This month we explore studies on genes responsible for osteogenesis (bone development), the link between thyroid function and osteoporosis, and the life-saving benefits of walking.
First, we will analyze new research that clarifies how certain bone cell precursors become bone-building cells. This discovery could point to new therapies for osteoporosis.
Next, we’ll examine a review of studies delving into the relationship between osteoporosis risk and thyroid-stimulating hormone (TSH), providing new evidence on the limited efficacy of osteoporosis drugs.
Finally, a comprehensive new study highlights the significant impact of daily walking on life expectancy, a finding that is sure to motivate you to lace up your walking shoes.
Research suggests a new way to combat bone loss
A new study published last August in the FASEB journal found that expression of a certain gene may help prevent bone loss associated with postmenopausal osteoporosis.
The experiment studied laboratory rats to investigate how differentiation of precursor cells called bone marrow mesenchymal stem cells (BMSCs) influence bone remodeling. Researchers discovered genes that regulate the osteogenic differentiation of BMSCs. In other words, they identified which genes influence BMSCs to become bone-building cells.
Ultimately, the study authors found a gene called AT-hook 1 (Hmga1) with high mobility group, which had a positive impact on bone loss.
Relevant excerpt
“Tests on rats showed an increase in Hmga1 expression during bone formation, but a decrease when the rats underwent ovariectomy, which simulated the conditions of menopause. Introducing more Hmga1 to these rats led to a remarkable recovery in bone resorption.
Yihe Hu, PhD, from Zhejiang University in China, the lead author, noted: “Our study showed that Hmga1 prevents bone loss by promoting the osteogenic differentiation of BMSCs in osteoporosis rats, suggesting that Hmga1 could be an important therapeutic target for osteoporosis. are.”1
Although the research was conducted on rats and not humans, the genetic processes are often similar, although we cannot be certain that all findings will apply directly to human biology.
Unfortunately, this intriguing discovery about gene activation in bone remodeling could be primarily aimed at the development of new pharmaceutical interventions. If the drug is similar to other similar drugs on the market, it will use a man-made compound to artificially increase Hmga1 expression – with currently unknown side effects.
Short content
In a study in rats, researchers identified a gene called high mobility group AT-hook 1 (Hmga1), which had a positive impact on bone loss. In rats, introducing more Hmga1 prevented bone loss. Pharmaceutical companies will likely try to develop a new drug based on this discovery.
Healthy thyroid function reduces the incidence of osteoporosis
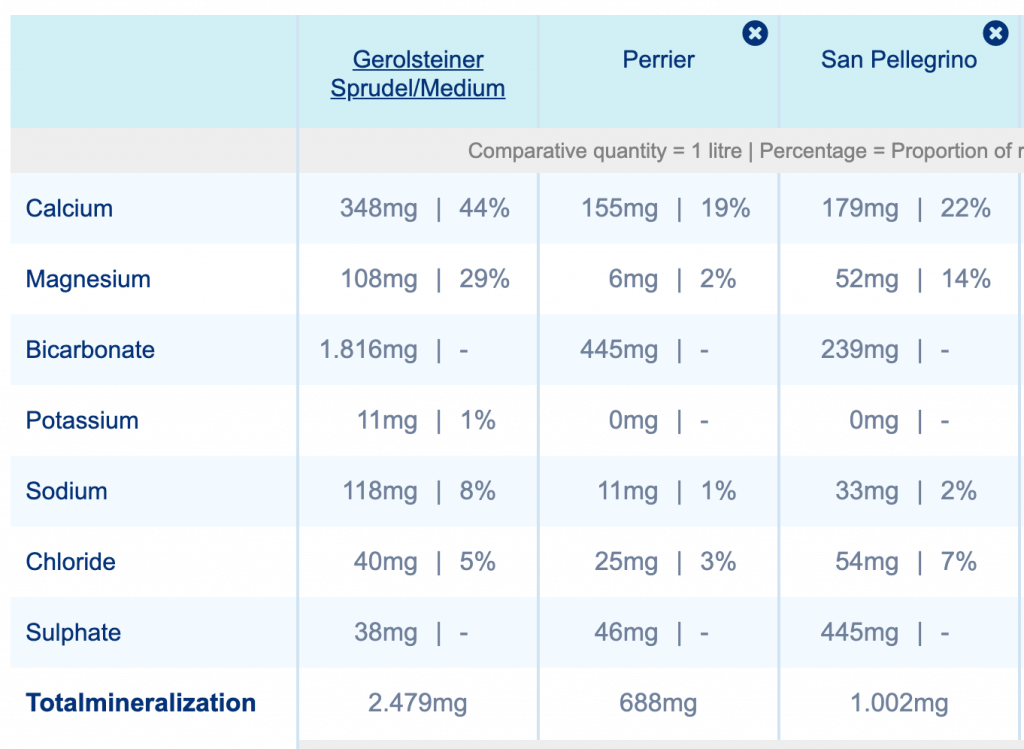
A meta-analysis recently published in the journal BMC Women’s Health found that levels of thyroid-stimulating hormone (TSH) at the high end of the normal range were associated with a reduced risk of osteoporosis in postmenopausal women.
The study authors analyzed 19 observational studies that collectively included 23,960 participants. Those studies provided information about the participants’ TSH levels and bone mass.
TSH is a hormone released by the pituitary gland that controls the thyroid gland, which in turn produces thyroid hormones. The hormones produced by the thyroid gland regulate energy expenditure and metabolism in all body systems.
Relevant excerpt
“According to the report, TSH was positively correlated with bone mineral density. After adjusting for confounding factors including age, body mass index (BMI) and bone mineral density, multivariate logistic regression showed that individuals with low TSH levels were almost twice as likely to have osteoporosis compared to individuals with high TSH levels. In addition, the risk of osteoporosis remained relatively similar among participants with low TSH who took anti-osteoporosis medications, compared to individuals who did not take the medications.”2
The central finding of this study highlights the crucial link between thyroid health and bone health. The connectivity of these systems helps explain why a holistic approach to preventing and reversing osteoporosis is more effective than Big Pharma’s narrow and harmful approach.
Furthermore, this study found that low TSH levels negated any potential benefit from anti-osteoporosis drugs. These data once again confirm how ineffective osteoporosis medications are.
Short content
A meta-analysis of 19 studies found that participants with thyroid-stimulating hormone (TSH) levels at the high end of the normal range were less likely to be diagnosed with osteoporosis. Additionally, they found that in participants with low TSH levels, there was no significant difference in bone mass between those who did and did not take osteoporosis medications. This shows how osteoporosis medications are ineffective.
Walk further to live longer
A large meta-analysis published in the European Journal of Preventive Cardiology found that walking at least 3,967 steps per day reduced the risk of death from any cause, and that walking 2,337 steps per day increased the risk of death reduced cardiovascular disease.
These incredible results came from analyzing 226,889 participants in 17 different studies around the world. In addition to the minimum number of steps to achieve the basic benefits, the researchers noted that additional steps yielded more benefits. The participants’ mortality risk decreased significantly with every 500 to 1,000 additional steps.
An increase of 1,000 steps per day was associated with a 15% reduction in the risk of death from any cause. An increase of 500 steps per day was associated with a 7% decrease in cardiovascular disease deaths. The benefits continued to accumulate up to the upper limit of steps observed in the study, which was 20,000 steps per day.
Relevant excerpt
“Maciej Banach, professor of cardiology at the Medical University of Lodz, says: “In a world where we have increasingly sophisticated medicines to tackle specific conditions such as cardiovascular disease, I think we should always emphasize that lifestyle changes, including diet and exercise, one of the main heroes of our analysis, could be at least as effective or even more effective in reducing cardiovascular risk and prolonging lives. “3
These are powerful words from Professor Banach and they reflect the core principle of the Osteoporosis Reversal Program. Diet, exercise, and lifestyle changes are the most effective tools (and certainly the safest tools) for improving health, building bone, and prolonging life.
You can take immediate action on this discovery by putting on your walking shoes and going for a walk. As Savers know, walking also benefits your bone health, which undoubtedly contributes to its power as a life extender.
Short content
A comprehensive meta-analysis of 17 studies found that walking at least 3,967 steps per day reduced the risk of death from any cause, and that walking 2,337 steps per day reduced the risk of dying from cardiovascular disease. The life extension benefits increased significantly with every additional 500 to 1,000 steps participants took, all the way up to the upper limit considered in the studies, 20,000 steps per day.
What this means for you
Staying healthy and independent requires a healthy diet, consistent exercise and wise lifestyle decisions. Current studies underline this truth, even as some indicate that new pharmaceutical products are in development.
The Osteoporosis Reversal Program takes full advantage of the latest research to provide a drug-free path to stronger bones and a fuller, healthier life. As today’s studies show, nourishing your body with natural health practices, such as regular exercise, proves to be more effective than resorting to quick medications.
Unlike medications, diet, exercise and lifestyle choices typically do not have negative side effects. In fact, you’ll find the opposite is true. As your bone health improves, so will your energy, your strength, and your overall well-being.
Keep learning, keep getting stronger, and stay on your all-natural path to a long-lasting and independent future.
References
1 https://www.revyuh.com/news/lifestyle/health-and-fitness/how-to-avoid-the-risk-of-osteoporosis-study-suggests-a-new-way-to-fight-brittle- bone disease/
2 https://www.endocrinologyadvisor.com/home/topics/androgen-and-reproductive-disorders/normal-tsh-levels-may-decrease-postmenopausal-osteoporosis-risk/
3 https://www.eurekalert.org/news-releases/997859