Introduction
Squatting exercises are fundamental for building strength in the lower body and are a cornerstone of many fitness routines. Whether you’re a seasoned athlete or a fitness enthusiast, squats likely play a crucial role in your workout regimen. However, knee pain after squatting is a common issue that many individuals encounter, potentially hindering progress and causing discomfort in daily activities.
Understanding the causes, symptoms, and remedies for knee pain after squatting is essential for maintaining long-term joint health and improving exercise efficiency. This comprehensive guide will delve into the intricacies of knee pain related to squatting, providing you with the knowledge to prevent injuries and optimize your workouts.
The Importance of Squatting Exercises
Before we dive into the problems associated with squatting, it’s crucial to understand why this exercise is so valuable:
1. **Muscle Engagement**: Squats engage multiple muscle groups simultaneously, including quadriceps, hamstrings, glutes, and calves.
2. **Functional Strength**: The movement mimics everyday actions, improving your ability to perform daily tasks.
3. **Bone Density**: Weight-bearing exercises like squats can help increase bone density, reducing the risk of osteoporosis.
4. **Hormonal Benefits**: Compound exercises like squats can boost the production of growth hormone and testosterone, aiding in muscle growth and overall health.
5. **Versatility**: Squats can be modified to suit various fitness levels and goals, from bodyweight squats to heavy barbell squats.
Given these benefits, it’s clear why squats are often called the “king of exercises.” However, with great power comes great responsibility, and proper execution is crucial to reap these benefits without incurring injuries.
Causes of Knee Pain After Squatting
Understanding the root causes of knee pain after squatting is the first step in prevention and treatment. Let’s explore the primary factors contributing to this issue:
1. Improper Squatting Technique
The most common cause of knee pain after squatting is poor form. Proper squatting technique is essential for distributing weight evenly and preventing undue stress on the knee joints. Common errors include:
– **Knees Extending Beyond Toes**: This places excessive stress on the knee joint.
– **Inward Knee Collapse**: Also known as “valgus collapse,” this misalignment can lead to ligament strain.
– **Insufficient Depth**: Not squatting deep enough can increase shear forces on the knee.
– **Back Not Straight**: A rounded back can lead to uneven weight distribution and knee strain.
2. Overuse and Excessive Training
While consistency is key in fitness, overtraining can lead to knee pain and other injuries. Factors contributing to overuse include:
– **High-frequency training** without adequate rest days
– **Excessive volume** (too many sets and repetitions)
– **Rapid increase in weight** without proper progression
3. Inadequate Warm-up and Cool-down
Neglecting proper warm-up and cool-down routines can leave muscles and joints unprepared for the stress of squatting. This increases the risk of injury and can exacerbate existing issues.
4. Muscle Imbalances and Weakness
Weakness or imbalances in the muscles surrounding the knee can lead to poor alignment during squats. Key muscle groups to consider include:
– Quadriceps
– Hamstrings
– Glutes
– Calves
– Hip abductors and adductors
5. Pre-existing Conditions
Certain pre-existing conditions can make individuals more susceptible to knee pain after squatting:
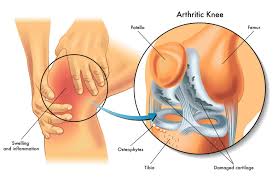
– Osteoarthritis
– Patellofemoral pain syndrome
– Meniscus tears
– Ligament injuries (ACL, MCL, etc.)
6. Equipment and Environment
Sometimes, the problem isn’t with the squatter but with their equipment or environment:
– **Improper footwear**: Shoes without adequate support or stability can affect knee alignment.
– **Uneven surfaces**: Squatting on an unstable or uneven surface can lead to improper form.
– **Incorrect equipment setup**: For barbell squats, improper rack height or bar position can contribute to poor form.
Symptoms of Knee Pain After Squatting
Recognizing the symptoms of knee pain after squatting is crucial for early intervention and prevention of further damage. Common symptoms include:
1. **Sharp or Dull Pain**: This can occur in various parts of the knee, including the front, sides, or back.
2. **Swelling and Inflammation**: Visible swelling or a feeling of warmth around the knee joint.
3. **Limited Range of Motion**: Difficulty in fully bending or straightening the knee.
4. **Instability**: A feeling that the knee might give way during movement.
5. **Clicking or Popping Sounds**: Audible noises during knee movement, often accompanied by pain.
6. **Stiffness**: Especially noticeable after periods of inactivity or upon waking.
7. **Pain When Touching**: Tenderness when applying pressure to specific areas of the knee.
It’s important to note that the severity and combination of these symptoms can vary depending on the underlying cause of the knee pain.
Diagnosis
Proper diagnosis is crucial for effective treatment of knee pain after squatting. Here’s an overview of the diagnostic process:
Self-Assessment
Begin with a self-assessment to gather information about your symptoms:
1. **Pain Scale**: Rate your pain on a scale of 1-10 during and after squatting.
2. **Pain Location**: Identify specific areas of the knee where pain occurs.
3. **Timing**: Note when the pain starts (during the squat, immediately after, or hours later).
4. **Duration**: Track how long the pain lasts after squatting.
5. **Associated Symptoms**: Record any swelling, stiffness, or sounds accompanying the pain.
Professional Diagnosis
If pain persists or worsens, seek a professional diagnosis. A healthcare provider may perform the following:
1. **Physical Examination**: Assessing tenderness, swelling, and range of motion.
2. **Strength Tests**: Evaluating the strength of muscles around the knee.
3. **Imaging Tests**:
– X-rays: To check for bone issues or arthritis
– MRI: For detailed images of soft tissues, including ligaments and cartilage
– CT Scan: If more detailed bone imaging is needed
4. **Arthroscopy**: In some cases, a minimally invasive procedure to directly visualize the inside of the knee joint.
Differential Diagnosis
Your healthcare provider will consider various conditions that can cause knee pain, including:
– Patellofemoral Pain Syndrome
– Meniscus Tears
– Ligament Sprains or Tears
– Osteoarthritis
– Tendinitis
– Bursitis

Treatment
Treatment for knee pain after squatting depends on the underlying cause and severity of the symptoms. Here’s a comprehensive approach to managing and treating knee pain:
1. RICE Method
The RICE method is often the first line of treatment for acute knee pain:
– **Rest**: Avoid activities that exacerbate the pain, including squatting.
– **Ice**: Apply ice for 15-20 minutes every 2-3 hours to reduce inflammation.
– **Compression**: Use an elastic bandage to minimize swelling.
– **Elevation**: Keep the affected leg elevated above heart level when possible.
2. Pain Management
Over-the-counter pain relievers can help manage pain and reduce inflammation:
– **NSAIDs**:(e.g., ibuprofen, naproxen): Reduce pain and inflammation.
– **Acetaminophen**: Provides pain relief without anti-inflammatory effects.
Always consult with a healthcare provider before starting any medication regimen.
3. Physical Therapy
A physical therapist can design a tailored program to address your specific needs:
– **Strengthening exercises**: Target muscles supporting the knee joint.
– **Flexibility exercises**: Improve range of motion and reduce stiffness.
– **Balance training**: Enhance stability and proprioception.
– **Manual therapy**: Hands-on techniques to improve joint mobility.
4. Corrective Exercises
Specific exercises can help address muscle imbalances and improve squatting technique:
– Wall slides
– Glute bridges
– Clamshells
– Single-leg squats
– Step-ups
5. Lifestyle Modifications
Making changes to your daily routine can support recovery:
– **Weight management**: Reducing excess body weight can decrease stress on the knees.
– **Low-impact activities**: Temporarily switch to exercises like swimming or cycling.
– **Proper footwear**: Ensure you’re wearing supportive shoes appropriate for your activities.
6. Advanced Treatments
For more severe or persistent cases, your healthcare provider might recommend:
– **Corticosteroid injections**: To reduce inflammation in the short term.
– **Hyaluronic acid injections**: To improve joint lubrication.
– **Platelet-rich plasma (PRP) therapy**: Uses your own blood components to promote healing.
– **Surgery**: In cases of severe injury or when conservative treatments fail. Options may include arthroscopy, ligament repair, or in rare cases, knee replacement.

Prevention
Preventing knee pain after squatting is always preferable to treating it. Here are comprehensive strategies to keep your knees healthy:
1. Perfect Your Technique
Proper squatting form is crucial for preventing knee pain:
– Keep your feet shoulder-width apart.
– Point your toes slightly outward.
– Keep your chest up and back straight.
– Lower your body as if sitting back into a chair.
– Ensure your knees track in line with your toes.
– Descend until your thighs are parallel to the ground (or as low as you can maintain proper form).
Consider working with a certified fitness professional to refine your technique.
2. Gradual Progression
Avoid increasing weight, sets, or repetitions too quickly:
– Follow the 10% rule: increase your total volume or weight by no more than 10% per week.
– Allow for adequate recovery between squat sessions.
3. Comprehensive Warm-up
A proper warm-up prepares your body for the demands of squatting:
– **Dynamic stretching**: Focus on hip flexors, quadriceps, hamstrings, and calves.
– **Activation exercises**: Include bodyweight squats, lunges, and leg swings.
– **Light cardio**: 5-10 minutes of jogging or jumping jacks to increase blood flow.
4. Strength and Flexibility Training
Develop a well-rounded lower body training program:
– **Strengthen supporting muscles**: Include exercises for quadriceps, hamstrings, glutes, and calves.
– **Core strengthening**: A strong core helps maintain proper form during squats.
– **Flexibility work**: Regular stretching helps maintain joint mobility and muscle flexibility.
5. Cross-training
Incorporate a variety of exercises to prevent overuse:
– **Low-impact activities**: Swimming, cycling, or elliptical training.
– **Unilateral exercises**: Single-leg squats or lunges to address muscle imbalances.
– **Upper body workouts**: Give your legs a break while maintaining overall fitness.
6. Proper Equipment
Ensure you have the right gear for squatting:
– **Supportive shoes**: Choose footwear with a stable base and good arch support.
– **Appropriate surface**: Squat
Certainly, I’ll continue expanding the article on knee pain after squatting exercises.
6. Proper Equipment
Ensure you have the right gear for squatting:
– **Supportive shoes**: Choose footwear with a stable base and good arch support. Avoid running shoes for squatting, as their cushioning can create instability.
– **Appropriate surface**: Squat on a flat, stable surface. Avoid uneven or slippery floors.
– **Assistive devices**: Consider using knee sleeves or wraps for additional support, especially when lifting heavy weights.
7. Nutrition and Hydration
Proper nutrition and hydration play a crucial role in joint health and recovery:
– **Stay hydrated**: Adequate water intake helps maintain synovial fluid in the joints, reducing friction.
– **Anti-inflammatory foods**: Incorporate foods rich in omega-3 fatty acids, such as fish, nuts, and seeds.
– **Collagen support**: Foods high in vitamin C and protein can support collagen production, essential for joint health.
– **Calcium and vitamin D**: Ensure adequate intake to support bone health.
8. Rest and Recovery
Allow sufficient time for your body to recover between workouts:
– **Sleep**: Aim for 7-9 hours of quality sleep per night to support tissue repair.
– **Active recovery**: On rest days, engage in light activities like walking or gentle stretching.
– **Periodization**: Incorporate deload weeks into your training program to prevent overuse.
9. Listen to Your Body
Pay attention to warning signs and adjust your training accordingly:
– **Pain vs. discomfort**: Learn to distinguish between normal muscle soreness and joint pain.
– **Gradual onset**: Address minor discomfort before it develops into significant pain.
– **Modify as needed**: Be willing to adjust your workout if you experience persistent discomfort.
When to Seek Medical Help
While many cases of knee pain after squatting can be managed with self-care and prevention strategies, there are situations where professional medical help is necessary. Consult a healthcare provider if you experience:
1. **Severe pain**: Pain that is intense, sharp, or prevents you from bearing weight on the affected leg.
2. **Persistent pain**: Discomfort that lasts more than a few days or worsens over time.
3. **Significant swelling**: Noticeable swelling that doesn’t subside with rest and ice.
4. **Instability**: A feeling that your knee might give way or inability to support your body weight.
5. **Reduced range of motion**: Difficulty fully bending or straightening your knee.
6. **Locking or catching**: Sensations of your knee locking in place or catching during movement.
7. **Visible deformity**: Any noticeable change in the appearance of your knee.
8. **Signs of infection**: Redness, warmth, fever, or chills accompanying knee pain.
Early intervention can prevent minor issues from developing into more serious conditions and help you return to your fitness routine more quickly.
Long-term Management and Rehabilitation
For those who have experienced knee pain after squatting, long-term management is crucial to prevent recurrence and maintain knee health. Here are strategies for ongoing care and rehabilitation:
1. Gradual Return to Squatting
After addressing the initial pain and its causes, reintroduce squatting exercises gradually:
– **Start with bodyweight**: Begin with unweighted squats to rebuild proper form and confidence.
– **Progressive loading**: Slowly increase weight over several weeks, monitoring for any pain or discomfort.
– **Varied squat types**: Incorporate different squat variations (e.g., box squats, goblet squats) to build overall strength and stability.
2. Ongoing Physical Therapy
Continue working with a physical therapist to:
– **Monitor progress**: Regular check-ins can help catch and address any recurring issues.
– **Advance exercises**: Progressively challenge your knees with more complex movements.
– **Maintain proper biomechanics**: Ensure you’re maintaining good form as you return to regular training.
3. Cross-training for Knee Health
Incorporate exercises that support knee health without the high impact of squatting:
– **Swimming**: Provides excellent cardiovascular benefits while being gentle on the joints.
– **Cycling**: Strengthens leg muscles with less stress on the knees.
– **Pilates**: Improves core strength and overall body alignment.
– **Yoga**: Enhances flexibility and body awareness.
4. Regular Assessments
Schedule periodic assessments with a sports medicine professional or orthopedic specialist:
– **Functional movement screens**: Identify any lingering imbalances or weaknesses.
– **Strength testing**: Ensure that supporting muscles are developing adequately.
– **Gait analysis**: Address any walking or running patterns that may stress the knees.
5. Maintenance Exercises
Incorporate specific exercises into your routine to maintain knee health:
– **Single-leg balance**: Improves proprioception and stability.
– **Hip abductor strengthening**: Supports proper knee alignment during squats.
– **Calf raises**: Enhances lower leg strength and ankle stability.
– **Foam rolling**: Helps maintain muscle flexibility and reduce tension.

6. Mental Health Considerations
Dealing with knee pain and the potential setbacks in your fitness journey can be mentally challenging. Consider these aspects of mental health:
– **Stay positive**: Focus on progress, no matter how small, and celebrate milestones in your recovery.
– **Set realistic goals**: Adjust your fitness expectations to align with your current capabilities.
– **Seek support**: Connect with others who have experienced similar challenges for advice and encouragement.
– **Mindfulness and stress reduction**: Practices like meditation can help manage pain perception and reduce overall stress.
Advanced Considerations for Athletes and Fitness Enthusiasts
For those deeply invested in fitness or competitive sports, additional considerations may be necessary:
1. Sport-Specific Training
Tailor your rehabilitation and prevention strategies to the demands of your specific sport or fitness goals:
– **Plyometric training**: Gradually reintroduce jumping exercises for explosive power.
– **Agility drills**: Incorporate quick direction changes to challenge knee stability.
– **Sport simulation**: Practice movements specific to your sport under controlled conditions.
2. Biomechanical Analysis
Consider undergoing a detailed biomechanical analysis:
– **3D motion capture**: Provides insights into your movement patterns during squats and other exercises.
– **Force plate testing**: Measures the force production and distribution during squatting movements.
– **EMG analysis**: Evaluates muscle activation patterns to identify any imbalances.
3. Nutrition for Joint Health
Work with a sports nutritionist to optimize your diet for joint health and performance:
– **Supplements**: Consider joint-supporting supplements like glucosamine and chondroitin sulfate.
– **Protein intake**: Ensure adequate protein for muscle repair and recovery.
– **Micronutrient balance**: Focus on vitamins and minerals that support joint health, such as vitamin K and magnesium.
4. Recovery Technologies
Explore advanced recovery methods to support knee health:
– **Cryotherapy**: Whole-body or localized cold therapy for reducing inflammation.
– **Compression therapy**: Use of pneumatic compression devices to enhance circulation and reduce swelling.
– **Electrical stimulation**: TENS or NMES units for pain management and muscle activation.
Conclusion
Knee pain after squatting is a common but manageable issue that affects many fitness enthusiasts and athletes. By understanding the causes, implementing proper prevention strategies, and addressing pain promptly and effectively, you can maintain healthy knees and continue to enjoy the benefits of squatting exercises.
Remember that every individual’s journey is unique, and what works for one person may not work for another. Be patient with your body, listen to its signals, and don’t hesitate to seek professional help when needed. With the right approach, you can build strong, resilient knees that support your fitness goals for years to come.
Ultimately, the key to success lies in a holistic approach that combines proper technique, gradual progression, adequate recovery, and ongoing maintenance. By integrating these principles into your fitness routine, you’ll not only reduce the risk of knee pain but also enhance your overall performance and longevity in physical activities.
Stay committed to your knee health, and you’ll be well-equipped to tackle any squatting challenge that comes your way. Happy squatting!