Anterior knee pain is a common condition that can have a significant impact on an individual’s quality of life. Understanding the causes and remedies for anterior knee pain is essential for effective management and treatment. In this article, we will explore the anatomy of the knee joint, the various causes of anterior knee pain, risk factors associated with this condition, methods for diagnosing anterior knee pain, and the treatment options available, including conservative management, physical therapy interventions, and surgical interventions.
Key Takeaways
- Understanding the anatomy of the knee joint is crucial in diagnosing and treating anterior knee pain.
- Identifying the causes of anterior knee pain helps in developing targeted treatment plans.
- Risk factors such as age, gender, and lifestyle can contribute to the development of anterior knee pain.
- Physical examination is a key diagnostic tool for evaluating anterior knee pain.
- Imaging studies such as X-rays and MRI scans are valuable in diagnosing structural abnormalities in the knee joint.
Understanding Anterior Knee Pain
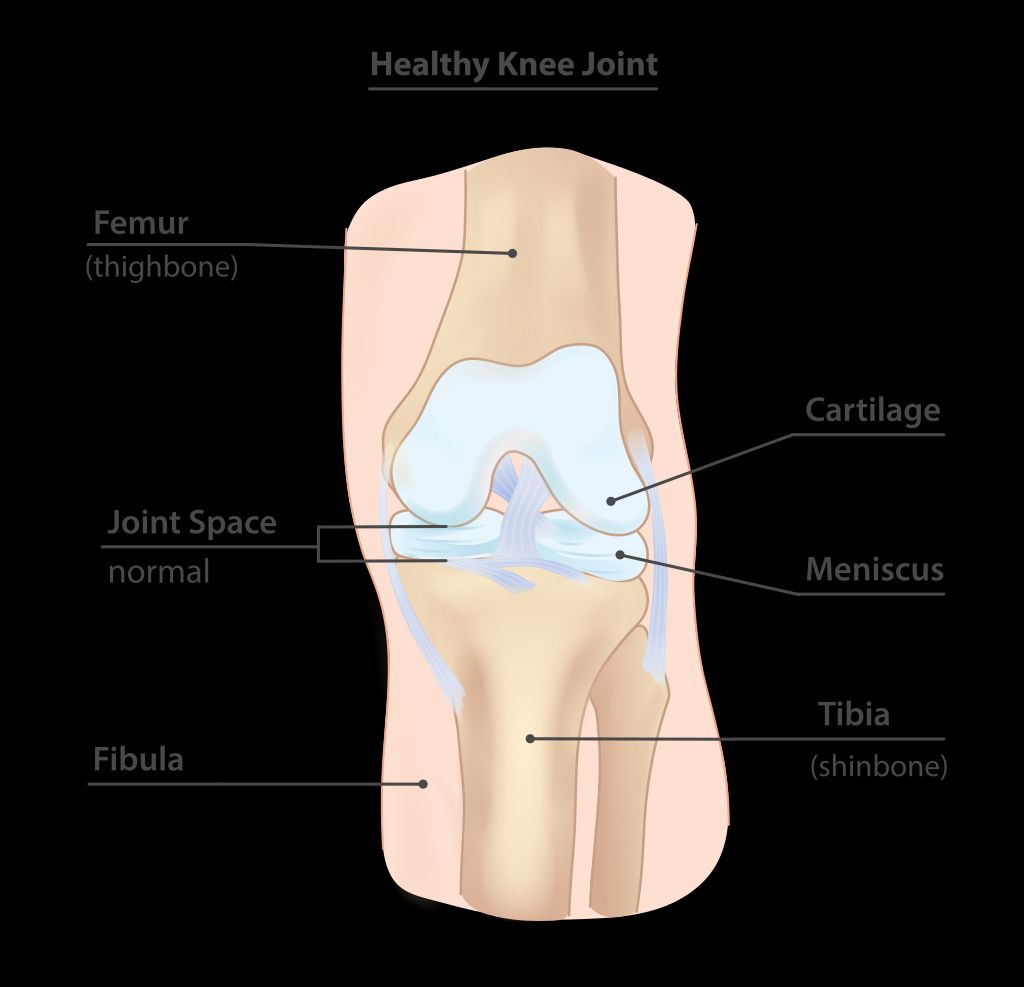
Anatomy of the Knee Joint
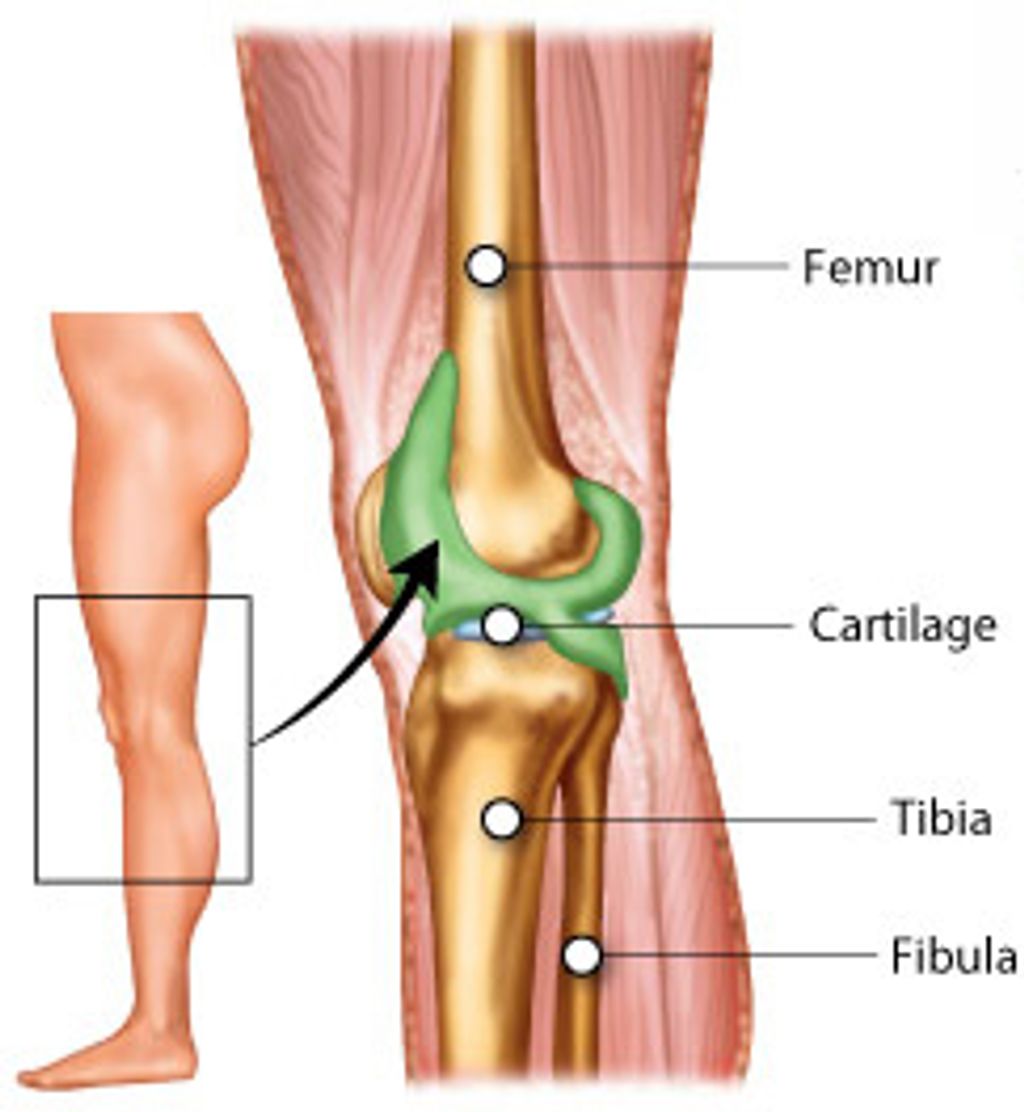
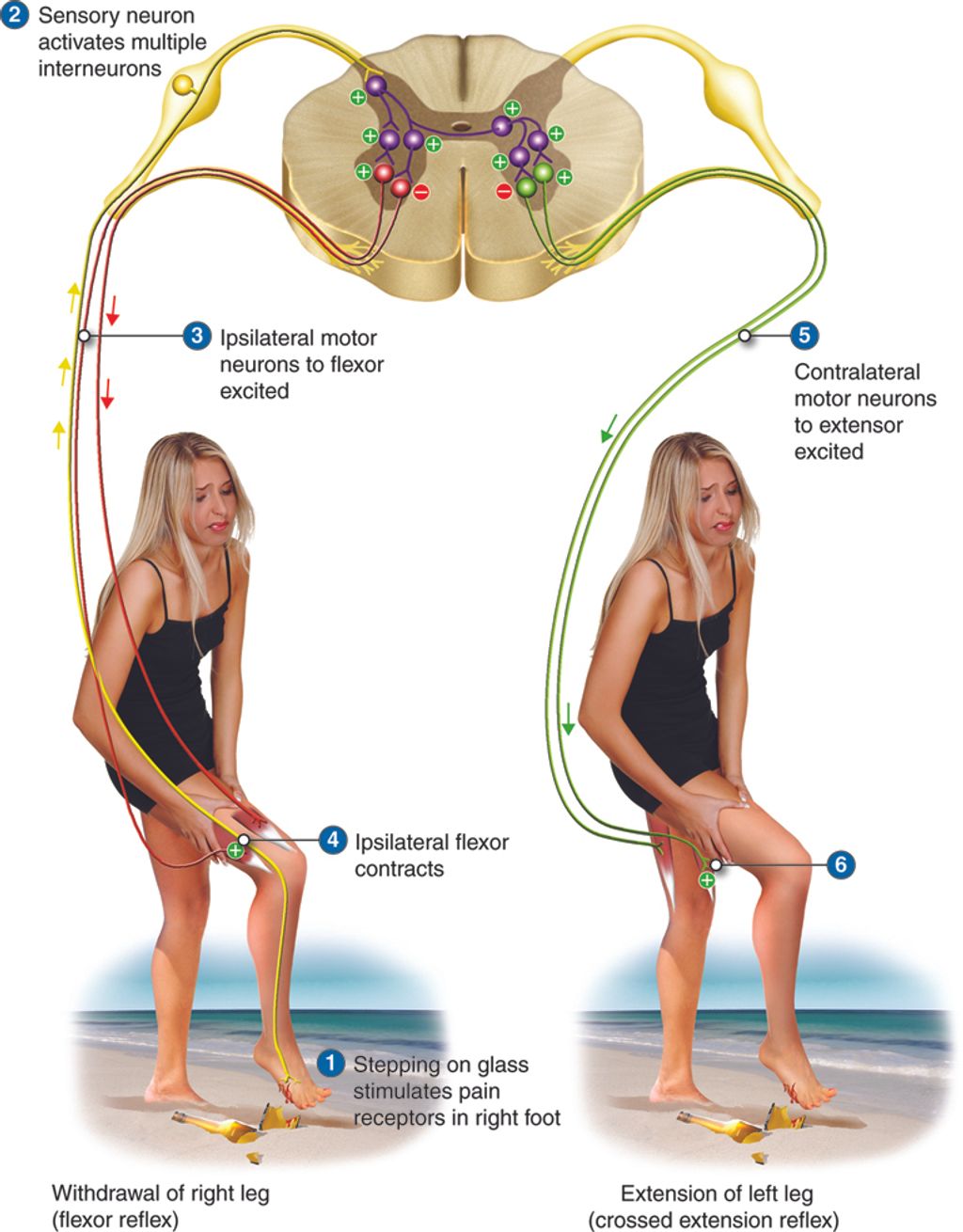
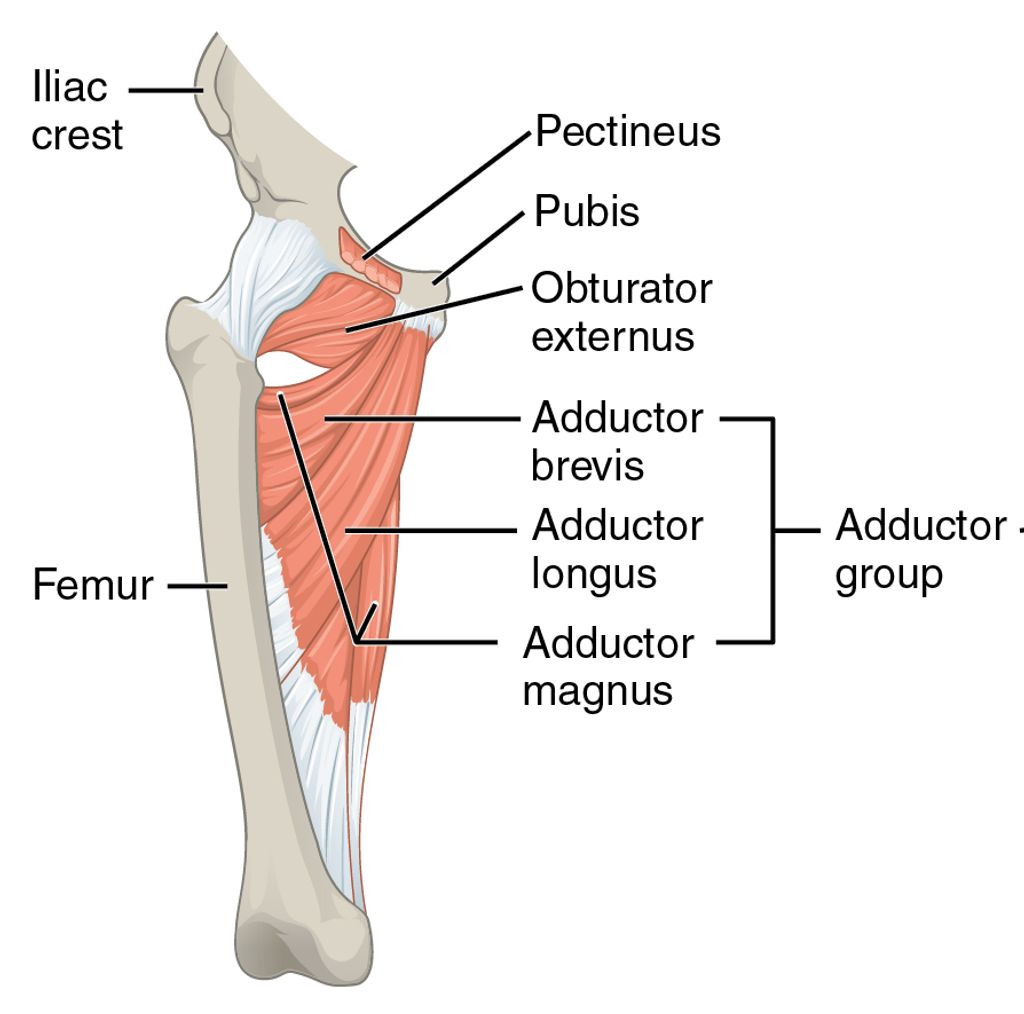
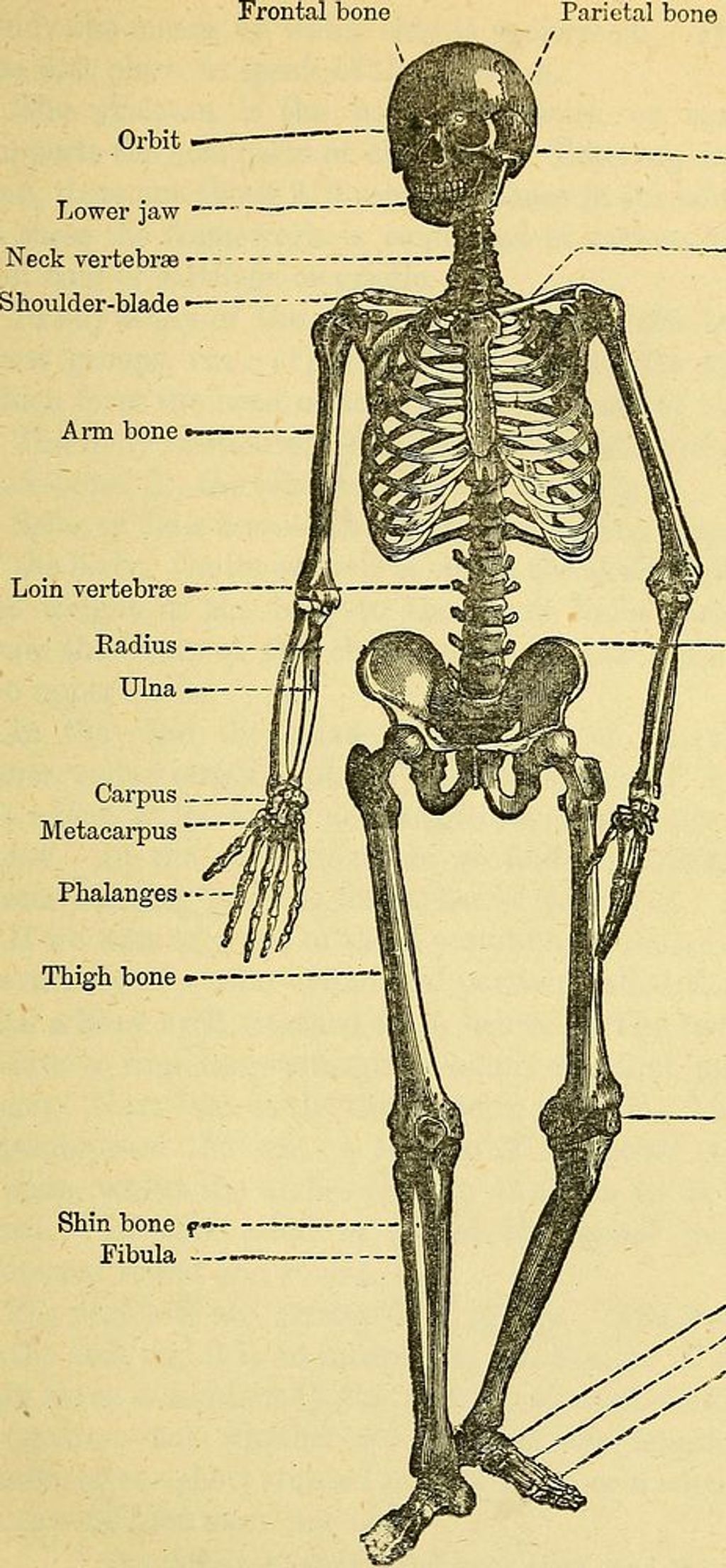
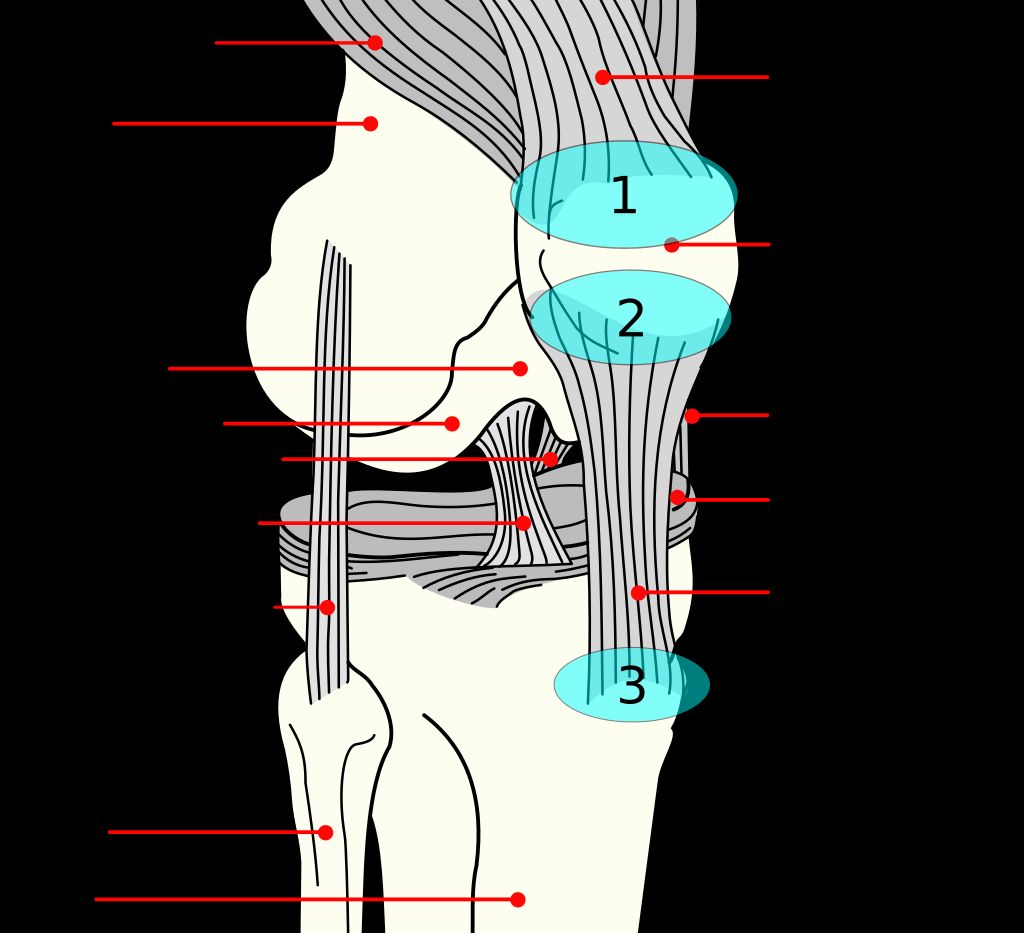
The knee joint is a complex structure that plays a crucial role in supporting our body weight and facilitating movement. Understanding the anatomy of the knee joint is essential for comprehending the mechanisms that can lead to anterior knee pain. The knee joint consists of the femur, tibia, and patella, all of which are connected by ligaments and surrounded by protective cartilage. This intricate arrangement allows for smooth and controlled movement, but it also makes the knee susceptible to various forms of stress and injury.
In some cases, anterior knee pain may be associated with specific anatomical abnormalities, such as patellar malalignment or abnormal tracking. These issues can lead to increased pressure on the patellofemoral joint, resulting in discomfort and reduced function. Understanding these structural variations is crucial for accurate diagnosis and effective treatment.
A key aspect of the knee joint’s anatomy is the distribution of forces during weight-bearing activities. Research has shown that the patellofemoral joint experiences significant pressure during activities like running, jumping, and squatting. This underscores the importance of proper biomechanics and muscle balance in preventing and managing anterior knee pain.
It is important to note that individual variations in knee joint anatomy can influence the development of anterior knee pain. Factors such as patellar shape, alignment, and muscle strength can significantly impact the distribution of forces within the knee joint, potentially contributing to pain and dysfunction.
Tip: Maintaining a healthy weight and engaging in exercises that promote knee stability and strength can help alleviate anterior knee pain and reduce the risk of future injury.
Causes of Anterior Knee Pain
Anterior knee pain can result from a variety of factors, including overuse and injury. Additionally, patellofemoral malalignment is a common cause of anterior knee pain. This misalignment can lead to increased pressure on the patellofemoral joint, contributing to pain and discomfort. In some cases, structural abnormalities such as patellar instability and cartilage damage may also play a role in the development of anterior knee pain.
When considering the causes of anterior knee pain, it’s important to recognize the impact of biomechanical factors. These may include muscle imbalance, poor alignment, and foot mechanics. Addressing these factors through targeted interventions can be crucial in managing and alleviating anterior knee pain.
For a more structured understanding of the causes of anterior knee pain, the following table outlines common contributing factors:
| Factor | Description |
|---|---|
| Overuse | Excessive strain on the knee joint due to repetitive movements or activities |
| Injury | Trauma or damage to the knee, such as ligament sprains, fractures, or meniscus tears |
| Patellofemoral Malalignment | Misalignment of the patella and femur, leading to abnormal tracking and pressure on the joint |
| Structural Abnormalities | Anatomical irregularities that affect the function and stability of the knee joint |
| Biomechanical Factors | Imbalances and dysfunctions in muscle strength, joint alignment, and lower limb mechanics |
In addressing anterior knee pain, understanding these causative factors is essential for developing effective treatment strategies and promoting optimal knee health.
Risk Factors for Anterior Knee Pain
We recognize that understanding the risk factors for anterior knee pain is crucial in both preventing and managing the condition. Certain factors increase the likelihood of developing pain in the anterior aspect of the knee. These include overuse of the knee joint, particularly in athletes or individuals with high levels of physical activity, and misalignment of the knee joint, which can lead to abnormal stress and wear.
Age is also a significant factor, as the risk of knee pain increases with age due to the natural wear and tear of the joint. Additionally, being overweight places extra stress on the knee joints, potentially leading to pain and discomfort. Here is a list of common risk factors:
- Overuse and repetitive motion
- Misalignment or instability of the knee joint
- Age-related degeneration
- Excess body weight
- Previous knee injuries
Tip: Maintaining a healthy weight and engaging in regular, low-impact exercise can help reduce the risk of developing anterior knee pain.
Diagnosing Anterior Knee Pain
Physical Examination
In our approach to diagnosing anterior knee pain, we place significant emphasis on the physical examination. This step is crucial as it allows us to assess the knee’s range of motion, stability, and the presence of any swelling or tenderness. We systematically evaluate the knee by palpating specific anatomical landmarks and performing certain maneuvers that can elicit pain or discomfort, indicative of underlying conditions.
During the examination, we may perform tests such as the patellar apprehension test or the McMurray’s test to assess for patellar instability or meniscal tears, respectively. It’s important to note that while these tests are valuable, they are not definitive and should be interpreted in the context of the entire clinical picture.
Tip: Always communicate with the patient during the examination to understand their pain threshold and to ensure they are comfortable.
Our findings from the physical examination guide us towards the next steps, which may include imaging studies or further clinical tests. The goal is to form a comprehensive understanding of the patient’s condition, which is essential for developing an effective treatment plan.
Imaging Studies
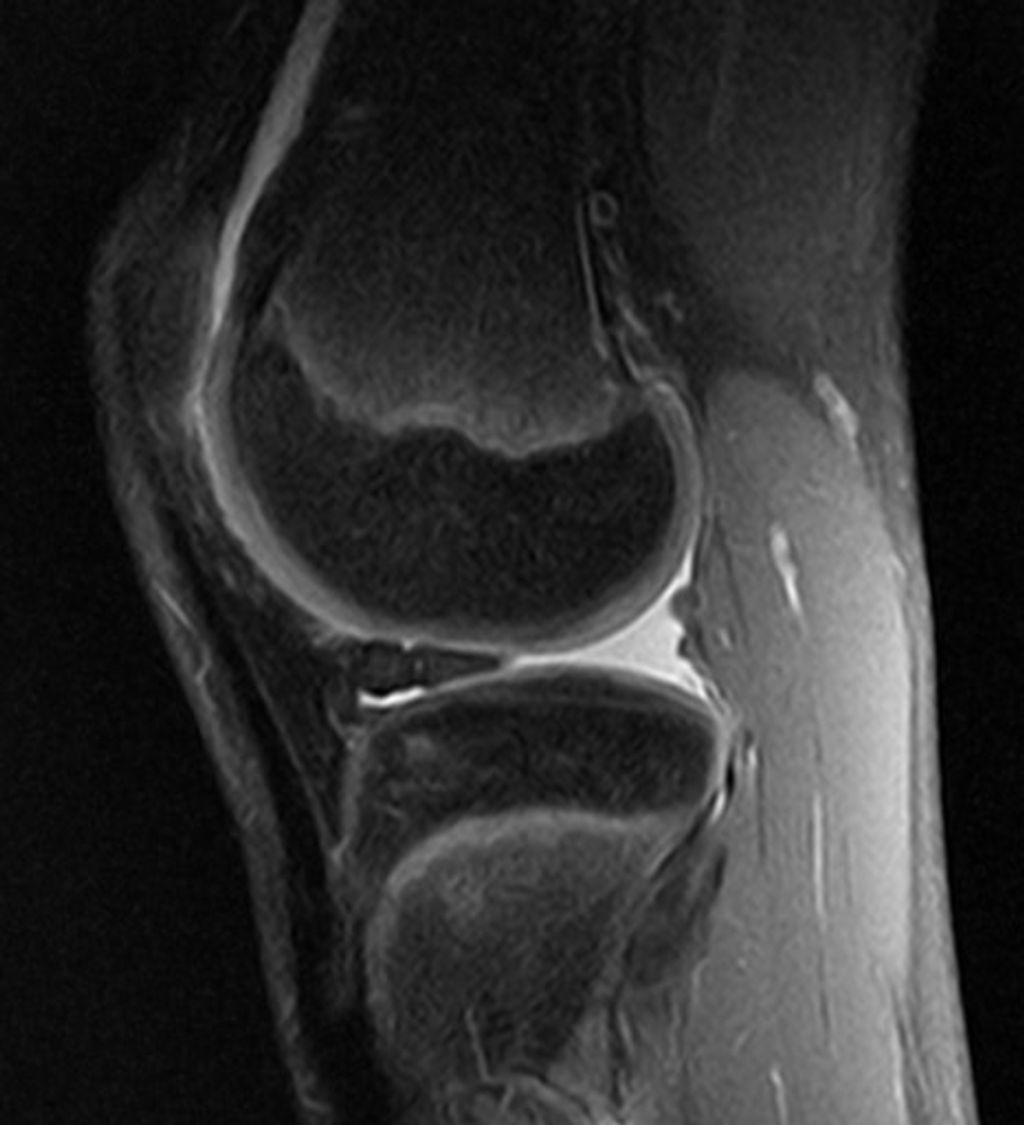
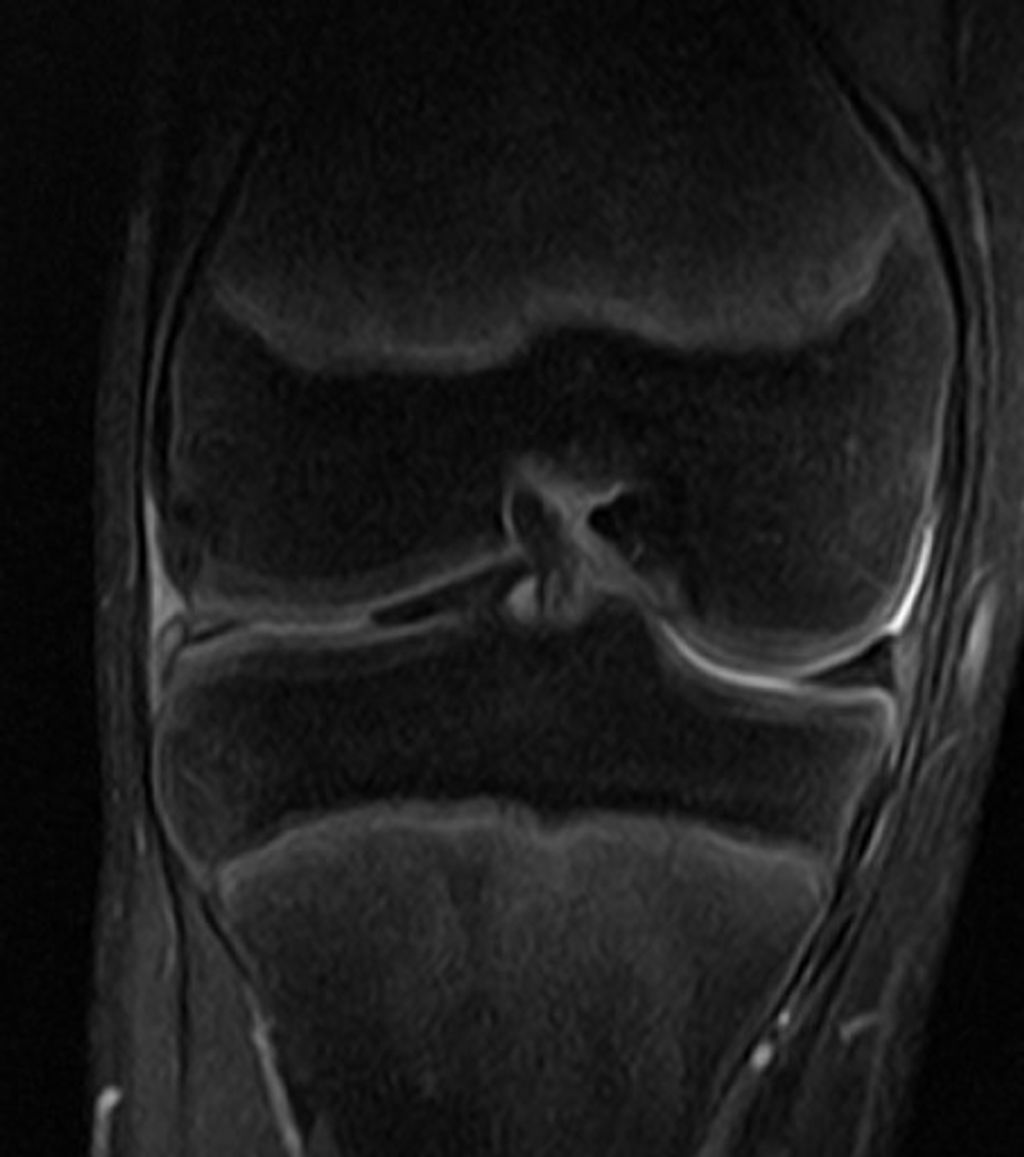
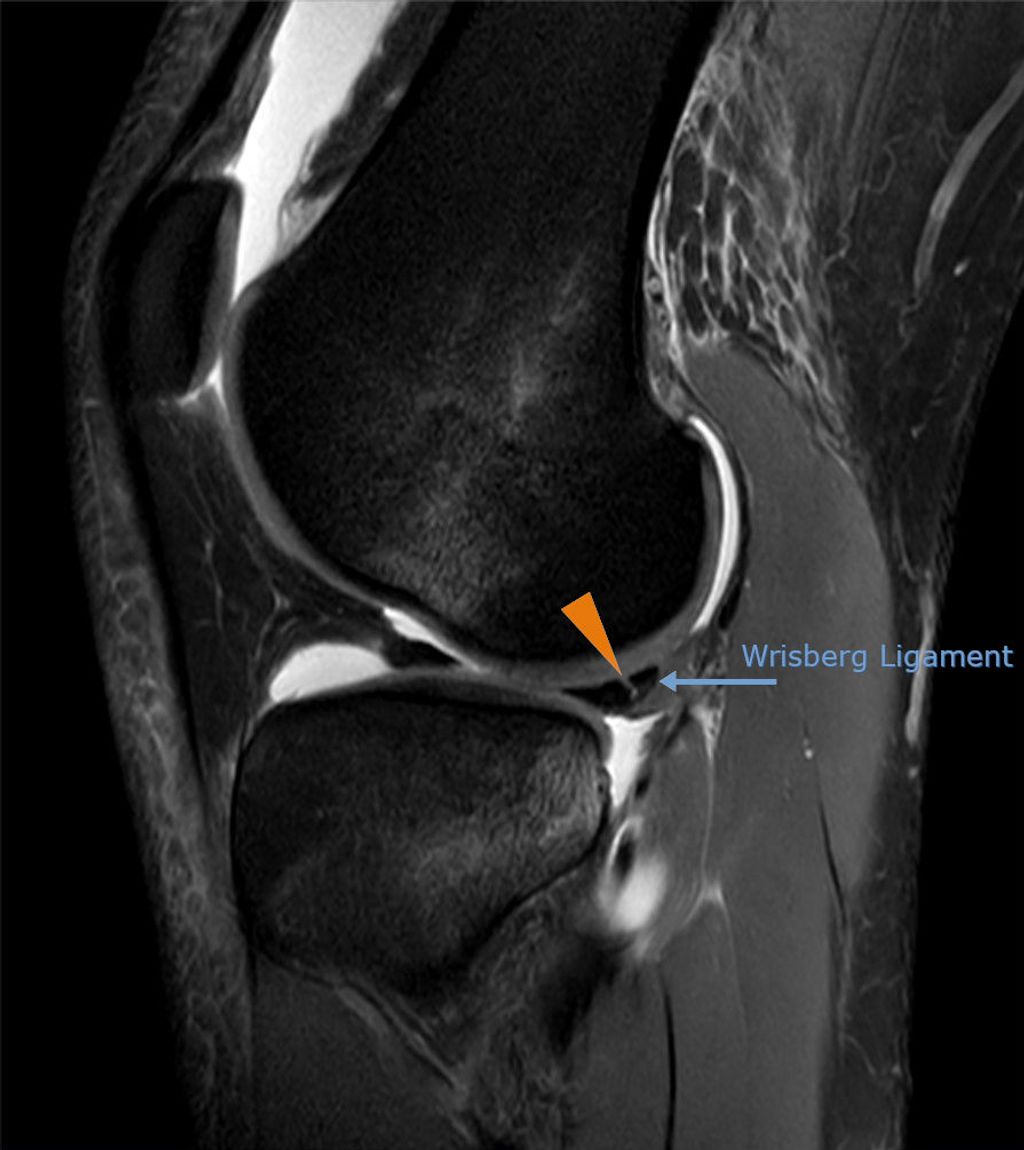
After conducting a thorough physical examination, we often turn to imaging studies to gain a deeper understanding of anterior knee pain. These studies provide us with a visual assessment that can reveal structural abnormalities, signs of wear, or other conditions that might not be apparent through physical examination alone.
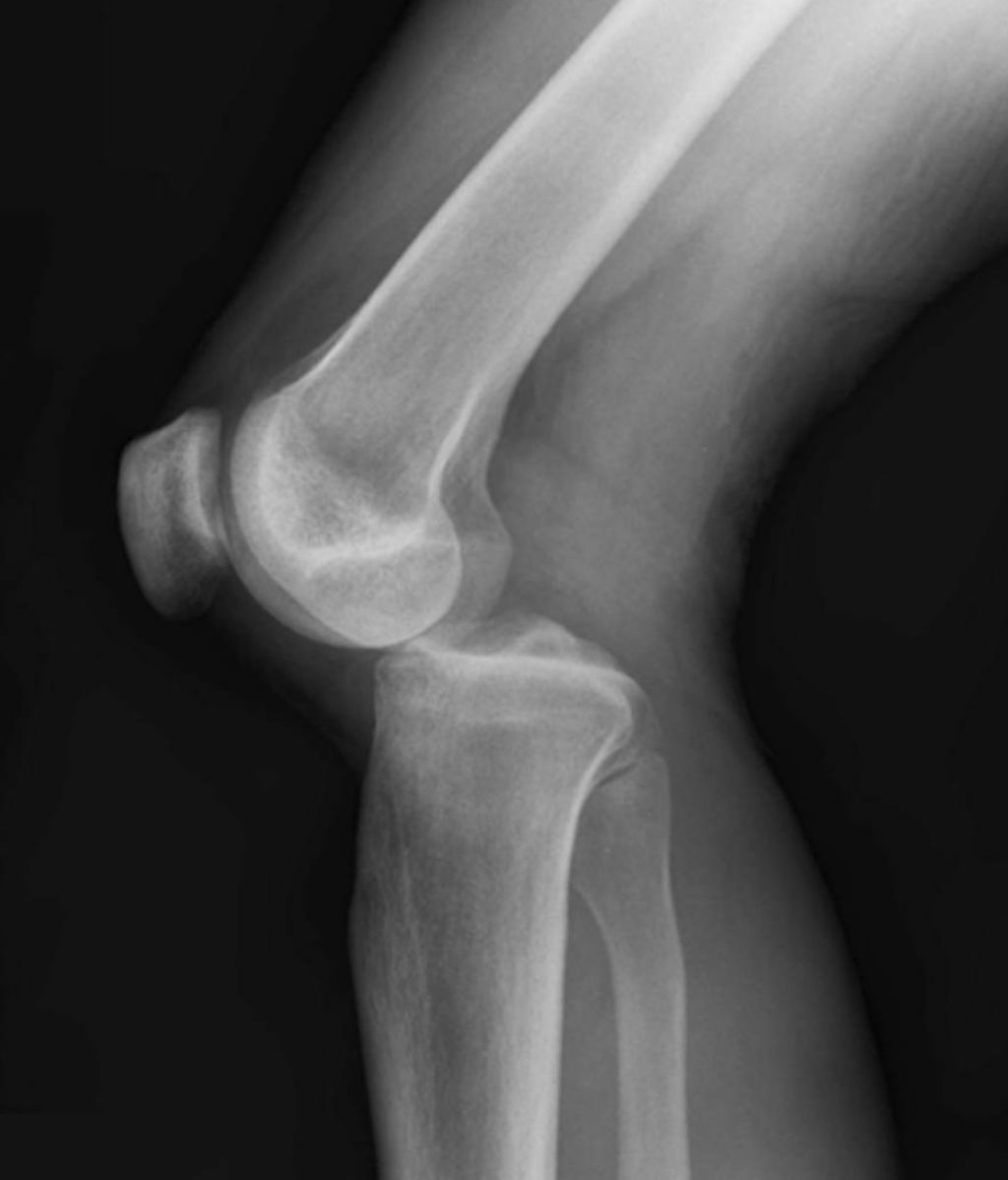
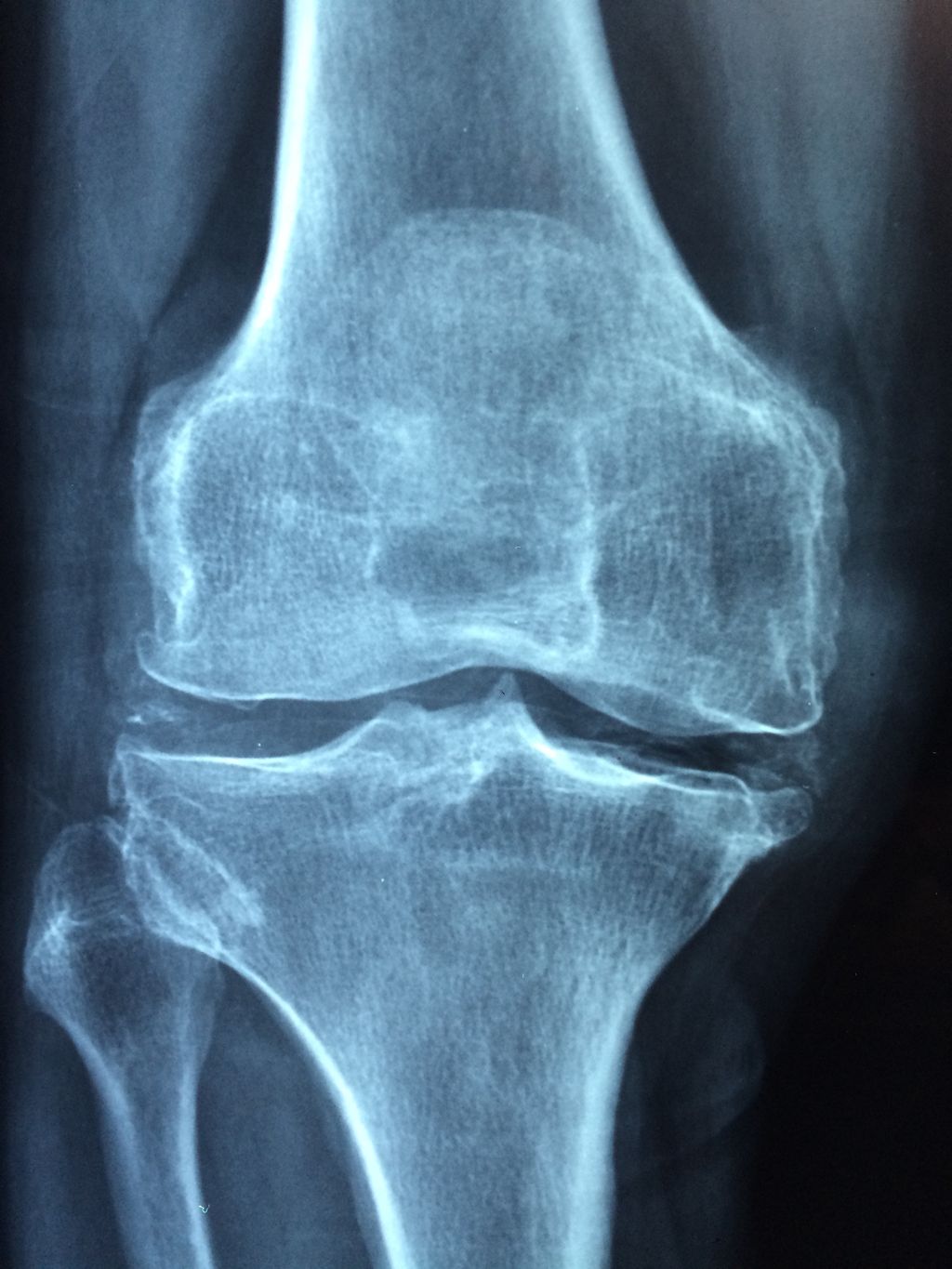
The most common imaging modalities we utilize include X-rays, magnetic resonance imaging (MRI), and ultrasound. X-rays are excellent for visualizing bone structures and can help us identify fractures or signs of osteoarthritis. MRI scans offer a more detailed view, particularly of soft tissues such as ligaments, tendons, and cartilage. Ultrasound is a real-time imaging technique that can assess the dynamic movement of the knee joint.
Tip: Always consider the patient’s history and physical exam findings when selecting the most appropriate imaging study.
Here is a brief overview of the indications for each imaging modality:
- X-rays: Recommended for suspected fractures, osteoarthritis, or bone tumors.
- MRI: Indicated for soft tissue injuries, ligament tears, or meniscal damage.
- Ultrasound: Useful for evaluating tendon pathology or guiding injections.
It’s important to remember that while imaging can be incredibly informative, it should not be the sole basis for a diagnosis. Clinical correlation is essential.
Differential Diagnosis
Once we have conducted a thorough physical examination and utilized imaging studies, we proceed to the crucial step of differential diagnosis. This process allows us to distinguish anterior knee pain from other conditions that may present with similar symptoms. We consider a range of potential diagnoses, including but not limited to patellofemoral pain syndrome, tendinitis, bursitis, and osteoarthritis.
To systematically approach differential diagnosis, we often use a combination of clinical findings and diagnostic tests. For instance, the presence of crepitus or a grinding sensation when the knee is extended might suggest osteoarthritis, while tenderness along the patellar tendon could indicate tendinitis.
Tip: Always consider the patient’s history and activity level when formulating a differential diagnosis, as these factors can significantly influence the underlying cause of knee pain.
Here is a simplified list of conditions we typically consider in our differential diagnosis:
- Patellofemoral pain syndrome
- Tendinitis
- Bursitis
- Osteoarthritis
- Meniscal injuries
- Ligamentous injuries
Our goal is to identify the specific cause of the knee pain to tailor the most effective treatment plan. The correct diagnosis is essential for successful management and recovery.
Treatment Options for Anterior Knee Pain
Conservative Management
After considering the various conservative management strategies, physical therapy interventions emerge as a crucial component of the treatment plan. These interventions focus on improving muscle strength, flexibility, and overall function of the knee joint. Additionally, they aim to address any biomechanical abnormalities that may contribute to anterior knee pain. A structured physical therapy program may include a combination of exercises, manual therapy, and modalities such as ice or heat application. It is important to note that the effectiveness of physical therapy interventions may vary based on individual patient characteristics and the underlying cause of the anterior knee pain.
Moreover, patients may benefit from a comprehensive approach that integrates patient education and lifestyle modifications. This may involve educating patients about proper body mechanics, activity modification, and the importance of maintaining a healthy weight. Furthermore, the incorporation of assistive devices such as knee braces or orthotics may provide additional support and stability to the knee joint, thereby alleviating anterior knee pain.
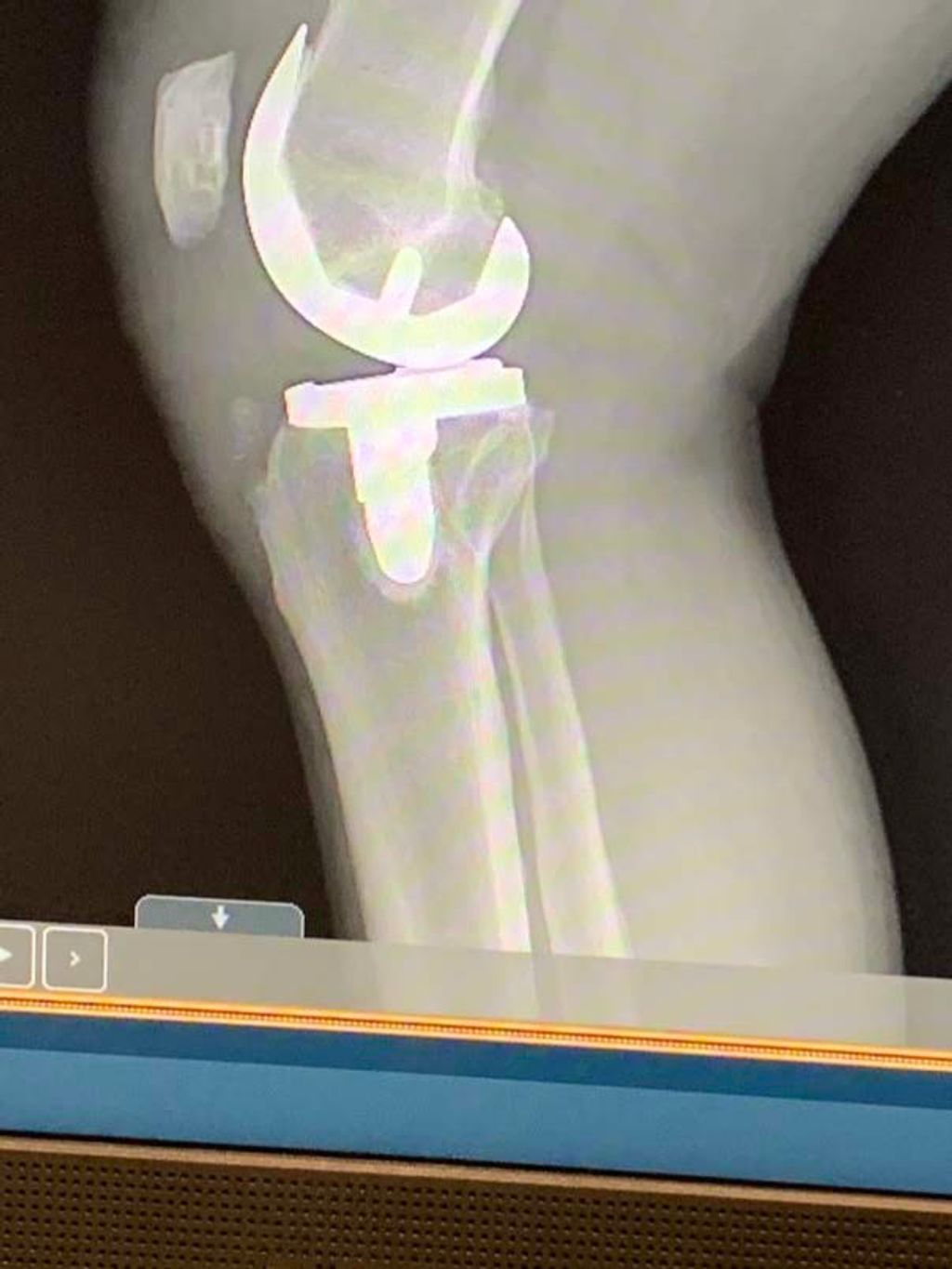
In some cases, when conservative measures do not yield the desired outcomes, surgical interventions may be considered. These interventions are typically reserved for individuals with severe or persistent anterior knee pain that significantly impairs their daily activities. Surgical options may include procedures to realign the patella, repair damaged cartilage, or reconstruct ligaments. It is essential for patients to have a thorough discussion with their healthcare provider to weigh the potential benefits and risks of surgical interventions.
Lastly, it is important to emphasize the significance of a personalized treatment approach. Each patient’s condition is unique, and the treatment plan should be tailored to address their specific needs and goals. By considering the individual’s symptoms, functional limitations, and treatment preferences, healthcare providers can optimize the management of anterior knee pain.
Physical Therapy Interventions
Physical therapy interventions play a crucial role in the management of anterior knee pain. Our approach focuses on strengthening the quadriceps and hamstrings, as well as improving flexibility and balance. Additionally, we emphasize patient education to promote self-management and adherence to the prescribed exercises.
A structured approach to physical therapy interventions may include:
- Quadriceps Strengthening Exercises
- Hamstring Strengthening Exercises
- Flexibility Training
- Balance and Proprioception Exercises
Tip: Consistent and diligent participation in the prescribed physical therapy program is essential for optimal outcomes and long-term relief from anterior knee pain.
Surgical Interventions
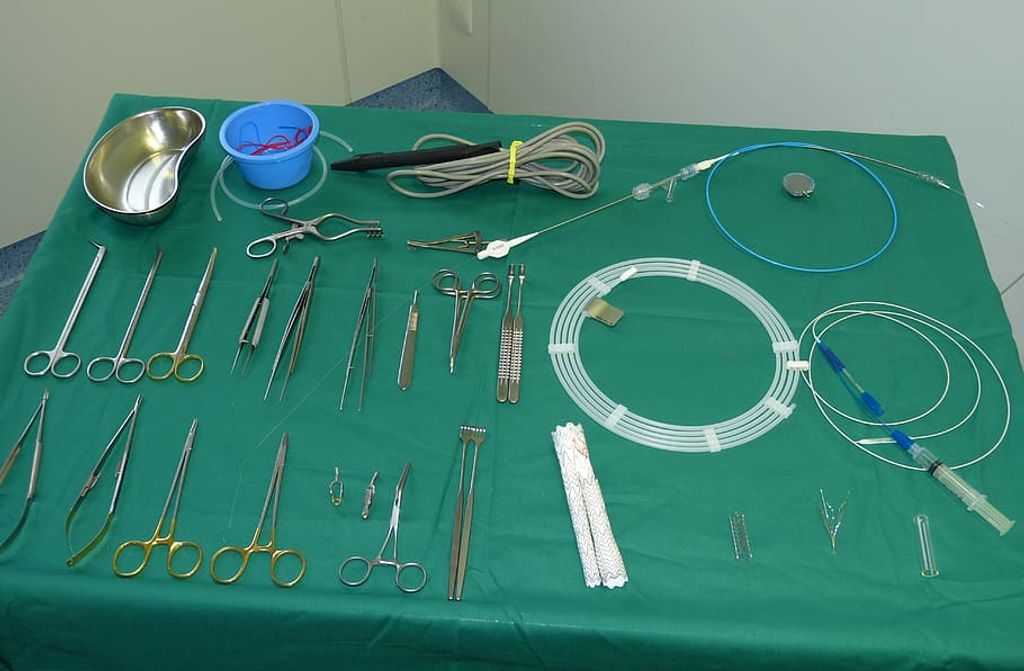
After exploring conservative and physical therapy options, we sometimes find that surgical interventions are necessary to address persistent anterior knee pain. These procedures range from minimally invasive arthroscopic surgery to more extensive reconstructive surgeries, such as an anterior cruciate ligament (ACL) reconstruction.
When we consider surgery, it’s crucial to understand the potential risks and benefits. The decision is always made in close consultation with the patient, considering their unique situation and health goals. Post-operative care is equally important to ensure a successful recovery. For instance, a client may experience a setback, such as an ACL issue 10 weeks post-surgery, but with the right strategies, these can be overcome.
Rehabilitation is a key component of the recovery process. Here’s a brief overview of the typical post-surgical rehabilitation timeline:
- Initial rest and inflammation control (0-2 weeks)
- Gradual increase in mobility and strength exercises (2-6 weeks)
- Progressive return to functional activities (6-12 weeks)
- Sport-specific training and reconditioning (>12 weeks)
Tip: Consistent follow-up with healthcare providers and adherence to the rehabilitation protocol are essential for a successful outcome.
Conclusion
In conclusion, anterior knee pain is a complex condition with multiple potential causes, including overuse injuries, biomechanical issues, and structural abnormalities. Understanding the underlying factors contributing to anterior knee pain is crucial for effective diagnosis and treatment. By addressing the root causes and implementing targeted interventions, individuals experiencing anterior knee pain can achieve improved functionality and long-term relief. Further research and clinical studies are needed to enhance our understanding of this prevalent issue and develop more comprehensive treatment strategies.
Frequently Asked Questions
What are the common causes of anterior knee pain?
Common causes of anterior knee pain include patellofemoral pain syndrome, patellar tendonitis, osteoarthritis, and overuse injuries.
How is anterior knee pain diagnosed?
Anterior knee pain is diagnosed through a physical examination, imaging studies such as X-rays and MRI, and a differential diagnosis to rule out other potential causes.
What are the risk factors for developing anterior knee pain?
Risk factors for anterior knee pain include overuse or repetitive strain on the knee joint, poor biomechanics, muscle imbalances, and previous knee injuries.
What are the conservative management options for anterior knee pain?
Conservative management options include rest, ice, elevation, nonsteroidal anti-inflammatory drugs (NSAIDs), and activity modification.
What types of physical therapy interventions are effective for anterior knee pain?
Physical therapy interventions such as strengthening exercises, stretching, manual therapy, and biomechanical correction can be effective for anterior knee pain.
When is surgical intervention recommended for anterior knee pain?
Surgical intervention is recommended for anterior knee pain when conservative treatments and physical therapy have not provided relief, and there is significant structural damage or malalignment of the knee joint.