Knowing when to see a doctor for knee pain is one of the most important health decisions you can make, yet only 12% of individuals with knee osteoarthritis are currently seeking medical care for their condition, despite many having severe disease. Knee pain is one of the most common complaints we hear from people of all ages, and understanding the difference between minor discomfort and a problem that needs professional attention can protect your mobility for life.
Key Takeaways
| Question | Answer |
|---|---|
| When should I see a doctor for knee pain immediately? | If your knee is severely swollen, deformed, or you cannot bear weight, seek emergency care right away. |
| How long should I wait before seeing a doctor for knee pain? | If knee pain lasts more than 3 days without improvement, or is severe from the start, book an appointment promptly. |
| Can knee pain go away on its own? | Minor knee pain from overuse can resolve with rest and ice, but persistent or severe pain rarely improves without treatment. |
| What type of doctor treats knee pain? | Your GP is the first point of contact. They may refer you to an orthopedic specialist or sports medicine physician. |
| Is knee pain always serious? | Not always, but certain symptoms like instability, locking, or swelling always warrant a professional evaluation. |
| What are common conditions behind knee hurt? | ACL tears, meniscus damage, chondromalacia patella, ligament injuries, and osteoarthritis are among the most frequent causes. |
| Can I make knee pain worse by ignoring it? | Yes. Delaying care can lead to joint damage, muscle atrophy, and in some cases, the need for surgery that could have been avoided. |
1. Understanding Knee Pain: What Is Normal and What Is Not
Most of us have felt a twinge or stiffness in our knee after a long walk or a tough workout. That kind of mild, temporary discomfort is part of daily life and usually settles down with rest.
However, knee pain that disrupts your sleep, limits your movement, or appears alongside swelling and instability is a different story entirely. Learning to read those signals is the first step toward protecting your joint health.

The knee is the largest and most complex joint in the human body. It bears the full weight of your frame with every step, so it is no surprise that it is vulnerable to both sudden injury and long-term wear.
For a comprehensive overview of the causes, management strategies, and recovery paths for knee pain, visit our ultimate guide to understanding, managing, and overcoming knee pain.
2. When to See a Doctor for Knee Pain After an Injury
A sudden injury is one of the clearest triggers for asking when to see a doctor for knee pain. If you heard a popping sound at the moment of impact, or if your knee immediately swelled, that is a medical emergency, not a “wait and see” situation.
Sports injuries, falls, and direct impacts to the knee can damage ligaments, tendons, cartilage, or bone. These structures do not heal correctly on their own without a proper diagnosis.
Common post-injury situations that require prompt evaluation include:
-
A loud pop at the time of the injury
-
Immediate and significant swelling
-
Inability to straighten or fully bend the knee
-
A feeling that the knee “gave way” or is unstable
-
Visible deformity of the joint
-
Numbness or tingling below the knee
If you are dealing with a traumatic incident, our detailed guide on traumatic knee injuries covers what to expect from diagnosis to recovery.
3. Warning Signs That Mean You Need Medical Attention for Knee Pain Right Now
Some symptoms demand an urgent doctor visit rather than home care. These are the red flags that tell you when to see a doctor for knee pain without any delay.
Seek same-day or emergency care if you experience any of the following:
-
Your knee is hot, red, and extremely tender (possible infection or gout)
-
You cannot put any weight on the leg at all
-
You have a fever alongside knee swelling
-
The knee looks visibly out of place or deformed
-
You sustained a high-impact injury in a car accident or a fall from height
Ignoring these signs does not make them disappear. In many cases, waiting makes the structural damage worse and extends your recovery time significantly.
Did You Know?
Patients who receive rehabilitation within the first 15 days of a knee pain diagnosis are 42% less likely to require surgery later on.
Source: advisory.com
4. Common Knee Conditions That Require a Doctor’s Diagnosis
Not every case of knee hurt comes from a single dramatic event. Many serious conditions develop gradually, and patients often dismiss the early signs as “just aging” or “a bit of soreness.”
Here are the conditions we see most often that require professional diagnosis and treatment:
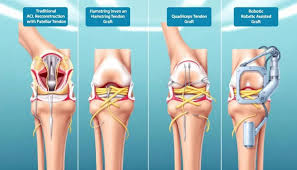
ACL and PCL Ligament Injuries
The anterior and posterior cruciate ligaments provide critical stability to the knee joint. Tears to these structures cause intense pain, rapid swelling, and a feeling that the knee is “loose.”
You can read more about ACL injuries and appropriate knee brace support or explore our guide on PCL knee injuries to understand the differences and treatment paths.

Torn Meniscus
The meniscus is the cartilage that cushions your knee joint. A tear causes pain, swelling, stiffness, and a locking or catching sensation in the joint.
If you suspect a meniscus problem, our comprehensive resource on torn meniscus injuries explains what to expect from your evaluation and treatment options.
Chondromalacia Patella
This condition involves the softening and breakdown of cartilage on the underside of the kneecap. It causes a dull, aching pain that is particularly noticeable when climbing stairs or sitting for long periods.
Our page on chondromalacia patella walks through the causes, risk factors, and treatment approaches in plain language.
Ligament Sprains and Tears
Beyond the ACL and PCL, the knee has several other ligaments that can be strained or torn. A full picture of the range of ligament knee injuries helps you understand which structure may be affected based on your symptoms.
5. When to See a Doctor for Knee Pain That Won’t Go Away
Chronic knee pain that lingers for weeks or months is one of the most underreported health concerns in 2026. Many people normalize the ache, adjusting their lives around it rather than addressing the source.
We recommend seeing a doctor for knee pain if:
-
Pain has persisted for more than 3 days without improvement
-
You are regularly taking over-the-counter pain relief just to function
-
The pain wakes you up at night
-
You have begun avoiding activities you used to enjoy
-
You notice a gradual increase in pain intensity over weeks or months
-
Stiffness is present every morning and takes more than 30 minutes to ease
Chronic knee hurt rarely resolves on its own. In most cases, the underlying cause, whether it is arthritis, a cartilage issue, or a tendon problem, requires guided intervention to improve.

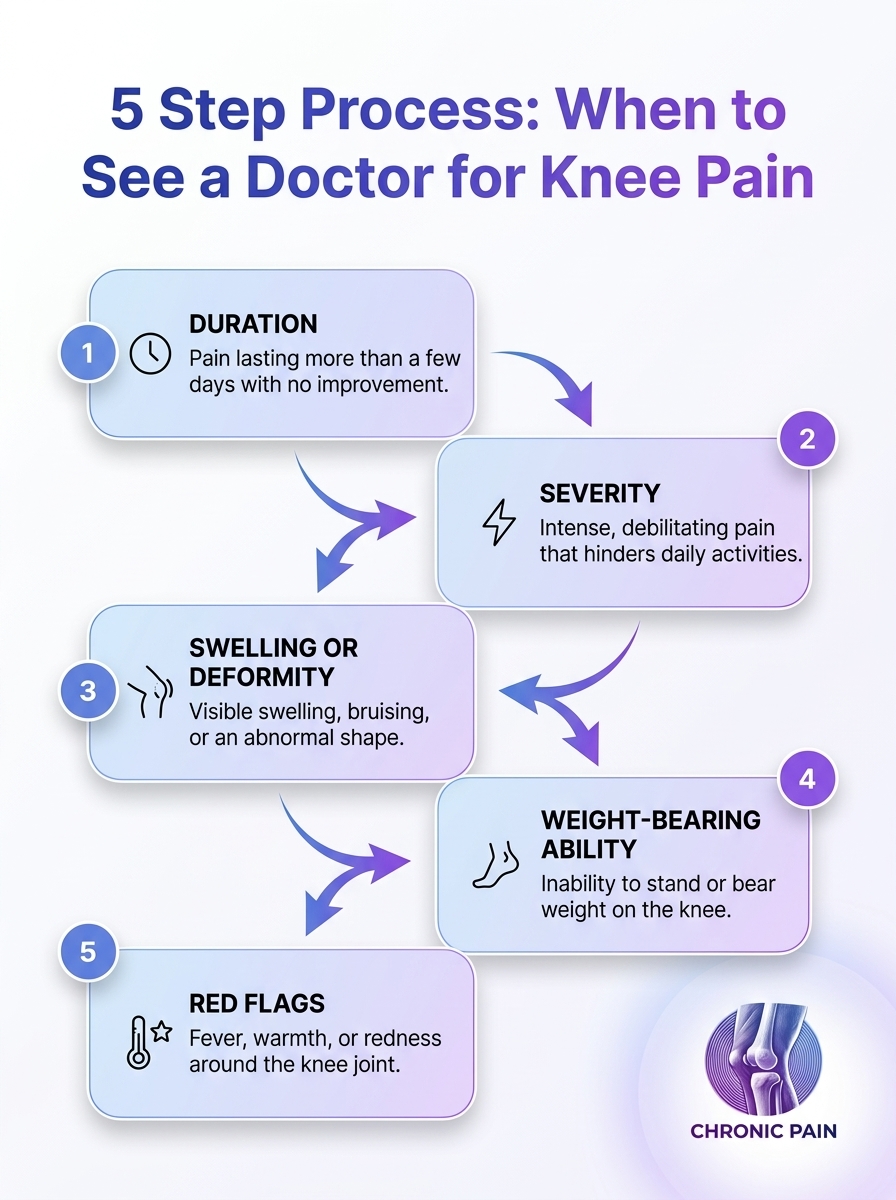
A concise 5-step guide to help readers decide when to seek medical care for knee pain. Learn which symptoms warrant a professional evaluation.
6. When to See a Doctor for Knee Pain With Swelling or Instability
Two specific symptoms deserve their own section because they are frequently misunderstood: swelling and instability.
Swelling inside the joint (a condition known as an effusion) is a sign that something is actively wrong. The body is producing excess fluid in response to injury or inflammation, and that process does not stop without treatment.
Instability, or the feeling that your knee might buckle or give way, indicates a structural problem with the ligaments or cartilage that support the joint. Walking on an unstable knee risks further damage with every step.
“If your knee swells up overnight without an obvious reason, that is your body telling you something is wrong. Do not wait for it to ‘go down on its own’ for weeks. See a professional.”
Both of these symptoms, swelling and instability, are clear indicators of when to see a doctor for knee pain as soon as possible rather than self-treating at home.
7. The Real Risks of Delaying Care for Knee Pain
One of the most important messages we want to share is that delay has consequences. The body has a limited window in which certain knee structures can heal or be rehabilitated before permanent changes occur.
When you push through knee hurt without getting a diagnosis, several things can happen:
-
Muscle atrophy: The muscles around the knee weaken rapidly when you reduce activity to avoid pain, making the joint less stable over time.
-
Compensatory injury: You begin to offload the painful knee by adjusting your gait, which places abnormal stress on your hip, ankle, and lower back.
-
Cartilage deterioration: Untreated inflammation breaks down cartilage progressively, moving a manageable condition toward a need for surgical intervention.
-
Psychological impact: Chronic knee pain is not just a physical battle. It affects sleep, mood, and mental health in ways that compound over time.

Did You Know?
Delaying physical therapy by 9 to 12 months from initial diagnosis increases the risk of chronic opioid use by 1.65 to 2.5 times.
Source: National Institutes of Health (NIH)
8. Specific Groups Who Should Be Especially Proactive About Knee Pain
While when to see a doctor for knee pain is relevant to everyone, certain groups face higher risks and should act at the first sign of a problem rather than waiting.
| Group | Why They Are at Higher Risk | Recommended Action |
|---|---|---|
| Athletes and active individuals | High repetitive stress on the joint; risk of ACL, meniscus, and ligament injuries | See a doctor within 24 hours of any significant injury |
| Adults over 50 | Higher risk of osteoarthritis, cartilage thinning, and slower healing rates | Schedule regular check-ups; don’t normalize morning stiffness |
| Women | Roughly twice as likely to report frequent knee pain compared to men | Be especially alert to early symptoms; seek evaluation sooner |
| Those with excess body weight | Every extra pound adds 4 pounds of pressure to the knee joint per step | Consult a doctor for both weight management and joint assessment |
| People with a family history of arthritis | Genetic predisposition increases lifetime risk of knee joint disease | Establish a care plan early, even before symptoms become severe |
9. What to Expect at Your Doctor’s Appointment for Knee Pain
Many people avoid booking an appointment because they are unsure what the process involves. We want to remove that barrier by walking you through what typically happens when you seek care for knee pain.
Step 1 – Medical history: Your doctor will ask about when the pain started, what makes it better or worse, whether there was a triggering event, and what your activity level is.
Step 2 – Physical examination: The doctor will examine the knee visually and manually, testing its range of motion, stability, and areas of tenderness.
Step 3 – Imaging: Depending on the findings, you may be referred for an X-ray to check for bone damage or an MRI to assess soft tissue structures including cartilage, tendons, and ligaments.
Step 4 – Diagnosis: With that information, your doctor can identify the specific cause of your knee hurt and recommend an appropriate care plan.
Step 5 – Treatment plan: This may include physical therapy, medication, a supportive brace, lifestyle changes, injections, or in some cases a surgical referral.

10. How to Prepare Before Seeing a Doctor for Knee Pain
Going to your appointment prepared helps you get more out of the consultation and ensures your doctor has all the information they need to make an accurate diagnosis.
Here is a simple checklist to complete before your visit:
-
Write down when the pain started and whether it came on suddenly or gradually
-
Note the exact location of the pain (front, back, inside, or outside of the knee)
-
Describe the character of the pain: sharp, dull, burning, throbbing, or stabbing
-
Track what triggers it: climbing stairs, sitting, walking, resting, or exercise
-
List all medications and supplements you currently take
-
Note any previous knee injuries or surgeries, even from years ago
-
Bring any imaging you already have, such as old X-rays or MRI reports
The more detail you can provide, the faster your doctor can move toward an accurate diagnosis and an effective treatment plan for your knee problem.
Conclusion
Understanding when to see a doctor for knee pain is not about being overly cautious. It is about protecting one of the most important joints in your body before minor problems become major ones.
In 2026, access to orthopedic and sports medicine care is better than ever, and early intervention consistently leads to better outcomes, faster recovery, and a lower risk of surgery. Whether you are dealing with a sudden injury, persistent knee hurt that will not clear up, or warning signs like swelling, instability, or locking, the right move is to get a professional evaluation promptly.
Do not normalize knee pain. Do not assume it will resolve itself. And do not wait until it stops you in your tracks completely before seeking the care you deserve. Your knee supports everything you do, and investing in its health today pays dividends for decades to come.
If you are ready to take the next step, start with our complete knee pain resource to explore your symptoms further, or dive deeper into any of the specific conditions we have covered throughout this article.