To prevent future fractures, you will likely need to learn new ways to perform daily life tasks. Things like sweeping and carrying groceries can break a bone if not done mindfully. Good alignment is the key to safe movement. Aligning your head, shoulders, spine, hips, knees and ankles improves balance and centers the weight on your legs. Certain postures and movements are dangerous for people with fragile spines. These include: slouching; forward bending and twisting; movements that are abrupt or jerky; and lifting heavy objects, either from the floor or from above. You can find more information about safe exercise in BHOF’s Boning Up on Osteoporosis booklet, available on the BHOF website.
What exercises should be avoided?
Staying active is imperative for good health and longevity. However, for people with VCFs or osteoporosis, some exercises may do more harm than good. If you have low bone density, osteoporosis, or curvature of the spine, you should avoid exercises that require you to bend forward at the waist, such as:
• Sit-ups
• Abdominal (stomach) crunches. • Toe touches
• Squats
If you have one or more VCFs, you may need to make changes to your recreational activities. Yoga, pilates, tennis and golf require twisting and bending movements that can overload the weakened spine. If you have VCFs, it’s also a good idea to avoid anything that could result in a fall, a hard bump, a quick stop, or a severe twist. Horse riding, ice hockey and gymnastics would probably no longer be possible. On the other hand, golf can be great if you make the right changes to your swing. Work with a physical therapist or trainer to ensure spinal safety.
Why is preventing falls so important?
Falls are the leading cause of bone fractures in the elderly. If you prevent falls, you will prevent most fractures. There are many factors that contribute to falls in the elderly. These include poor vision, balance problems, weak legs, dizziness and slow reflexes. Much can be done to reduce the risk of falls. Keep your glasses prescription up to date. Work with your physical therapist on muscle strengthening and balance training. Tell your doctor right away if you feel dizzy. Dizziness is a common side effect of many medications and diseases. Stay as active as possible to build endurance and agility.
Homes and workplaces can be made safer. Take an inventory of your environment. Remove loose carpets, slippery surfaces and tripping hazards. Make sure there are grab bars in your bathroom and strong handrails on your stairs. Provide brighter light, especially outdoors and in stairwells. Professional home security experts can help you assess, select, and install all necessary features.
What can be done for severe VCF pain?
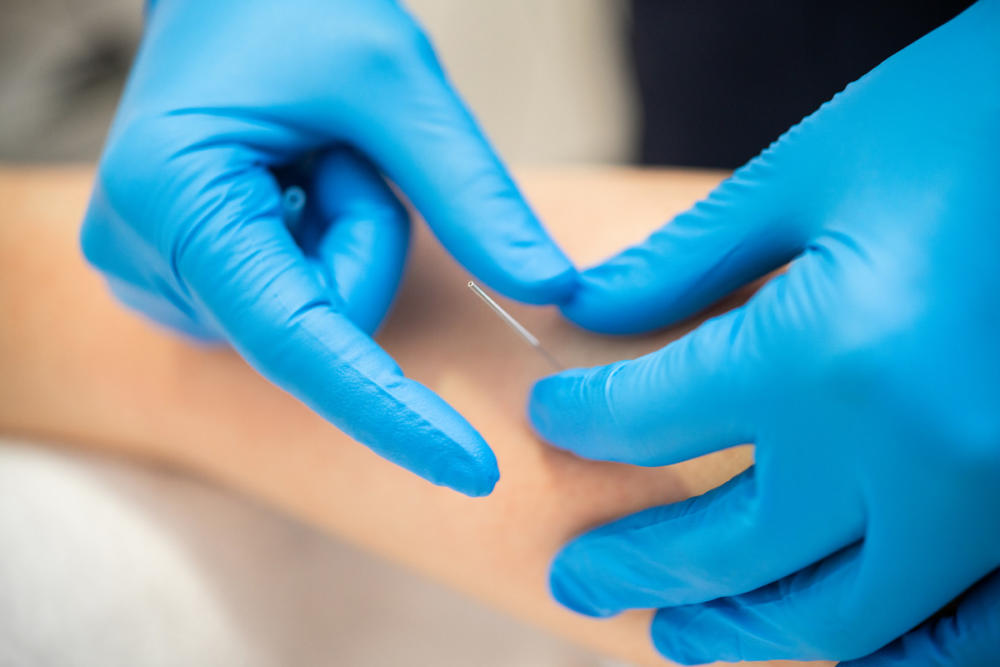
Most patients with VCF feel better after a few weeks of rest, braces and painkillers. However, some VCFs cause extreme pain that persists. In these cases, there are options to consider. You may be able to achieve better pain control by working with a doctor who specializes in pain management. You can get relief from a combination of medications and physical treatments such as acupuncture or massage. Sometimes a VCF is still unbearably painful after a month of rest, medication and physiotherapy. Your doctor may refer you for further testing. In some cases, surgery may be recommended.
When a vertebral bone is broken, bone fragments can rub against each other, causing severe pain
pain. Preventing these fragments from moving usually relieves the pain. A surgery called vertebral augmentation is designed to do just that. A spinal augmentation is called a “minimally invasive” operation because it involves relatively less operating time and less recovery time. Unlike major surgery, only one or two small openings in the skin are required. Bone cement is injected into the fractured vertebra through a needle. Once the cement hardens, the bone fragments are cemented into place.
There are two types of vertebral augmentation: vertebroplasty and kyphoplasty. Both use bone cement to stabilize broken vertebral bone. The difference is that in kyphoplasty the crushed vertebra is expanded using a balloon. This creates more space for cement and pushes the bone upward, returning it to its more natural shape.
Spinal enlargement is reimbursed by many health insurers; However, you will need to confirm this with your specific insurance company.
Resume
A strong adult skeleton starts in childhood with optimal diet, exercise and sunshine. Even if you don’t reach your full skeletal potential, fractures can be prevented. Universal recommendations for bone health include adequate vitamin D and calcium, exercise, and avoiding smoking and excessive alcohol intake. Additional fracture prevention measures may be necessary. If you have a history of fractures, have a family history of fragility, or have been diagnosed with osteoporosis, you and your healthcare provider should discuss options for effective fracture treatment.
Traditional first-line management for VCF focuses on bed rest, bracing, and pain management. Although this is effective for most patients, pain persists in some patients. For individuals who experience severe pain after four to six weeks of conservative treatment, minimally invasive spinal augmentation may offer hope for improvement.
For more information, please visit the BHOF website: www.bonehealthandosteoporosis.org. There you’ll find newsletters, exercise and safe exercise guides, fracture medications, access to support groups, and more.
click here to download the PDF version of this article.