The ‘Quad-Plus’ ACL Reconstruction Standard 2026 represents the most significant shift in knee surgery protocols in over a decade, and the numbers behind it are hard to ignore: adding Lateral Extra-articular Tenodesis (LET) to a quadriceps tendon ACL reconstruction reduces the re-tear rate from roughly 12-15% all the way down to just 3%. If you have been living with knee pain after an ACL injury, or you are facing a reconstruction decision right now, understanding this standard could change the outcome of your surgery and your life beyond it.
Key Takeaways
| Question |
Answer |
| What is the Quad-Plus ACL Reconstruction Standard 2026? |
It is a surgical protocol that combines a quadriceps tendon autograft with a Lateral Extra-articular Tenodesis (LET) procedure to maximize rotational stability and reduce re-tear risk. |
| Why is the quadriceps tendon preferred in 2026? |
It is nearly twice as thick as the patellar tendon, has 88% lower donor-site morbidity, and allows full strength recovery through targeted rehabilitation. |
| Who benefits most from this standard? |
Young, high-demand athletes (ages 13-25) and anyone who pivots, cuts, or rotates heavily in their sport or daily life. |
| What does ‘Plus’ refer to? |
The ‘Plus’ refers to the LET add-on procedure that controls rotational instability and dramatically lowers the chance of the new ACL failing. |
| Does it help with long-term knee pain? |
Yes. With 96% patient satisfaction rates and lower donor-site discomfort, patients report significantly less ongoing knee pain compared to older techniques. |
| How long is recovery under this standard? |
Most athletes return to full competition between 9 and 12 months, with biological healing time being the most important recovery factor. |
| Are there related knee injuries I should know about? |
Yes. ACL tears frequently occur alongside a torn meniscus or other ligament knee injuries, which can affect your reconstruction plan. |
What Is the Quad-Plus ACL Reconstruction Standard 2026?
Let’s be direct about what this term actually means, because the name can sound intimidating when it doesn’t have to be.
The ‘Quad-Plus’ ACL Reconstruction Standard 2026 is a two-part surgical approach. The “Quad” part refers to using the quadriceps tendon (the large tendon above your kneecap) as the graft material to rebuild your torn ACL. The “Plus” part refers to adding a Lateral Extra-articular Tenodesis, or LET, at the same time.
Think of it this way: the Quad graft replaces the torn ligament itself, while the LET acts like a secondary anchor on the outside of the knee, preventing the kind of rotational looseness that causes that terrifying “giving way” feeling.
This is not a fringe idea born overnight. It is the result of years of clinical trials, meta-analyses, and real-world outcomes data that surgeons and researchers have assembled specifically to address the biggest failure point in ACL surgery: the re-tear.

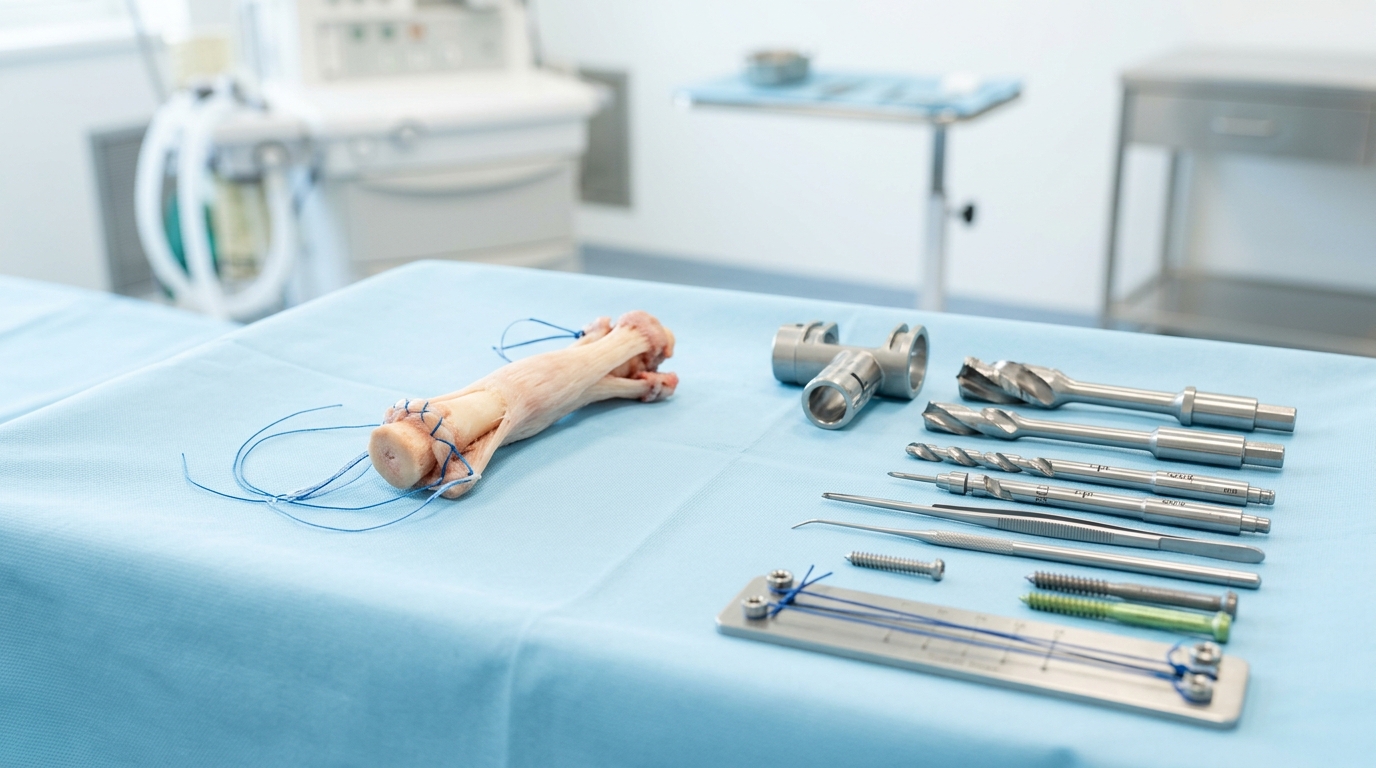
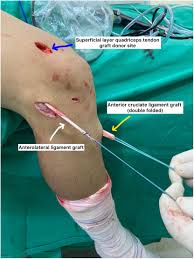
Why the Quad Tendon Became the Graft of Choice for ACL Reconstruction in 2026
For years, surgeons debated between three main graft options: the patellar tendon (BTB), the hamstring tendons, and the quadriceps tendon. In 2026, the quadriceps tendon has pulled clearly ahead, and the reasons are grounded in solid anatomy and patient outcomes.
The quadriceps tendon is nearly twice as thick in cross-sectional area as the patellar tendon and contains 20% more collagen fibrils per cross-section. That density matters enormously when you are asking a new piece of tissue to replace one of the most loaded ligaments in the human body.
More importantly for everyday patients, the Quad tendon causes significantly less donor-site trouble. You are not left with the kneeling pain that so commonly follows a BTB harvest, and you are not facing the permanent strength deficits sometimes seen with hamstring grafts.
If knee hurt after surgery has ever scared you away from pursuing reconstruction, the Quad graft data is genuinely reassuring. Patients report far less post-operative discomfort at the harvest site compared to the older patellar tendon approach.

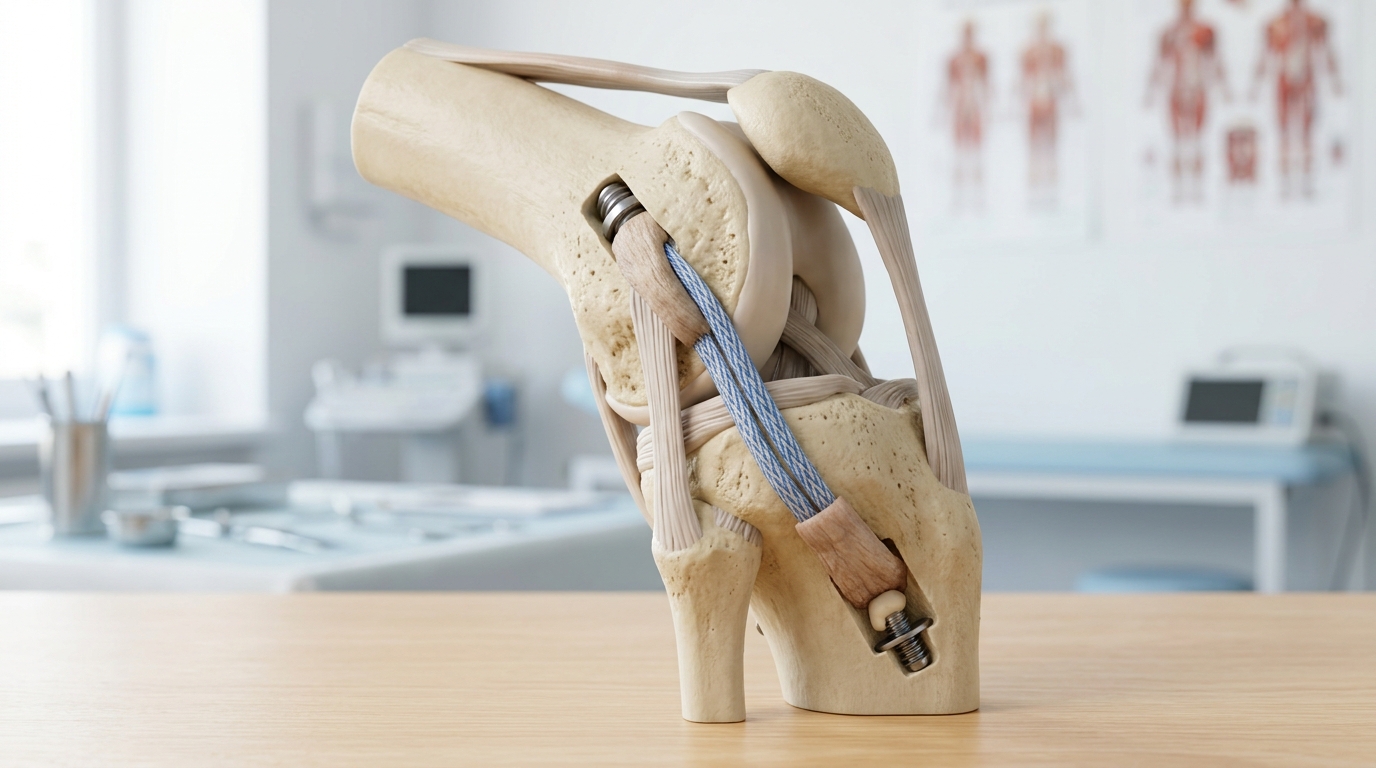
Understanding the ‘Plus’: What Lateral Extra-Articular Tenodesis Adds to the Quad-Plus ACL Reconstruction Standard 2026
Here is where the Quad-Plus ACL Reconstruction Standard 2026 really separates itself from everything that came before it.
Isolated ACL reconstruction, even with a perfect graft, leaves roughly 28% of patients with residual rotational instability. That means more than 1 in 4 patients still feels their knee slipping when they pivot, cut, or change direction quickly. The LET procedure brings that number down to just 9.3%.
What is LET exactly? It is a secondary procedure performed on the outside (lateral side) of the knee during the same operation. The surgeon uses a small strip of the iliotibial band to create an extra stabilizing anchor, reinforcing the knee’s rotational control without significantly adding to your recovery time.
This is not adding complexity for the sake of it. For anyone who plays basketball, soccer, skiing, martial arts, or any sport that involves rapid direction changes, this ‘Plus’ element is the difference between a knee that performs and one that eventually fails again.
Did You Know?
Quadriceps tendon (QT) autografts are associated with 88% lower odds of donor-site morbidity (such as kneeling pain) compared to traditional Bone-Patellar Tendon-Bone (BTB) grafts.
Source: isakos.com

Who Is the Quad-Plus ACL Reconstruction Standard 2026 Designed For?
The honest answer is: most people who tear their ACL. But certain groups benefit from it the most.
-
Young athletes (ages 13-25): Quad tendon grafts have a yearly failure rate of only 0.72% in patients under 25, compared to 1.70% for hamstring grafts. In competitive cohorts, 100% of athletes treated with quadriceps tendon autografts successfully returned to competition.
-
Pivoting sport athletes: Soccer, basketball, football, volleyball, skiing, tennis. Any sport involving rapid direction changes makes LET not just helpful but arguably essential.
-
People with high pre-injury activity levels: The more you demand from your knee, the more you need a robust reconstruction standard.
-
Anyone who has already re-torn an ACL: Revision surgery outcomes under the Quad-Plus approach are significantly better than older revision protocols.
-
Patients worried about long-term knee pain: If kneeling pain or anterior knee pain after surgery is a concern, the Quad graft is the most forgiving donor site of the three main options.
If you have experienced a traumatic knee injury, this is particularly relevant to you, because high-energy ACL tears are often the ones that also carry the highest rotational instability risk going forward.


The Quad-Plus ACL Reconstruction Standard 2026 vs. Older Techniques: A Direct Comparison
Let’s stop using vague language and look at what the numbers actually say side by side.
| Metric |
Hamstring Graft (Isolated) |
BTB Graft (Isolated) |
Quad-Plus Standard 2026 |
| Re-tear Rate (under 25) |
~1.70% per year |
~12-15% overall |
0.72% / ~3% overall |
| Rotational Instability |
~28% |
~28% |
9.3% |
| Donor-Site Knee Pain |
Moderate (permanent in some) |
High (kneeling pain common) |
88% lower than BTB |
| Patient Satisfaction |
~78-82% |
~80-84% |
96% |
| Return to Sport (Ages 13-24) |
Variable |
Variable |
100% in competitive cohorts |
The data is not subtle. Across every meaningful outcome metric, the Quad-Plus ACL Reconstruction Standard 2026 outperforms the techniques it is replacing.
Knee Pain and Recovery: What to Expect After Quad-Plus ACL Surgery
Let’s get real about the recovery because it is not a walk in the park, even with the best surgical standard available.
The most important thing to understand is that the graft heals on its own biological timeline, and no amount of motivation or effort can speed that up fundamentally. For every month an athlete delays their return to sport up to 9 months, the risk of re-injury drops by 51%. That is not a small number, and it is why the Quad-Plus standard builds in protected timelines rather than aggressive early return.
Here is a general recovery roadmap under this standard:
-
Weeks 1-6: Swelling management, range of motion restoration, and protecting the graft. Knee pain at this stage is normal and manageable.
-
Months 2-4: Progressive strengthening, neuromuscular control work, and early proprioception training.
-
Months 5-8: Quad graft users experience a transient strength deficit in this window (this is expected and temporary). Athletes using Quad grafts typically catch up completely to their baseline strength by the time of return to play, unlike hamstring graft patients who can face permanent deficits.
-
Months 9-12: Sport-specific training, return-to-play testing, and clearance decision. The 9-month minimum is not arbitrary; it is where the biology of graft maturation aligns with statistical safety.
Understanding the full picture of your knee pain and what drives it is critical during this recovery phase. Pain is information, not punishment, and knowing what it means at each stage protects your new ACL.


Associated Knee Injuries That Can Affect Your Quad-Plus Reconstruction Plan
Here is something that often gets glossed over in the surgical conversation: ACL tears rarely happen in isolation.
Studies consistently show that a significant percentage of ACL injuries occur alongside other structural damage. A concurrent torn meniscus is present in up to 50% of acute ACL injuries. Cartilage damage, PCL stress, and other ligament injuries also frequently accompany ACL tears, especially in high-energy mechanisms.
This matters for the Quad-Plus standard because your surgeon needs to address all of the damaged structures during your reconstruction, not just the ACL itself. Leaving a torn meniscus untreated while performing a perfect Quad-Plus reconstruction will still leave you with significant knee pain and joint problems down the road.
Common associated injuries to discuss with your surgeon include:
You deserve a surgeon who looks at your knee as a system, not just a single torn structure. The Quad-Plus standard is designed with that systems-thinking approach built in.


How Surgeon Adoption of the Quad-Plus ACL Reconstruction Standard 2026 Is Changing Clinical Practice
The medical world doesn’t change overnight, but the adoption curve for this standard is notably steep.
The national utilization of LET in ACL reconstructions grew five-fold from just 0.6% in 2015 to 3.7% in recent cohorts, with a 20% annual increase in usage since 2017. In 2026, that number is accelerating further as the clinical evidence base reaches critical mass.
What is driving this shift? Three things:
-
Outcome data: The re-tear and instability numbers are simply too compelling to ignore
-
Patient demand: Athletes who research their options are increasingly asking specifically for this approach
-
Surgical education: Fellowship programs and sports medicine conferences in 2026 are actively teaching the combined technique as the preferred standard for high-risk patients
If your surgeon has not heard of or does not offer the Quad-Plus approach, that is valuable information about whether you are seeing the right specialist for your injury.
Did You Know?
96% of patients receiving a Quadriceps tendon graft report being ‘satisfied’ or ‘very satisfied’ with their surgical results, a patient satisfaction rate that outperforms both hamstring and patellar tendon grafts.
Source: National Institutes of Health (NIH)
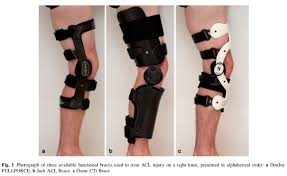
The Role of Knee Bracing and Conservative Support in the Quad-Plus ACL Reconstruction Standard 2026
Surgery is the centerpiece of this standard, but it does not work in isolation. The pre-operative and post-operative support strategy matters enormously.
Before surgery, many patients benefit from bracing to control instability and reduce the risk of secondary cartilage damage while waiting for their procedure. Understanding your ACL injury and appropriate knee brace options during this period is genuinely important for protecting the joint you are about to invest significant time and resources into repairing.
Post-operatively, functional bracing during the return-to-sport phase provides an additional layer of confidence, particularly during the 6-9 month window when the graft is maturing but sport-specific loading is beginning. The brace is a tool, not a cure, but it is a useful tool in the right context.
It is also worth noting that conservative management is a real option for some patients, particularly those with lower activity demands. Not everyone with a torn ACL needs surgery. But for anyone with the instability profile that the Quad-Plus standard is designed to address, non-surgical management rarely provides the same level of rotational stability that the ‘Plus’ procedure delivers.

Key Questions to Ask Your Surgeon About the Quad-Plus ACL Reconstruction Standard 2026
Knowing what to ask is half the battle. Here is a direct list of questions that will tell you quickly whether your surgeon is aligned with where ACL reconstruction science is in 2026.
-
“Do you use quadriceps tendon autograft as your primary graft choice for high-demand patients?”
-
“Do you add LET (Lateral Extra-articular Tenodesis) for high-risk cases, and do I qualify?”
-
“What is your personal re-tear rate with this approach?”
-
“How do you assess my rotational instability pre-operatively?”
-
“What is your return-to-sport testing protocol, and what criteria do I need to meet before clearance?”
-
“Do you address associated injuries like a meniscus tear or cartilage damage in the same procedure?”
-
“What does my rehabilitation timeline look like specifically, not generically?”
A surgeon who is confident in the Quad-Plus approach will answer these questions directly and specifically. Vague answers about “standard protocols” should prompt a second opinion.


Five key considerations shape the Quad-Plus ACL Reconstruction Standard 2026. This infographic highlights each factor for clinicians and researchers.

Is the Quad-Plus ACL Reconstruction Standard 2026 Right for You?
You are not just a torn ligament. You are a person who wants to get back to their sport, their job, their daily life, without the constant fear that their knee is going to fail them again.
The Quad-Plus ACL Reconstruction Standard 2026 is the most evidence-backed answer to that fear that surgical science has produced. But it is not a magic solution, and it still requires a committed rehabilitation partner, a skilled surgeon who performs the combined technique regularly, and your own patience with the biological healing process.
What it does offer is the best statistical foundation for a successful, durable outcome. A 3% overall re-tear rate, 9.3% residual instability, 88% lower donor-site morbidity, and 96% patient satisfaction are not marketing claims. They are published, peer-reviewed outcomes that are now driving a genuine shift in how orthopedic surgery approaches the ACL in 2026.
“The body wants to heal. Our job as patients, clinicians, and educators is to give it the best possible foundation to do so.”
If you are dealing with ongoing knee hurt from an ACL tear or are evaluating your reconstruction options, start by getting comprehensive information and then having a detailed conversation with a surgeon who specializes in this specific approach. The difference in your long-term outcome could be enormous.
Conclusion
The ‘Quad-Plus’ ACL Reconstruction Standard 2026 is not hype. It is the convergence of better graft science, smarter surgical augmentation, and a clearer understanding of why ACL repairs have historically failed at such high rates in young, active patients.
By combining the structural advantages of the quadriceps tendon graft with the rotational control that LET provides, this standard addresses the two biggest failure points in ACL reconstruction simultaneously. The result is a four-fold reduction in re-tear rates, dramatically lower residual instability, and patient satisfaction scores that no previous technique has matched.
If you are facing an ACL reconstruction decision in 2026, you deserve to walk into that conversation armed with the knowledge that a better standard exists. Learn about your ACL injury and support options, understand the associated structures like your PCL and cartilage, and don’t settle for a surgical plan that doesn’t reflect what the science says in 2026.
Your knee pain has a story, and the Quad-Plus ACL Reconstruction Standard 2026 is one of the most important chapters in writing a better ending to it. For a deeper understanding of all the forces at play in your knee, explore our comprehensive guide to understanding, managing, and overcoming knee pain and take the next step toward getting back to the life you want to live.