Introduction
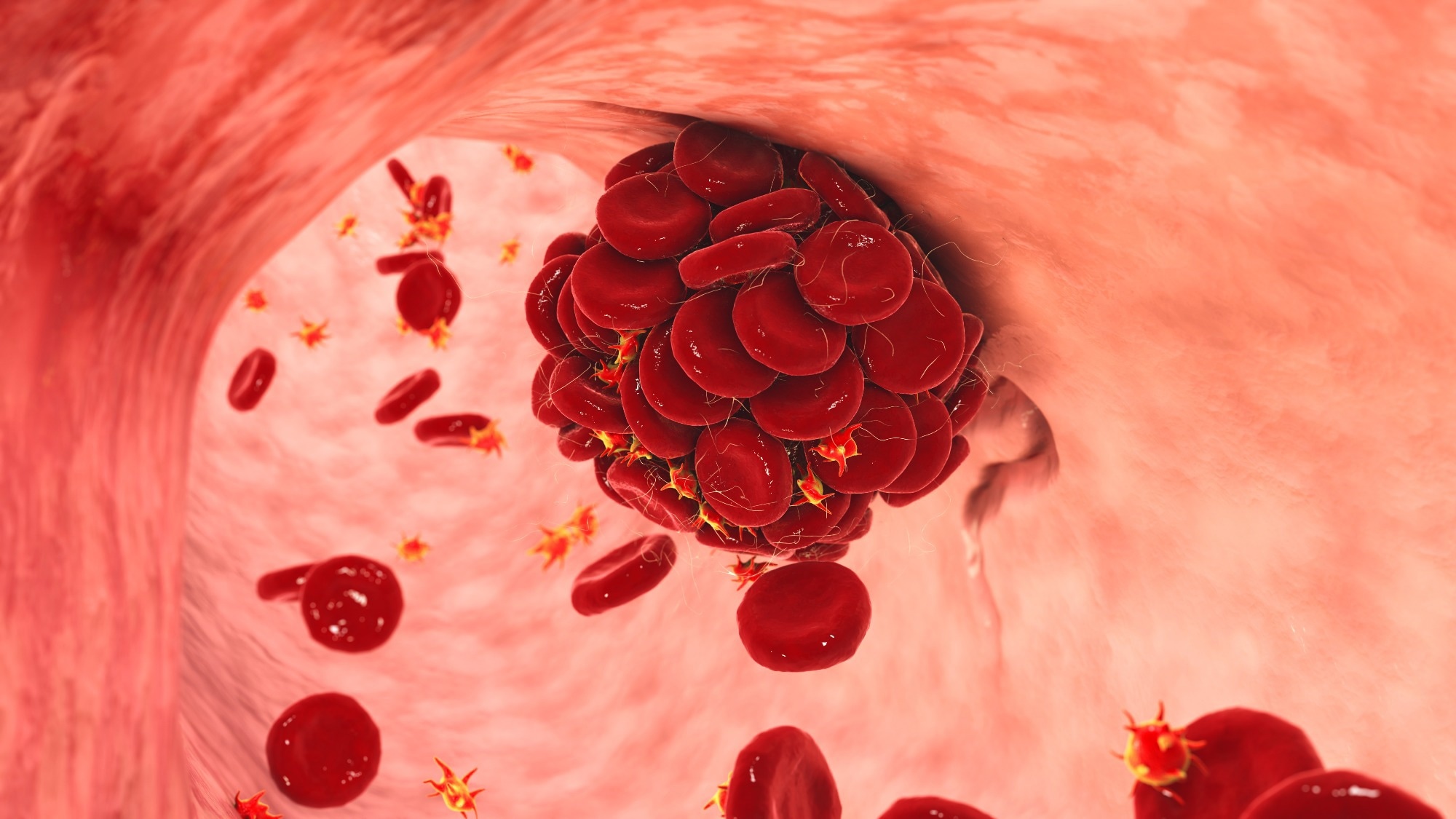
Rheumatoid arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints, leading to pain, stiffness and swelling. Although the exact cause of RA remains unknown, research suggests that both genetic and environmental factors of rheumatoid arthritis play an important role in its development. No single trigger will cause RA, but rather there is a complex interplay of genetics and environmental triggers that can ‘initiate’ the development of rheumatoid arthritis. Each of these factors is unique to the person and all contribute to the onset and progression of this condition.
Understanding rheumatoid arthritis
Before we delve into the environmental factors, it is important to have a basic understanding of rheumatoid arthritis. RA is a chronic inflammatory disease that mainly affects the joints, but can also affect other organs. It is characterized by the immune system mistakenly attacking the body’s own tissues, especially the synovium, which lines the joints.
Environmental triggers of rheumatoid arthritis
Although genetics contribute to a person’s susceptibility to RA, environmental factors can trigger the disease in individuals with a genetic predisposition. These triggers can be external factors that interact with the body’s immune system and potentially lead to the development of RA. Several environmental factors have been identified and studied in association with rheumatoid arthritis.
Genetic predisposition and environmental factors
Individuals with certain genetic variations are more likely to develop rheumatoid arthritis. However, genetic predisposition alone is not sufficient to cause the disease. Environmental factors play a crucial role in the onset of RA in genetically susceptible individuals. Factors such as infections, smoking, diet, air pollution, stress, hormonal changes, weather conditions and exposure to chemicals are mentioned as possible triggers.
The role of infections in causing rheumatoid arthritis
Infections, especially those caused by certain bacteria and viruses, have been linked to the development of rheumatoid arthritis. It is believed that these infections can trigger an abnormal immune response, leading to the production of antibodies that attack the body’s own tissues. This process can eventually cause the onset of RA in susceptible individuals.
The impact of smoking on rheumatoid arthritis
Smoking has long been recognized as a major environmental cause of rheumatoid arthritis. Research has shown that smokers have a higher risk of developing RA than non-smokers. The chemicals in tobacco smoke can activate immune cells and promote inflammation, contributing to the development and progression of the disease.
Diet and rheumatoid arthritis
Although the relationship between diet and rheumatoid arthritis is complex and not yet fully understood, certain dietary factors have been linked to the risk and severity of RA. For example, diets rich in omega-3 fatty acids, found in oily fish and flaxseed, have shown potential anti-inflammatory effects and may help reduce symptoms of RA. On the other hand, diets high in saturated fats and processed foods can promote inflammation and worsen the condition.
The influence of air pollution
Air pollution, especially particulate matter (PM2.5) and diesel exhaust, has been identified as a potential environmental trigger for rheumatoid arthritis. Inhalation of these pollutants can lead to oxidative stress, inflammation and immune system dysfunction. Long-term exposure to air pollution has been linked to an increased risk of developing RA and worsening symptoms in individuals already diagnosed with the condition.
Stress and rheumatoid arthritis
Chronic stress has been implicated as a trigger for rheumatoid arthritis. Stress can compromise the immune system and promote inflammation, potentially worsening RA symptoms. Although stress alone does not cause the disease, it can contribute to its onset and influence its progression.
Hormonal factors
Hormonal changes, especially in women, have been linked to an increased risk of rheumatoid arthritis. The fluctuation of hormones, such as estrogen, during the reproductive phase and menopause can affect the immune response and contribute to the development or worsening of RA symptoms.
Weather and rheumatoid arthritis
Many people with rheumatoid arthritis report that changes in weather conditions, especially cold and damp weather, can worsen their symptoms. Others say humidity increases swelling and pain in their joints. Although the exact mechanisms behind this association are not yet fully understood, it is thought that changes in temperature and barometric pressure may influence joint inflammation and pain perception in some individuals with RA.
Chemical exposure and rheumatoid arthritis
Exposure to certain chemicals, such as solvents, pesticides and heavy metals, has been linked to an increased risk of developing rheumatoid arthritis. These chemicals can disrupt the immune system and promote inflammation, potentially triggering the onset of RA or worsening its symptoms.
Preventive measures and lifestyle changes
While it may not be possible to completely prevent rheumatoid arthritis, certain preventative measures and lifestyle changes can help reduce the risk and control symptoms. These include maintaining a healthy diet, avoiding smoking and exposure to secondhand smoke, managing stress levels, staying physically active, protecting oneself from infections and minimizing exposure to environmental pollutants and chemicals.
Conclusion
In conclusion, rheumatoid arthritis is a complex disease influenced by both genetic and environmental factors. Environmental factors of rheumatoid arthritis, such as infections, smoking, diet, air pollution, stress, hormonal changes, weather conditions, and chemical exposure may contribute to the onset and progression of RA in genetically predisposed individuals. Understanding these triggers and taking preventative measures can play an important role in controlling the disease and improving the quality of life for people with rheumatoid arthritis.
Frequently Asked Questions
1. Can rheumatoid arthritis be completely prevented?
Rheumatoid arthritis cannot be completely prevented, but certain lifestyle changes can help reduce the risk and manage symptoms effectively.
2. Are all infections associated with rheumatoid arthritis?
Although certain infections have been linked to the development of rheumatoid arthritis, not all infections have been linked to the disease.
3. Is there a specific diet for rheumatoid arthritis?
There is no one-size-fits-all diet for rheumatoid arthritis. However, a balanced and healthy diet that is rich in nutrients and low in processed foods can support overall health and possibly alleviate symptoms.
4. How does air pollution affect rheumatoid arthritis?
Air pollution, especially particulate matter and diesel exhaust, can promote inflammation and oxidative stress, potentially worsening symptoms and increasing the risk of developing rheumatoid arthritis.
5. Can stress alone cause rheumatoid arthritis?
Stress alone may not cause rheumatoid arthritis, but it can contribute to its onset and influence its progression by affecting the immune system and promoting inflammation.
Similar:
Like it Loading…
Related