Millions of Americans suffer from knee osteoarthritis, a degenerative joint condition that causes pain and limits mobility. As the search for non-invasive, drug-free treatments continues, low-level laser therapy has emerged as a promising option. This therapy involves exposing the affected tissue to low levels of red and near-infrared light, which can penetrate deep into the tissue to stimulate healing.
We will explore how this innovative treatment uses specific wavelengths of light to potentially reduce inflammation, improve circulation, and promote healing in damaged knee tissues. By examining the scientific principles behind this therapy and the typical treatment protocols, we aim to provide a comprehensive understanding of its benefits and effectiveness for knee osteoarthritis management.
Key Takeaways
- Low-level laser therapy is a non-invasive treatment option for knee osteoarthritis.
- It uses specific wavelengths of light to penetrate deep into the tissue.
- The therapy aims to reduce inflammation, improve circulation, and promote healing.
- We will examine the scientific principles and typical treatment protocols.
- The goal is to provide a comprehensive understanding of its benefits and effectiveness.
Understanding Knee Osteoarthritis and Its Impact
Understanding the complexities of knee osteoarthritis is crucial for managing its impact on daily life. Knee osteoarthritis (KOA) is a degenerative, inflammatory condition that affects the knee joint, leading to discomfort, impairment, and a lower quality of life.
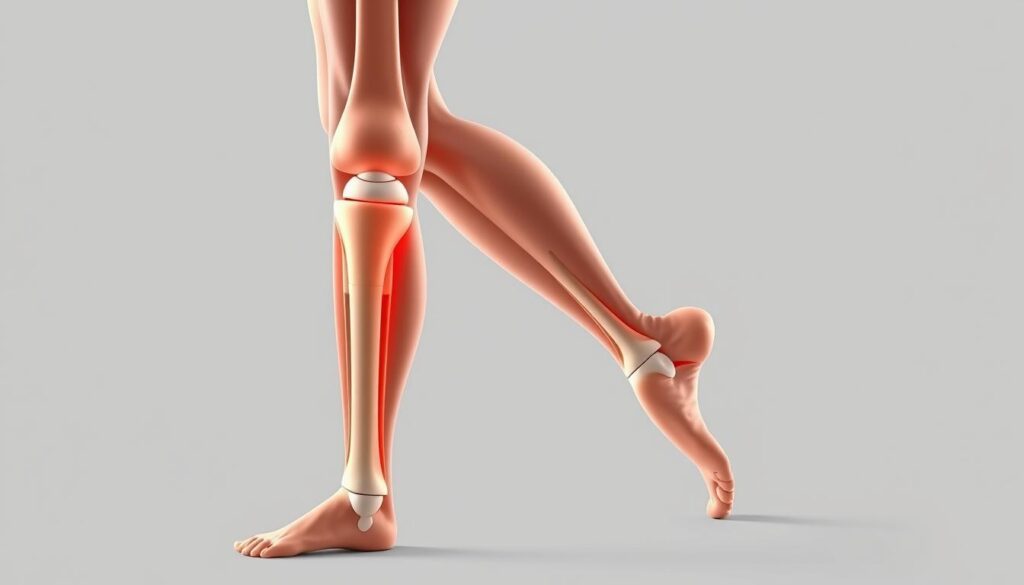
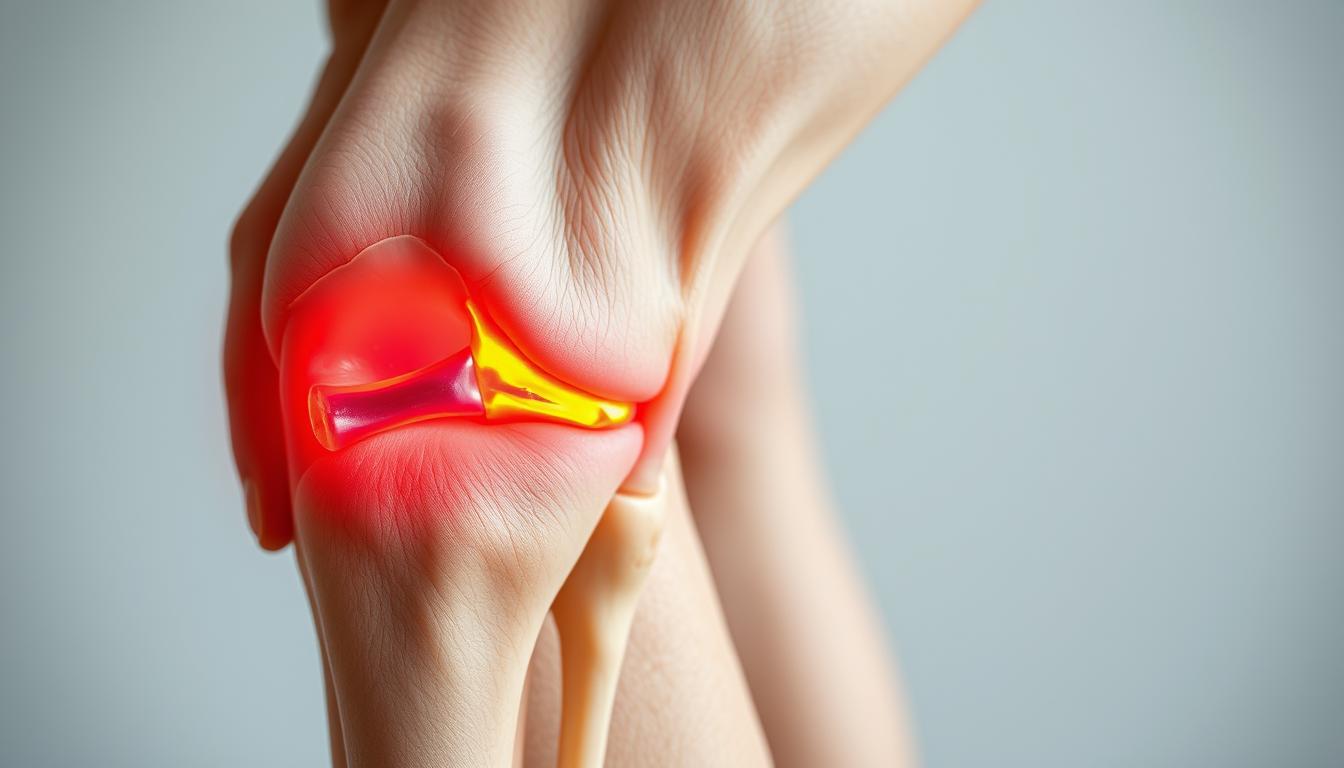
What Happens in Knee Osteoarthritis
In KOA, the cartilage that cushions the joints deteriorates, causing bone-on-bone contact. This results in pain and stiffness, particularly after periods of rest or inactivity. The condition is also characterized by swelling and a decreased range of motion, making everyday activities challenging.
The degenerative nature of KOA means that its symptoms can progress over time, from occasional discomfort during activity to persistent knee pain that significantly limits mobility and independence.
Common Symptoms and Their Effect on Quality of Life
The symptoms of KOA can have a profound impact on an individual’s life, affecting not just physical capabilities but also psychological well-being. Common symptoms include pain, stiffness, swelling, and a distinctive “creaking” or “grinding” sensation in the knee.
As KOA progresses, it can limit basic activities like walking and climbing stairs, as well as more complex activities such as exercise, work performance, and social engagement. The chronic nature of the condition can also lead to anxiety, depression, and sleep disturbances, further compounding the physical challenges.
By understanding the full spectrum of how KOA affects daily functioning, we can better appreciate the importance of finding effective management strategies that address both the physical symptoms and their broader life impacts.
What Is Cold Laser Therapy for Knee Osteoarthritis
Cold laser therapy, also known as low-level laser therapy (LLLT), is a non-invasive treatment that has gained attention for its potential in managing knee osteoarthritis. This therapy involves the application of low-intensity laser or light-emitting diodes to the affected area.
Definition and Alternative Names
Low-level laser therapy (LLLT) is characterized by the electronic level absorption of laser light without the production of heat in the visible to near-infrared spectral spectrum (390-1,100 nm). It’s also known as photobiomodulation or low-intensity laser therapy. LLLT is used for various medical conditions, including pain relief, wound healing, and inflammation reduction in knee osteoarthritis.
How It Differs from Other Laser Treatments
Cold laser therapy differs significantly from other laser treatments used in medicine, primarily in its power output, wavelength, and therapeutic mechanisms. Unlike high-power lasers used for surgical procedures, cold lasers operate at power levels typically below 500 milliwatts. The therapeutic effects of cold lasers are achieved through photobiomodulation, a process involving light-induced photochemical reactions rather than thermal effects.
The key differences between cold laser therapy and other laser-based treatments can be summarized as follows:
- Power output: Cold lasers operate at lower power levels compared to surgical lasers.
- Wavelength: Specific wavelength ranges (typically 600-1000 nm) are used for treating knee osteoarthritis due to their optimal tissue penetration properties.
- Therapeutic mechanisms: Cold laser therapy relies on photobiomodulation, distinguishing it from other laser treatments that may cause tissue destruction or ablation.
By understanding these distinctions, we can appreciate why cold laser therapy represents a unique approach to treating knee osteoarthritis.
The Science Behind Cold Laser Therapy
The therapeutic effects of cold laser therapy on knee osteoarthritis are rooted in its ability to stimulate cellular processes at the molecular level. This non-invasive treatment modality utilizes specific wavelengths of light to induce beneficial changes in tissue, promoting healing and regeneration.
Wavelengths and Their Importance
The effectiveness of cold laser therapy is significantly influenced by the wavelengths used. Typically, red and near-infrared wavelengths are employed because they can penetrate deep into tissue. These wavelengths are absorbed by cellular components, particularly cytochrome c oxidase in the mitochondria, triggering a cascade of biochemical reactions. The choice of wavelength is critical as it determines the depth of penetration and the specific biological effects that are elicited.

Photobiomodulation Process Explained
The process by which cold laser therapy exerts its effects is known as photobiomodulation (PBM). PBM involves the absorption of light energy by cells, leading to enhanced mitochondrial ATP production, improved cell signaling, and increased synthesis of growth factors. This results in multiple beneficial effects, including reduced inflammation, enhanced protein synthesis, and accelerated tissue repair. By modulating oxidative stress and inflammatory cytokine production, cold laser therapy addresses some of the underlying pathological processes in knee osteoarthritis, potentially offering benefits beyond mere pain relief.
Through the photobiomodulation process, cold laser therapy promotes regeneration and healing in damaged knee joint structures. By understanding these mechanisms, we gain insight into the therapeutic potential of cold laser therapy for knee osteoarthritis.
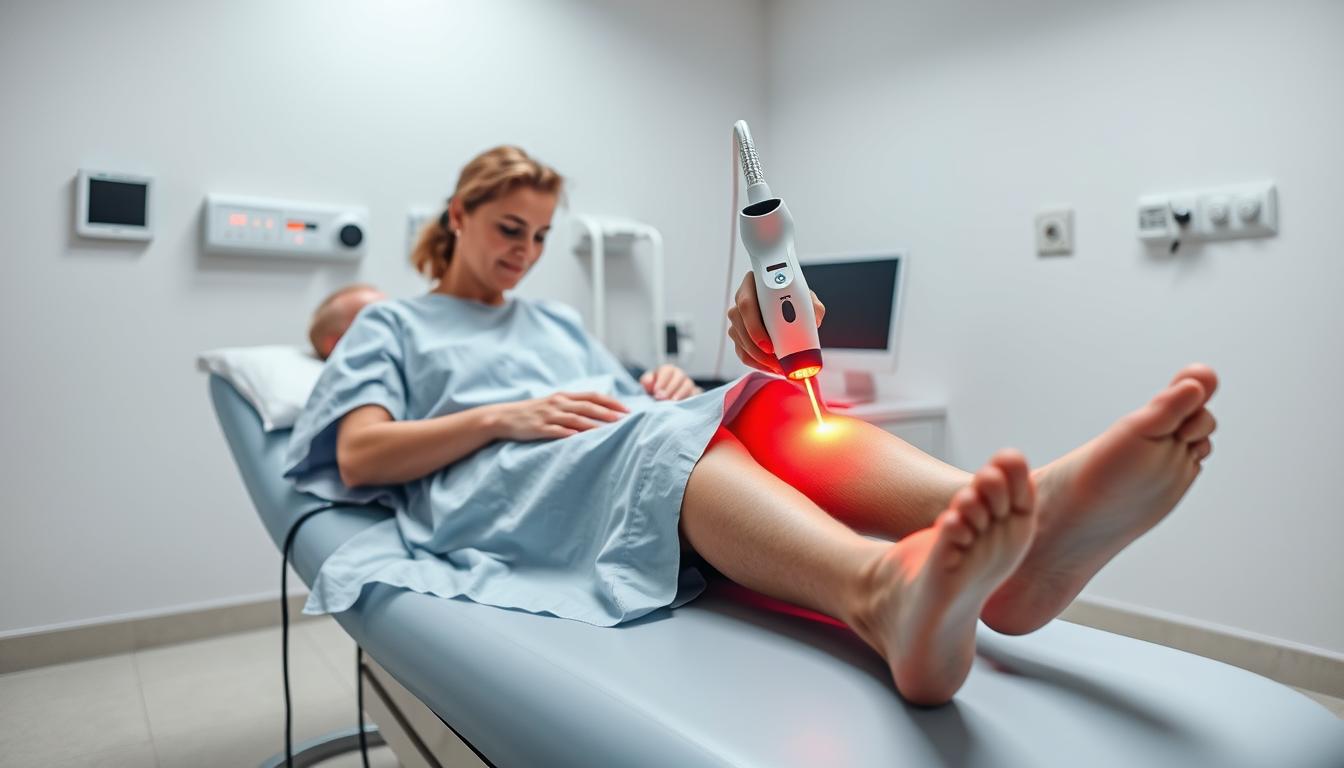
The Cold Laser Therapy Procedure
When considering cold laser therapy for knee osteoarthritis, understanding the procedure is crucial for setting realistic expectations. Cold laser therapy, also known as low-level laser therapy (LLLT) or photobiomodulation (PBM), is a non-invasive treatment that has been studied for its potential to reduce pain and inflammation in the knee.
What to Expect During Treatment
During a cold laser therapy session, a healthcare professional will position the laser device over the affected knee area. The treatment is typically painless, with some patients possibly experiencing a warm or tingling sensation. The laser emits a specific wavelength of light that penetrates the skin to stimulate cellular processes, promoting healing and reducing inflammation.
Treatment Duration and Frequency
The duration and frequency of cold laser therapy treatments can vary based on the severity of knee osteoarthritis and individual patient response. Generally, a treatment session lasts between 5 to 15 minutes per knee. Treatments are often administered 2-3 times per week initially, with the frequency adjusted based on patient progress.
| Treatment Aspect | Typical Protocol |
|---|---|
| Session Duration | 5-15 minutes per knee |
| Initial Frequency | 2-3 times per week |
| Total Sessions | 8-12 sessions or more |
Cold laser therapy is a cumulative treatment, meaning that its effects build up over multiple sessions. Patients typically need to undergo several treatments before noticing significant improvement. The total number of treatments required can range from a few weeks to several months, depending on the condition’s severity and the patient’s response to therapy.
Benefits of Cold Laser Therapy for Knee Pain
Cold laser therapy offers a multifaceted approach to managing knee pain by addressing both the symptoms and underlying causes. This treatment modality has gained attention for its potential to provide relief and promote healing in patients suffering from knee osteoarthritis.
Pain Reduction Mechanisms
One of the primary benefits of cold laser therapy is its ability to reduce pain. The therapy achieves this through several mechanisms. The light energy emitted during treatment helps to lessen inflammation and promote regeneration of damaged tissue.
Studies have shown that this can lead to a significant reduction in pain experienced by patients. For instance, a study observed that during the treatment period, weekly thermograms showed increasing temperature in previously cold areas, indicating improved circulation and reduced inflammation. The pain reduction effect is further supported by the observation that at follow-up measurements 2 months after treatment, thermographic changes remained elevated, suggesting sustained benefits.
Improved Circulation and Healing
Cold laser therapy also enhances circulation to the knee joint, which is vital for healing. The photobiomodulation effect stimulates vasodilation and the formation of new capillaries in the treated tissues. As a result, improved microcirculation brings more oxygen and nutrients to damaged knee structures while facilitating the removal of metabolic waste products and inflammatory mediators that can impede healing.
The enhanced circulation and subsequent healing processes contribute to the repair of damaged cartilage, synovial membrane, and other knee joint structures affected by osteoarthritis. Furthermore, cold laser therapy may influence the activity of chondrocytes and synoviocytes, potentially slowing the degenerative processes characteristic of knee osteoarthritis.
By addressing the underlying tissue damage, cold laser therapy offers benefits that extend beyond symptomatic relief. By understanding these mechanisms, patients and healthcare providers can better appreciate the potential of cold laser therapy as a valuable treatment option for knee osteoarthritis.
Clinical Evidence and Research Findings
A comprehensive understanding of cold laser therapy’s impact on knee osteoarthritis requires an examination of the latest clinical evidence and research findings. The therapy’s effectiveness is supported by a growing body of research, including systematic reviews and meta-analyses that evaluate its efficacy in treating knee osteoarthritis.
Key Studies and Their Results
Numerous studies have investigated the effects of cold laser therapy on knee osteoarthritis. A notable systematic review and meta-analysis of randomized placebo-controlled trials, involving a total sample of 1063 patients, demonstrated that low-level laser therapy (LLLT) at specific wavelengths (785-860 nm and 904 nm) significantly reduced pain and disability in patients with knee osteoarthritis.
Therapeutic Effects of Cold Laser Therapy
| Wavelength (nm) | Dosage (J) | Effects on KOA Patients |
|---|---|---|
| 785-860 | 4-8 | Significant pain reduction |
| 904 | 1-3 | Improved functional ability |
However, it’s crucial to note that not all studies are without criticism. For instance, a systematic review by Huang et al. (2015) was later criticized by Stausholm et al. (2017) for methodological deficiencies and type-II errors in their meta-analysis.
What the Systematic Reviews Tell Us
Systematic reviews have played a pivotal role in assessing the collective evidence for cold laser therapy in treating knee osteoarthritis. These reviews have addressed the variability in treatment parameters across individual studies, such as wavelength, dosage, and frequency, and their implications for interpreting the overall evidence.
The quality of evidence has evolved over time, from earlier reviews indicating limited support to more recent analyses showing consistent positive effects for specific laser parameters and treatment protocols. Nonetheless, methodological challenges persist, including issues with blinding, standardization of treatment parameters, and the selection of appropriate outcome measures.
By examining the systematic evidence, we can better understand the current scientific consensus on cold laser therapy for knee osteoarthritis and identify areas requiring further research.
Potential Side Effects and Limitations
The safety profile of cold laser therapy for knee osteoarthritis is generally favorable, but certain precautions and contraindications need to be considered.
Safety Profile of Cold Laser Therapy
Cold laser therapy is typically well-tolerated, with few side effects reported. Most patients experience no adverse effects, and the treatment is considered safe when performed by a qualified healthcare professional.
Common side effects, if any, are usually mild and temporary. Some patients may experience slight discomfort or warmth at the laser therapy site, but these effects generally resolve quickly.
When Cold Laser Therapy Isn’t Recommended
Despite its safety profile, cold laser therapy is not suitable for everyone. Certain conditions may contraindicate its use, such as the presence of cancerous lesions, as laser therapy could potentially stimulate tumor growth.
- Application directly over the thyroid gland or eyes is contraindicated.
- Pregnant women should avoid cold laser therapy due to the lack of research on its effects on the fetus.
- Patients with undiagnosed knee pain should not receive laser therapy until a proper diagnosis is made.
It’s crucial for patients to consult with their healthcare provider to determine if cold laser therapy is appropriate for their specific condition.
Ideal Candidates for Cold Laser Therapy
As with any medical treatment, cold laser therapy is not suitable for everyone, and careful patient selection is crucial for its success. We need to consider various factors to determine whether a patient can benefit from this therapy.
Medical Conditions That Respond Well
Cold laser therapy has shown promise in treating various conditions, particularly those involving pain and inflammation. Knee osteoarthritis is one such condition where this therapy has demonstrated potential benefits. Studies have indicated that cold laser therapy can help reduce knee pain and improve functional ability in patients with osteoarthritis. Other conditions that may respond well to cold laser therapy include chronic pain syndromes and inflammatory disorders.
Contraindications and Precautions
While cold laser therapy is generally considered safe, there are certain contraindications and precautions to be aware of. For instance, it’s not recommended for patients with cancerous lesions, as it may potentially stimulate tumor growth. Additionally, cold laser therapy should not be applied directly over the eyes or thyroid gland. Pregnant women are also advised to avoid this therapy due to the lack of research on its effects on the developing fetus. Patients with photosensitivity disorders or those taking photosensitizing medications require special precautions.
Proper diagnosis is essential before initiating cold laser therapy to ensure that the treatment is appropriate for the patient’s condition. This involves ruling out underlying serious conditions that may require different interventions. By carefully evaluating patients and considering these factors, healthcare providers can make informed decisions about the suitability of cold laser therapy for their patients.
Cold Laser Devices for Home Use
Cold laser therapy devices designed for home use offer a convenient and potentially effective solution for managing knee arthritis.

Features to Look For
When selecting a cold laser device for home use, several features are crucial to ensure safety and effectiveness. Optimal wavelength and adjustable intensity are key factors, as they allow for personalized treatment based on individual needs and comfort levels.
Additionally, the device should be user-friendly, with clear instructions and possibly pre-set treatment protocols for knee osteoarthritis. It’s also beneficial to look for devices with multiple treatment heads or adjustable applicators to target different areas around the knee.
Professional Guidance
Before initiating home-based cold laser therapy, it’s crucial to consult with a healthcare professional to confirm the diagnosis and discuss the suitability of this treatment for your specific condition.
A healthcare provider can offer valuable guidance on treatment parameters, including the optimal locations to treat around the knee, session duration, frequency, and the total number of treatments. They can also advise on how to integrate cold laser therapy into a comprehensive management plan that may include exercise, weight management, and conventional medical treatments.
By following professional guidance, individuals can maximize the safety and effectiveness of home-based cold laser therapy, ensuring it complements other treatments for optimal knee osteoarthritis management.
Comparing Cold Laser Therapy to Other Treatment Options
As patients explore treatment options for knee osteoarthritis, comparing the efficacy, safety, and convenience of cold laser therapy with other approaches becomes increasingly important. Knee osteoarthritis management can involve a range of strategies, from conservative treatments to surgical interventions.
Medication-Based Approaches
Medication-based approaches for knee osteoarthritis often include oral analgesics, NSAIDs, and corticosteroid injections. While these can provide symptom relief, they may have side effects and don’t address the underlying condition. In contrast, cold laser therapy is a non-pharmacological treatment that can reduce pain and inflammation without the risk of systemic side effects.
Physical and Occupational Therapy
Physical and occupational therapy play a crucial role in managing knee osteoarthritis by improving joint mobility, strengthening surrounding muscles, and enhancing functional ability. Cold laser therapy can complement these therapies by reducing pain and inflammation, potentially improving the effectiveness of exercise programs.
Surgical Interventions
Surgical options for knee osteoarthritis range from arthroscopic procedures to partial or total knee replacement. While surgery can be effective for advanced cases, it carries risks and requires significant recovery time. Cold laser therapy offers a non-invasive alternative that may delay or avoid the need for surgery in some patients.
| Treatment Option | Invasiveness | Recovery Time |
|---|---|---|
| Cold Laser Therapy | Non-invasive | Minimal to none |
| Medication-Based Approaches | Varies (oral to injections) | Varies |
| Surgical Interventions | Invasive | Significant |
Cost Considerations and Insurance Coverage
When considering cold laser therapy for knee osteoarthritis, understanding the financial implications is crucial. As with any medical treatment, the costs associated with cold laser therapy can vary widely depending on several factors.
Typical Treatment Costs
The cost of cold laser therapy sessions can differ based on the provider, location, and the number of sessions required. On average, a single session can range from $50 to $200. A typical treatment plan may involve multiple sessions over several weeks or months.
According to a study published in a reputable medical journal, the total cost for a full course of cold laser therapy can range from $500 to $2,000 or more, depending on the complexity of the case and the time required for treatment.
Navigating Insurance for Cold Laser Therapy
Insurance coverage for cold laser therapy is often limited because it is considered an alternative medicine approach by many providers. As stated in this article, “It’s a form of alternative medicine and considered unproven by many doctors and insurance providers. So, your treatments may not be covered through your health insurance.”
To navigate this complex landscape, patients should first check their insurance coverage before starting treatment. Some providers may cover cold laser therapy under specific circumstances, such as when it is deemed medically necessary.
Strategies for maximizing insurance coverage include obtaining proper referrals from healthcare providers, documenting medical necessity, and appealing denied claims with supporting clinical evidence. When insurance coverage is not available, alternative payment options such as flexible spending accounts (FSAs), health savings accounts (HSAs), and payment plans can help make cold laser therapy more accessible.
Taking the Next Step with Cold Laser Therapy
If you’re considering cold laser therapy for your knee osteoarthritis, understanding the process and what to expect is crucial. Cold laser therapy may provide temporary pain relief for osteoarthritis of the knee, but its effectiveness can vary from person to person. As an alternative medicine approach, more research is needed to fully determine its efficacy.
When exploring cold laser therapy, finding a qualified provider is essential. We recommend asking potential providers about their experience with cold laser therapy, the type of equipment they use, their treatment protocols, and the expected outcomes based on their clinical experience. This information will help you make an informed decision about your care.
Before starting therapy, establishing baseline measurements and clear treatment goals is vital. This enables an objective assessment of your progress and the treatment’s effectiveness. By setting clear goals, you and your healthcare provider can work together to optimize your treatment plan.
Cold laser therapy can be a valuable component of a comprehensive knee osteoarthritis management plan. This plan may include exercise, weight management, appropriate medications, and lifestyle modifications. By combining these approaches, you can potentially achieve better outcomes and improve your quality of life.
It’s also important to maintain realistic expectations and engage in ongoing communication with your healthcare providers. This ensures that your treatment plan is tailored to your needs and adjusted as necessary. By taking an active role in your care and staying informed, you can make the most of cold laser therapy and other treatments for knee osteoarthritis.
In conclusion, while cold laser therapy is not a one-size-fits-all solution, it may offer pain relief and improved function for some individuals with knee osteoarthritis. By understanding the benefits and limitations of this treatment and working closely with your healthcare team, you can make informed decisions about your care and take a proactive approach to managing your condition.
FAQ
What is the mechanism behind low-level laser therapy (LLLT) for knee pain relief?
We use specific wavelengths of light to stimulate cellular processes, promoting pain relief and healing. This process is known as photobiomodulation.
How long does a typical cold laser treatment session last?
A: Treatment sessions are relatively short, usually lasting between 10 to 30 minutes, depending on the severity of the condition and the treatment area.
Are there any side effects associated with cold laser therapy for osteoarthritis?
We have found that cold laser therapy is generally well-tolerated, with minimal risk of adverse effects. Some patients may experience temporary discomfort or skin sensitivity.
Can cold laser therapy be used in conjunction with other treatments for knee osteoarthritis?
Yes, we often recommend combining cold laser therapy with other treatments, such as physical therapy or exercise, to enhance its effectiveness.
How many treatments are typically required to experience significant pain relief?
The number of treatments needed can vary depending on the individual and the severity of their condition. On average, patients may require multiple sessions spaced over several weeks.
Is cold laser therapy covered by insurance?
Coverage varies depending on the insurance provider and policy. We recommend checking with your insurance company to determine the extent of coverage for cold laser therapy.
Can I use a cold laser device at home for knee pain relief?
Yes, there are cold laser devices available for home use. However, we advise consulting with a healthcare professional to ensure proper use and to discuss the most effective treatment plan.