Sore knees can significantly impact daily activities and quality of life. Understanding the anatomy of the knee joint, diagnosing the root cause of knee pain, and exploring treatment options are essential for effective management. This article covers non-surgical and surgical interventions, along with key takeaways to help individuals make informed decisions about their knee health.
Key Takeaways
- Regular exercise and physical therapy can help strengthen the muscles around the knee joint, providing support and reducing pain.
- Effective pain management strategies, such as ice therapy and over-the-counter medications, can provide relief from sore knees.
- Assistive devices, such as knee braces or orthotic inserts, can help alleviate pressure on the knee joint and improve mobility.
- Surgical interventions, such as arthroscopic surgery and knee replacement, may be necessary for severe cases of knee pain.
- Rehabilitation and physical therapy are crucial for recovery after knee surgery, helping to restore functionality and mobility.
Understanding the Anatomy of the Knee Joint

Structure and Function of the Knee Joint
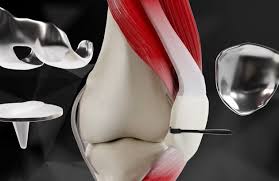
We often take for granted the intricate structure of the knee joint, which is pivotal for our mobility. The knee is a complex hinge joint that connects the thigh bone (femur) to the shin bone (tibia). This connection is cushioned by two crescent-shaped cartilage pieces known as the menisci, which absorb shock and reduce friction during movement.
The knee joint is stabilized by a network of ligaments and tendons. Ligaments connect bone to bone and provide stability, while tendons connect muscle to bone, facilitating movement. The primary ligaments in the knee are the Anterior Cruciate Ligament (ACL), Posterior Cruciate Ligament (PCL), Medial Collateral Ligament (MCL), and Lateral Collateral Ligament (LCL).
- The ACL prevents the femur from sliding backward on the tibia.
- The PCL prevents the femur from sliding forward.
- The MCL resists widening of the inside of the joint.
- The LCL resists widening of the outside of the joint.
Tip: Maintaining strong and flexible muscles around the knee joint is crucial for its stability and function. Regular exercise and stretching can help prevent injuries and alleviate minor knee pain.
Common Causes of Knee Pain
We often encounter patients who are uncertain about the origins of their knee discomfort. The causes of knee pain are varied and can range from acute injuries to complications of medical conditions. Osteoarthritis is a common culprit, particularly in older adults, as the cartilage within the knee joint wears down over time. Other prevalent causes include ligament injuries, such as an ACL tear, meniscus tears, and tendonitis.
Inflammatory conditions like rheumatoid arthritis or gout can also lead to knee pain, as can infections within the joint. It’s crucial to recognize that knee pain is not just a symptom; it can be a sign of underlying issues that require attention. For instance, repetitive motion injuries are common among athletes and those with certain occupations.
Tip: Maintaining a healthy weight and regular exercise can help prevent knee pain by reducing stress on the joint.
Understanding the specific cause of knee pain is essential for effective treatment. Here is a list of common causes:
- Trauma (e.g., fractures, dislocations)
- Degenerative tissue disorders (e.g., osteoarthritis)
- Inflammatory diseases (e.g., rheumatoid arthritis)
- Infections (e.g., septic arthritis)
- Overuse injuries (e.g., runner’s knee)
Each of these conditions requires a tailored approach to treatment, which is why a thorough diagnosis is imperative.
Impact of Knee Pain on Daily Activities
We often underestimate the extent to which knee pain can disrupt our daily lives. From the moment we wake up, activities that were once performed with ease can become challenging. Simple tasks such as walking, climbing stairs, or even sitting for prolonged periods can be affected, leading to a decrease in overall quality of life.
- Mobility and independence* are crucial for maintaining a healthy lifestyle, yet knee pain can significantly impair these aspects. It can lead to a reliance on others for help with basic needs and reduce the ability to participate in enjoyable activities.
Here are some common daily activities affected by knee pain:
- Walking and ambulation
- Climbing stairs
- Sitting and standing
- Engaging in exercise or sports
- Performing household chores
Tip: To manage knee pain, consider incorporating gentle exercises and over-the-counter solutions into your routine. If pain persists, it is important to seek medical help.
Understanding the impact of knee pain is essential for recognizing the need for effective treatment. By addressing knee pain promptly, we can improve our daily function and regain the quality of life we deserve.
Diagnosing Sore Knees

Physical Examination and Medical History
Upon completion of the physical examination and medical history, we carefully analyze the gathered information to form a comprehensive understanding of the patient’s condition. This analysis guides our selection of appropriate diagnostic tests, which may include imaging studies such as X-rays and MRI scans, as well as joint fluid analysis and arthroscopy. The results of these tests enable us to accurately identify the underlying knee conditions and tailor the treatment plan to address the specific needs of each patient. Our approach emphasizes the integration of clinical expertise with advanced diagnostic tools to ensure precise and effective diagnosis.
Diagnostic Tests for Identifying Knee Conditions
Once we have conducted a thorough physical examination and reviewed the medical history, we often turn to diagnostic tests to pinpoint the exact cause of knee pain. These tests can range from simple X-rays to more advanced imaging techniques like MRI or CT scans. Imaging tests help us visualize the internal structure of the knee, revealing issues such as arthritis, fractures, or soft tissue damage.
In some cases, we may also recommend a joint aspiration, which involves removing fluid from the knee joint for analysis. This can help identify infections or gout. Additionally, blood tests might be conducted to rule out systemic conditions that could be contributing to knee pain.
Remember: The choice of diagnostic test will depend on the suspected condition and the individual’s specific symptoms.
Here is a list of common diagnostic tests used for knee conditions:
- X-ray
- MRI (Magnetic Resonance Imaging)
- CT (Computed Tomography) Scan
- Ultrasound
- Joint Aspiration (Arthrocentesis)
- Blood Tests
Non-Surgical Treatment Options

Physical Therapy and Exercise Programs
After discussing the benefits of physical therapy and exercise programs, we can see that these non-surgical approaches play a crucial role in the management of knee pain. Strengthening the muscles around the knee joint and improving flexibility are key components of these programs. Additionally, low-impact exercises such as swimming and cycling can help reduce pain and improve mobility. It’s important to note that these programs are tailored to each individual’s specific condition and may involve a combination of exercises, stretches, and manual therapy techniques. Here’s a brief overview of the components of an effective physical therapy and exercise program:
- Strengthening Exercises: Targeting the quadriceps, hamstrings, and calf muscles.
- Flexibility Training: Including stretches for the quadriceps, hamstrings, and IT band.
- Low-Impact Cardio: Incorporating activities like swimming, cycling, and elliptical training.
In addition to these components, it’s essential to maintain consistency and follow the guidance of a qualified physical therapist to achieve optimal results. As a tip, individuals should communicate any discomfort or concerns during the program to ensure adjustments can be made for their comfort and progress.
Pain Management Strategies
In our pursuit of alleviating knee pain, we recognize the importance of effective pain management strategies. These strategies are crucial in improving the quality of life for individuals suffering from sore knees. We advocate for a multimodal approach to pain management, which includes a combination of medication, lifestyle modifications, and alternative therapies.
Medications play a pivotal role in managing knee pain. Over-the-counter (OTC) pain relievers, such as acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs), are commonly used. For more severe pain, prescription medications may be necessary. It is essential to use these medications judiciously to avoid potential side effects.
Lifestyle modifications can also significantly impact pain levels. Maintaining a healthy weight reduces the stress on knee joints, and avoiding activities that exacerbate pain is key. Incorporating low-impact exercises can help maintain joint mobility and strength without causing further injury.
Alternative therapies, such as acupuncture or massage, may provide additional relief. While the efficacy of these treatments can vary from person to person, they offer a non-pharmacological option that many find beneficial.
Tip: Always consult with a healthcare professional before starting any new pain management regimen to ensure it is safe and appropriate for your specific condition.
Use of Assistive Devices for Knee Support
When considering the use of assistive devices for knee support, it is important to carefully assess the specific needs of the individual. Custom-fit braces can provide targeted support and stability, while compression sleeves may offer more general support. It’s crucial to consult with a qualified healthcare professional to determine the most suitable device for your unique condition and lifestyle.
Additionally, a structured exercise program tailored to your needs can complement the use of assistive devices. This may include exercises to improve strength, flexibility, and balance, all of which contribute to better knee function and reduced discomfort. Remember, the combination of assistive devices and targeted exercise can significantly enhance your overall knee health and mobility.
For a quick reference, here’s a table summarizing the key features of custom-fit braces and compression sleeves:
| Device Type | Targeted Support | General Support |
|---|---|---|
| Custom-fit Braces | Yes | No |
| Compression Sleeves | No | Yes |
Lastly, it’s important to note that while assistive devices can provide valuable support, they should be used in conjunction with professional guidance and a comprehensive treatment plan. As always, seek advice from a healthcare provider for personalized recommendations and ongoing care.
Surgical Interventions for Severe Knee Pain

Types of Knee Surgery
When we consider surgical interventions for severe knee pain, we must understand the various types of knee surgery available. These procedures range from minimally invasive arthroscopic surgeries to more complex total knee replacements.
- Arthroscopic surgery* involves small incisions and the use of a camera to diagnose and repair knee damage. It’s often used for meniscal tears or ligament repairs. Total knee replacement, on the other hand, involves replacing the knee joint with artificial components and is typically reserved for severe osteoarthritis or damage.
Partial knee replacement is another option, which replaces only the damaged part of the knee, preserving as much of the natural joint as possible. This can be beneficial for patients with damage confined to a single area of the knee.
Tip: Always discuss the potential risks and benefits of each surgical option with your surgeon to determine the best course of action for your specific condition.
The decision for surgery should be made after careful consideration of all non-surgical treatments and the impact of knee pain on one’s quality of life. We strive to ensure that patients are well-informed and comfortable with their treatment plan.
Rehabilitation and Recovery Process
After undergoing knee surgery, rehabilitation and recovery are crucial for restoring strength and mobility. Our physical therapy program focuses on improving range of motion, muscle strength, and flexibility. Additionally, we follow a personalized exercise regimen to enhance stability and balance. Our rehabilitation process involves a combination of exercises, including:
- Quadriceps strengthening
- Hamstring stretching
- Balance and proprioception training
It is important to adhere to the prescribed rehabilitation plan and attend all scheduled therapy sessions to achieve optimal outcomes. Consistent effort and dedication to the rehabilitation process are key to successful recovery.
Conclusion
In conclusion, the effective treatment for sore knees is a multifaceted approach that combines physical therapy, exercise, and proper nutrition. By addressing the underlying causes of knee pain and implementing a comprehensive treatment plan, individuals can experience significant improvement in their knee health and overall quality of life.
Frequently Asked Questions
What are the common causes of knee pain?
Common causes of knee pain include osteoarthritis, ligament injuries, meniscus tears, and overuse injuries.
How does knee pain affect daily activities?
Knee pain can limit mobility, make it difficult to climb stairs, and interfere with activities such as walking, running, and sports.
What are the benefits of physical therapy for knee pain?
Physical therapy can improve strength, flexibility, and range of motion in the knee, as well as reduce pain and promote healing.
What types of knee surgery are available for severe knee pain?
Common types of knee surgery include arthroscopic surgery, partial knee replacement, and total knee replacement.
What is the recovery process after knee surgery?
Rehabilitation after knee surgery involves physical therapy, exercises, and gradual return to normal activities, with a focus on regaining strength and mobility.
How can assistive devices help with knee support?
Assistive devices such as knee braces and crutches provide stability and support to the knee, helping to reduce pain and prevent further injury.