Are you experiencing sudden pain and swelling behind your knee? Could it be due to a ruptured Baker’s cyst? A Baker’s cyst can cause significant discomfort and limit mobility. Understanding how to manage its rupture at home is crucial for relief and recovery.
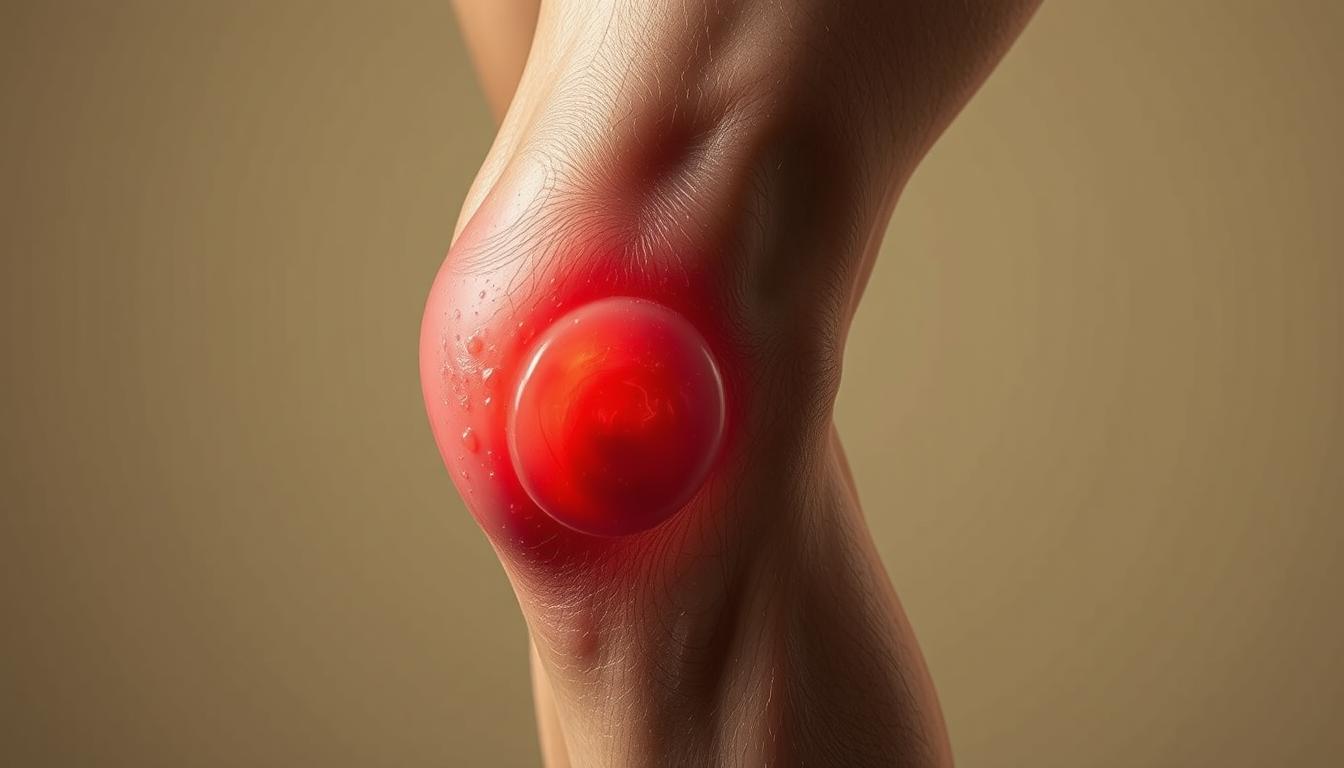
A Baker’s cyst is a fluid-filled swelling that causes a bulge and a feeling of tightness behind your knee. It might be related to an underlying condition such as arthritis, as noted on WebMD. Effective home care can help alleviate the symptoms.
Key Takeaways
- Rest and elevate your leg to reduce swelling.
- Apply a cold pack to ease pain and inflammation.
- Use compression wraps to help reduce swelling.
- Over-the-counter medication can help manage pain.
- Avoid activities that may have caused the cyst.
Understanding Baker’s Cyst and Its Rupture
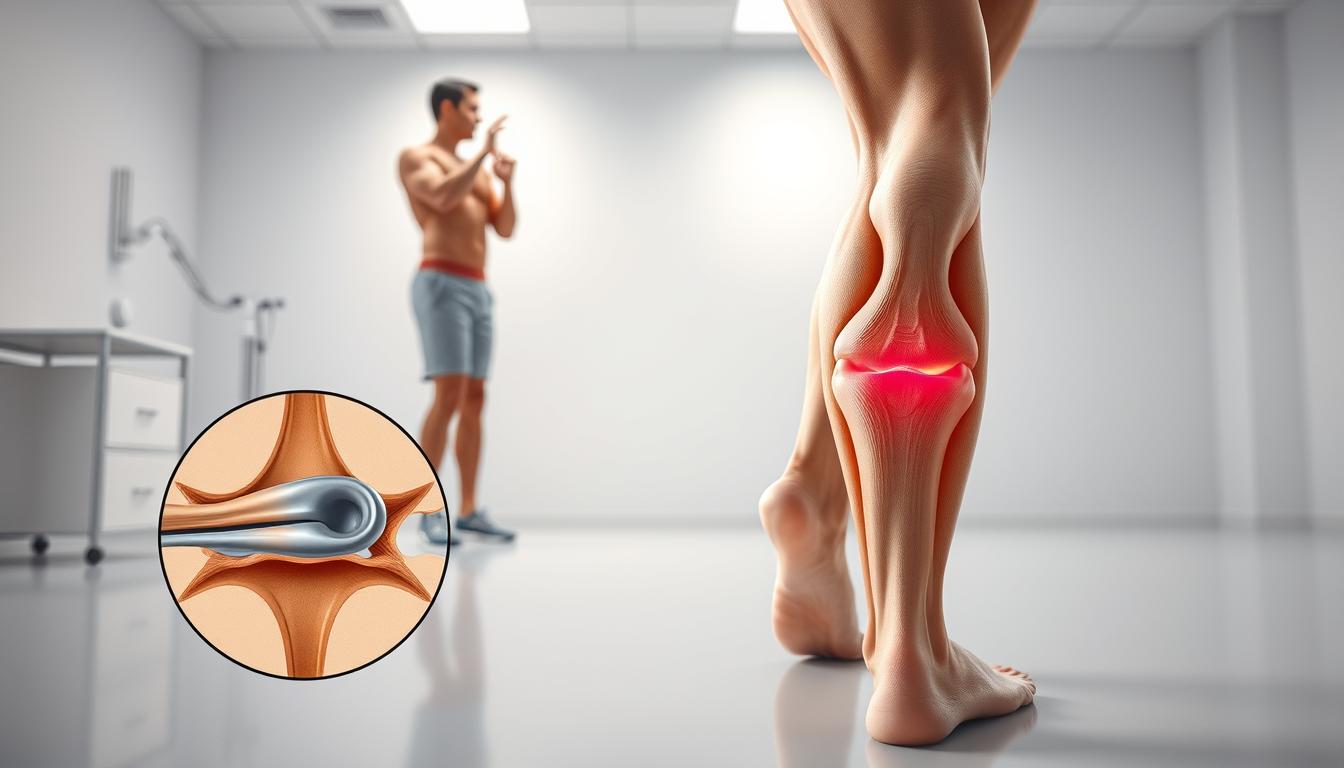
Behind the knee, a Baker’s cyst can develop, leading to pain and swelling due to the accumulation of synovial fluid. This condition is characterized by a fluid-filled lump and can significantly impact one’s quality of life if not properly managed.
What Is a Baker’s Cyst?
A Baker’s cyst is essentially a fluid-filled lump that forms behind the knee due to the overproduction of synovial fluid, which is the fluid that lubricates the knee joint. This overproduction can be a result of various factors, including knee injuries or conditions like arthritis.
Common Symptoms of Baker’s Cyst
The symptoms of a Baker’s cyst can vary but commonly include pain and swelling behind the knee, stiffness, and limited mobility of the knee joint. In some cases, the cyst may not cause any symptoms at all.
Causes of Baker’s Cyst Rupture
A Baker’s cyst can rupture, leading to sharp knee pain and swelling in the calf. The rupture is often caused by the cyst becoming too full of fluid, leading to increased pressure until it bursts.
| Symptom/Complication | Description | Potential Outcome |
|---|---|---|
| Pain and Swelling | Pain and swelling behind the knee due to fluid accumulation. | Limited mobility and discomfort. |
| Cyst Rupture | The cyst bursts, releasing fluid into the leg. | Sharp pain, swelling in the calf, and potential for further complications. |
| Stiffness and Limited Mobility | Reduced ability to move the knee joint freely. | Impact on daily activities and quality of life. |
By understanding the causes, symptoms, and potential complications of a Baker’s cyst, individuals can better manage their condition and seek appropriate medical care when necessary.
Immediate Steps After a Rupture
Understanding the immediate steps to take after a Baker’s cyst ruptures can significantly impact the recovery process. A ruptured Baker’s cyst can cause sudden and severe symptoms, which may be alarming and require prompt action.
Recognizing Signs of Rupture
A ruptured Baker’s cyst can manifest through several distinct symptoms. These may include a sudden, sharp pain in the knee or calf area, swelling, and bruising. It’s crucial to recognize these signs to differentiate a ruptured Baker’s cyst from other conditions, such as a blood clot, which may require different treatments.
The pain from a ruptured Baker’s cyst can sometimes be confused with other serious conditions. Therefore, understanding the specific characteristics of the pain and associated symptoms is vital for appropriate self-care.
Initial Home Treatments to Consider
Upon suspecting a Baker’s cyst rupture, several initial home treatments can be considered to alleviate symptoms. Rest is crucial, as it allows the affected area to begin the healing process. Applying ice to the affected area can help reduce pain and swelling.
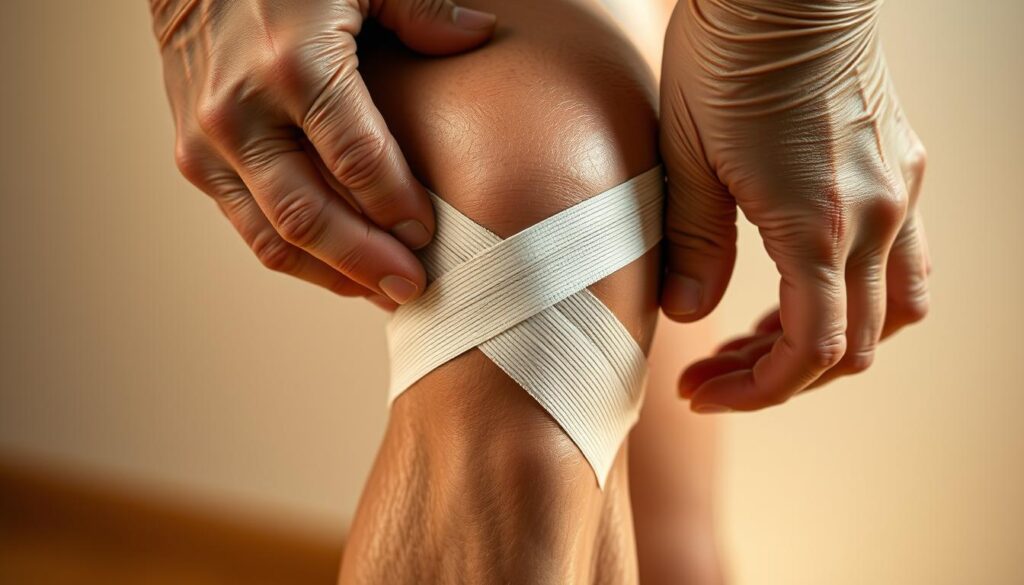
Compression is another effective method. Using a compression bandage can help reduce swelling by constricting the affected area. It’s essential to balance compression with comfort to avoid cutting off circulation.
- Rest the affected leg to prevent further irritation.
- Apply ice to reduce pain and swelling.
- Use compression to minimize swelling.
These initial steps are critical in managing the immediate symptoms of a Baker’s cyst rupture and can be part of an effective self-care for Baker’s cyst rupture strategy.
Pain Management Strategies
Effective pain management strategies are essential for comfort and recovery following a Baker’s cyst rupture. Managing pain is not just about alleviating discomfort; it’s also crucial for regaining mobility and improving the overall quality of life during the recovery period.
Over-the-Counter Pain Relievers
Over-the-counter (OTC) pain relievers are often the first line of defense against pain caused by a Baker’s cyst rupture. Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and naproxen are commonly used to reduce inflammation and alleviate pain. It’s essential to follow the recommended dosage and consult with a healthcare provider before taking any medication, especially if you have a history of stomach ulcers or other health conditions.
“The use of NSAIDs can significantly reduce the pain associated with a Baker’s cyst rupture,” says Dr. John Smith, an orthopedic specialist. “However, it’s crucial to use them judically and under the guidance of a healthcare professional.”
Alternative Pain Management Techniques
For those who prefer not to rely solely on medication or are looking for additional relief, alternative pain management techniques can be beneficial. Chiropractic care, for instance, can help improve joint mobility and reduce pain through spinal manipulation and other manual therapies. Acupuncture is another alternative method that has been shown to provide relief for some individuals by stimulating healing and reducing pain through the insertion of fine needles into specific points on the body.
It’s also worth considering physical therapy as part of a comprehensive pain management plan. A physical therapist can provide exercises tailored to improve knee function and strength, thereby reducing pain and enhancing recovery.
- Apply ice to reduce inflammation
- Use compression bandages to support the knee
- Elevate the affected leg to minimize swelling
By combining these strategies, individuals can develop a robust pain management plan that addresses their specific needs and promotes a smoother recovery.
Rest and Activity Modifications
Recovery from a Baker’s cyst rupture requires a delicate balance between rest and gradual activity resumption. This balance is crucial for healing and preventing further injury.
Importance of Resting
Resting the affected knee is vital after a Baker’s cyst rupture. Adequate rest allows the body to heal the cyst and reduces the risk of further inflammation. “Rest is fundamental to the recovery process,” as it enables the body to repair damaged tissues.
Avoid activities that exacerbate the condition, such as heavy lifting, bending, or strenuous exercises. Instead, focus on gentle movements that promote blood flow without putting excessive strain on the knee.

When to Gradually Resume Activities
As the pain subsides and mobility improves, it’s essential to gradually introduce activities to regain strength and flexibility. Start with low-impact exercises like cycling or swimming, which are easier on the knee joint.
It’s crucial to listen to your body and not rush the recovery process.
“Patience is key when recovering from a Baker’s cyst rupture, as premature return to strenuous activities can lead to re-injury.”
Gradually increasing activity levels helps in achieving a full recovery.
- Monitor your body’s response to increased activity.
- Adjust your activities based on pain levels.
- Consult a healthcare professional if you experience increased pain or discomfort.
Ice Therapy for Reduced Inflammation
Reducing inflammation is key to caring for a Baker’s cyst rupture at home, and applying ice is a recommended self-care technique. Ice therapy, also known as cryotherapy, is a simple and effective method for minimizing swelling and alleviating pain.
Benefits of Applying Ice
Applying ice to the affected area has several benefits. It helps in reducing inflammation by constricting blood vessels, numbs the pain, and decreases the metabolic rate, thereby limiting the extent of the injury. Regular application of ice can significantly improve the recovery process.
How to Properly Apply Ice
To apply ice therapy effectively, it’s essential to follow the correct procedure. Wrap ice packs or a bag of frozen peas in a towel to avoid direct contact with the skin, which can cause ice burn. Apply the ice pack to the affected area for 15-20 minutes, with a minimum of 30 minutes between applications. This cycle can be repeated several times a day as needed.
For more detailed information on managing a ruptured Baker’s cyst, you can visit Healthline’s guide on ruptured Baker’s cyst, which provides comprehensive insights into the condition and its management.
| Application Method | Duration | Frequency |
|---|---|---|
| Ice pack wrapped in a towel | 15-20 minutes | Every 2-3 hours |
| Frozen peas bag wrapped in a towel | 15-20 minutes | Every 2-3 hours |
Compression Techniques
After a Baker’s cyst ruptures, employing the right compression methods can significantly aid in the healing process. Compression helps reduce swelling by restricting the flow of fluid into the affected area, thereby alleviating pain and discomfort.
There are several ways to apply compression, with the most common methods involving the use of compression bandages and garments. These tools are invaluable for managing swelling and supporting the knee during the recovery period.
Use of Compression Bandages
Compression bandages are a straightforward and effective way to apply pressure to the affected area. They come in various widths and can be adjusted to fit comfortably around the knee. When using compression bandages, it’s essential to ensure they are not too tight, as this can impede circulation. A good rule of thumb is to check that the bandage is snug but still allows for normal blood flow.
Benefits of using compression bandages include:
- Easy to apply and adjust
- Reusable, making them a cost-effective option
- Available in different sizes to accommodate various knee dimensions
Benefits of Compression Garments
Compression garments are another effective option for managing swelling after a Baker’s cyst rupture. These garments are designed to provide graduated compression, meaning they are tighter at the extremities and looser as they move up the limb. This design helps push fluid upwards, towards the heart, reducing swelling and promoting circulation.
Key advantages of compression garments include:
- They provide consistent compression, which can be more reliable than bandages
- Available in a range of styles and sizes to suit different needs and preferences
- Can be worn discreetly under clothing, making them a convenient option for daily wear
Both compression bandages and garments are valuable tools in the management of a Baker’s cyst rupture. By applying gentle, consistent pressure, they help reduce swelling, alleviate pain, and support the knee during the healing process.
Elevation and Its Importance
One of the simplest yet most effective ways to alleviate symptoms of a ruptured Baker’s cyst is by elevating the affected leg. Elevating the leg helps reduce swelling by improving blood flow and reducing fluid accumulation in the affected area.
Proper Techniques for Elevating the Leg
To properly elevate your leg, you should place it on a pillow or cushion so that it is above the level of your heart. This can be done while lying down or sitting comfortably. It’s essential to ensure that your leg is supported and relaxed to maximize the benefits of elevation.
For optimal results, elevate your leg above the level of your heart for at least 15-20 minutes, several times a day. This can be particularly helpful after activities that exacerbate the condition or in the initial stages following a rupture.
The Impact of Elevation on Swelling
Elevation affects swelling by reducing fluid accumulation and improving circulation. When the leg is elevated, gravity helps reduce blood flow to the affected area, thereby decreasing inflammation and swelling. This simple technique is a valuable component of managing a ruptured Baker’s cyst.
| Technique | Benefits | Frequency |
|---|---|---|
| Elevating the leg above heart level | Reduces swelling, improves circulation | Several times a day, 15-20 minutes |
| Using pillows or cushions for support | Enhances comfort, ensures proper elevation | As needed during rest or relaxation |
For more information on managing knee-related issues, you can visit https://kneehurt.com/knee-hurts-going-up-stairs-not-down/ to understand how certain activities affect knee health.
When to Seek Professional Help
Effective Baker’s cyst rupture home care involves not just self-care but also being aware of the signs that indicate the need for professional medical help. While many cases can be managed at home, certain symptoms and complications necessitate medical evaluation.
It’s crucial to monitor your condition closely and be aware of the signs that indicate a need for medical attention. These signs include:
- Increased pain or swelling that doesn’t improve with home care
- Redness or warmth around the affected area, which could indicate infection
- Significant bruising or discoloration
- Difficulty walking or bearing weight on the affected leg
- Fever or chills, which could be signs of an underlying infection
Signs Indicating a Need for Medical Attention
If you experience any of the above symptoms, it’s essential to seek medical help. A healthcare provider can assess the severity of the rupture and provide appropriate treatment.
Possible Treatment Options from Healthcare Providers
Healthcare providers may offer various treatment options depending on the severity of the Baker’s cyst rupture. These can include:
- Drainage of the cyst to relieve pressure and pain
- Physical therapy to improve knee mobility and strength
- Medications such as corticosteroids to reduce inflammation
- Surgical intervention in some cases to address underlying issues or repair damaged tissues
Understanding these treatment options can help you prepare for a consultation with your healthcare provider and make informed decisions about your care.
Lifestyle Changes to Prevent Recurrence
Making informed lifestyle choices is vital for reducing the risk of Baker’s cyst recurrence and enhancing recovery. After experiencing a Baker’s cyst rupture, it’s crucial to adopt habits that promote knee health and overall well-being.
One of the key lifestyle adjustments involves incorporating exercises that strengthen the muscles around the knee. Strengthening these muscles can help provide better support to the knee joint, reducing the likelihood of another cyst forming.
Exercises to Strengthen Knee Muscles
Engaging in regular exercise can significantly improve knee stability and function. Some beneficial exercises include:
- Straight Leg Raises: This exercise helps strengthen the quadriceps muscles without putting excessive strain on the knee joint.
- Hamstring Curls: Strengthening the hamstrings can help balance the muscle forces around the knee, reducing the risk of cyst recurrence.
- Wall Squats: This exercise is effective for strengthening the quadriceps, hamstrings, and gluteal muscles, all of which are crucial for knee stability.
In addition to exercises, dietary recommendations play a vital role in maintaining joint health and preventing Baker’s cyst recurrence.
Dietary Recommendations for Joint Health
A diet rich in anti-inflammatory foods and nutrients can help reduce inflammation and promote healing. Some dietary recommendations include:
| Nutrient | Food Sources | Benefits |
|---|---|---|
| Omega-3 Fatty Acids | Fatty fish, flaxseeds, chia seeds | Reduces inflammation |
| Antioxidants | Berries, leafy greens, other fruits and vegetables | Protects against oxidative stress |
| Vitamin D | Fortified dairy products, fatty fish, sunlight exposure | Essential for bone health |
By combining these exercises and dietary recommendations, individuals can significantly reduce the risk of Baker’s cyst recurrence and improve their overall knee health.
Long-Term Home Care Tips
After experiencing a Baker’s cyst rupture, continued monitoring of symptoms and self-care is crucial for long-term recovery and prevention of future issues. Effective home care can significantly impact the healing process and overall knee health.
Effective Symptom Monitoring
Regularly checking for signs of swelling, pain, or limited mobility can help identify potential issues early. Keeping a symptom journal can be a useful tool in tracking changes and patterns, allowing for timely adjustments to home care routines.
Strategies for Ongoing Self-Care
Implementing tips for home care after a Baker’s cyst rupture, such as maintaining a healthy weight, engaging in gentle exercises, and using home remedies for Baker’s cyst rupture like ice therapy, can support long-term knee health. Incorporating these habits into daily routines can help prevent future complications and promote overall well-being.
FAQ
What is a Baker’s cyst and how does it rupture?
A Baker’s cyst is a fluid-filled swelling that causes a bulge and a feeling of tightness behind the knee. It can rupture due to various reasons such as overuse, injury, or underlying conditions like arthritis, leading to pain and swelling.
How do I manage a ruptured Baker’s cyst at home?
Managing a ruptured Baker’s cyst at home involves a combination of rest, ice therapy, compression, and elevation. Over-the-counter pain relievers can help alleviate pain and discomfort.
What are the signs that indicate a Baker’s cyst has ruptured?
Signs of a ruptured Baker’s cyst include sudden pain behind the knee, swelling, bruising, and sometimes a feeling of fluid running down the leg. If you experience these symptoms, it’s essential to take immediate action to alleviate discomfort.
Can I use ice therapy for a ruptured Baker’s cyst?
Yes, ice therapy is beneficial in reducing inflammation and pain associated with a ruptured Baker’s cyst. Apply ice packs wrapped in a cloth to the affected area for 15-20 minutes, several times a day.
How can I prevent the recurrence of a Baker’s cyst?
Preventing the recurrence of a Baker’s cyst involves making lifestyle changes such as strengthening the muscles around the knee through exercises, maintaining a healthy weight, and following dietary recommendations that support joint health.
When should I seek medical attention for a ruptured Baker’s cyst?
Seek medical attention if you experience severe pain, significant swelling, difficulty walking, or if the pain and swelling do not improve with home care. Healthcare providers can offer further treatment options and guidance.
Are there any alternative pain management techniques for a ruptured Baker’s cyst?
Yes, alternative pain management techniques include acupuncture, physical therapy, and using topical creams or gels that contain pain-relieving ingredients. These can be used alongside conventional pain relievers.
How long does it take to recover from a ruptured Baker’s cyst?
Recovery time varies depending on the severity of the rupture and individual health. Generally, with proper home care and rest, symptoms can improve within a few weeks, but it’s crucial to continue with self-care strategies to prevent future complications.
Can compression bandages or garments help with a ruptured Baker’s cyst?
Yes, compression bandages or garments can help reduce swelling by applying pressure to the affected area. They are a useful adjunct to other home care strategies like elevation and ice therapy.
What are some long-term home care tips for managing Baker’s cyst?
Long-term home care involves monitoring symptoms, continuing exercises to strengthen the knee, maintaining a healthy lifestyle, and being aware of the signs that may indicate a recurrence or complication, allowing for early intervention.