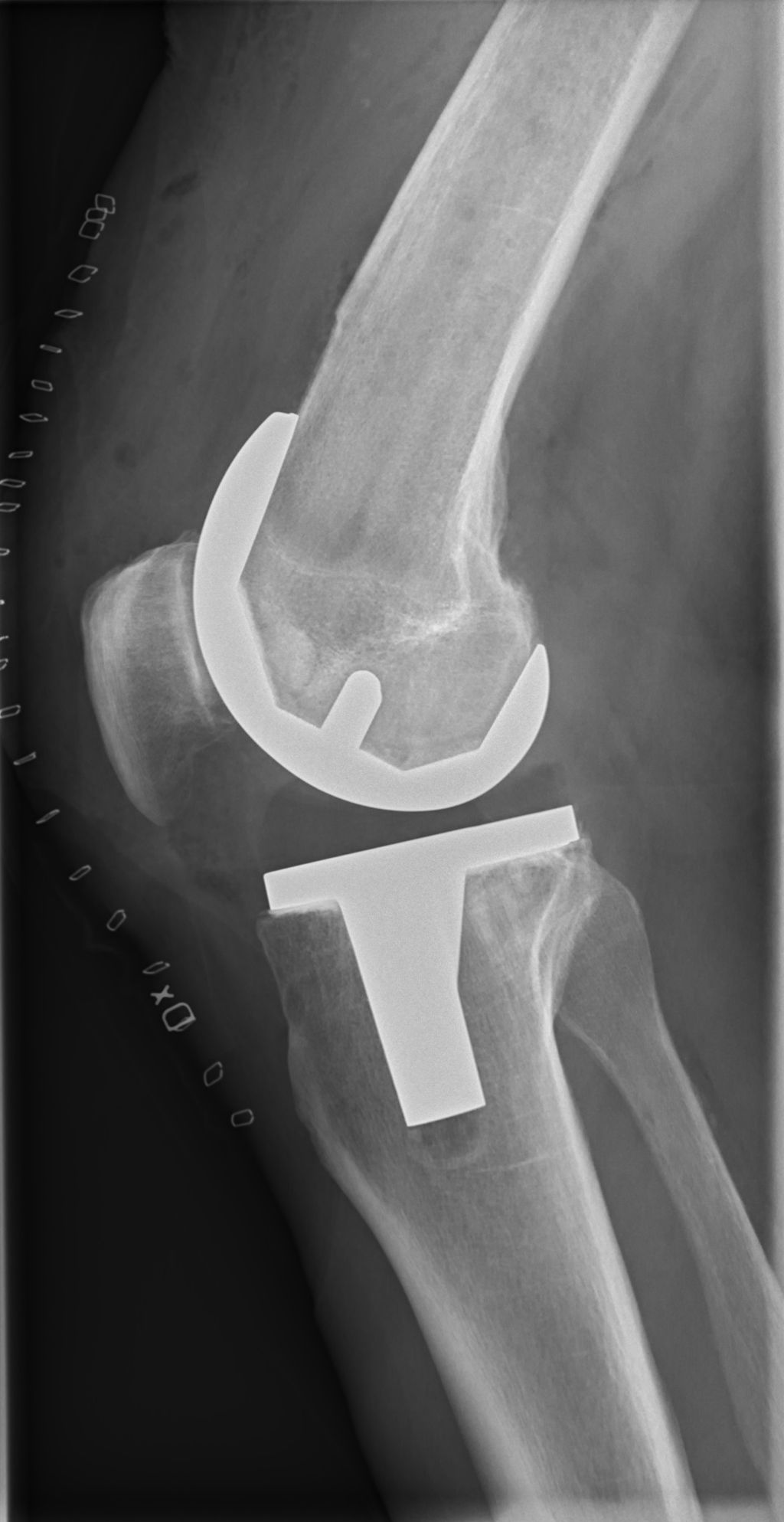
Double knee replacement surgery is a complex procedure that offers significant benefits to individuals with severe knee joint issues. This surgery involves replacing both knee joints with artificial implants, providing relief from pain, improved mobility, and enhanced quality of life. Understanding the key takeaways from this surgery is essential for patients and their families to make informed decisions about the procedure and its potential outcomes.
Key Takeaways
- Double knee replacement surgery offers significant improvement in mobility and function.
- Patients experience substantial pain relief and enjoy an enhanced quality of life after the surgery.
- The long-term success rates of double knee replacement surgery are promising, leading to improved joint function and reduced disability.
- Preoperative preparation plays a crucial role in ensuring a successful outcome of the surgery.
- Recovery and rehabilitation are vital aspects of the postoperative care, contributing to the overall success of double knee replacement surgery.
Understanding Double Knee Replacement Surgery
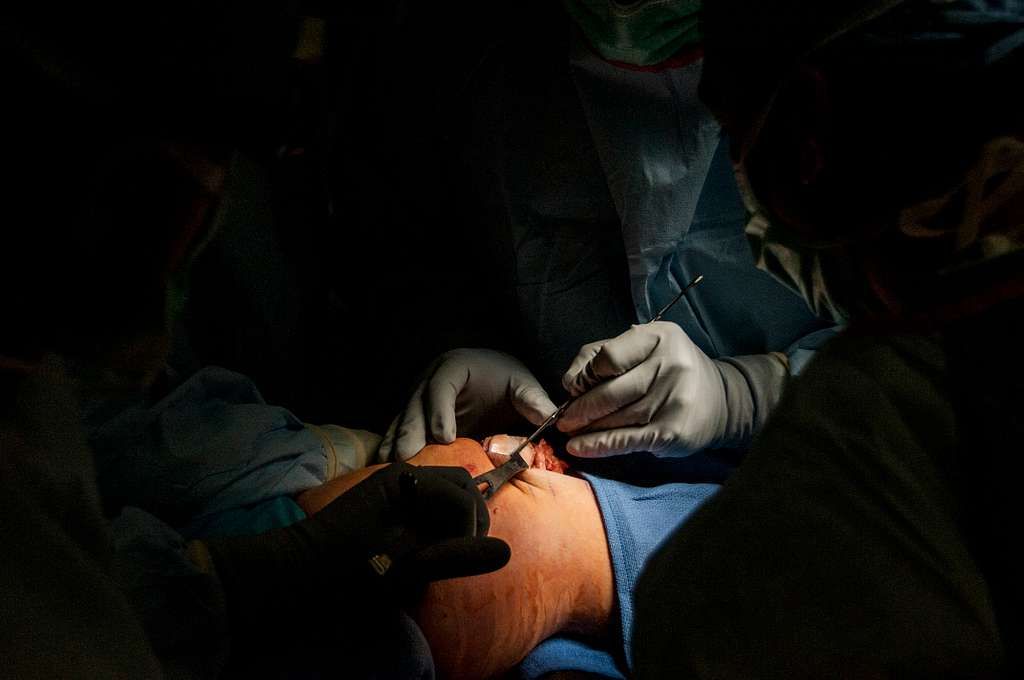
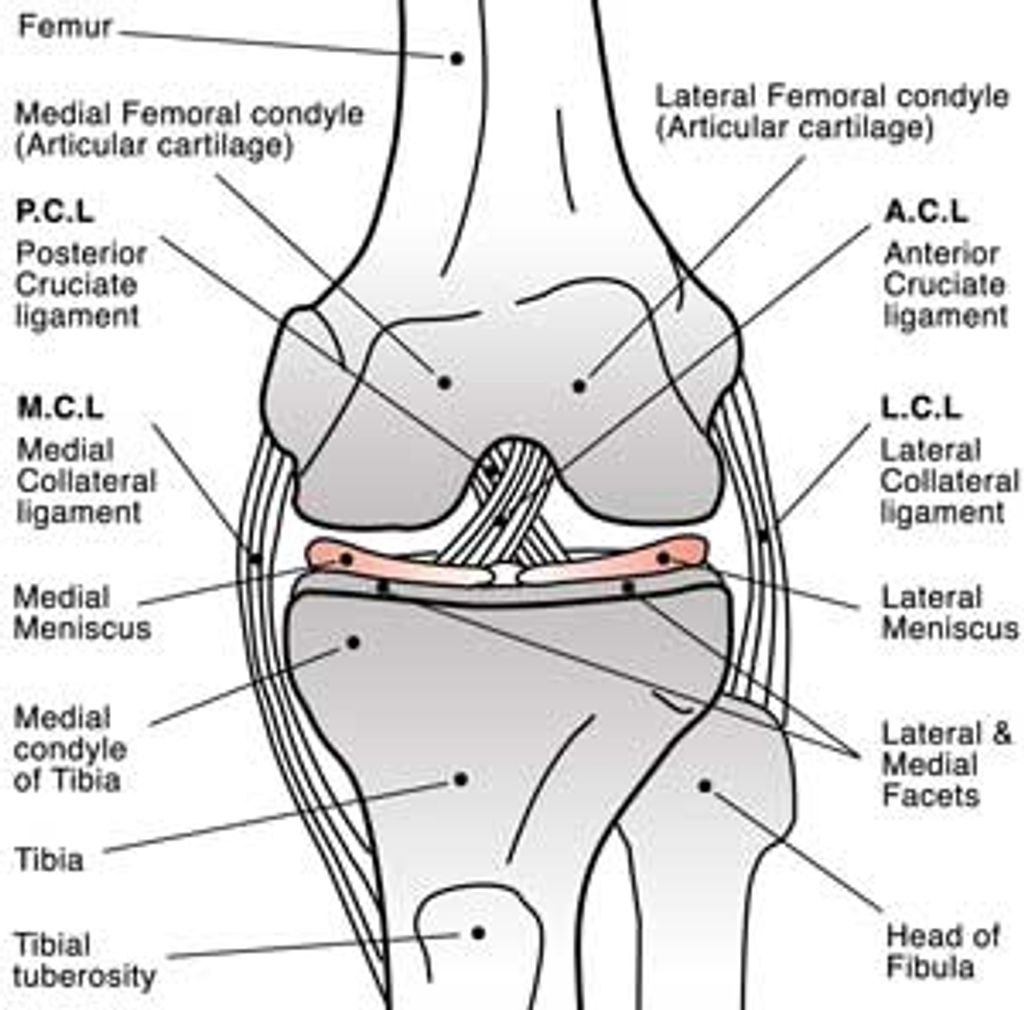
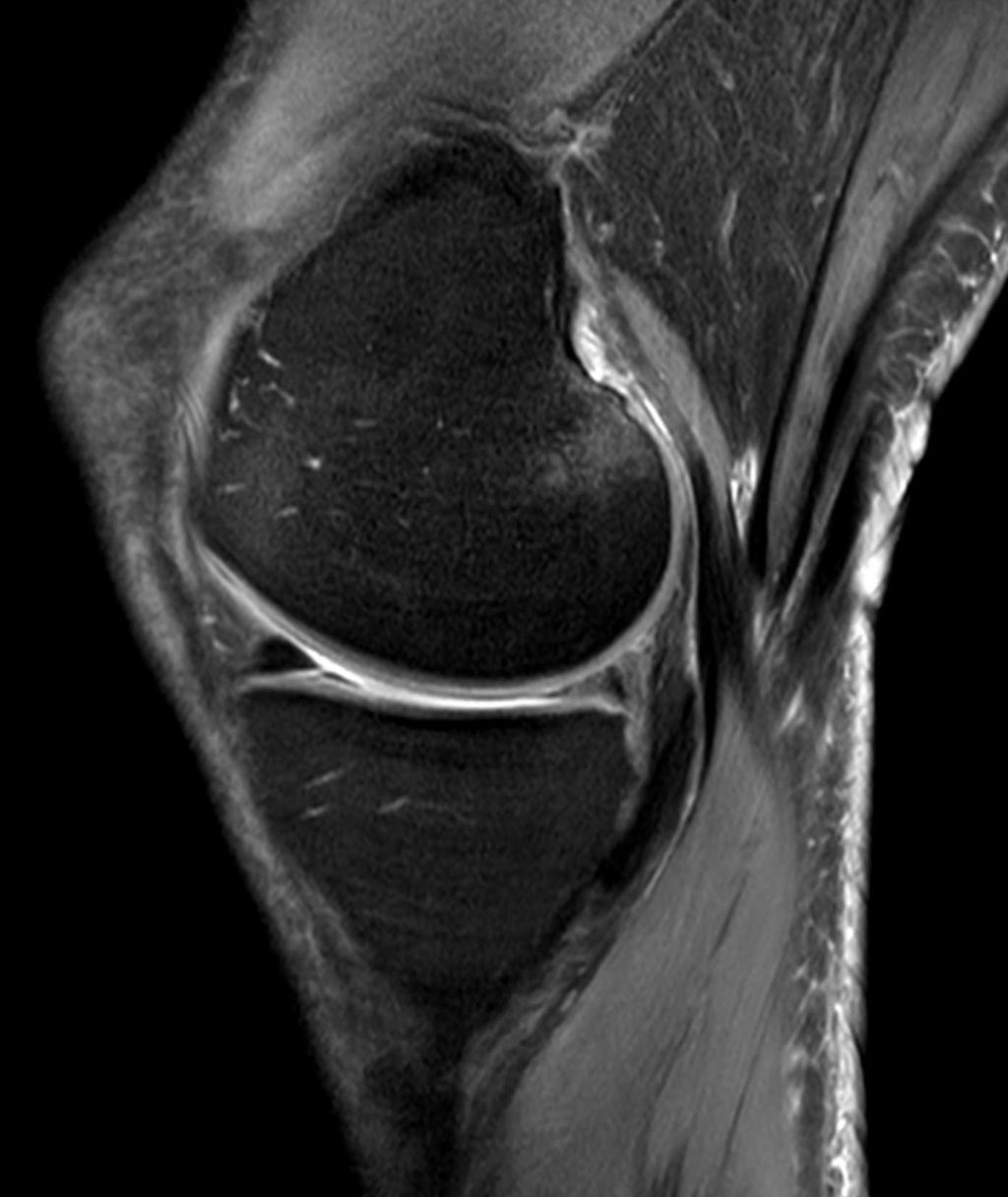
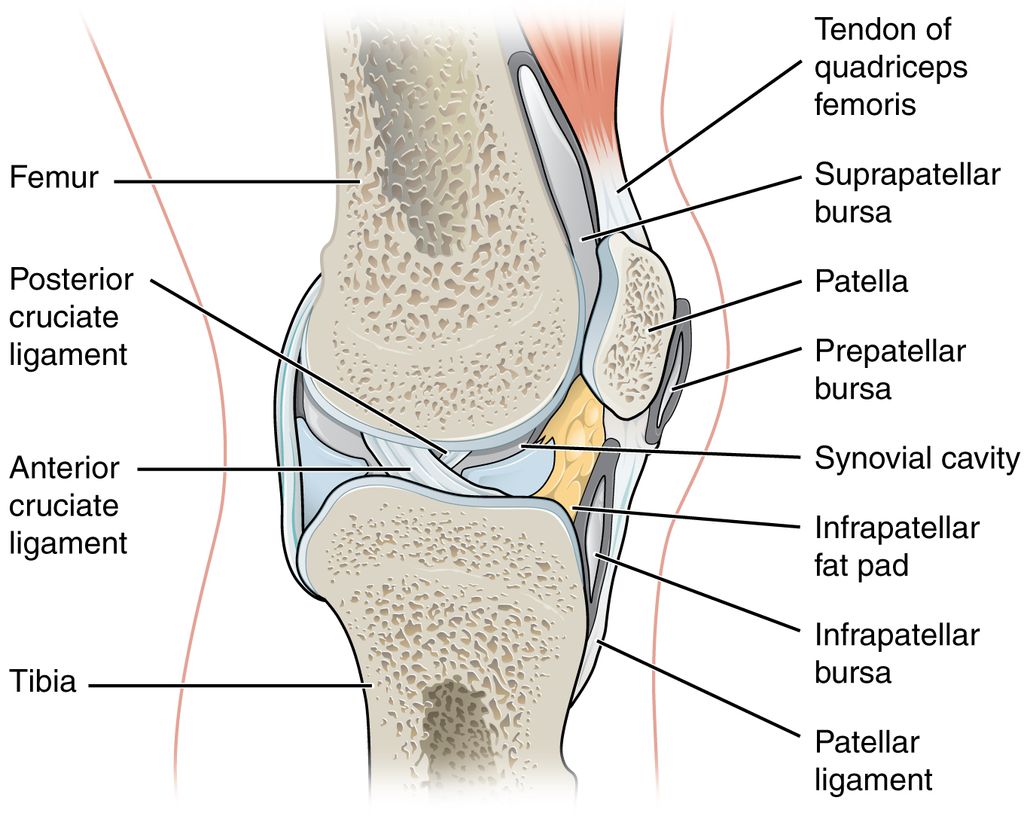
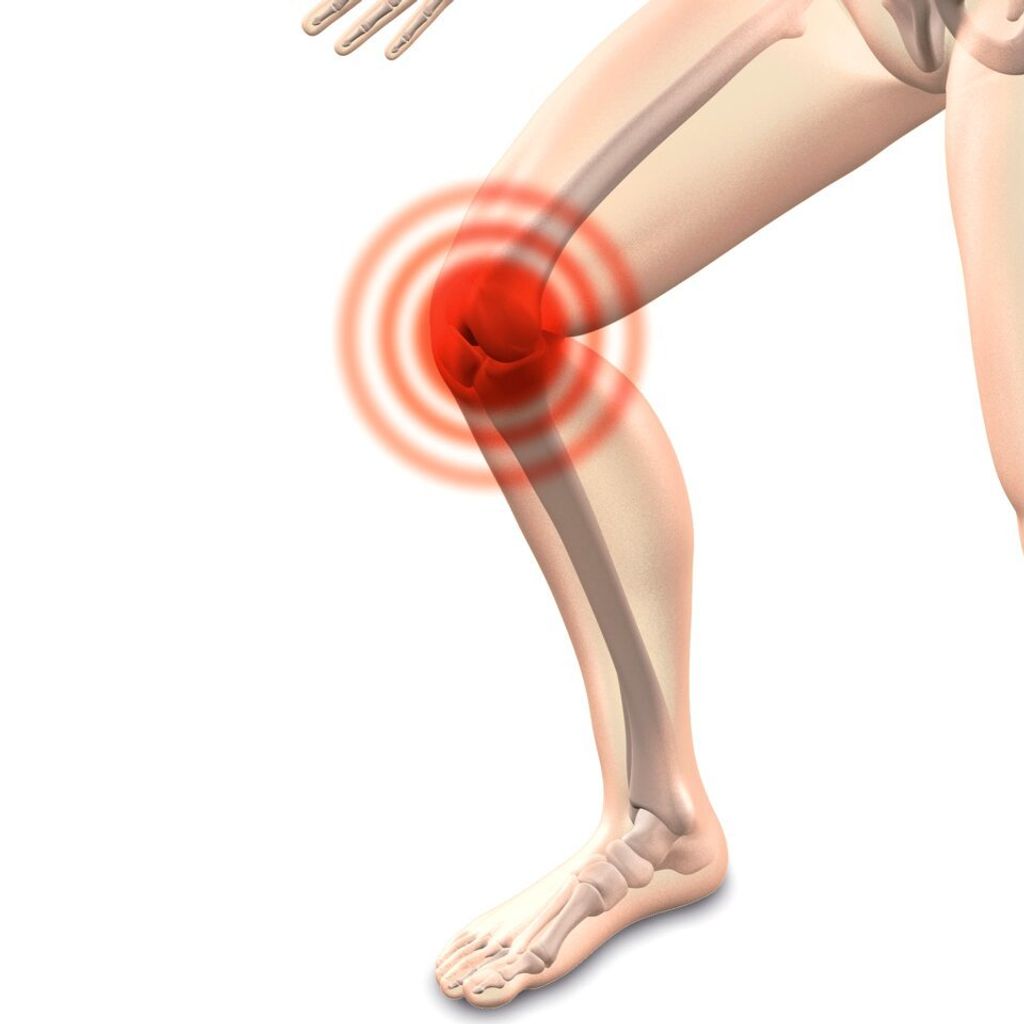
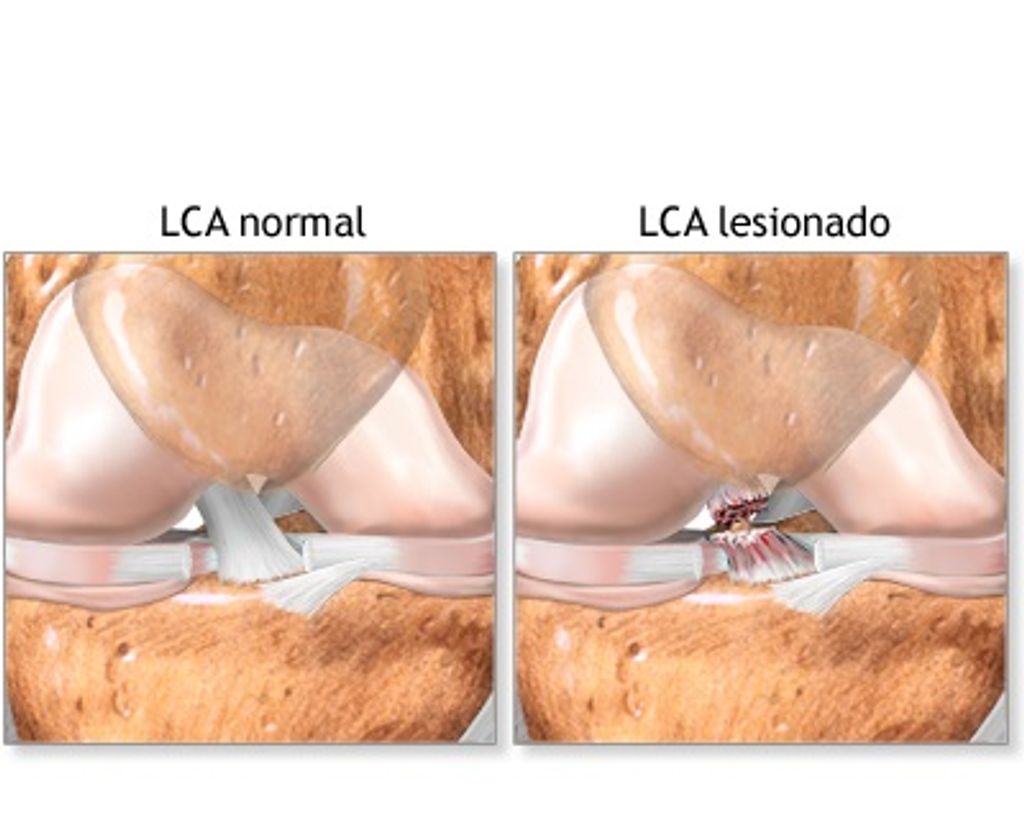
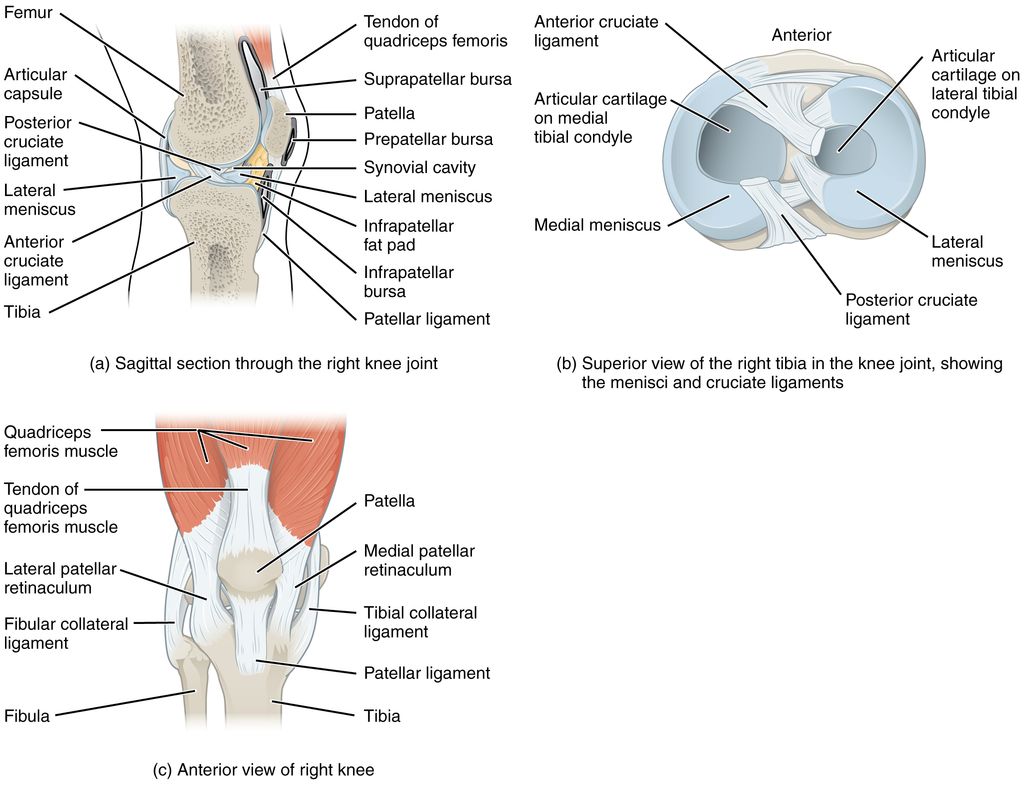
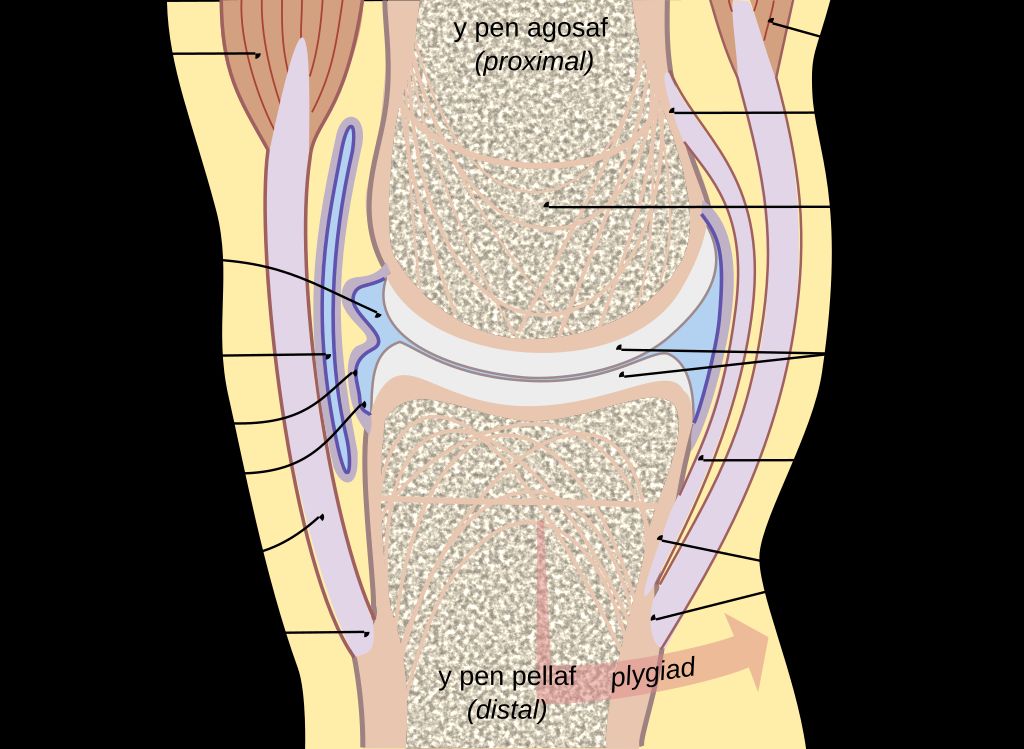
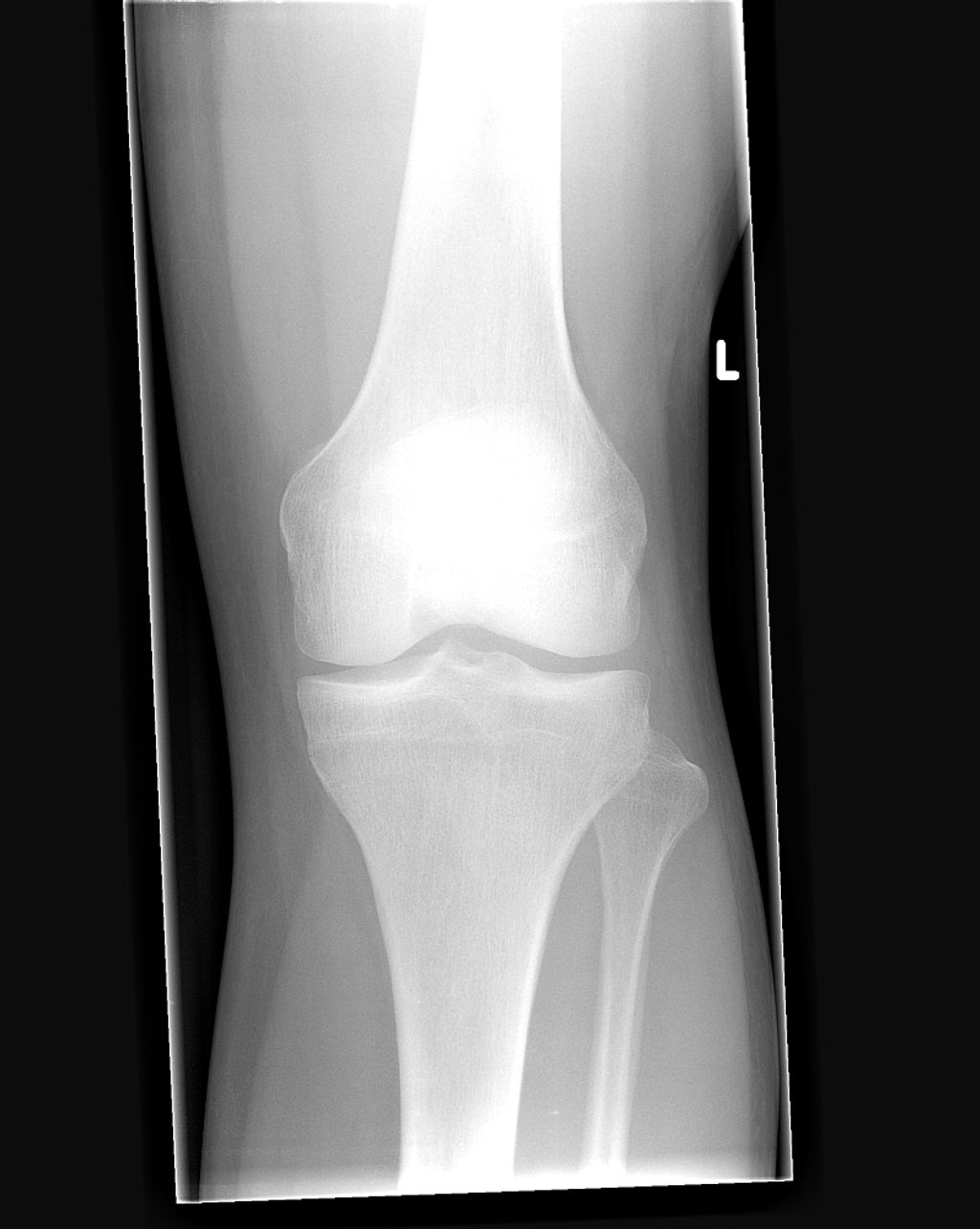
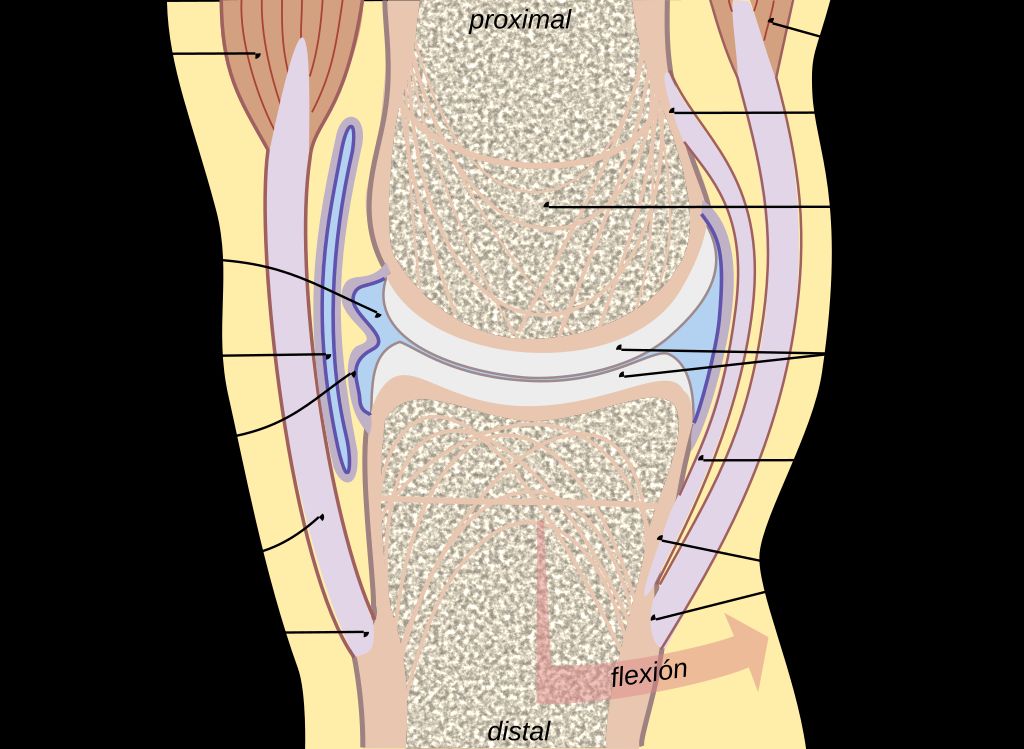
The Anatomy of the Knee Joint
Double knee replacement surgery, also known as bilateral knee arthroplasty, is a complex procedure that involves the replacement of both knee joints with artificial implants. This surgery is typically recommended for individuals who experience severe pain and limited mobility in both knees, often due to advanced osteoarthritis or other degenerative joint conditions. The decision to undergo double knee replacement surgery is carefully evaluated based on the patient’s overall health, lifestyle, and the extent of joint damage. It is important to consider the potential risks and benefits of this procedure before making a decision.
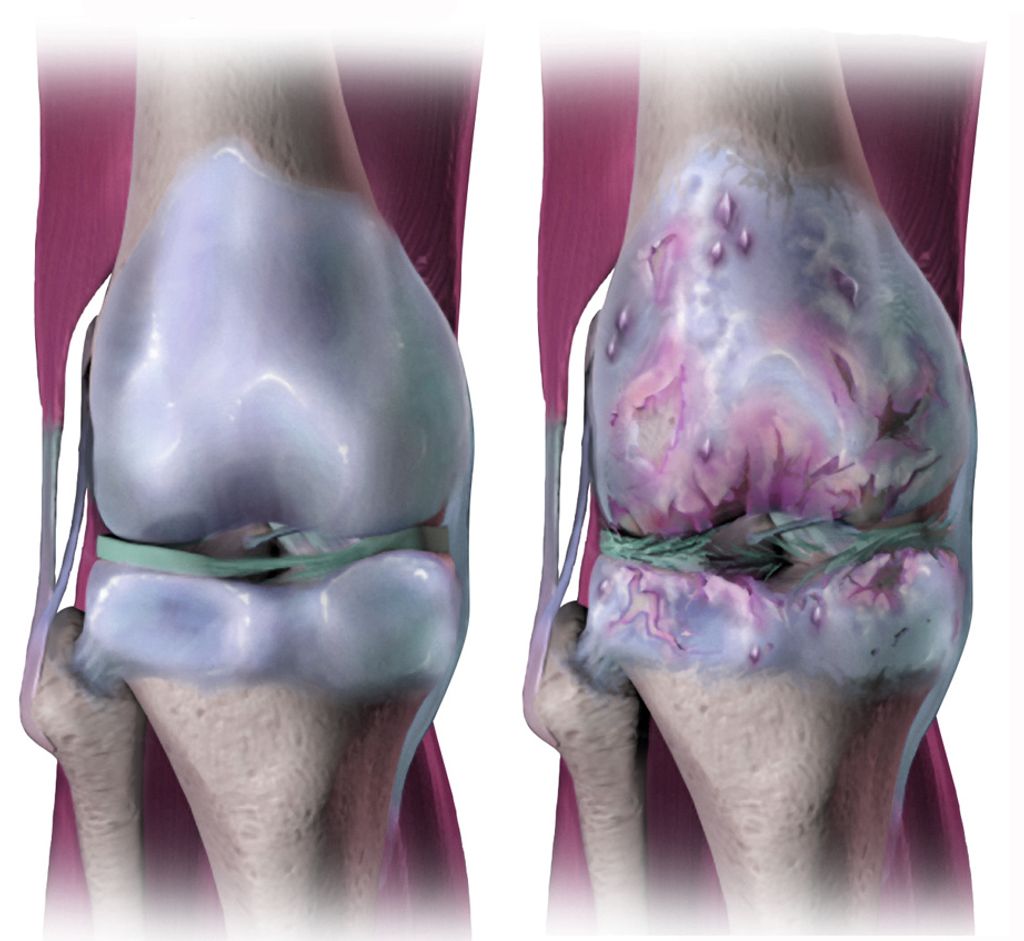
Indications for Double Knee Replacement Surgery
Double knee replacement surgery is indicated for severe osteoarthritis that affects both knees, leading to significant pain and limited mobility. It is also recommended for individuals who have not experienced relief from conservative treatments such as medication and physical therapy. In addition, patients with deformities in both knees that interfere with daily activities may be candidates for this procedure. Here are the common indications for double knee replacement surgery:
- Severe pain and stiffness in both knees
- Difficulty in performing routine activities
- Limited range of motion
- Failure of non-surgical treatments to provide relief
- Deformities in both knees
It is important to consult with a qualified orthopedic surgeon to determine if double knee replacement surgery is the most suitable option for your condition.
Risks and Complications
After undergoing double knee replacement surgery, we may experience some common risks and complications. These may include infection, blood clots, and implant loosening. It’s important to note that these risks are carefully managed by the medical team to ensure the best possible outcomes. Additionally, we will receive detailed guidance on postoperative care and rehabilitation to minimize these risks and promote a successful recovery.
In some cases, the risk of complications can be quantified. Here’s a brief overview of the potential risks:
| Complication | Risk Percentage |
|---|---|
| Infection | 1-2% |
| Blood Clots | 2-3% |
| Implant Loosening | 1-2% |
We should keep in mind that these percentages are general estimates and may vary based on individual health factors and surgical techniques. It’s essential to follow the postoperative care instructions provided by the medical team to minimize these risks and achieve a successful recovery.
We are encouraged to communicate any concerns or unusual symptoms to the healthcare professionals promptly. Early detection and intervention can significantly reduce the impact of potential complications and contribute to a positive outcome.
Recovery and Rehabilitation
After completing the recovery and rehabilitation process, we can expect significant improvements in mobility and function. Additionally, patients often experience a notable reduction in pain and an overall enhancement in quality of life. The long-term success rates of this procedure are quite promising, with a high percentage of patients reporting sustained benefits over time.
| Benefits | Outcomes |
|---|---|
| Improved mobility and function | Significant improvement |
| Pain relief and quality of life | Notable reduction in pain and enhanced quality of life |
| Long-term success rates | High percentage of sustained benefits |
It is important to maintain a consistent rehabilitation routine to maximize the benefits of the surgery and ensure long-term success.
The Surgical Procedure
Preoperative Preparation
After completing the preoperative preparation, we are ready to move forward with the surgical techniques. This involves the careful removal of damaged knee joint surfaces and the precise placement of the prosthetic components. The surgical team will work diligently to ensure the success of the procedure, aiming for optimal outcomes and minimal complications.
We understand the importance of this phase and are committed to providing the best care possible for our patients.
Surgical Techniques
Here is a brief overview of the surgical techniques involved in double knee replacement surgery:
| Technique | Description |
|---|---|
| Total Knee Replacement | Involves replacing the entire knee joint with prosthetic components to restore function. |
| Partial Knee Replacement | Targets only the damaged portion of the knee joint, preserving healthy tissue. |
We are dedicated to ensuring a smooth transition to the postoperative care phase, where we will continue to monitor and support our patients as they begin their journey towards recovery and rehabilitation.
Surgical Techniques
After the surgical techniques are completed, careful monitoring and postoperative care are crucial for a successful recovery. This involves regular check-ups, physical therapy sessions, and adherence to prescribed medications. Additionally, maintaining a healthy diet and following the recommended exercise regimen can significantly contribute to the overall outcome of the surgery. It’s important to note that each patient’s post-surgery recovery progress, setbacks, and strategies for overcoming setbacks may vary.
Postoperative Care
After the surgical procedure, careful monitoring and management of pain and inflammation are crucial for a successful recovery. Our team will provide personalized guidance on physical therapy exercises and assistive devices to support your rehabilitation journey. Additionally, a comprehensive plan for medication management and wound care will be tailored to your specific needs. It’s important to follow the prescribed postoperative care regimen to optimize your healing process and achieve the best possible outcomes.
Benefits and Outcomes
Improvement in Mobility and Function
Following double knee replacement surgery, we’ve observed a significant improvement in patients’ mobility and function. The ability to perform everyday activities with ease, which was once hindered by severe knee pain, is often restored. This enhanced mobility can profoundly impact one’s independence and overall well-being.
Patients typically experience:
- A noticeable reduction in joint stiffness
- Increased range of motion
- Improvement in walking gait
- Enhanced ability to climb stairs and rise from a seated position
It is crucial to adhere to a prescribed physical therapy regimen post-surgery to maximize improvements in mobility and function.
The journey to regain full function can vary from person to person, but the collective goal remains the same: to return to a more active and pain-free lifestyle. We encourage our patients to set incremental goals and celebrate each milestone achieved on the path to recovery.
Pain Relief and Quality of Life
Double knee replacement surgery offers significant improvements in pain relief and quality of life. Patients experience a reduction in chronic pain and an increase in overall comfort and mobility. Studies have shown that the procedure leads to enhanced physical function and a greater sense of well-being. Additionally, the surgery has been associated with improved mental health and emotional well-being, contributing to a more fulfilling and active lifestyle. These positive outcomes are supported by a high success rate and long-term patient satisfaction.
- Implement a table for presenting structured, quantitative data. Ensure it’s succinct and formatted correctly in Markdown.
- Use a bulleted or numbered list for less structured content, like steps, qualitative points, or a series of related items.
Long-Term Success Rates
After undergoing double knee replacement surgery, we can expect to experience a significant improvement in mobility and function. This includes the ability to engage in daily activities with greater ease and comfort. Additionally, we can anticipate substantial pain relief, leading to an overall enhancement in our quality of life. The long-term success rates of this procedure are promising, with a high percentage of patients reporting satisfaction and improved outcomes. For a detailed overview of the success rates, refer to the following table:
| Time Frame | Success Rate |
|---|---|
| 1 Year | 90% |
| 5 Years | 85% |
| 10 Years | 80% |
It is important to note that consistent follow-up care and adherence to postoperative guidelines are crucial for maximizing the benefits of double knee replacement surgery. We should prioritize regular check-ups and communicate any concerns with our healthcare professionals to ensure a successful recovery.
Conclusion
In conclusion, double knee replacement surgery offers a multitude of benefits for individuals suffering from severe knee joint issues. The procedure provides significant improvements in mobility, pain relief, and overall quality of life. With advancements in medical technology and surgical techniques, the success rates and recovery times for double knee replacement surgeries have continued to improve. As a result, patients can experience a more active and fulfilling lifestyle, free from the limitations imposed by debilitating knee conditions. The decision to undergo double knee replacement surgery should be carefully considered in consultation with medical professionals, taking into account individual health circumstances and long-term goals. Overall, the positive outcomes and enhanced well-being associated with double knee replacement surgery underscore its significance as a viable treatment option for those in need.
Frequently Asked Questions
What is the recovery time for double knee replacement surgery?
The recovery time for double knee replacement surgery varies for each individual, but most patients can expect to regain mobility and function within a few weeks to a few months after surgery.
Are both knees replaced at the same time during double knee replacement surgery?
Yes, in double knee replacement surgery, both knees are typically replaced in the same surgical procedure.
What are the potential risks of double knee replacement surgery?
Some potential risks of double knee replacement surgery include infection, blood clots, implant failure, and nerve damage. However, these risks are minimized with proper preoperative evaluation and postoperative care.
How long do the benefits of double knee replacement surgery last?
The benefits of double knee replacement surgery can last for many years, with most patients experiencing long-term improvement in mobility, function, and pain relief.
What is the success rate of double knee replacement surgery?
The success rate of double knee replacement surgery is generally high, with the majority of patients experiencing significant improvement in quality of life and functionality after surgery.
What activities can I engage in after double knee replacement surgery?
After double knee replacement surgery, patients can engage in low-impact activities such as walking, swimming, and cycling. However, high-impact activities and sports that place excessive stress on the knees should be avoided to protect the longevity of the implants.