Knee Replacement Nerve Damage in New York
Introduction
Knee replacement surgery has become an increasingly common procedure, offering hope and relief to countless individuals suffering from debilitating knee pain and reduced mobility. For residents of New York, where an active lifestyle is often the norm, the promise of regained independence through this surgery is particularly appealing. However, as with any major medical procedure, knee replacement surgery comes with its own set of risks and potential complications. One of the most concerning of these is nerve damage.
In this comprehensive guide, we’ll delve deep into the world of knee replacement surgery and the associated risk of nerve damage. We’ll explore the intricacies of the procedure, the potential causes of nerve complications, and the various symptoms that may indicate nerve damage has occurred. Moreover, we’ll provide valuable insights into diagnosis, treatment options, and long-term management strategies specifically tailored for New Yorkers.
Whether you’re considering knee replacement surgery, recovering from a recent procedure, or simply seeking to educate yourself on the topic, this post will serve as an essential resource. Let’s embark on this journey to understand and navigate the challenges of nerve damage following knee replacement surgery in the bustling metropolis of New York.
Section 1: Overview of Knee Replacement Surgery
Knee replacement surgery, medically termed as knee arthroplasty, is a sophisticated orthopedic procedure designed to replace damaged parts of the knee joint with artificial components. This surgical intervention is typically recommended when conservative treatments fail to alleviate severe pain and disability caused by conditions such as osteoarthritis, rheumatoid arthritis, or significant knee injuries.
The Rising Trend in New York
In recent years, New York has witnessed a substantial increase in the number of knee replacement surgeries performed. This uptick can be attributed to several factors:
- Aging Population: As the baby boomer generation enters their senior years, the demand for joint replacement surgeries has surged.
- Increased Prevalence of Joint Disorders: Sedentary lifestyles and obesity contribute to a higher incidence of joint problems.
- Advancements in Surgical Techniques: Improved procedures have made knee replacements more accessible and appealing to a broader range of patients.
Types of Knee Replacement Surgeries
There are several types of knee replacement surgeries, each catering to specific patient needs:
- Total Knee Replacement (TKR)
- The most common type
- Involves replacing the entire knee joint
- Suitable for patients with widespread knee damage
- Partial Knee Replacement (PKR)
- Replaces only one part of the knee joint
- Less invasive than TKR
- Ideal for patients with localized knee damage
- Revision Knee Replacement
- Performed to replace a previous knee implant
- More complex than initial knee replacement surgeries
(Insert an illustrative image showing the types of knee replacement surgeries here)
The Procedure
A typical knee replacement surgery involves the following steps:
- Preparation: The patient is administered anesthesia, and the surgical site is cleaned and prepared.
- Incision: The surgeon makes an incision over the knee to access the joint.
- Removal of Damaged Bone: Damaged cartilage and bone are carefully removed.
- Placement of Implants: Artificial components are placed to replicate the natural knee joint.
- Closure: The incision is closed with sutures or staples, and a sterile dressing is applied.
While knee replacement surgeries boast high success rates, it’s crucial to understand that, like all surgical procedures, they come with inherent risks. One of the most significant concerns is the potential for nerve damage, which we will explore in detail in the following sections.
Section 2: Causes of Nerve Damage in Knee Replacement
Understanding the potential causes of nerve damage during knee replacement surgery is crucial for both patients and healthcare providers. This knowledge can help in taking preventive measures and making informed decisions. Let’s delve into the various factors that can lead to nerve complications:
Surgical Factors
- Intraoperative Nerve Injury
- Direct trauma: Nerves can be accidentally cut, stretched, or compressed during the surgical procedure.
- Thermal injury: Use of high-speed drills or cement can cause localized heat damage to nearby nerves.
- Postoperative Swelling
- Edema: Excessive swelling after surgery can compress nerves, leading to temporary or permanent damage.
- Hematoma formation: Blood accumulation can put pressure on surrounding nerves.
- Tourniquet Use
- Ischemia: Prolonged use of a tourniquet during surgery can lead to oxygen deprivation in nerves.
- Reperfusion injury: When blood flow is restored after tourniquet removal, it can cause additional damage to nerve tissues.
### Patient-Specific Factors
- Pre-Existing Conditions
- Diabetes: Patients with diabetes are at higher risk due to pre-existing neuropathy.
- Peripheral neuropathy: Any pre-existing nerve condition increases vulnerability to further damage.
- Obesity
- Increased surgical difficulty: Excess weight can make the procedure more challenging, potentially increasing the risk of nerve injury.
- Postoperative complications: Obese patients may face a higher risk of swelling and slower healing.
- Age
- Decreased nerve resilience: Older patients may have less robust nerves, making them more susceptible to damage.
- Smoking
- Impaired healing: Smokers often experience slower healing, which can exacerbate nerve-related issues.
Anatomical Considerations
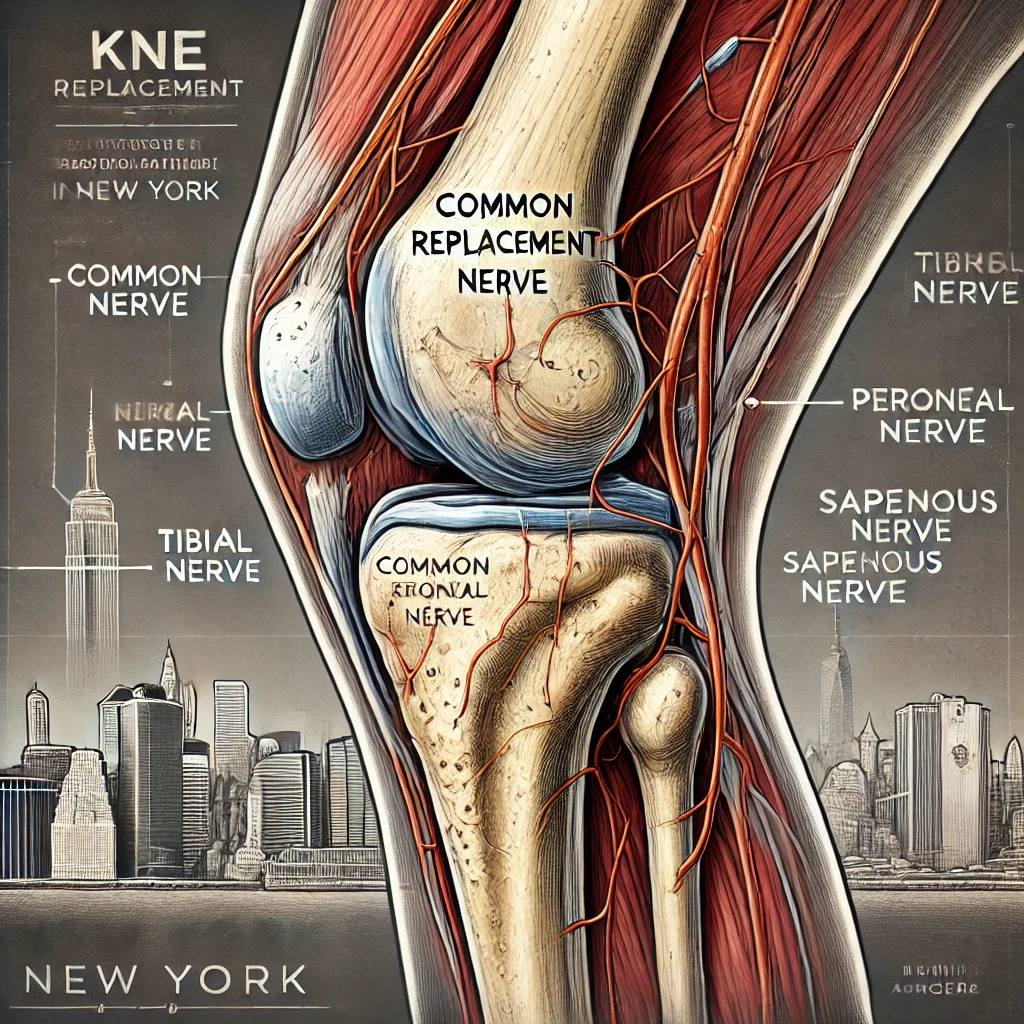
The knee joint is surrounded by several important nerves, each at risk during surgery:
- Common Peroneal Nerve
- Location: Passes around the head of the fibula
- Risk: Particularly vulnerable due to its superficial position
- Tibial Nerve
- Location: Runs through the popliteal fossa behind the knee
- Risk: Can be affected during posterior approaches to the knee
- Saphenous Nerve
- Location: Runs along the medial aspect of the knee
- Risk: May be damaged during medial incisions
(Include a diagram or image showing the anatomy of knee nerves here)
Risk Factors: A Comparative View
To better understand the relative impact of various risk factors, consider the following table:
| Risk Factor | Relative Risk | Preventive Measures |
|---|---|---|
| Diabetes | High | Strict glycemic control pre and post-surgery |
| Obesity | Moderate to High | Weight management, physical therapy |
| Smoking | Moderate | Smoking cessation programs |
| Age (>70 years) | Moderate | Careful patient selection, tailored surgical approach |
| Pre-existing neuropathy | High | Thorough pre-operative assessment, nerve-sparing techniques |
Understanding these risk factors is crucial for both patients and surgeons in New York. It allows for better pre-operative planning, informed consent discussions, and the implementation of preventive strategies to minimize the risk of nerve damage during knee replacement surgery.
Section 3: Symptoms of Nerve Damage Post-Knee Replacement
Recognizing the symptoms of nerve damage early is crucial for prompt intervention and better outcomes. For New Yorkers who have undergone knee replacement surgery, being aware of these signs can make a significant difference in their recovery journey. Let’s explore the various symptoms that may indicate nerve damage:
Common Symptoms
- Numbness and Tingling
- Description: A pins-and-needles sensation or loss of feeling in the affected area
- Location: Often experienced in the lower leg, foot, or toes
- Onset: Can occur immediately after surgery or develop gradually
- Burning Sensation
- Description: A persistent burning feeling, often described as “on fire”
- Location: Typically around the knee, extending down the leg
- Intensity: Can range from mild to severe, often worsening at night
- Sharp, Shooting Pain
- Description: Sudden, intense pain that may feel like an electric shock
- Pattern: Often radiates down the leg following the path of the affected nerve
- Triggers: Can be spontaneous or triggered by specific movements
- Weakness or Paralysis
- Description: Difficulty moving certain muscles or complete loss of muscle function
- Severity: Can range from mild weakness to complete paralysis
- Impact: May affect walking, standing, or specific leg movements
- Hypersensitivity
- Description: Increased sensitivity to touch or temperature changes
- Manifestation: Even light touch or slight temperature variations can cause discomfort
- Area: Usually localized to the skin around the knee or lower leg
Symptom Progression
It’s important to note that symptoms can evolve over time:
- Immediate Post-Surgery: Numbness or tingling is common and often temporary
- Days to Weeks Post-Surgery: Persistent or worsening symptoms may indicate nerve damage
- Months Post-Surgery: Chronic symptoms suggest long-term nerve complications
Symptom Severity Scale
To help patients and healthcare providers assess the severity of nerve damage symptoms, consider the following scale:
| Severity Level | Description | Action Required |
|---|---|---|
| Mild | Occasional numbness or tingling, minimal impact on daily activities | Monitor and report to surgeon at next follow-up |
| Moderate | Persistent symptoms, some impact on mobility or sleep | Schedule an earlier appointment with your |