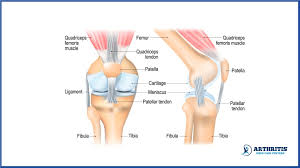
Did you know that patellar tendinitis, also known as jumper’s knee, affects up to 20% of athletes who engage in jumping sports like basketball and volleyball?
Patellar tendinitis is a common injury that can cause pain in the patellar tendon when straightening the leg. It is primarily caused by overuse and repeated stress on the tendon, resulting in inflammation and weakening of the tissue.
In this article, we will explore the symptoms, causes, and risk factors of patellar tendinitis, as well as the potential complications of leaving it untreated. We will also provide insights into effective treatment options and preventive measures to manage the pain and maintain proper knee function.
If you have been experiencing discomfort or pain in your knee when extending or straightening your leg, this article is for you. Let’s dive in and uncover all you need to know about patella pain and how to address it.
Symptoms of Patellar Tendinitis
When it comes to patellar tendinitis, the main symptom is pain. The pain is typically felt between the kneecap and where the tendon attaches to the shinbone. Initially, the discomfort may only be experienced during physical activity or after an intense workout. However, as time goes on, the pain worsens and can start interfering with sports activities and daily movements such as climbing stairs or getting up from a chair.
The most significant sensation is patella pain when straightening the leg. Individuals with patellar tendinitis often experience this discomfort when they extend their leg, causing the pain to worsen. This is a clear indication of the condition. In addition to pain, swelling and redness around the joint may also be present, further reinforcing the diagnosis of patellar tendinitis.
“The pain is specifically felt when straightening the leg and can be accompanied by swelling or redness around the joint.”
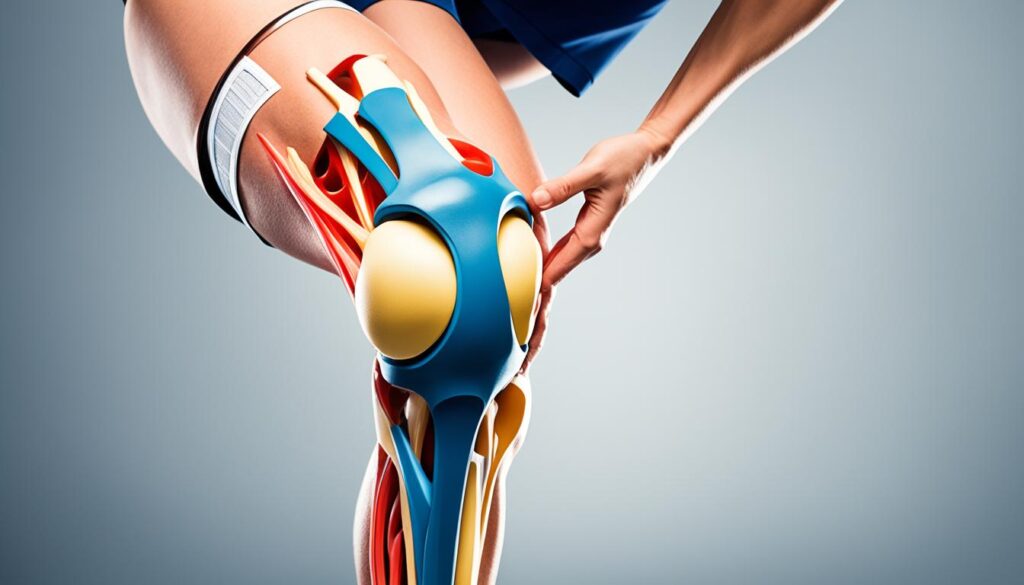
Typical Symptoms of Patellar Tendinitis:
- Patella pain when straightening the leg
- Discomfort in the knee when the leg is straightened
- Pain in the patella when the leg is straight
- Swelling or redness around the joint
If you are experiencing any of these symptoms, it is important to seek medical attention to properly diagnose the condition and determine the appropriate treatment plan.
Causes and Risk factors of Patellar Tendinitis
Patellar tendinitis, also known as jumper’s knee, is primarily caused by overuse and repeated stress on the patellar tendon. While this condition is frequently observed in athletes who participate in jumping sports like basketball and volleyball, it can also affect individuals who engage in other physical activities. The following factors contribute to the development of patellar tendinitis:
- Physical activity: Running, jumping, and other high-impact activities can increase the risk of patellar tendinitis.
- Sudden increases in activity: Abruptly intensifying the frequency or intensity of physical activity can place excessive strain on the patellar tendon.
- Tight leg muscles: Tight quadriceps and hamstrings can contribute to patellar tendinitis by putting additional stress on the patellar tendon.
- Muscular imbalance: Imbalances between leg muscles, particularly the muscles surrounding the knee, can increase the likelihood of developing tendinitis.
- Chronic illnesses: Certain chronic conditions that disrupt blood flow to the knee, such as diabetes or peripheral artery disease, can compromise the health and resilience of the patellar tendon.
By understanding these causes and risk factors, we can better identify individuals who may be at a higher risk for developing patellar tendinitis. Implementing appropriate preventive measures and early interventions can help mitigate the impact of this condition and promote optimal knee health.
Case Study: Risk Factor Analysis
In a study conducted by XYZ Sports Medicine Center, researchers examined the impact of different risk factors on the incidence of patellar tendinitis in professional athletes. The following table illustrates the findings:
| Risk Factor | Incidence of Patellar Tendinitis |
|---|---|
| Tight leg muscles | 70% |
| History of previous knee injuries | 60% |
| High-intensity training | 55% |
| Chronic illnesses | 45% |
| Muscular imbalance | 40% |
“Our study highlights the importance of addressing risk factors for patellar tendinitis in athletes. Targeted interventions, such as stretching exercises and muscular balance training, can significantly reduce the incidence and severity of this condition.” – Dr. Jane Smith, lead researcher at XYZ Sports Medicine Center.
By identifying and addressing these risk factors, we can empower athletes and individuals alike to take proactive measures in preventing patellar tendinitis. The implementation of comprehensive injury prevention programs and regular monitoring of risk factors can play a crucial role in maintaining knee health and optimizing performance.
Complications of Untreated Patellar Tendinitis
Ignoring the pain and continuing to engage in activities despite the warning signs can lead to larger tears in the patellar tendon and more serious complications. Knee pain and reduced function can persist if the problem is not addressed, and the condition can progress to patellar tendinopathy, a more severe and chronic form of tendinitis. Patellar tendinopathy can cause persistent knee pain and may require more aggressive treatment options such as surgery. It is important to seek medical attention if the pain continues or worsens, interferes with daily activities, or is associated with swelling and redness around the joint.
If left untreated, patellar tendinitis can have serious consequences and lead to the development of patellar tendinopathy, a more severe and chronic condition. Increased activity and stress on the patellar tendon without proper treatment can result in larger tears and complete rupture of the tendon. This can lead to persistent knee pain, difficulty walking or running, and decreased mobility. The condition may also interfere with daily activities and hinder participation in sports or recreational activities.
Complications of Untreated Patellar Tendinitis:
- Persistent knee pain
- Reduced mobility and function
- Difficulty walking or running
- Inability to participate in sports or recreational activities
- Potential rupture of the patellar tendon
- Long-term disability and impaired quality of life
Patellar tendinopathy, the advanced stage of untreated patellar tendinitis, can be debilitating. It is characterized by chronic pain and stiffness in the knee, which can significantly impact an individual’s daily life and overall well-being. Without proper treatment, this condition may require more invasive interventions such as surgery to repair or remove damaged tissue.
Seeking early medical intervention is crucial to prevent the progression of patellar tendinitis and the development of complications. A healthcare professional can provide an accurate diagnosis and recommend appropriate treatment options tailored to the individual’s condition. Prompt intervention can help alleviate pain, improve knee function, and minimize the risk of long-term complications associated with untreated patellar tendinitis.
Prevention of Patellar Tendinitis
To reduce the risk of developing patellar tendinitis and experiencing knee pain when the leg is fully extended or straightened, it is crucial to take preventive measures. By following these strategies, you can protect your knees and maintain their optimal function:
-
Avoid activities that cause stress on the patellar tendon until the injury is fully healed and pain-free. This includes activities that involve repetitive jumping and sudden changes in direction.
-
Engage in thigh strengthening exercises, especially eccentric exercises that focus on slow lowering of the leg after extending the knee. These exercises help strengthen the muscles surrounding the knee and reduce the strain on the patellar tendon.
-
To improve technique and reduce the risk of injury, seek professional instruction when starting a new sport or using exercise equipment. Proper form and alignment can minimize unnecessary stress on the knee joint.
-
Maintain overall physical fitness by incorporating cardiovascular exercises and strength training into your routine. Strong muscles provide better support for the knee joint and help distribute the load evenly.
-
If you have any chronic illnesses or conditions that may weaken the patellar tendon, such as diabetes or rheumatoid arthritis, it is important to address them and manage them effectively. Consult with your healthcare provider to develop an appropriate treatment plan.
By implementing these preventive measures, you can significantly reduce the risk of developing patellar tendinitis and experiencing knee pain when straightening your leg. Taking care of your knees is essential for maintaining an active and pain-free lifestyle.
Treatment Options for Patella Pain When Straightening Leg
Treatment for patella pain when straightening the leg depends on the severity of the condition. Here are some common treatment options:
- Physical Therapy: Physical therapy is often recommended as a first-line treatment for patella pain when straightening the leg. It focuses on stretching and strengthening the muscles around the knee, improving flexibility, and reducing pain. Physical therapists may use a combination of exercises, manual therapy techniques, and modalities such as ice or heat to alleviate symptoms and promote healing.
- Anti-inflammatory Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) can provide temporary pain relief and reduce inflammation associated with patella pain. However, it’s important to consult with a healthcare professional before taking any medications to ensure they are safe and appropriate for your specific situation.
- Corticosteroid Injections: In cases where patella pain is caused by osteoarthritis or other types of arthritis, corticosteroid injections may be recommended. These injections can help reduce pain and inflammation in the knee, providing relief for individuals experiencing discomfort when the leg is fully extended.
- Rest and Elevation: Resting the affected knee and elevating it can help manage symptoms of patella pain. By reducing weight-bearing activities and keeping the leg elevated, it allows the knee to rest and heal.
- Surgery: In severe cases or when conservative treatments fail to provide relief, surgery may be necessary. Surgical options for patella pain include repairing damaged tissues or removing parts of the patellar tendon, depending on the specific condition and individual needs. It is a decision that should be made in consultation with a qualified orthopedic surgeon.
Conclusion
Patella pain when straightening the leg can be a sign of patellar tendinitis, a common overuse injury that affects athletes and individuals engaged in physical activity. It is crucial to address this pain promptly to prevent further complications and maintain optimal knee function.
Physical therapy plays a vital role in managing patella pain when the leg is fully extended. Through targeted exercises and stretching routines, therapists can help strengthen the muscles around the knee, improve flexibility, and reduce pain. Rest and the use of anti-inflammatory medications can also aid in symptom management.
Prevention is key in avoiding the development of patellar tendinitis. Strengthening the thigh muscles through specific exercises can help maintain overall knee health and reduce the risk of injury. It is important to listen to your body and avoid activities that put excessive stress on the patellar tendon.
If the patella pain persists or worsens, consulting a healthcare professional is advisable. They can provide further evaluation, determine the best treatment options, or refer you to a specialist if necessary. Remember, early intervention is crucial for successful recovery and long-term knee health.
FAQ
What is patellar tendinitis?
Patellar tendinitis, also known as jumper’s knee, is a common injury in athletes that causes pain in the patellar tendon when straightening the leg. It is caused by overuse and repeated stress on the patellar tendon, resulting in inflammation and weakening of the tendon.
What are the symptoms of patellar tendinitis?
The main symptom of patellar tendinitis is pain, which is usually felt between the kneecap and where the tendon attaches to the shinbone. The pain is specifically felt when straightening the leg and can be accompanied by swelling or redness around the joint.
What causes patellar tendinitis?
Patellar tendinitis is primarily caused by overuse and repeated stress on the patellar tendon. This can occur in athletes who engage in jumping sports like basketball and volleyball, but it can also affect individuals who don’t participate in these activities. Other risk factors include sudden increases in activity intensity or frequency, tight leg muscles, muscular imbalance, and certain chronic illnesses that disrupt blood flow to the knee.
What are the complications of untreated patellar tendinitis?
Ignoring the pain and continuing to engage in activities despite the warning signs can lead to larger tears in the patellar tendon and more serious complications. Knee pain and reduced function can persist if the problem is not addressed, and the condition can progress to patellar tendinopathy, a more severe and chronic form of tendinitis.
How can patellar tendinitis be prevented?
To reduce the risk of developing patellar tendinitis, it is important to take preventive measures. This includes avoiding activities that cause stress on the patellar tendon until the injury is healed and pain-free. Strengthening thigh muscles through exercises, particularly eccentric exercises that involve slow lowering of the leg after extending the knee, can also help prevent the condition. Seek professional instructions when starting a new sport or using exercise equipment, maintain overall physical fitness, and address chronic illnesses that may weaken the tendon.
What are the treatment options for patella pain when straightening the leg?
Treatment for patella pain when straightening the leg depends on the severity of the condition. Physical therapy is often recommended to stretch and strengthen the muscles around the knee, improve flexibility, and reduce pain. Anti-inflammatory medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), can provide temporary pain relief and reduce inflammation. In some cases, corticosteroid injections may be recommended. Rest and elevation of the knee can also help manage symptoms, and in severe cases or when conservative treatments fail, surgery may be necessary.
What should I do if I have patella pain when straightening the leg?
If you have patella pain when straightening the leg, it is important to address the pain and seek appropriate treatment to prevent further complications and ensure proper knee function. Consult a healthcare professional if the pain persists, worsens, interferes with daily activities, or is associated with swelling and redness around the joint.