Your knee suddenly gives out during a jump. Sharp pain shoots through the front of your leg. You can’t straighten your knee properly anymore. These frightening symptoms often signal a patellar tendon injury, a condition that affects thousands of active individuals each year.
The patellar tendon connects your kneecap to your shinbone. This vital structure allows you to straighten your knee and bears significant force during everyday activities. When this tendon becomes injured, simple movements become challenging and painful.
Whether you’re an athlete, weekend warrior, or someone experiencing sudden knee pain, understanding patellar tendon injury helps you make informed decisions about your care and recovery.
⚠️ Seek Immediate Medical Attention If:
- You heard a popping sound followed by immediate severe pain
- You cannot straighten your knee or bear weight on your leg
- Your kneecap appears higher than normal or moves abnormally
- Significant swelling develops rapidly after injury
What Is the Patellar Tendon and How Does It Work?
The patellar tendon serves as a crucial connector in your knee’s extensor mechanism. This tough, fibrous tissue runs from the bottom of your patella (kneecap) down to the tibia (shinbone), typically measuring about four inches in length.
Anatomy Components
Your knee’s extensor system includes several key structures working together. The quadriceps muscles in your thigh generate power. These muscles connect to the quadriceps tendon above your kneecap. The patella acts as a pulley, increasing the mechanical advantage of your thigh muscles.
Below the kneecap, the patellar tendon completes this chain by anchoring to a bony prominence on your tibia called the tibial tuberosity. When your quadriceps muscles contract, this entire system works in harmony to straighten your leg.
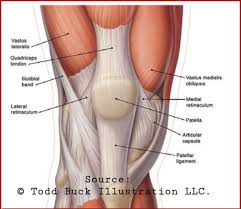
Anatomy Components
Your knee’s extensor
How the Patellar Tendon Functions
Every time you stand up, climb stairs, jump, or kick, your patellar tendon transmits tremendous force. During activities like jumping, this tendon can experience forces exceeding eight times your body weight.
The tendon’s unique structure allows it to handle these intense loads. Collagen fibers arrange themselves in parallel bundles, providing exceptional tensile strength. Blood vessels supply nutrients to keep the tissue healthy and responsive to training stress.
Types of Patellar Tendon Injuries
Patellar tendon injury encompasses several distinct conditions. Each type presents different challenges and requires specific treatment approaches.
Patellar Tendinitis (Jumper’s Knee)
Patellar tendinitis develops gradually through repetitive stress. Athletes who frequently jump or change direction experience this condition most often. Basketball players, volleyball athletes, and runners face particularly high risk.
The inflammation typically begins at the point where the tendon attaches to the kneecap. Microscopic tears accumulate in the tendon tissue over time. Without proper rest and treatment, these small tears can progress to more serious degeneration.
Early Stage Symptoms
Initial tendinitis presents mild discomfort that athletes often ignore:
- Pain after intense activity or sport
- Stiffness the morning after exercise
- Tenderness when pressing below the kneecap
- Temporary relief with warm-up activities
Advanced Stage Symptoms
Progressive tendinitis interferes with daily function:
- Pain during normal walking or climbing stairs
- Difficulty sitting with bent knee for extended time
- Constant ache even at rest
- Weakness when trying to straighten knee against resistance
Patellar Tendon Tear
A patellar tendon tear represents a more severe injury. This acute trauma usually results from a sudden, forceful contraction of the quadriceps muscle against resistance. Landing awkwardly from a jump or stumbling on stairs can cause these tears.
Tendon tears occur in two forms. Partial tears involve damage to some tendon fibers while others remain intact. Complete tears rupture the entire tendon, severing the connection between your kneecap and shinbone.
Distinguishing Tear Severity
Partial Patellar Tendon Tear: You may still be able to straighten your knee and walk, though with significant pain and difficulty. The kneecap position typically remains normal.
Complete Patellar Tendon Tear: You cannot straighten your knee on your own. The kneecap often shifts upward (high-riding patella). Weight-bearing becomes impossible without assistance.
Patellar Tendinopathy
Patellar tendinopathy describes chronic degeneration of the tendon tissue. Unlike tendinitis, which involves inflammation, tendinopathy reflects failed healing and structural breakdown of collagen fibers.
This condition develops when repeated stress exceeds the tendon’s ability to repair itself. The tissue becomes disorganized and weakened. Athletes who ignore early tendinitis warnings often progress to tendinopathy, which proves more difficult to treat.
What Causes Patellar Tendon Injury?
Sports and Physical Activities
Certain sports place exceptional demands on the patellar tendon. Jumping sports create the highest risk because landing generates enormous force through this small structure. Basketball, volleyball, and high jump require repeated explosive movements that stress the tendon.
Running activities, particularly those involving hills or speed work, also challenge the tendon. Soccer players face injury risk from kicking motions and rapid direction changes. Even recreational athletes can develop problems if they increase training intensity too quickly.
Traumatic Events
Acute tendon tears typically follow specific trauma patterns. A forceful eccentric contraction occurs when your quadriceps muscle contracts while lengthening. This happens when you land from a jump with your knee slightly bent.
Direct impact to the front of your knee can also damage the tendon. Car accidents, falls, and collisions during contact sports sometimes result in tears. Older individuals may tear their patellar tendon during relatively minor incidents if pre-existing degeneration has weakened the tissue.
High-Risk Activities
- Basketball and volleyball (frequent jumping)
- Track and field jumping events
- Skiing (eccentric quad loading)
- Soccer and football (kicking, cutting)
- Distance running with excessive mileage
- CrossFit and plyometric training
Lower-Risk Activities
- Swimming (minimal knee impact)
- Cycling on flat terrain
- Elliptical machine exercise
- Walking on level surfaces
- Yoga and stretching routines
- Upper body strength training
Individual Risk Factors
Age influences injury risk significantly. Athletes between 20 and 40 experience the highest rates of patellar tendinitis. This age group combines high activity levels with sufficient exposure time to develop overuse problems.
For acute tendon tears, age creates a different pattern. People over 40 face increased tear risk because tendons naturally weaken with aging. Blood supply to the tendon decreases, reducing the tissue’s ability to repair minor damage.
Anatomical Factors
- Tight quadriceps or hamstring muscles
- Muscle strength imbalances around knee
- Abnormal kneecap tracking patterns
- Flat feet or high arches affecting leg alignment
Training Factors
- Rapid increases in training volume
- Insufficient rest between intense sessions
- Hard training surfaces (concrete, asphalt)
- Inadequate warm-up before activity
Medical Factors
- Previous knee injuries or surgeries
- Chronic diseases affecting tendons
- Long-term corticosteroid use
- Autoimmune conditions
Recognizing Patellar Tendon Injury Symptoms
Identifying symptoms early allows for prompt treatment and better outcomes. The specific symptoms depend on whether you have gradual tendinitis or an acute tear.
Pain Characteristics
Pain location provides important diagnostic clues. Patellar tendinitis typically causes pain directly below the kneecap where the tendon attaches. This pain often feels sharp during activity but may become a dull ache afterward.
The pain pattern follows predictable stages. Early-stage pain appears only after sports or vigorous activity. As the condition progresses, pain begins during warm-up but may decrease once you’re fully warmed up. Advanced cases produce constant pain that interferes with daily activities like climbing stairs or getting up from a chair.
A complete patellar tendon tear creates immediate, severe pain. Many people describe feeling or hearing a pop at the moment of injury. The pain intensity makes bearing weight extremely difficult.
Swelling and Physical Changes
Swelling develops differently based on injury type. Chronic patellar tendinitis may produce only mild swelling localized below the kneecap. You might notice slight fullness or puffiness in this area, especially after activity.
Acute tendon tears cause rapid, significant swelling. The knee may swell within minutes to hours after the injury. A visible deformity often accompanies complete tears, with the kneecap appearing higher than normal when compared to the uninjured leg.
Functional Limitations
Loss of function varies by injury severity. People with mild tendinitis continue most activities despite discomfort. However, movements requiring powerful knee extension become problematic. Jumping, running uphill, or rising from a deep squat prove particularly difficult.
Complete patellar tendon tear creates dramatic functional loss. You cannot actively straighten your knee against gravity. Attempting to stand from a seated position becomes nearly impossible. The leg may buckle when you try to put weight on it.
When Symptoms Indicate Serious Injury
Certain symptom combinations suggest you need immediate medical evaluation rather than home treatment. Contact a doctor promptly if you experience sudden inability to straighten your knee, visible deformity of your kneecap position, severe swelling that develops within hours, or a palpable gap in the tendon below your kneecap.
Concerned About Your Knee Symptoms?
Don’t wait for symptoms to worsen. Our orthopedic specialists can evaluate your knee pain and create a personalized treatment plan to get you back to the activities you love.
How Doctors Diagnose Patellar Tendon Injury
Accurate diagnosis requires combining clinical examination with appropriate imaging studies. Your doctor follows a systematic approach to determine the exact nature and severity of your injury.
Physical Examination
Your appointment begins with a detailed discussion of your symptoms and how the injury occurred. The doctor asks about the timing of pain, specific activities that worsen symptoms, and any prior knee problems.
The physical exam assesses multiple aspects of knee function. Your doctor observes how you walk and whether your gait appears normal. Visual inspection compares both knees, looking for swelling, bruising, or abnormal kneecap position.
Palpation helps identify the pain’s exact location. Tenderness directly over the patellar tendon suggests tendinitis or tendinopathy. The examiner feels for any gaps or defects in the tendon, which indicate a tear.
Functional testing evaluates your ability to extend the knee. You may be asked to straighten your leg against resistance while lying down. Inability to perform this movement strongly suggests a complete tendon rupture.
Imaging Tests
X-rays serve as the initial imaging study for most knee injuries. While X-rays don’t show tendon tissue directly, they reveal important information. A complete patellar tendon tear often causes the kneecap to migrate upward, which appears clearly on X-ray.
X-rays also rule out other problems like fractures or arthritis. Some chronic tendon injuries create calcium deposits within the tendon that show up on X-ray images.
Advanced Imaging
Magnetic resonance imaging (MRI) provides the most detailed view of tendon structure. MRI scans show inflammation, partial tears, and degenerative changes within the tissue. This information helps doctors plan appropriate treatment.
Your doctor may order MRI when physical examination findings remain unclear, when symptoms persist despite initial treatment, or when surgery is being considered. The scan typically takes 30 to 45 minutes to complete.
Ultrasound offers another option for imaging the patellar tendon. This test costs less than MRI and can be performed during your office visit. Skilled examiners can identify tears and measure tendon thickness. However, ultrasound results depend heavily on the operator’s experience.
| Imaging Method | What It Shows | Best For | Limitations |
| X-ray | Bone position, calcium deposits, fractures | Initial screening, detecting kneecap position changes | Cannot visualize tendon tissue directly |
| MRI | Tendon structure, tears, inflammation, degeneration | Detailed assessment before surgery, unclear diagnosis | Expensive, requires 30-45 minutes, not always available |
| Ultrasound | Tendon tears, thickness, blood flow | Office-based evaluation, guided injections | Operator-dependent, less detailed than MRI |
Differential Diagnosis
Several other knee conditions can mimic patellar tendon injury. Your doctor must distinguish your condition from these alternatives to provide effective treatment.
Quadriceps tendon tear occurs above the kneecap rather than below it. This injury produces similar symptoms but requires different surgical techniques if operation becomes necessary. Patellar fracture also causes sudden pain and difficulty extending the knee, but X-rays clearly show the broken bone.
Other conditions like patellofemoral pain syndrome or knee bursitis can cause front-of-knee pain similar to tendinitis. Careful examination and sometimes imaging help distinguish these problems from true patellar tendon pathology.
Treatment Options for Patellar Tendon Injury
Treatment approaches vary dramatically based on injury type and severity. Conservative management successfully treats many cases of tendinitis and partial tears. Complete rupture almost always requires surgical repair.
Conservative Treatment for Tendinitis
Non-surgical treatment begins with modifying activities that stress the injured tendon. This doesn’t mean complete rest in most cases. Rather, you reduce high-impact activities while maintaining fitness through alternative exercises.
The RICE protocol provides initial symptom relief. Rest involves avoiding movements that provoke pain. Ice applications of 15 to 20 minutes several times daily reduce inflammation. Compression with an elastic bandage controls swelling. Elevation when sitting or lying down also helps minimize swelling.
Medication Management
Over-the-counter pain relievers help manage symptoms during the healing process. Ibuprofen and naproxen reduce both pain and inflammation. These medications work best when taken regularly for several days rather than only when pain becomes severe.
Acetaminophen provides pain relief without anti-inflammatory effects. This option works well if you cannot tolerate anti-inflammatory medications. Always follow dosing instructions and consult your doctor about appropriate medication choices for your situation.
Supportive Devices
A knee brace or strap can reduce stress on the injured tendon during daily activities. Patellar tendon straps work by applying pressure below the kneecap, which alters force distribution through the tendon. Many athletes find these devices allow them to continue modified activity during healing.
Crutches may be recommended for severe cases to limit weight-bearing stress. Using crutches for a few days or weeks gives the tendon time to begin healing before you resume normal walking.
Physical Therapy
Physical therapy forms the cornerstone of conservative patellar tendon injury treatment. A structured therapy plan addresses multiple aspects of recovery simultaneously.
Therapy Goals
Your physical therapy treatment plan focuses on specific objectives. Reducing pain and inflammation represents the initial priority. Therapists use various modalities including ice, heat, ultrasound, or electrical stimulation to manage symptoms.
Restoring normal range of motion comes next. Gentle stretching exercises prevent stiffness that often develops when you protect an injured knee. Maintaining flexibility in your quadriceps, hamstrings, and calf muscles reduces stress on the healing tendon.
Exercise Progression
Strengthening exercises follow a careful progression. You begin with isometric exercises that contract muscles without moving the joint. These exercises maintain muscle strength while minimizing tendon stress.
As healing progresses, you advance to eccentric exercises. These controlled lengthening contractions have shown particular effectiveness for treating patellar tendinopathy. Eccentric squats performed on a decline board represent a well-researched treatment for jumper’s knee.
Early Phase Exercises
- Quad sets (tightening thigh muscle)
- Straight leg raises
- Ankle pumps for circulation
- Gentle hamstring stretches
- Stationary bike with light resistance
Advanced Phase Exercises
- Eccentric decline squats
- Single leg press exercises
- Step-down movements
- Controlled jumping progressions
- Sport-specific training drills
Surgical Treatment
Surgery becomes necessary for complete patellar tendon tear and some cases of severe tendinopathy that don’t respond to conservative treatment. The surgical approach depends on the specific injury pattern.
Tendon Repair Surgery
Complete tendon tears require prompt surgical repair for best results. The surgeon makes an incision over the front of your knee to access the torn tendon. The torn ends are identified and prepared for repair.
Strong sutures reattach the tendon to the kneecap or tibia, depending on where the tear occurred. For tears at the bone attachment site, the surgeon may drill small holes in the bone and thread sutures through these holes to secure the tendon.
Surgery timing significantly impacts outcomes. Acute tears repaired within a few weeks of injury typically heal better than chronic tears. Delayed repairs face challenges because the tendon may retract and become scarred, making reattachment more difficult.
Tendinopathy Surgery
Chronic tendinopathy sometimes requires surgery when months of conservative treatment fail. The procedure removes degenerated tissue and stimulates healing in the remaining healthy tendon.
Some surgeons use minimally invasive techniques with small incisions and specialized instruments. Others perform open procedures that allow direct visualization and thorough tissue debridement. Your surgeon recommends the approach best suited to your specific condition.
Expert Surgical & Conservative Care
Our experienced orthopedic team offers comprehensive patellar tendon treatment, from advanced physical therapy programs to state-of-the-art surgical techniques. We’ll create a customized treatment plan based on your injury severity and lifestyle goals.
Recovery Timeline and Rehabilitation Process
Recovery duration varies significantly based on injury severity and treatment method. Understanding typical timelines helps you set realistic expectations and stay motivated throughout rehabilitation.
Non-Surgical Recovery Timeline
Mild patellar tendinitis often improves within six to twelve weeks with proper treatment. You may notice reduced pain within the first few weeks, but tissue healing requires more time. Returning to high-impact activities too quickly commonly causes symptom recurrence.
Moderate to severe tendinopathy takes longer to resolve. Many people require three to six months of dedicated rehabilitation before returning to full sport participation. Some cases, particularly those involving significant tendon degeneration, may need up to a year of treatment.
Post-Surgical Recovery
Recovery after patellar tendon repair follows a carefully structured protocol. The initial phase focuses on protecting the surgical repair while preventing excessive stiffness.
Immediate Post-Operative Period
You’ll wear a knee brace locked in full extension immediately after surgery. This brace protects the repair during early healing. Most patients use crutches to avoid bearing full weight on the operated leg for several weeks.
During the first two weeks, the focus remains on wound healing and controlling swelling. Gentle ankle and hip exercises maintain circulation and prevent blood clots. You perform quadriceps muscle contractions to minimize muscle atrophy.
Progressive Mobilization Phase
Around two to four weeks after surgery, your surgeon allows gradual knee bending. Physical therapy intensifies during this phase. You work on regaining range of motion through controlled exercises while still protecting the healing tendon.
Weight-bearing progresses according to your surgeon’s protocol. Some patients transition from crutches to a cane, then to independent walking over six to eight weeks. The brace is gradually unlocked to permit more knee motion.
| Recovery Phase | Time Period | Key Milestones | Activities Permitted |
| Protection Phase | 0-6 weeks | Wound healing, swelling control, brace wear | Gentle muscle contractions, limited weight-bearing |
| Motion Phase | 6-12 weeks | Restore knee bending, discontinue brace, full weight-bearing | Walking, stationary cycling, progressive stretching |
| Strengthening Phase | 3-6 months | Rebuild muscle strength, improve endurance | Resistance training, swimming, light jogging |
| Return to Activity | 6-12 months | Sport-specific training, unrestricted activities | Jumping sports, competitive athletics, full participation |
Rehabilitation Exercises
Your rehabilitation program evolves as healing progresses. Each phase builds upon previous gains while introducing new challenges.
Flexibility Work
Maintaining flexibility throughout the leg proves essential. Tight muscles increase stress on the healing tendon and limit functional improvement. Your therapist teaches specific stretches for your quadriceps, hamstrings, hip flexors, and calf muscles.
Hold each stretch for 30 seconds and repeat three to five times. Perform stretching exercises at least twice daily. You should feel a gentle pull but never sharp pain during stretching.
Strength Development
Progressive resistance training rebuilds the muscle strength you lost during the injury period. The quadriceps muscle weakens rapidly when you cannot use your knee normally. Targeted exercises counteract this muscle loss.
Your therapist carefully monitors exercise intensity to challenge your muscles without overstressing the healing tendon. Weight machines, resistance bands, and body weight exercises all play roles in your strengthening program.
Functional Training
As strength improves, exercises become more functional and sport-specific. Balance training on unstable surfaces improves knee stability. Agility drills prepare you for the quick direction changes required in many sports.
Jumping exercises progress gradually from small two-legged hops to full-height single-leg jumps. Your therapist ensures you master proper landing mechanics to reduce re-injury risk when you return to sport.
Return to Activity Criteria
Returning to sports or demanding work requires meeting specific criteria rather than simply waiting a predetermined time. Your doctor and therapist assess several factors before clearing you for full activity.
Signs You’re Ready to Return
- Full knee range of motion compared to uninjured leg
- Strength testing shows at least 90% of uninjured side
- No pain during sport-specific movements
- Successful completion of functional hop tests
- Confidence in your knee during cutting and jumping
Warning Signs to Continue Therapy
- Persistent pain during or after exercise
- Swelling that increases with activity
- Limited knee motion or stiffness
- Significant strength deficit compared to other leg
- Fear or hesitation during jumping movements
Preventing Patellar Tendon Injury
Preventing patellar tendon problems requires addressing multiple risk factors simultaneously. Athletes and active individuals benefit from implementing comprehensive prevention strategies.
Training Modifications
Smart training progression prevents overuse injuries. The ten percent rule provides useful guidance: avoid increasing your training volume by more than ten percent per week. This applies to running mileage, jumping repetitions, and overall workout intensity.
Adequate recovery between intense training sessions allows tendons to adapt to stress. Schedule rest days or easy training days after high-intensity workouts. Listen to your body and reduce training if you develop persistent knee soreness.
Surface Considerations
Training surface impacts the stress your tendons experience. Hard surfaces like concrete create more impact force than softer options. When possible, choose grass, tracks, or cushioned gym floors for high-impact activities.
Varying your training surfaces also helps. Running exclusively on the same surface can create repetitive stress patterns. Mix road running with trail running or track work to distribute forces differently.
Strength and Flexibility Programs
Balanced lower extremity strength reduces injury risk. Your quadriceps, hamstrings, hip muscles, and core all contribute to proper movement mechanics. Weakness in any area can increase patellar tendon stress.
Eccentric strengthening deserves special attention for tendon health. Exercises that emphasize the lowering phase of movements build tendon resilience. Eccentric squats, step-downs, and controlled jumping progressions all provide these benefits.
Essential Stretches
- Standing quadriceps stretch
- Hamstring stretches (seated or standing)
- Hip flexor lunges
- Calf stretches against wall
- IT band foam rolling
Strengthening Exercises
- Single-leg squats
- Step-ups and step-downs
- Leg press variations
- Nordic hamstring curls
- Hip abductor exercises
Balance Training
- Single-leg standing holds
- Wobble board exercises
- BOSU ball activities
- Dynamic balance drills
- Eyes-closed balance challenges
Equipment and Footwear
Proper footwear provides crucial support during athletic activities. Running shoes should match your foot type and gait pattern. Replace athletic shoes every 300 to 500 miles of use, as cushioning deteriorates over time.
Sport-specific shoes offer features designed for particular movement patterns. Basketball shoes provide ankle support and cushioning for jumping. Court shoes for volleyball or tennis support lateral movements. Using appropriate footwear for your activity reduces injury risk.
Some athletes benefit from custom orthotics or over-the-counter arch supports. These devices can correct biomechanical problems that increase tendon stress. A sports medicine professional can assess whether orthotics might help you.
Warm-Up and Cool-Down Routines
Never skip warm-up before intense activity. A proper warm-up increases blood flow to muscles and tendons, improving tissue elasticity. Start with five to ten minutes of light cardiovascular activity like jogging or cycling.
Dynamic stretching works better than static stretching before activity. Leg swings, walking lunges, and high knees prepare your body for athletic movements. Save static stretching for your cool-down period.
Cool down with light activity and stretching after workouts. This practice helps clear metabolic waste products and maintains flexibility. Spend ten to fifteen minutes on cool-down activities.
Quick Prevention Checklist
- Progress training volume gradually (10% rule)
- Include adequate rest days in your schedule
- Maintain balanced strength in all leg muscles
- Perform regular flexibility work
- Wear appropriate, well-maintained footwear
- Always warm up before intense activity
- Address minor pain promptly before it worsens
When to Seek Medical Attention
Knowing when to consult a healthcare professional can prevent minor problems from becoming serious injuries. Certain symptoms warrant prompt medical evaluation.
Emergency Situations
Seek immediate medical care if you experience sudden, severe knee pain accompanied by inability to straighten your leg. These symptoms suggest possible tendon rupture requiring urgent evaluation.
A popping sensation followed by immediate loss of function also demands prompt attention. The sooner a complete tear gets diagnosed and treated, the better your recovery prospects become.
Rapid swelling within the first few hours after injury sometimes indicates severe damage. While not every swollen knee represents an emergency, significant swelling warrants same-day evaluation.
Non-Emergency Medical Consultation
Schedule an appointment with your doctor if knee pain persists beyond a few weeks despite rest and home treatment. Continuing to exercise through persistent pain risks converting a minor problem into chronic tendinopathy.
Pain that progressively worsens over time deserves medical attention. This pattern suggests ongoing tissue damage rather than simple inflammation that should improve with rest.
Any knee pain that interferes with daily activities like climbing stairs or getting up from a chair warrants professional evaluation. You shouldn’t have to significantly modify your lifestyle to accommodate knee pain.
Questions to Ask Your Doctor
- What specific type of patellar tendon injury do I have?
- Will I need imaging tests to confirm the diagnosis?
- Should I completely stop exercising or can I do modified activities?
- What treatment options are available for my condition?
- How long will recovery typically take?
- When should I follow up if symptoms don’t improve?
- What signs would indicate my condition is worsening?
Specialist Referrals
Your primary care doctor may refer you to a specialist for certain situations. Orthopedic surgeons specialize in bone and tendon injuries. They provide expert evaluation and perform surgery when necessary.
Sports medicine physicians focus specifically on athletic injuries. These doctors understand the unique demands athletes place on their bodies and can guide return-to-sport decisions.
Physical therapists play a crucial role in conservative treatment and post-surgical rehabilitation. Many patients benefit from starting therapy early in their treatment course.
Get Expert Care for Your Patellar Tendon Injury
Our orthopedic specialists have extensive experience treating all types of patellar tendon injuries. From initial diagnosis through complete recovery, we provide comprehensive care tailored to your specific needs and goals. Don’t let knee pain sideline you from the activities you love.
Schedule Your Evaluation Today
Take the first step toward recovery by connecting with our experienced orthopedic team. Complete the form below and we’ll contact you within one business day to schedule your comprehensive knee evaluation.
Taking Control of Your Knee Health
Patellar tendon injury affects people across all activity levels, from elite athletes to weekend exercisers. Understanding the different types of injuries, recognizing symptoms early, and pursuing appropriate treatment dramatically improves your recovery prospects.
Whether you’re dealing with early-stage tendinitis or recovering from surgical tendon repair, following your treatment plan consistently gives you the best chance of returning to full activity. Physical therapy plays a vital role in nearly every treatment approach, rebuilding the strength and function your knee needs.
Prevention strategies help protect against future injury once you’ve recovered. Smart training progressions, balanced strength development, and proper equipment choices reduce your risk of recurrence. Many athletes return to their sports stronger than before their injury when they commit to comprehensive rehabilitation and prevention programs.
Don’t ignore persistent knee pain or sudden loss of function. Early intervention prevents minor problems from becoming chronic conditions requiring more extensive treatment. Your knee health impacts your quality of life, mobility, and ability to enjoy the activities you love. Taking action now protects your long-term function and keeps you active for years to come.
Key Takeaways
- Patellar tendon injuries range from mild tendinitis to complete rupture
- Early symptoms include pain below the kneecap that worsens with activity
- Complete tears require prompt surgical repair for best outcomes
- Conservative treatment with physical therapy successfully treats most tendinitis cases
- Recovery timelines vary from weeks to months depending on injury severity
- Prevention through proper training and strengthening reduces future injury risk
- Seek medical evaluation for persistent pain or sudden loss of knee function







