:
- Swelling and redness
- Tenderness to touch
- Stiffness, especially in the morning
- Pain during movement or at rest
Tip: Regular monitoring of knee health and seeking prompt medical advice when experiencing unusual warmth or pain can prevent the progression of inflammatory conditions.
Overuse and Strain
We often overlook the fact that our knees bear a significant burden in our daily activities. Overuse and strain are not uncommon, especially among athletes and individuals with physically demanding jobs. The repetitive motion and constant pressure can lead to a condition we refer to as hot knees, characterized by warmth and discomfort in the knee area.
To better understand the impact of these factors, consider the following:
- Repetitive movements that stress the knee joint, such as running, jumping, or squatting.
- Prolonged periods of activity without adequate rest, which can exacerbate knee strain.
- Insufficient warm-up or stretching before engaging in physical activity.
It’s crucial to listen to our bodies and provide the necessary rest and recovery time to prevent overuse injuries. Incorporating rest days and proper warm-up routines can significantly reduce the risk of developing hot knees.
When we experience symptoms of hot knees, it’s important to assess our recent activities to identify potential causes. By doing so, we can take proactive steps to modify our behavior and seek appropriate treatment if necessary.
Environmental Factors
In our exploration of hot knees, we must consider the role of environmental factors. These are external elements that can exacerbate knee discomfort or contribute to the sensation of heat in the knee area. For instance, high temperatures and humidity can lead to increased joint swelling, which in turn may cause a sensation of warmth or ‘hot knees’.
- Exposure to cold weather, conversely, can stiffen the joints and exacerbate pain, although it might not directly relate to the sensation of heat.
We should also be mindful of the surfaces on which we walk or run. Hard surfaces can increase the impact on our knees, potentially leading to inflammation and a feeling of heat. Here’s a simple list of environmental factors to consider:
- High ambient temperatures
- High humidity levels
- Cold weather conditions
- Hard walking or running surfaces
Tip: To mitigate the effects of environmental factors, we can adjust our activities according to the weather and choose appropriate footwear to cushion our knees from hard surfaces.
Diagnostic Methods for Hot Knees
Physical Examination
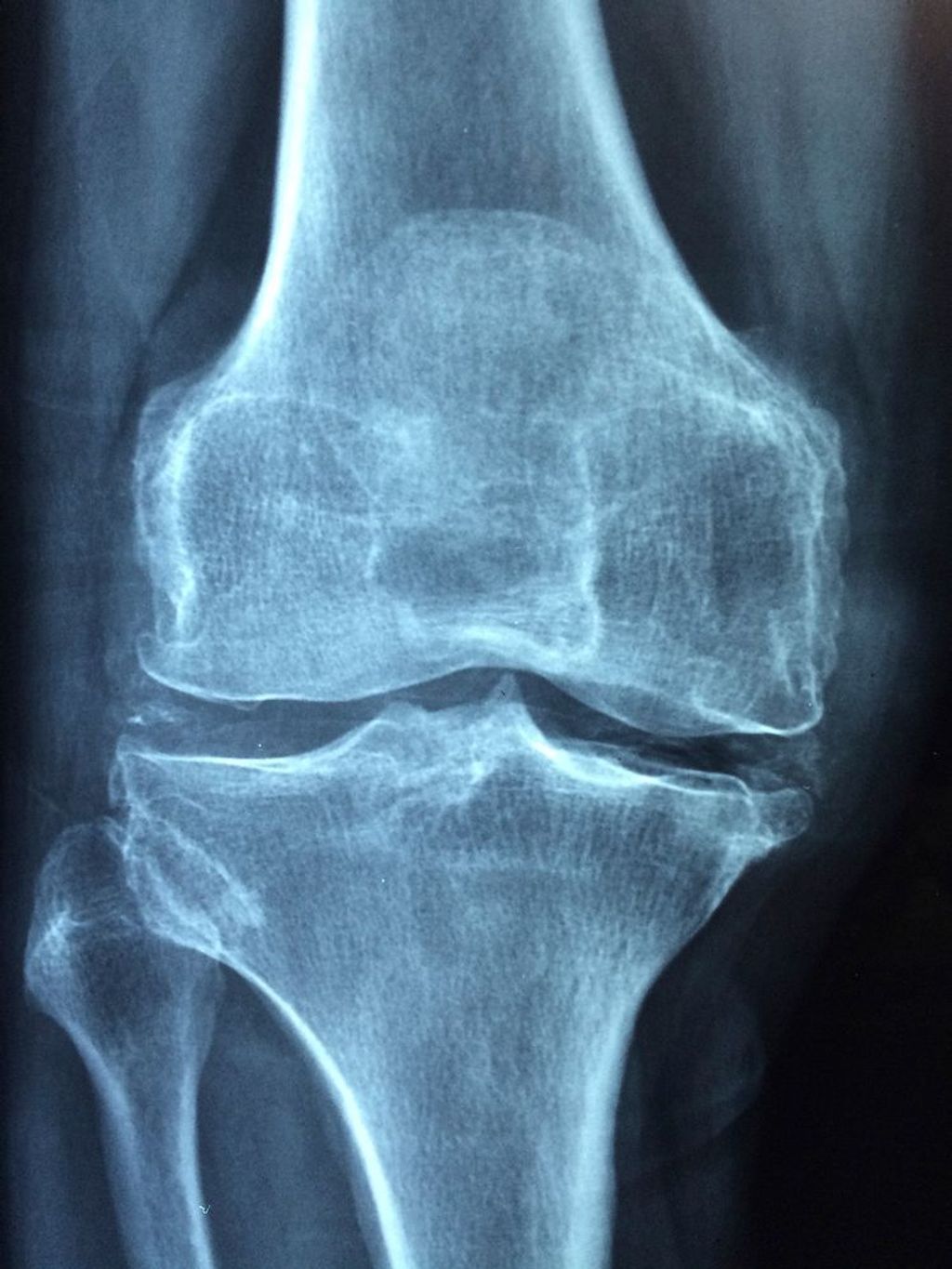
After conducting a thorough physical examination, medical professionals may proceed with imaging techniques such as X-rays and MRI scans to assess the internal structures of the knee joint. These imaging methods provide detailed visual information about bone density, cartilage health, and the presence of any abnormalities. Additionally, laboratory tests, including blood tests and joint fluid analysis, can help in identifying underlying inflammatory markers and ruling out other potential causes of hot knees. Here’s a brief overview of the diagnostic methods:
- Physical Examination
- Imaging Techniques
- X-rays
- MRI scans
- Laboratory Tests
- Blood tests
- Joint fluid analysis
It’s important to note that accurate diagnosis is crucial for effective treatment. Early detection of the underlying cause can lead to better outcomes and prevent further complications. As a tip, patients should communicate any relevant symptoms and concerns to their healthcare provider for a comprehensive evaluation and personalized care plan.
Imaging Techniques
After conducting a thorough physical examination, we often turn to imaging techniques to gain a deeper understanding of the underlying causes of hot knees. These techniques allow us to visualize the internal structures of the knee joint in great detail, aiding in the diagnosis of conditions that may not be apparent through a physical exam alone.
The most commonly used imaging modalities include:
- X-rays: To detect bone abnormalities and degenerative changes.
- MRI (Magnetic Resonance Imaging): For a detailed view of soft tissues, including ligaments, tendons, and cartilage.
- Ultrasound: To assess soft tissue structures and their movement.
- CT (Computed Tomography) Scans: To provide a more comprehensive view of the knee’s bone and soft tissue architecture.
Tip: Always discuss the results of imaging tests with your healthcare provider to understand the implications for your specific condition.
It’s essential to choose the most appropriate imaging technique based on the patient’s symptoms and the suspected diagnosis. For instance, while X-rays are excellent for visualizing bone fractures, an MRI might be necessary to evaluate a suspected meniscal tear or ligament injury.
Laboratory Tests
Following the physical examination and imaging, we often turn to laboratory tests to further investigate the causes of hot knees. These tests can reveal underlying conditions that may not be apparent through other diagnostic methods. For instance, a complete blood count (CBC) can indicate signs of infection or inflammation, while specific markers like erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) can help in assessing the severity of these conditions.
Blood tests are not the only tools at our disposal. Synovial fluid analysis, extracted from the knee joint, can provide valuable insights into the health of the joint and the presence of conditions such as gout or infections. Here’s a simplified breakdown of potential laboratory tests:
- CBC: Detects infection and inflammation.
- ESR and CRP: Measure inflammation levels.
- Synovial fluid analysis: Identifies joint-related issues.
Remember, the results of laboratory tests should always be interpreted in the context of the patient’s overall health and in conjunction with other diagnostic findings.
Treatment Approaches for Hot Knees
Medication and Pain Management
When it comes to medication and pain management, it is crucial to consult with a healthcare professional to determine the most suitable approach for our individual needs. Understanding the potential side effects and interactions of medications is essential for informed decision-making. Additionally, exploring non-pharmacological methods such as physical therapy and lifestyle modifications can complement the treatment plan and contribute to long-term relief. It’s important to consider a holistic approach to managing hot knees, addressing both the symptoms and the underlying causes.
- Medication and pain management should be tailored to individual needs.
- Non-pharmacological methods like physical therapy and lifestyle modifications can complement the treatment plan.
- Consultation with a healthcare professional is essential for informed decision-making.
It is advisable to keep a record of any changes in symptoms or response to treatment, as this can provide valuable insights into the effectiveness of the chosen approach.
Physical Therapy
After completing the course of medication, physical therapy plays a crucial role in the rehabilitation process. Our approach focuses on strengthening the muscles around the knee joint and improving flexibility and range of motion. This is achieved through a combination of targeted exercises and manual therapy techniques. Additionally, we emphasize the importance of maintaining a healthy lifestyle, including regular exercise and proper nutrition, to support the long-term well-being of the knee joint.
- Implement a table for presenting structured, quantitative data. Ensure it’s succinct and formatted correctly in Markdown.
- Use a bulleted or numbered list for less structured content, like steps, qualitative points, or a series of related items.
Lifestyle Modifications
In our journey to alleviate hot knees, we recognize the importance of lifestyle modifications. Simple changes in daily habits can significantly impact our knee health. For instance, maintaining a healthy weight reduces the stress on knee joints, potentially lessening inflammation and pain.
- Regular exercise, tailored to individual needs and limitations, ensures that the muscles supporting the knees are strong and flexible. It’s crucial to choose activities that do not exacerbate knee pain, such as swimming or cycling, rather than high-impact sports.
Diet also plays a vital role in managing knee health. Incorporating anti-inflammatory foods like omega-3 rich fish, green leafy vegetables, and berries can help reduce symptoms. Additionally, staying hydrated is essential for joint lubrication.
Remember: It’s always advisable to consult with a healthcare professional before making significant lifestyle changes, especially if you have an underlying health condition.
If over-the-counter solutions are insufficient, it’s important to seek medical help. Choosing the right knee sleeve or support can provide relief and prevent further injury. Here’s a simple list of tips for managing knee pain:
- Use knee supports as needed
- Engage in low-impact exercises
- Maintain a balanced diet
- Stay hydrated
- Monitor your weight
- Rest your knees when necessary
Conclusion
In conclusion, the management of hot knees is a complex issue that requires a multifaceted approach. Understanding the underlying causes, such as overuse and inflammation, is crucial in developing effective solutions. It is imperative to prioritize prevention through proper warm-up and cool-down techniques, as well as the use of supportive gear. Additionally, seeking professional medical advice and treatment is essential for individuals experiencing persistent knee discomfort. By addressing the root causes and implementing proactive measures, individuals can effectively manage and alleviate the symptoms associated with hot knees.
Frequently Asked Questions
What are the common causes of hot knees?
Common causes of hot knees include inflammatory conditions, overuse and strain, and environmental factors.
How can I identify if I have hot knees?
Hot knees can be identified through symptoms such as warmth, redness, swelling, and pain in the knee joint.
Are hot knees a sign of a serious medical condition?
Hot knees can be a sign of an underlying medical condition, especially if the symptoms persist or worsen. It is important to seek medical advice for proper evaluation.
What diagnostic tests are used to assess hot knees?
Diagnostic tests for hot knees may include physical examination, imaging techniques such as X-rays and MRI, and laboratory tests to check for inflammation and other markers.
What are the treatment options for hot knees?
Treatment options for hot knees may include medication and pain management, physical therapy, and lifestyle modifications such as rest, ice, and elevation.
Can hot knees be prevented?
Hot knees can be prevented by avoiding overuse and strain, maintaining a healthy weight, using proper footwear, and practicing exercises to strengthen the knee muscles.