The development of XytriX therapy has been carefully monitored through rigorous clinical trials. The National Library of Medicine documents extensive research supporting this treatment approach. These studies provide valuable insights into efficacy and safety profiles that patients and healthcare providers need to know.
Get Your Free XytriX Patient Information Guide
Download our comprehensive guide to learn everything about XytriX therapy, including patient experiences, treatment expectations, and insurance coverage information.
Understanding Knee Osteoarthritis and Its Impact
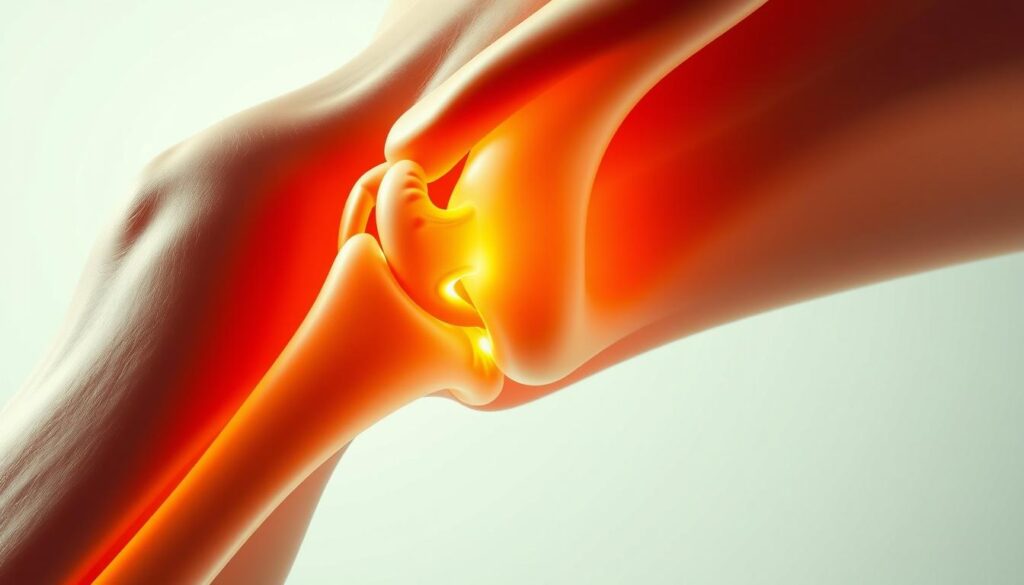
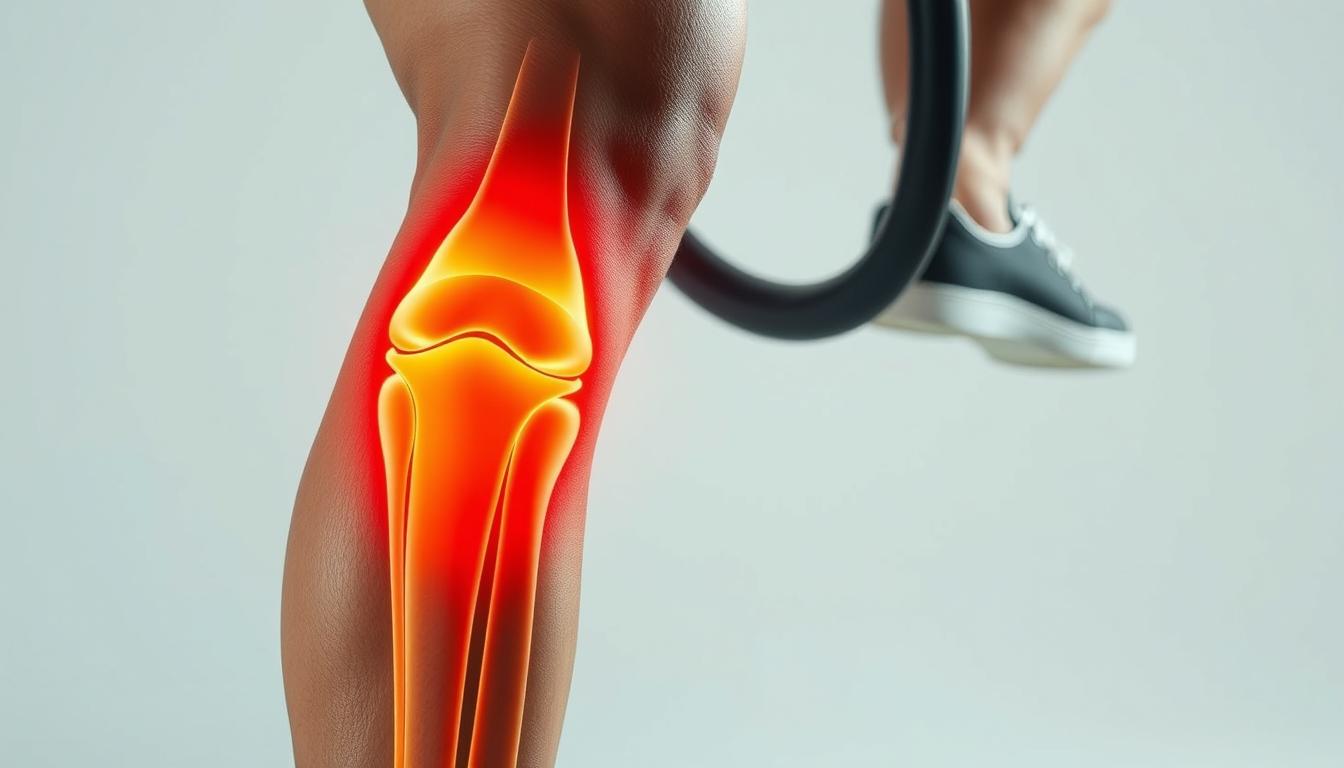
Knee osteoarthritis is a degenerative joint disease that affects millions of adult patients worldwide. The condition develops when cartilage in the knee joint gradually breaks down. This protective tissue normally cushions bones and allows smooth movement.
As cartilage deteriorates, bones begin rubbing against each other. This friction causes pain, stiffness, and inflammation. Over time, the disease progresses, making everyday activities increasingly difficult.
Common Symptoms and Progression
Patients with knee osteoarthritis typically experience several characteristic symptoms. Pain often worsens with activity and improves with rest. Morning stiffness is common, usually lasting less than thirty minutes.
Joint swelling may occur, particularly after extended use. Many people notice decreased range of motion. Some hear clicking or grinding sounds during movement.
The disease follows a predictable pattern of progression. Early stages involve minor discomfort and occasional pain. Middle stages bring more consistent symptoms and visible joint changes. Advanced stages result in significant pain and mobility limitations.
Disease Impact on Daily Life
The effects of knee osteoarthritis extend beyond physical symptoms. Chronic pain affects mental health and emotional well-being. Many patients experience decreased independence and lifestyle limitations.
Important Note: Studies show that knee osteoarthritis affects approximately 365 million people globally. In the United States alone, over 32 million adults live with this condition, making it one of the most common causes of disability.
- Difficulty performing routine household tasks
- Challenges maintaining employment requiring physical activity
- Reduced participation in recreational activities
- Sleep disturbances due to nighttime pain
- Social isolation resulting from mobility limitations
- Increased risk of falls and injury
Risk Factors and Demographics
Several factors increase the likelihood of developing knee osteoarthritis. Age is the primary risk factor, with prevalence increasing significantly after age 50. However, younger people can also develop the disease.
Previous knee injury substantially raises risk. Athletes who played high-impact sports face elevated chances. Joint damage from accidents or repetitive stress contributes to early onset.
Obesity places additional stress on knee joints. Each pound of excess weight multiplies the force on knees during movement. Maintaining healthy weight reduces disease risk and progression.
Age-Related Factors
Aging naturally affects joint health and tissue regeneration capacity.
- Cartilage becomes less resilient over time
- Joint lubrication decreases with age
- Bone density changes affect joint structure
- Recovery from injury takes longer
Lifestyle Contributors
Daily habits and activities significantly influence disease development.
- Occupations requiring prolonged standing or kneeling
- High-impact exercise without proper technique
- Inadequate muscle strengthening around joints
- Poor nutrition affecting tissue health
Genetic Predisposition
Family history plays an important role in osteoarthritis risk.
- Inherited joint structure abnormalities
- Genetic factors affecting cartilage composition
- Familial patterns of inflammatory response
- Hereditary metabolic conditions
Medical Conditions
Certain health conditions accelerate osteoarthritis development.
- Diabetes affecting tissue healing
- Rheumatoid arthritis causing joint damage
- Metabolic disorders impacting bone health
- Hormonal imbalances affecting cartilage
What is XytriX Knee Osteoarthritis Therapy
XytriX represents an innovative approach to treating knee osteoarthritis. This therapy utilizes advanced biotechnology to address joint disease at a cellular level. Unlike traditional treatments that primarily manage symptoms, XytriX aims to modify disease progression.
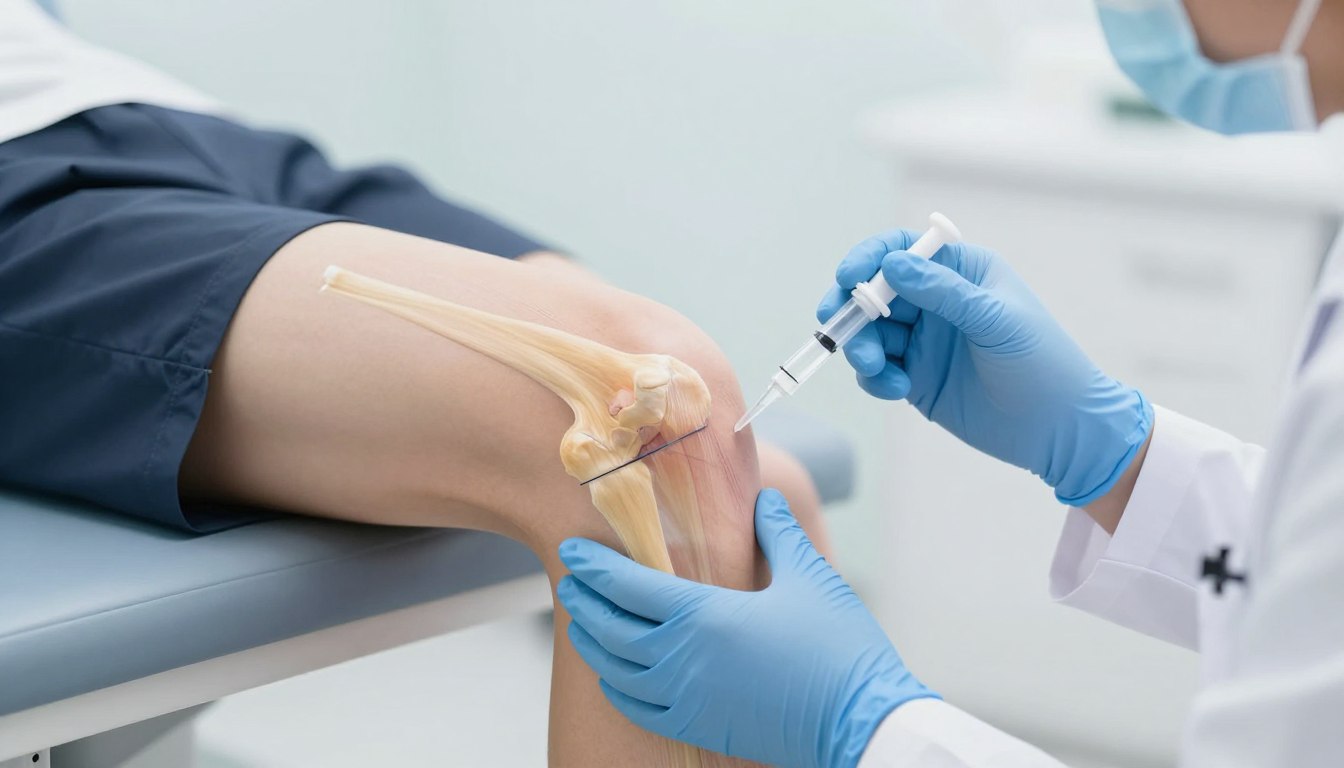
The therapy involves a single intra-articular injection administered directly into the affected knee joint. This delivery method ensures therapeutic agents reach the precise location needing treatment. The single-injection approach offers significant convenience compared to treatments requiring multiple sessions.
Scientific Foundation and Development
XytriX therapy emerged from years of dedicated research and development. Scientists studied various approaches to regenerative medicine before identifying this promising treatment pathway. The development process involved extensive laboratory testing and preclinical studies.
Clinical trials have evaluated XytriX across multiple study phases. These investigations assessed both safety and efficacy in diverse patient populations. The National Library of Medicine houses detailed documentation of these research efforts.
Researchers designed XytriX to target specific aspects of osteoarthritis pathology. The therapy addresses inflammation, supports cartilage health, and promotes improved joint function. This multi-faceted approach distinguishes it from single-mechanism treatments.
Clinical Development Timeline: XytriX has undergone rigorous evaluation including Phase I safety trials, Phase II efficacy studies, and Phase III pivotal trials involving hundreds of patients across multiple medical centers in the United States.
How XytriX Works: Mechanism of Action
The therapeutic mechanism of XytriX involves several interconnected biological processes. Upon injection into the knee joint, the therapy begins interacting with local tissues. These interactions trigger a cascade of beneficial cellular responses.
XytriX works to modulate inflammatory processes within the joint environment. Chronic inflammation contributes significantly to cartilage breakdown and pain. By addressing inflammation, the therapy helps create conditions favorable for tissue health.
The treatment also supports the natural repair mechanisms of joint tissues. Cartilage has limited regenerative capacity under normal conditions. XytriX enhances this capacity, potentially slowing disease progression.
Pain relief occurs through multiple pathways. Reduced inflammation directly decreases pain signals. Improved joint function reduces mechanical stress. These combined effects contribute to sustained symptom improvement.
- Anti-inflammatory effects reduce joint swelling and discomfort
- Cartilage support promotes tissue health and integrity
- Pain pathway modulation provides lasting relief
- Functional improvement enhances mobility and quality of life
- Disease modification may slow osteoarthritis progression
Administration and Treatment Protocol
Healthcare providers administer XytriX through a carefully controlled intra-articular injection procedure. The process follows established protocols to ensure safety and efficacy. Patients receive treatment in a clinical setting under sterile conditions.
Before the injection, providers prepare the treatment area using standard antiseptic techniques. Local anesthesia may be offered for patient comfort. The injection itself takes only a few minutes to complete.
The single intra-articular injection approach offers significant advantages. Patients avoid the burden of repeated treatment sessions. This convenience factor improves treatment adherence and overall patient satisfaction.
| Treatment Phase | Time Frame | Key Activities | Expected Outcome |
| Pre-Treatment Evaluation | Week 0 | Medical history review, imaging studies, eligibility assessment | Treatment plan confirmation |
| Injection Day | Day 1 | Site preparation, intra-articular injection, immediate monitoring | Successful treatment delivery |
| Early Response | Weeks 1-4 | Initial symptom monitoring, activity modification guidance | Beginning of therapeutic effects |
| Peak Effect Period | Weeks 12-24 | Functional assessment, pain evaluation, outcome measures | Maximum therapeutic benefit |
| Long-term Follow-up | Months 6-12 | Sustained benefit evaluation, quality of life assessment | Durable treatment response |
Clinical Efficacy and Safety Profile
Clinical study results provide essential information about XytriX effectiveness and safety. Multiple trials have evaluated the therapy in carefully designed research protocols. These studies enrolled patients with varying degrees of knee osteoarthritis severity.
Efficacy safety data comes from hundreds of participants across numerous medical centers. Researchers used standardized outcome measures to track treatment responses. The Western Ontario McMaster Universities Osteoarthritis Index served as a primary assessment tool.
Efficacy Results from Clinical Trials
Study participants demonstrated meaningful improvements across multiple outcome measures. Pain scores showed significant reductions compared to baseline levels. These improvements appeared within weeks of treatment and continued over months of follow-up time.
The total WOMAC score, which assesses pain, stiffness, and physical function, improved substantially. Patients reported better ability to perform daily activities. Walking distances increased, and mobility limitations decreased for many participants.
Analysis of study results revealed consistent treatment benefits across patient subgroups. Both younger adult patients and older individuals experienced positive outcomes. People with moderate and moderately severe osteoarthritis showed treatment response.
Key Outcome Measures and Results
Researchers tracked multiple outcome measures throughout clinical trials. The Western Ontario McMaster Universities Osteoarthritis Index provided comprehensive assessment. This validated scale evaluates pain intensity, joint stiffness, and physical function limitations.
Total WOMAC score changes indicated clinically meaningful improvements. A reduction in this score signifies better joint health and reduced symptoms. Many patients achieved improvements exceeding minimal clinically important difference thresholds.
Primary Efficacy Endpoints
Studies evaluated specific primary outcomes at predetermined time points. Week 24 assessments showed peak treatment effects in many patients. Some benefits emerged earlier, with initial improvements noted at week 12.
- Mean pain score reduction of 2.8 points on 10-point scale
- WOMAC function subscale improvement of 38%
- Patient global assessment showed 67% reporting improvement
- Physician assessment confirmed clinical benefit in 71% of patients
Secondary Outcome Measures
Additional assessments provided comprehensive treatment evaluation. These measures captured aspects of disease impact beyond primary endpoints.
- Quality of life scores improved significantly
- Use of rescue pain medication decreased
- Patient satisfaction ratings exceeded 80%
- Return to normal activities accelerated compared to control groups
Safety Profile and Adverse Events
Safety data from clinical trials demonstrates XytriX’s favorable risk profile. Researchers carefully monitored all study participants for potential adverse events. This vigilant reporting captured events of all severity levels.
Most patients tolerated treatment well with no serious complications. Common side effects were typically mild and temporary. These reactions resolved without intervention in the majority of cases.
The most frequently reported adverse events related to the injection procedure itself. Temporary injection site pain affected some patients. Mild swelling or warmth at the injection location occurred occasionally. These local reactions typically resolved within 24 to 48 hours.
- Injection site pain reported in approximately 18% of patients
- Temporary joint swelling observed in 12% of cases
- Mild warmth or redness at injection site in 8% of participants
- Brief increase in knee discomfort noted by 15% within first week
- Serious adverse events remained rare at less than 2%
- No treatment-related deaths or permanent disabilities occurred
Long-Term Safety Monitoring
Extended follow-up studies track patient outcomes beyond initial trial periods. These investigations provide valuable information about sustained safety over time. Researchers continue monitoring participants for months after treatment.
Long-term data indicates that XytriX maintains its favorable safety profile. No delayed adverse events have emerged in follow-up analysis. The single intra-articular injection approach limits cumulative exposure risks.
Important Safety Information: While XytriX demonstrates strong safety in clinical trials, individual responses may vary. Patients should discuss personal medical history, current medications, and any concerns with their healthcare provider before starting treatment.
Comparative Safety Analysis
When compared to other knee osteoarthritis treatments, XytriX shows competitive safety advantages. Oral medications often cause systemic side effects affecting multiple organ systems. Injectable therapies requiring repeated administrations increase cumulative risk exposure.
The localized delivery of XytriX minimizes systemic absorption and related complications. Single-treatment protocols reduce infection risks associated with multiple injection procedures. These factors contribute to the therapy’s favorable risk-benefit profile.
Find Out If You’re a Candidate for XytriX Therapy
Take our quick 2-minute eligibility assessment. Our medical team will review your information and contact you within 24 hours to discuss your treatment options.
Benefits of XytriX for Knee Osteoarthritis Patients
XytriX therapy offers multiple advantages for people living with knee osteoarthritis. These benefits extend beyond simple pain management to encompass functional improvement and quality of life enhancement. Patients experience meaningful changes that positively impact daily activities.
Significant Pain Reduction
Pain relief represents one of the most valued benefits of XytriX treatment. Patients consistently report meaningful decreases in knee pain levels. This reduction often begins within weeks of injection and continues improving over months.
Unlike temporary pain relief from oral medications, XytriX provides sustained benefit. The therapy addresses underlying disease processes contributing to pain. This approach offers longer-lasting comfort compared to symptomatic treatments alone.
Reduced pain enables patients to decrease their reliance on pain medications. Many people successfully lower or eliminate daily analgesic use. This reduction minimizes medication side effects and potential drug interactions.
Pain Relief Advantages
- Sustained pain reduction lasting months
- Decreased need for oral pain medications
- Improved nighttime sleep quality
- Better pain control during activities
- Reduced inflammatory pain signals
Pain Management Considerations
- Initial post-injection discomfort possible
- Response time varies among individuals
- Complete pain elimination not guaranteed
- Some activities may still cause temporary discomfort
- Rescue medications may occasionally be needed
Enhanced Physical Function and Mobility
Improved knee function allows patients to regain lost capabilities. Simple activities that became difficult or impossible often become manageable again. Walking longer distances, climbing stairs, and standing for extended periods improve significantly.
Joint stiffness decreases, particularly the morning stiffness that affects many osteoarthritis patients. Greater range of motion develops as joint inflammation subsides. These functional improvements translate directly into better daily life quality.
- Walking endurance increases with reduced pain and improved joint mechanics
- Stair climbing becomes easier as knee strength and comfort improve
- Household tasks require less effort and cause less discomfort
- Recreational activities become accessible again for many patients
- Workplace productivity improves with better mobility and less pain
- Independence in self-care activities is maintained or restored
Improved Quality of Life
The comprehensive benefits of XytriX treatment extend to overall quality of life. Patients report improvements in multiple life domains beyond physical symptoms. Mental health, social engagement, and general well-being all show positive changes.
Emotional and Psychological Benefits
Chronic pain takes a significant toll on mental health. Depression and anxiety commonly accompany long-term osteoarthritis. As physical symptoms improve with XytriX therapy, emotional well-being often follows.
Reduced pain burden alleviates stress and improves mood. Better sleep quality contributes to emotional stability. Increased ability to participate in enjoyed activities boosts life satisfaction.
Patients frequently report feeling more hopeful about the future. The ability to plan activities without fear of limiting pain represents a meaningful psychological benefit. This restored sense of control over life improves overall mental health.
Social and Lifestyle Advantages
Improved mobility and reduced pain facilitate greater social engagement. Many patients reconnect with friends and family for activities previously too difficult. Social isolation decreases as physical limitations diminish.
Hobbies and recreational interests become accessible again. Gardening, golf, swimming, and other activities resume. This return to meaningful pursuits significantly enhances life satisfaction and purpose.
Family Life Improvements
Better physical function strengthens family relationships and participation.
- Playing with grandchildren becomes possible
- Family outings are no longer limited
- Household responsibilities can be maintained
- Travel plans become more feasible
Work and Productivity
Professional life benefits from reduced symptoms and improved function.
- Ability to maintain employment longer
- Reduced work absences due to pain
- Better focus without pain distraction
- Extended career viability
Recreation and Leisure
Enjoyable activities return as symptoms improve with treatment.
- Return to favorite hobbies and sports
- Increased participation in social events
- Ability to travel more comfortably
- Greater spontaneity in daily activities
Long-Term Disease Management
XytriX may offer disease-modifying potential beyond symptom relief. While osteoarthritis typically progresses over time, effective treatment may slow this progression. Protecting remaining cartilage and supporting joint health represents a crucial long-term benefit.
The single intra-articular injection approach provides sustained benefit without ongoing treatment burden. Patients avoid the inconvenience and cost of frequent medical appointments. This convenience factor improves treatment satisfaction and adherence to recommended care.
“After years of dealing with knee pain that limited my daily activities, XytriX therapy gave me back my mobility. I can now enjoy walks with my family and participate in activities I thought were behind me. The improvement in my quality of life has been remarkable.”
The XytriX Treatment Process: What to Expect
Understanding the treatment process helps patients prepare mentally and physically for XytriX therapy. The journey from initial consultation through follow-up care involves several well-defined steps. Each phase serves an important purpose in ensuring optimal treatment outcomes.
Initial Consultation and Evaluation
The treatment journey begins with a comprehensive medical evaluation. Healthcare providers review your complete medical history, including previous treatments and current medications. This information helps determine if XytriX represents an appropriate treatment option.
Physical examination of the affected knee assesses disease severity and functional limitations. Providers evaluate range of motion, joint stability, and pain levels. This hands-on assessment provides crucial information for treatment planning.
Diagnostic imaging studies may be ordered or reviewed. X-rays reveal bone changes and joint space narrowing characteristic of osteoarthritis. MRI scans can provide detailed views of cartilage and soft tissues. These imaging results help confirm diagnosis and guide treatment decisions.
Pre-Treatment Requirements
- Complete medical history documentation
- Physical examination of knee joint
- Review of current medications and allergies
- Imaging studies (X-ray, possibly MRI)
- Discussion of treatment expectations
- Informed consent process
Patient Preparation Steps
- Arrange transportation for injection day
- Discontinue certain medications if advised
- Plan for rest period after procedure
- Prepare questions for medical team
- Complete required paperwork
- Verify insurance coverage details
The Injection Procedure
The actual XytriX injection takes place in a clinical setting equipped for sterile procedures. The process typically requires 30 to 45 minutes including preparation and post-procedure observation time. The injection itself takes only a few minutes.
Before the injection, the treatment area undergoes thorough cleaning with antiseptic solution. This crucial step minimizes infection risk. Some providers use ultrasound guidance to ensure precise needle placement within the joint space.
Local anesthesia may be offered to minimize discomfort during the procedure. A small needle administers the anesthetic before the treatment injection. Many patients report the procedure causes minimal pain, similar to other injections they have received.
- Patient positioning for optimal knee joint access
- Skin preparation with antiseptic cleaning solution
- Local anesthesia administration if requested
- Precise needle insertion into joint space
- Single intra-articular injection of XytriX therapy
- Needle removal and injection site protection
- Brief observation period before discharge
Immediate Post-Injection Period
After receiving XytriX injection, patients rest briefly in the treatment facility. Medical staff monitor for any immediate adverse reactions. This observation period typically lasts 15 to 30 minutes before discharge.
Most patients can walk and bear weight on the treated knee immediately after injection. However, providers recommend limiting strenuous activities for the first 24 to 48 hours. This rest period allows the therapy to begin working without excessive mechanical stress.
Some temporary discomfort at the injection site is normal and expected. This may include mild pain, warmth, or slight swelling. These symptoms typically resolve within one to two days without intervention.
First 48 Hours Care Instructions: Apply ice to the injection site for 15 minutes several times daily. Avoid high-impact activities, prolonged standing, or strenuous exercise. Take over-the-counter pain relievers if needed for injection site discomfort. Contact your provider if severe pain, significant swelling, or fever develops.
Recovery Timeline and Expectations
The timeline for experiencing XytriX benefits varies among individuals. Some patients notice initial improvements within the first few weeks. Others require additional time before significant changes become apparent.
Week one typically involves recovery from the injection procedure itself. Any injection site discomfort should resolve during this period. Patients gradually return to normal daily activities as comfortable.
Weeks two through four often mark the beginning of therapeutic effects. Pain levels may start decreasing. Some patients notice improved ability to perform certain activities. These early improvements often continue progressing over subsequent weeks.
| Time Period | Expected Progress | Activity Level | Follow-up Schedule |
| Days 1-3 | Injection site healing, potential mild discomfort | Light activities only, avoid strenuous exercise | Contact provider if concerns arise |
| Week 1 | Resolution of injection-related symptoms | Gradual return to normal activities | Phone check-in with medical team |
| Weeks 2-4 | Initial therapeutic effects may begin | Resume most regular activities as tolerated | Optional visit if questions arise |
| Weeks 8-12 | Noticeable pain reduction and function improvement | Full activity participation encouraged | Scheduled outcome assessment visit |
| Weeks 12-24 | Peak therapeutic effects typically achieved | Maintain active lifestyle and exercise | Follow-up visit at week 24 |
| Months 6-12 | Sustained benefit maintenance | Continue healthy joint maintenance habits | Annual or as-needed follow-up |
Follow-Up Care and Monitoring
Scheduled follow-up appointments allow providers to monitor treatment response. These visits typically occur at predetermined time points after injection. Week 12 and week 24 assessments are common in clinical practice.
During follow-up visits, providers reassess pain levels using standardized scales. Functional capacity is evaluated through physical examination and patient-reported outcome measures. The Western Ontario McMaster Universities Osteoarthritis Index may be repeated to track progress.
Patients should maintain contact with their healthcare team throughout the recovery process. Questions or concerns can be addressed through phone consultations between scheduled visits. This ongoing communication ensures optimal treatment outcomes and patient satisfaction.
Schedule Your XytriX Consultation Today
Speak with a knee osteoarthritis specialist who can answer your questions about XytriX therapy. Our experienced medical team is ready to help you determine if this treatment is right for you.
Consultations available Monday-Friday, 8 AM – 6 PM EST. Same-day appointments often available.
Who is an Ideal Candidate for XytriX Therapy
Not every person with knee osteoarthritis qualifies as an ideal candidate for XytriX therapy. Specific criteria help identify patients most likely to benefit from this treatment approach. Understanding these factors helps set appropriate expectations and optimize outcomes.
Disease Severity and Stage Requirements
XytriX therapy shows optimal effectiveness in patients with specific disease stages. Clinical trials primarily enrolled individuals with moderate to moderately severe knee osteoarthritis. This patient population demonstrated the most significant treatment benefits.
Very early-stage osteoarthritis may not require such advanced intervention. Conservative treatments often provide adequate relief for mild disease. Conversely, end-stage osteoarthritis with bone-on-bone contact may respond less favorably to injection therapies.
Radiographic findings help determine disease stage and treatment appropriateness. Joint space narrowing visible on X-rays indicates cartilage loss. The degree of narrowing correlates with osteoarthritis severity and helps guide treatment selection.
- Moderate knee osteoarthritis with persistent symptoms despite conservative care
- Radiographic evidence of joint space narrowing but retained cartilage
- Pain levels significantly impacting daily activities and quality of life
- Functional limitations interfering with work or recreation
- Desire to delay or avoid knee replacement surgery
- Inadequate response to previous conservative treatment attempts
Age and General Health Considerations
Clinical study participants included adult patients across a wide age range. Both middle-aged individuals and older adults participated in trials. Age alone does not disqualify patients from receiving XytriX therapy.
Overall health status matters more than chronological age. Patients should be healthy enough to tolerate the injection procedure and follow post-treatment recommendations. Certain medical conditions may require careful evaluation before proceeding with treatment.
Health Factors Affecting Eligibility
Several health conditions require evaluation when considering XytriX therapy. Active joint infection represents an absolute contraindication to intra-articular injection. The procedure must wait until infection fully resolves.
Bleeding disorders or anticoagulation therapy require special consideration. Increased bleeding risk may complicate injection procedures. Healthcare providers assess individual risk and may adjust blood-thinning medications temporarily.
Uncontrolled diabetes can affect wound healing and infection risk. Blood sugar control should be optimized before elective procedures. Well-managed diabetes does not preclude XytriX treatment.
Previous Treatment History
Ideal candidates typically have tried conservative treatments without achieving adequate relief. Physical therapy, weight management, and oral medications represent first-line approaches. When these measures prove insufficient, advanced therapies like XytriX become appropriate.
Previous corticosteroid injections do not disqualify patients from XytriX therapy. Many trial participants had received prior injections. However, adequate time should pass between different injection treatments to ensure proper evaluation of each therapy’s effects.
| Candidate Category | Characteristics | Treatment Outlook |
| Ideal Candidate | Moderate osteoarthritis, failed conservative care, good overall health, realistic expectations | Excellent potential for significant benefit |
| Good Candidate | Moderately severe disease, some response to previous treatments, mild comorbidities | Very good likelihood of meaningful improvement |
| Possible Candidate | Early or advanced disease, multiple health conditions, uncertain treatment adherence | Requires individual evaluation and discussion |
| Poor Candidate | End-stage bone-on-bone arthritis, active infection, unrealistic expectations | Alternative treatments likely more appropriate |
Patient Expectations and Goals
Realistic treatment expectations significantly influence satisfaction with outcomes. XytriX offers substantial benefits for many patients, but results vary among individuals. Complete elimination of all symptoms is uncommon, though meaningful improvement is typical.
Patients seeking to delay or avoid knee replacement surgery often find XytriX valuable. The therapy can provide symptom relief that extends the time before surgical intervention becomes necessary. This delay allows patients to maintain their natural joint longer.
Goals of improved function and quality of life align well with XytriX capabilities. Patients wanting to return to favorite activities or improve daily functioning typically achieve these objectives. Those expecting miraculous transformation may experience disappointment.
“I wasn’t looking for a miracle cure, just something that would help me stay active and reduce my daily pain. XytriX exceeded my expectations. My knee feels better than it has in years, and I’ve been able to return to hiking, which I thought I’d have to give up forever.”
Lifestyle and Compliance Factors
Successful treatment requires patient cooperation with post-injection instructions. Following activity restrictions during the initial healing period is essential. Patients unable or unwilling to comply with these recommendations may experience suboptimal results.
Commitment to complementary care measures enhances XytriX benefits. Maintaining healthy weight reduces joint stress. Regular appropriate exercise strengthens supporting muscles. These lifestyle factors significantly influence long-term outcomes.
Physical Factors
- Body mass index under 40 preferred
- Ability to participate in rehabilitation
- No active joint or systemic infection
- Adequate joint space remaining on imaging
Psychological Factors
- Realistic expectations about outcomes
- Understanding of treatment limitations
- Motivation for self-care participation
- Mental health stability
Social Factors
- Transportation to appointments available
- Support system for recovery period
- Financial resources or insurance coverage
- Time availability for follow-up care
How XytriX Compares to Other Osteoarthritis Treatments
Understanding how XytriX relates to other available treatments helps patients and providers make informed decisions. Knee osteoarthritis care includes numerous options ranging from conservative measures to surgical intervention. Each approach has distinct advantages, limitations, and appropriate use cases.
Conservative Treatment Approaches
First-line osteoarthritis management typically includes non-invasive therapies. These approaches form the foundation of care for most patients. Physical therapy, exercise programs, weight management, and oral medications represent standard initial treatments.
Physical therapy strengthens muscles supporting the knee joint. Improved muscle function reduces joint stress and may decrease pain. Exercise programs maintain mobility and prevent stiffness. These interventions require ongoing commitment and time investment.
Oral medications include over-the-counter pain relievers and prescription anti-inflammatory drugs. These provide symptomatic relief but don’t modify disease progression. Long-term use of oral medications carries risks of gastrointestinal, cardiovascular, and kidney complications.
Conservative Treatment Benefits
- Low risk and non-invasive approaches
- Readily accessible and affordable options
- Supports overall health and fitness
- Can be combined with other therapies
- Appropriate for all disease stages
Conservative Treatment Limitations
- Often provides only modest benefit
- Requires ongoing daily commitment
- Effects cease when treatment stops
- May be insufficient for moderate to severe disease
- Medication side effects with long-term use
Corticosteroid Injections
Intra-articular corticosteroid injections have been used for decades in osteoarthritis management. These injections provide anti-inflammatory effects within the joint. Pain relief often occurs rapidly, sometimes within days of injection.
The duration of benefit from corticosteroid injections varies considerably. Some patients experience relief lasting weeks or months. Others find effects diminish quickly. Repeated injections show progressively shorter duration of benefit.
Safety concerns limit the frequency of corticosteroid injections. Repeated exposure may accelerate cartilage breakdown. Most guidelines recommend limiting injections to three or four per year in the same joint. This restriction limits their usefulness for long-term management.
Hyaluronic Acid Injections
Viscosupplementation with hyaluronic acid represents another injection-based treatment. This naturally occurring joint fluid component may improve lubrication and reduce inflammation. Treatment typically requires a series of three to five injections over several weeks.
Evidence regarding hyaluronic acid efficacy remains mixed. Some studies show meaningful benefit while others demonstrate minimal advantage over placebo. Patient response varies widely, with some experiencing significant relief and others noting little change.
The multiple-injection protocol of hyaluronic acid therapy contrasts with XytriX’s single intra-articular injection approach. Convenience favors treatments requiring fewer procedures. Multiple injections increase time commitment, cost, and cumulative risk exposure.
| Treatment Type | Administration | Duration of Effect | Key Advantages | Main Limitations |
| XytriX Therapy | Single intra-articular injection | Months (6-12 typical) | Sustained benefit, disease modification potential, single treatment | Newer therapy, cost considerations, variable individual response |
| Corticosteroid Injections | Intra-articular injection | Weeks to months (2-12 typical) | Rapid pain relief, widely available, decades of use | Temporary effect, injection frequency limits, potential cartilage damage |
| Hyaluronic Acid | Series of 3-5 injections | Months (3-6 typical) | Natural substance, may improve lubrication, established safety | Multiple injections required, mixed efficacy evidence, variable response |
| Oral NSAIDs | Daily oral medication | Hours (requires continuous use) | Readily available, affordable, immediate effect | Systemic side effects, ongoing cost, only symptomatic relief |
| Physical Therapy | Multiple therapy sessions | Ongoing (requires continued exercise) | Low risk, overall health benefits, strengthens joint support | Time commitment, modest effect alone, requires sustained effort |
| Knee Replacement Surgery | One-time surgical procedure | Years to decades (15-20+ typical) | Definitive solution, dramatic improvement, long-lasting | Major surgery, recovery time, prosthetic complications, irreversible |
Surgical Options and Joint Replacement
Total knee replacement represents the definitive treatment for end-stage osteoarthritis. This major surgical procedure removes damaged joint surfaces and replaces them with prosthetic components. Outcomes are generally excellent, with most patients achieving significant pain relief and function improvement.
However, surgery carries inherent risks including infection, blood clots, and anesthesia complications. Recovery requires months of rehabilitation. The prosthetic joint has a finite lifespan, typically 15 to 20 years. Younger patients may require revision surgery during their lifetime.
Many patients prefer delaying surgery as long as possible. Preserving the natural joint remains preferable when conservative measures can provide adequate symptom control. XytriX and similar advanced therapies may extend the time before surgery becomes necessary.
Combination Therapy Approaches
Osteoarthritis management often involves combining multiple treatment modalities. XytriX therapy can integrate into comprehensive care plans alongside other interventions. Physical therapy, appropriate exercise, weight management, and occasional pain medication use complement XytriX treatment.
This multimodal approach addresses disease from multiple angles. Injection therapy targets joint-level pathology. Physical measures strengthen supporting structures. Lifestyle modifications reduce mechanical stress. Together, these interventions optimize outcomes.
- XytriX provides sustained symptom relief and potential disease modification
- Physical therapy strengthens muscles and improves joint mechanics
- Weight management reduces load on weight-bearing joints
- Appropriate exercise maintains mobility and cardiovascular health
- Assistive devices like braces provide additional joint support
- Occasional pain medication addresses breakthrough symptoms
Cost-Effectiveness Considerations
Treatment costs represent an important practical consideration. Conservative therapies generally cost less initially but require ongoing expenses. Medications, physical therapy sessions, and assistive devices accumulate costs over time.
Advanced injection therapies including XytriX involve higher upfront costs. However, the single intra-articular injection approach may prove cost-effective over time. Avoiding repeated treatments reduces cumulative expenses and time investment.
Delaying or preventing knee replacement surgery generates substantial cost savings. Total knee replacement and associated rehabilitation exceed tens of thousands of dollars. Effective non-surgical management provides both clinical and economic benefits.
Compare Your Treatment Options with Expert Guidance
Speak directly with a knee osteoarthritis specialist who can help you understand how XytriX compares to other treatments based on your specific condition, health status, and goals.
Free consultation available. Our specialists will review your medical history and help you make an informed decision about the best treatment approach for your needs.
Potential Side Effects and Risks of XytriX Therapy
Like all medical treatments, XytriX therapy carries potential side effects and risks. Understanding these possibilities helps patients make informed decisions and recognize when to seek medical attention. Most adverse events are mild and resolve without intervention.
Common Side Effects
The most frequently reported side effects relate to the injection procedure itself. Temporary pain at the injection site affects approximately one in five patients. This discomfort typically remains mild and resolves within 24 to 48 hours.
Mild swelling may develop in the treated knee joint. This reaction represents a normal inflammatory response to the injection. Ice application and rest usually provide adequate relief. Swelling typically subsides within a few days.
Some patients experience temporary warmth or redness around the injection site. These symptoms indicate localized inflammation. They should resolve quickly without specific treatment. Persistent or worsening symptoms warrant medical evaluation.
Mild Side Effects
These common reactions typically resolve without medical intervention.
- Injection site pain (mild to moderate, short-term)
- Temporary joint swelling lasting 1-3 days
- Warmth or redness at injection location
- Brief increase in knee discomfort
- Mild bruising around injection site
- Temporary stiffness in treated joint
Managing Common Side Effects
Simple measures effectively address most minor reactions.
- Apply ice packs for 15 minutes several times daily
- Rest the treated knee and avoid strenuous activity
- Elevate the leg when resting to reduce swelling
- Use over-the-counter pain relievers if needed
- Avoid hot baths or heating pads initially
- Contact provider if symptoms worsen or persist
Serious but Rare Complications
Serious adverse events occur rarely with XytriX therapy. Clinical trial data showed serious complications in fewer than 2% of participants. These events require immediate medical attention when they occur.
Joint infection represents the most concerning potential complication of any intra-articular injection. Signs include severe pain, significant swelling, fever, and warmth in the joint. Infection requires prompt antibiotic treatment and possibly drainage procedures.
Allergic reactions to treatment components can occur, though they remain uncommon. Symptoms may include rash, itching, difficulty breathing, or swelling of the face and throat. Severe allergic reactions require emergency medical care.
Seek Immediate Medical Attention If You Experience: Severe or worsening knee pain unrelieved by prescribed medications; significant swelling with warmth and redness; fever above 100.4°F (38°C); inability to bear weight on the leg; signs of allergic reaction including rash, hives, or breathing difficulty; drainage or pus from the injection site.
Infection Risk and Prevention
While joint infection risk remains low with proper technique, it cannot be eliminated entirely. Strict sterile procedures during injection significantly reduce this risk. Healthcare providers follow established protocols to maintain aseptic conditions.
Patients can help minimize infection risk by maintaining good skin hygiene before the procedure. Avoiding scratching or irritating the knee area prior to injection is important. Following post-injection care instructions reduces contamination risk.
- Sterile technique during all aspects of injection procedure
- Thorough skin preparation with antiseptic solution
- Single-use, sterile equipment for each injection
- Post-procedure monitoring for early infection signs
- Patient education about infection symptoms and reporting
- Prompt treatment if infection develops
Individual Risk Factors
Certain patient characteristics may increase the likelihood of experiencing side effects. Pre-existing health conditions require careful evaluation. Providers assess individual risk profiles before recommending XytriX therapy.
Patients with compromised immune systems face higher infection risk. Diabetes, especially when poorly controlled, affects wound healing and immune function. Immunosuppressive medications taken for other conditions also increase vulnerability.
Bleeding disorders or anticoagulation therapy warrant special consideration. These conditions increase bleeding and bruising risk. Providers may temporarily adjust blood-thinning medications around the procedure. Close monitoring ensures safe treatment delivery.
| Risk Factor Category | Specific Considerations | Risk Management Approach |
| Immune System | Diabetes, immunosuppressive medications, HIV, cancer treatment | Enhanced monitoring, antibiotic prophylaxis consideration, optimization of underlying condition |
| Bleeding Risk | Anticoagulation therapy, bleeding disorders, antiplatelet medications | Medication adjustment timing, careful injection technique, prolonged post-procedure monitoring |
| Allergies | Previous allergic reactions, multiple drug allergies, severe allergy history | Detailed allergy history review, component testing if available, emergency equipment availability |
| Skin Conditions | Active skin infection, psoriasis, eczema near injection site | Treatment of skin conditions before injection, alternative injection site consideration, enhanced sterile preparation |
Long-Term Safety Considerations
Extended follow-up studies continue monitoring patients for delayed adverse events. Current evidence suggests XytriX maintains its favorable safety profile over time. No concerning late-emerging complications have been identified.
The single intra-articular injection approach offers safety advantages over treatments requiring repeated administrations. Cumulative exposure remains limited, reducing overall risk burden. This feature particularly benefits patients requiring long-term osteoarthritis management.
Ongoing post-marketing surveillance tracks real-world safety as more patients receive XytriX therapy. This monitoring system identifies rare complications that might not appear in clinical trials. Such surveillance ensures continued treatment safety as use expands.
Reporting and Managing Adverse Events
Patients should report any unusual symptoms to their healthcare providers promptly. Early recognition of complications allows timely intervention. Don’t hesitate to contact your medical team with concerns, even if symptoms seem minor.
Healthcare providers document and report serious adverse events through established channels. This reporting contributes to the broader safety database. Information gathered helps improve treatment protocols and patient education.
“Understanding potential risks helped me make an informed decision about XytriX therapy. My doctor thoroughly explained what to expect and when to call with concerns. I experienced only mild injection site soreness that resolved in a day. The benefits have far outweighed any temporary discomfort.”
Insurance Coverage and Cost Considerations
Understanding financial aspects of XytriX therapy helps patients plan for treatment. Cost and insurance coverage vary significantly depending on multiple factors. Early investigation of these practical matters prevents surprises and facilitates access to care.
Insurance Coverage Status
Insurance coverage for XytriX therapy depends on several factors. Plan type, specific policy provisions, and medical necessity determination all influence coverage. The therapy’s relatively recent FDA approval process means coverage policies continue evolving.
Some insurance plans classify XytriX as an experimental or investigational treatment. This designation often results in coverage denial. However, as clinical evidence accumulates and the therapy gains acceptance, more insurers are reconsidering coverage policies.
Medical necessity criteria must be satisfied for insurance approval. Documentation of failed conservative treatments typically supports medical necessity claims. Providers submit detailed justification explaining why XytriX represents an appropriate treatment choice.
Coverage Tip: Contact your insurance company before treatment to verify coverage and understand your financial responsibility. Request pre-authorization if your plan requires it. Ask about appeal processes if initial coverage is denied.
Out-of-Pocket Costs
For patients paying entirely out-of-pocket, XytriX treatment costs vary by provider and location. The therapy represents a significant investment, though pricing remains competitive with other advanced osteoarthritis treatments. Single injection protocols may prove cost-effective compared to multi-session alternatives.
Treatment costs typically include several components. The therapy itself represents the largest expense. Physician fees for administration add to the total. Facility fees may apply depending on where treatment occurs. Pre-treatment evaluations and imaging studies incur additional costs.
- XytriX therapy product cost varies by provider and region
- Physician administration fees for injection procedure
- Facility fees if treatment occurs in hospital or surgery center
- Pre-treatment consultation and evaluation charges
- Imaging studies like X-rays or MRI if needed
- Follow-up visit costs for monitoring treatment response
Financial Assistance Options
Several resources may help reduce treatment costs for eligible patients. Manufacturer patient assistance programs sometimes offer financial support. These programs typically have income requirements and application processes.
Healthcare financing companies provide payment plans for medical procedures. These arrangements allow spreading costs over time through monthly installments. Interest rates and terms vary among lenders. Careful review of financing agreements prevents unexpected obligations.
Patient Assistance Programs
Manufacturer and nonprofit programs may help eligible patients afford treatment.
- Income-based assistance for qualifying patients
- Co-pay assistance for insured patients
- Free or reduced-cost treatment programs
- Application process and eligibility verification
Alternative Funding Sources
Additional financial resources may be available through various channels.
- Healthcare credit cards with promotional financing
- Medical payment plans through providers
- Health savings accounts (HSA) or flexible spending accounts (FSA)
- Nonprofit organizations supporting arthritis patients
Cost Comparison with Alternative Treatments
Evaluating XytriX costs requires comparing to alternative treatment approaches. While initial investment may seem substantial, long-term cost-effectiveness matters more than upfront price. Treatments requiring ongoing expenses accumulate significant costs over time.
Conservative treatments like physical therapy and medications involve lower individual costs but continuous expenses. Multiple therapy sessions over months or years add up. Daily medications create ongoing financial burden. These cumulative costs may exceed single-treatment therapies.
| Treatment Type | Typical Cost Range | Treatment Frequency | Annual Cost Estimate |
| XytriX Therapy | $3,000 – $6,000 | Single injection (effect lasts months) | $3,000 – $6,000 |
| Hyaluronic Acid Series | $1,500 – $3,000 per series | 3-5 injections, may repeat 2-3 times yearly | $3,000 – $9,000 |
| Corticosteroid Injections | $150 – $500 per injection | Every 3-4 months (maximum 3-4 yearly) | $600 – $2,000 |
| Oral Medications | $50 – $300 monthly | Daily, ongoing | $600 – $3,600 |
| Physical Therapy | $75 – $200 per session | 2-3 times weekly initially, then periodic maintenance | $2,000 – $5,000 |
| Total Knee Replacement | $30,000 – $50,000 | One-time (prosthetic lasts 15-20 years typically) | $1,500 – $3,300 (amortized) |
Tax Deductions and Healthcare Accounts
Medical expenses including XytriX therapy may qualify for tax deductions. The IRS allows deducting qualified medical expenses exceeding a certain percentage of adjusted gross income. Consult a tax professional regarding your specific situation and potential deductions.
Health savings accounts (HSA) and flexible spending accounts (FSA) offer tax-advantaged ways to pay for medical care. Contributions reduce taxable income. Withdrawals for qualified medical expenses remain tax-free. XytriX therapy typically qualifies as a legitimate HSA or FSA expense.
Value Proposition and Return on Investment
Beyond direct financial costs, consider the value of improved quality of life. Reduced pain and better function enable continued employment for many patients. Workplace productivity increases when osteoarthritis symptoms improve. These factors provide substantial personal economic benefit.
Delaying or avoiding knee replacement surgery saves considerable expense. Total joint replacement costs tens of thousands of dollars plus rehabilitation and recovery time. Even if XytriX eventually leads to surgery, extending this timeline by years provides financial and quality-of-life benefits.
Financial Planning Tip: When evaluating XytriX costs, consider total value over time rather than just initial price. Calculate potential savings from reduced medication use, fewer doctor visits, maintained work productivity, and delayed surgery. Many patients find the investment worthwhile when considering these comprehensive benefits.
Real Patient Experiences with XytriX Therapy
Understanding how XytriX has affected real patients provides valuable perspective beyond clinical trial statistics. Individual experiences vary, but common themes emerge regarding treatment benefits, challenges, and overall satisfaction. These stories offer insight into what new patients might expect.
Success Stories and Positive Outcomes
Many patients report significant life-changing improvements following XytriX treatment. Pain reduction enables return to activities they had abandoned due to osteoarthritis limitations. The ability to play with grandchildren, pursue hobbies, or simply walk without discomfort profoundly impacts quality of life.
“Before XytriX, I was considering early retirement because my knee pain made it difficult to stand for long periods at my job. Three months after treatment, I’m back to working full shifts without constant discomfort. I’ve even started taking evening walks again, something I hadn’t done in years. This therapy gave me back my independence.”
Patients frequently describe improved sleep quality as a major benefit. Chronic pain often disrupts nighttime rest, creating a cycle of fatigue and reduced pain tolerance. As XytriX reduces pain, sleep improves, leading to better overall functioning and mood.
Common Positive Outcomes
- Significant reduction in daily knee pain levels
- Improved ability to perform work responsibilities
- Return to recreational activities and hobbies
- Better sleep quality without nighttime pain
- Reduced reliance on pain medications
- Enhanced emotional well-being and outlook
- Greater independence in daily living activities
- Ability to delay or avoid knee replacement surgery
Varied Response Patterns
Not all patients experience identical results from XytriX therapy. Response timing varies considerably among individuals. Some notice improvements within weeks while others require more time to experience maximum benefit.
“My improvement was gradual rather than sudden. I didn’t wake up one day with a perfect knee. Instead, I slowly realized I was doing more activities without thinking about pain. By three months post-injection, I had definitely improved, though I still have some limitations. For me, the therapy provided meaningful benefit even though it wasn’t a complete cure.”
The degree of improvement also varies. Some patients achieve near-complete pain relief while others experience more modest reductions. Factors influencing response include disease severity, overall health, adherence to post-treatment recommendations, and individual biological variability.
Challenges and Realistic Expectations
Honest patient accounts include challenges alongside benefits. Managing expectations requires understanding that XytriX works better for some individuals than others. No treatment succeeds for everyone, and osteoarthritis remains a chronic progressive disease.
Some patients experienced initial disappointment when immediate dramatic improvement didn’t occur. Learning that benefits develop gradually helped adjust expectations. Patience during the first weeks and months proved important for realistic outcome assessment.
What if XytriX doesn’t work as well as hoped?
Treatment response varies among patients. If benefits seem inadequate after sufficient time, discuss options with your provider. Alternative or additional treatments may be considered. Some patients benefit from combining XytriX with other therapies like physical therapy or weight management.
How long should I wait before judging treatment effectiveness?
Most providers recommend waiting at least 12 weeks before fully evaluating XytriX effectiveness. Some patients notice earlier improvements, but peak benefits typically develop over several months. Keep a symptom diary to objectively track changes that might be gradual.
Can XytriX be repeated if effects wear off?
The duration of benefit from XytriX varies among patients. While clinical trial data provides general timelines, individual experiences differ. Discuss repeat treatment possibilities with your healthcare provider if initial benefits begin declining. Long-term treatment protocols continue being studied.
Impact on Daily Life Activities
Patients consistently emphasize functional improvements when describing XytriX benefits. The ability to complete everyday tasks without pain or limitation represents meaningful success. These practical improvements often matter more than numeric pain scale reductions.
“The best part about XytriX wasn’t just that my pain decreased—it was that I could do normal things again. Grocery shopping, climbing stairs, getting in and out of the car—these simple activities had become major challenges. Now I do them without thinking twice. That’s real quality of life improvement.”
Home and Family
Patients report meaningful improvements in domestic and family activities.
- Playing with children or grandchildren
- Completing household chores and yard work
- Participating in family outings and events
- Maintaining independence in self-care
Work and Career
Professional life benefits from restored function and reduced pain.
- Maintaining full work schedules and duties
- Standing or walking required for jobs
- Improved focus without pain distraction
- Extended career longevity
Recreation and Leisure
Enjoyable activities become accessible again after treatment.
- Walking, hiking, or light jogging
- Golf, tennis, or other sports
- Gardening and outdoor hobbies
- Travel without mobility concerns
Frequently Asked Questions About XytriX Therapy
Patients considering XytriX therapy naturally have many questions. Understanding common concerns helps individuals make informed treatment decisions. The following addresses frequently asked questions based on patient inquiries and clinical experience.
How soon after XytriX injection can I return to normal activities?
Most patients resume light daily activities within 24 hours after injection. Walking and routine tasks are generally fine immediately. However, strenuous exercise, high-impact activities, or prolonged standing should be avoided for 48 to 72 hours.
Your healthcare provider will give specific activity guidelines based on your situation. Following these recommendations helps optimize treatment outcomes. Gradual activity resumption over the first week allows the therapy to begin working effectively.
Is XytriX therapy painful?
The injection procedure itself causes minimal discomfort for most patients. Local anesthesia can be provided to numb the area before injection. Many people describe the sensation as similar to other injections they’ve received.
Some temporary soreness at the injection site is common in the first day or two. This discomfort typically remains mild and responds well to ice and over-the-counter pain relievers. Severe or prolonged pain is uncommon and should be reported to your provider.
How long do the benefits of XytriX last?
Clinical trial data shows benefits lasting at least six months for many patients, with some experiencing improvements extending to 12 months or longer. Individual duration varies based on multiple factors including disease severity and overall health.
As XytriX represents a relatively new therapy, long-term data continues accumulating. Some patients may require repeat treatment when initial benefits decline. Your healthcare provider can discuss repeat treatment options based on your response.
Can I receive XytriX in both knees?
Yes, patients with bilateral knee osteoarthritis can receive XytriX in both knees. However, providers typically recommend treating one knee first, allowing that joint to heal before treating the second knee. This staged approach ensures better mobility during recovery.
Some providers may treat both knees simultaneously if circumstances warrant. This decision depends on individual factors including disease severity, mobility status, and support system availability during recovery.
Does XytriX work for severe or end-stage osteoarthritis?
XytriX shows optimal effectiveness in moderate to moderately severe osteoarthritis. Very advanced disease with complete cartilage loss and bone-on-bone contact may respond less favorably. These cases often require surgical intervention for meaningful improvement.
Your healthcare provider will evaluate X-rays and clinical findings to determine if XytriX represents an appropriate option for your disease stage. Honest discussion about realistic expectations helps ensure satisfaction with treatment decisions.
Can I combine XytriX with other osteoarthritis treatments?
XytriX often works well as part of a comprehensive treatment plan. Physical therapy, appropriate exercise, weight management, and occasional pain medication can complement XytriX therapy. This multimodal approach addresses osteoarthritis from multiple angles.
However, avoid other knee injections immediately before or after XytriX to prevent confusion about which treatment produces effects. Discuss timing of other interventions with your provider to optimize overall management strategy.
What happens if XytriX doesn’t help my knee pain?
While most patients experience meaningful benefit, XytriX doesn’t work equally well for everyone. If adequate improvement doesn’t occur after sufficient time, discuss alternative options with your provider. Other injection therapies, continued conservative care, or surgical evaluation may be considered.
Treatment failure doesn’t necessarily mean other approaches won’t help. Each therapy has different mechanisms and effectiveness profiles. Your healthcare team can develop alternative strategies tailored to your needs.
Are there any dietary or lifestyle restrictions after XytriX injection?
No specific dietary restrictions apply after XytriX treatment. However, maintaining healthy nutrition supports overall joint health and healing. Anti-inflammatory foods may provide additional benefit for osteoarthritis management.
Lifestyle modifications that support joint health enhance treatment outcomes. Weight management reduces knee stress. Low-impact exercise maintains mobility without excessive joint loading. Avoiding high-impact activities during initial recovery protects the treated joint.
How does XytriX compare to stem cell therapy for knee osteoarthritis?
Both XytriX and stem cell approaches represent regenerative medicine strategies. They aim to modify disease processes rather than simply managing symptoms. However, these therapies have different mechanisms, evidence levels, and regulatory statuses.
XytriX has undergone rigorous clinical trial evaluation documented in the National Library of Medicine. Stem cell therapy evidence remains more limited with variable quality. Discuss the relative merits of each approach with a knowledgeable provider familiar with current research.
Will insurance cover XytriX therapy?
Insurance coverage varies widely depending on your specific plan and policy provisions. Some insurers cover XytriX while others currently classify it as experimental or investigational. Coverage policies continue evolving as evidence accumulates.
Contact your insurance company before treatment to verify coverage and understand your financial responsibility. Request pre-authorization if required. If initially denied, appeal processes may be available, especially with strong medical necessity documentation from your provider.
Future Developments and Ongoing Research
The field of osteoarthritis treatment continues advancing rapidly. XytriX represents current innovation, but ongoing research explores further improvements and applications. Understanding the development pipeline provides insight into future treatment possibilities.
Ongoing Clinical Trials and Studies
Multiple research efforts continue evaluating XytriX therapy. Extended follow-up studies track patients for longer periods, documenting duration of benefit and long-term safety. These investigations provide crucial information about sustained treatment effects.
Researchers are exploring XytriX applications in different patient populations. Studies examining treatment in younger patients or those with early-stage disease may expand approved indications. Investigation of bilateral treatment protocols optimizes approaches for people with osteoarthritis in both knees.
Combination therapy trials evaluate whether XytriX works synergistically with other treatments. Pairing injection therapy with optimized physical therapy, nutritional interventions, or complementary injections may enhance outcomes. These multimodal approaches could become standard care.
- Long-term outcome studies following patients for multiple years
- Dose-optimization research exploring ideal therapeutic amounts
- Comparison trials directly evaluating XytriX against other advanced therapies
- Biomarker studies identifying which patients respond best to treatment
- Cost-effectiveness analyses examining economic value of therapy
- Quality of life research documenting broader treatment impacts
Regulatory Developments
The FDA approval pathway for XytriX involved rigorous evaluation of safety and efficacy data. As additional evidence accumulates, regulatory designations may evolve. Regenerative Medicine Advanced Therapy (RMAT) designation, if granted, could expedite further development.
Regulatory approvals in other countries expand global access to XytriX therapy. International clinical trials provide data from diverse patient populations. These worldwide efforts contribute to comprehensive understanding of treatment benefits and limitations.
FDA Development Status: XytriX therapy continues progressing through regulatory pathways in the United States. The FDA carefully evaluates all available safety and efficacy data before making approval decisions. Patients and providers can track development updates through official FDA communications and clinical trial databases.
Expanding Treatment Applications
While current focus centers on knee osteoarthritis, researchers are investigating XytriX potential for other joints. Hip, shoulder, and ankle osteoarthritis represent possible future applications. If proven safe and effective, these expanded indications would benefit millions more patients.
Earlier disease intervention represents another research frontier. Current treatment primarily targets moderate to advanced osteoarthritis. Determining whether XytriX can prevent progression in early-stage disease would revolutionize management strategies. Such disease-modifying potential could preserve joints before significant damage occurs.
Potential Future Indications
- Hip joint osteoarthritis treatment
- Shoulder osteoarthritis applications
- Ankle and foot joint involvement
- Hand and finger osteoarthritis management
- Post-traumatic arthritis prevention
- Early-stage disease modification
Research Directions
- Genetic markers predicting treatment response
- Imaging biomarkers tracking cartilage changes
- Personalized dosing based on individual factors
- Combination with tissue engineering approaches
- Preventive treatment in high-risk populations
- Pediatric applications for juvenile arthritis
Technological Advances
Improvements in delivery technology may enhance XytriX effectiveness. Precision injection techniques using advanced imaging guidance ensure optimal placement. Sustained-release formulations could extend therapeutic duration. These refinements would improve convenience and outcomes.
Artificial intelligence and machine learning applications may identify ideal treatment candidates. By analyzing large datasets, algorithms could predict which patients will benefit most from XytriX. This personalized medicine approach optimizes resource allocation and patient selection.
Patient Access and Healthcare Integration
As XytriX gains acceptance, integration into standard care pathways improves patient access. Development of treatment protocols and clinical guidelines helps providers make appropriate treatment decisions. Insurance coverage expansion facilitates affordability for broader patient populations.
Patient education initiatives increase awareness of advanced treatment options. Many people with osteoarthritis remain unaware of therapies beyond basic pain medications. Improving knowledge about innovative treatments like XytriX empowers patients to advocate for comprehensive care.
Looking Ahead: The next five to ten years will likely bring significant advances in osteoarthritis treatment. XytriX represents one component of an evolving therapeutic landscape. Continued research, technological innovation, and clinical experience will refine treatment approaches and expand options for patients suffering from this common and debilitating condition.
Conclusion: Making Informed Decisions About XytriX Therapy
XytriX Knee Osteoarthritis Therapy represents a significant advancement in treatment options for people struggling with knee pain and functional limitations. This comprehensive guide has explored the therapy’s mechanism of action, clinical efficacy, safety profile, and practical considerations that matter to patients.
The decision to pursue XytriX treatment should involve careful consideration of individual circumstances. Disease severity, previous treatment responses, overall health status, and personal goals all influence whether this therapy represents the optimal choice. No single treatment works perfectly for everyone with knee osteoarthritis.
Key Takeaways
XytriX offers substantial benefits for appropriately selected patients with moderate to moderately severe knee osteoarthritis. Clinical trials demonstrate meaningful pain reduction, functional improvement, and enhanced quality of life. The single intra-articular injection approach provides convenience compared to multi-session treatments.
Safety data from multiple study populations shows favorable risk profiles. Most adverse events remain mild and temporary. Serious complications occur rarely when proper injection techniques and patient selection criteria are followed. Long-term monitoring continues demonstrating sustained safety over time.
Ideal XytriX Candidates
- Moderate to moderately severe knee osteoarthritis confirmed by imaging
- Inadequate relief from conservative treatments
- Good overall health without contraindications
- Realistic expectations about potential outcomes
- Desire to delay or avoid knee replacement surgery
- Commitment to complementary care measures
Important Considerations
- Treatment costs and insurance coverage status
- Individual response varies among patients
- Complete pain elimination uncommon
- Benefits develop gradually over weeks to months
- Long-term durability continues being studied
- Other treatment options remain available
Next Steps
If XytriX therapy interests you, the next step involves consulting with a healthcare provider experienced in osteoarthritis management. Comprehensive evaluation determines your candidacy and helps set realistic expectations. Bring questions, medical records, and imaging studies to this consultation.
Discuss how XytriX fits into your overall treatment plan. Consider timing relative to other interventions you may be pursuing. Understand the complete treatment process from initial evaluation through follow-up care. Clarify financial responsibilities and insurance coverage before proceeding.
Remember that osteoarthritis management typically involves multiple approaches working together. XytriX can be an important component of comprehensive care that also includes appropriate exercise, weight management, and lifestyle modifications supporting joint health.
Ready to Explore XytriX Therapy for Your Knee Osteoarthritis?
Take the first step toward potentially reducing your knee pain and improving your quality of life. Our experienced medical team is ready to help you determine if XytriX therapy is right for you.
Schedule a Consultation
Meet with a knee specialist who can evaluate your condition and discuss whether XytriX therapy is appropriate for your situation.
Free Eligibility Assessment
Complete a quick assessment to find out if you may be a candidate for XytriX therapy. Get results within 24 hours.
Speak With a Specialist
Call now to speak directly with a patient coordinator who can answer your questions about XytriX therapy.
Our team is available Monday through Friday, 8 AM to 6 PM EST. Same-day appointments often available. All consultations are confidential and HIPAA-protected.
Living Well with Knee Osteoarthritis
Advances like XytriX therapy provide hope for people living with knee osteoarthritis. While this condition cannot be cured, effective management significantly improves quality of life. Modern treatments offer more options than ever before for maintaining mobility, reducing pain, and preserving independence.
Staying informed about available treatments empowers you to make the best decisions for your health. Continue learning about osteoarthritis management through reputable sources including the National Library of Medicine and professional medical organizations. Knowledge helps you become an active participant in your care.
Most importantly, don’t accept declining mobility and chronic pain as inevitable. Many effective treatments exist, with new options continuing to emerge. Working with knowledgeable healthcare providers and maintaining hope for improvement make a real difference in managing this challenging condition.