Knee and hip pain on one side can be a debilitating condition that affects daily activities and quality of life. Understanding the anatomy, causes, diagnosis, and treatment options is essential for effective management. This article aims to provide insight into the complexities of unilateral knee and hip pain and offer key takeaways for a better understanding.
Key Takeaways
- Unilateral knee and hip pain can be caused by inflammatory conditions, degenerative joint diseases, or traumatic injuries.
- Physical examination, imaging studies, and differential diagnosis are crucial for accurate diagnosis and assessment of unilateral knee and hip pain.
- Conservative management, surgical interventions, and rehabilitation strategies are the main treatment options for unilateral knee and hip pain.
- Early intervention and proper diagnosis are essential for preventing long-term complications associated with unilateral knee and hip pain.
- Multidisciplinary approach involving healthcare professionals such as orthopedic surgeons, physical therapists, and pain management specialists is beneficial for comprehensive management of unilateral knee and hip pain.
Anatomy of Knee and Hip Joints
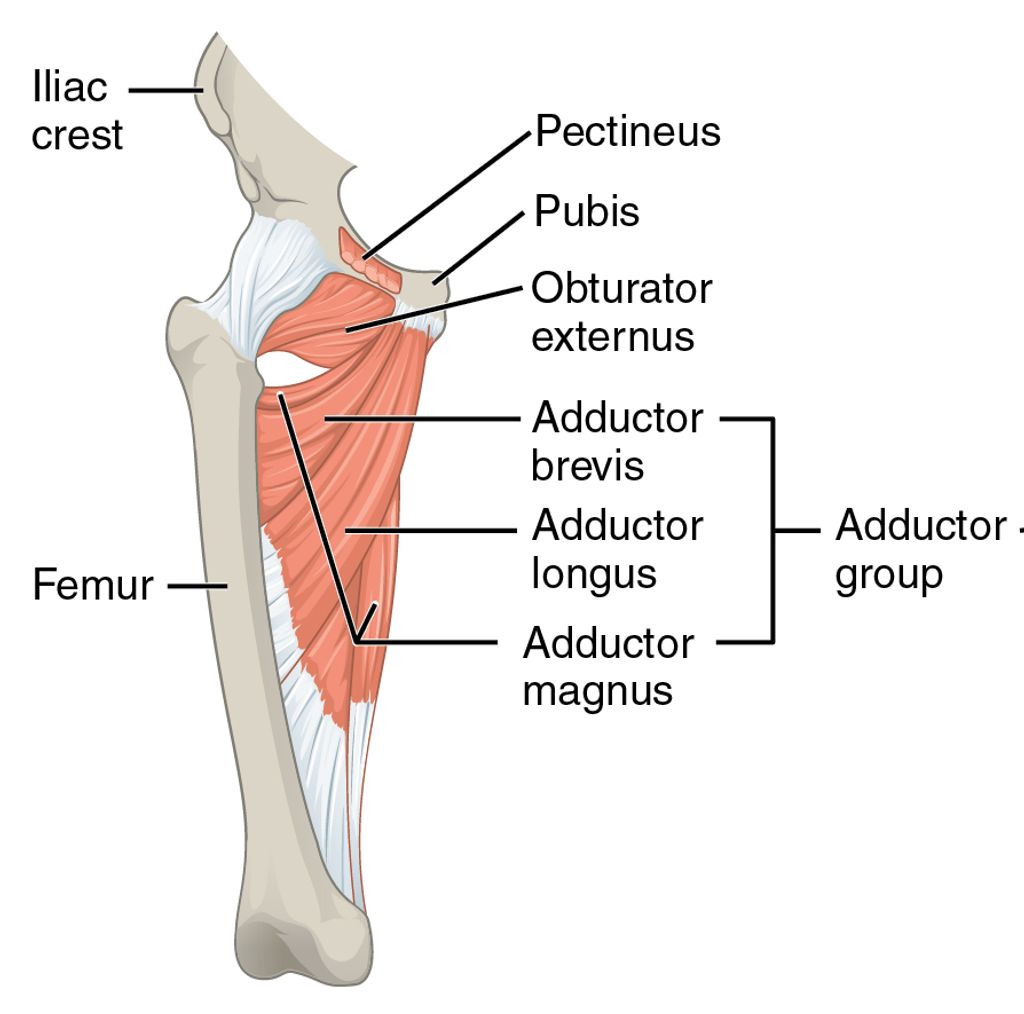
Structure and Function of Knee Joint
The knee joint is a complex hinge joint that allows for flexion, extension, and limited rotation. Articular cartilage covers the ends of the bones, providing smooth movement and cushioning. Ligaments, including the anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL), provide stability and prevent excessive movement. The menisci, located between the femur and tibia, act as shock absorbers and enhance joint stability.
| Structure | Function |
|---|---|
| Femur | Articulates with tibia and patella |
| Tibia | Supports body weight and articulates with femur |
| Patella | Protects knee joint and enhances leverage |
| Quadriceps muscles | Extend the knee joint and stabilize the patella |
| Hamstring muscles | Flex the knee joint and aid in hip extension |
Structure and Function of Hip Joint
We understand the hip joint to be a pivotal element in the human body’s mobility. It is a ball-and-socket joint, where the femoral head fits into the acetabulum of the pelvis, allowing for a wide range of motion. The stability of the hip joint is maintained by a complex interplay of ligaments, muscles, and the joint capsule.
The primary function of the hip joint is to support the weight of the body in both static and dynamic postures. This joint enables us to perform essential movements such as walking, running, and jumping. It is also crucial for maintaining balance and posture.
- Ligaments of the Hip Joint
- Iliofemoral ligament
- Pubofemoral ligament
- Ischiofemoral ligament
Tip: Regular exercise and maintaining a healthy weight can significantly reduce the risk of developing hip pain.
In our research, we often encounter various factors that can affect the hip joint’s health, such as the impact of youth baseball batting on hip pain or the benefits of strength training in cricketers. While these activities are specific to athletes, the lessons learned can be applied to the general population to prevent hip pain and maintain joint health.
Causes of Unilateral Knee and Hip Pain
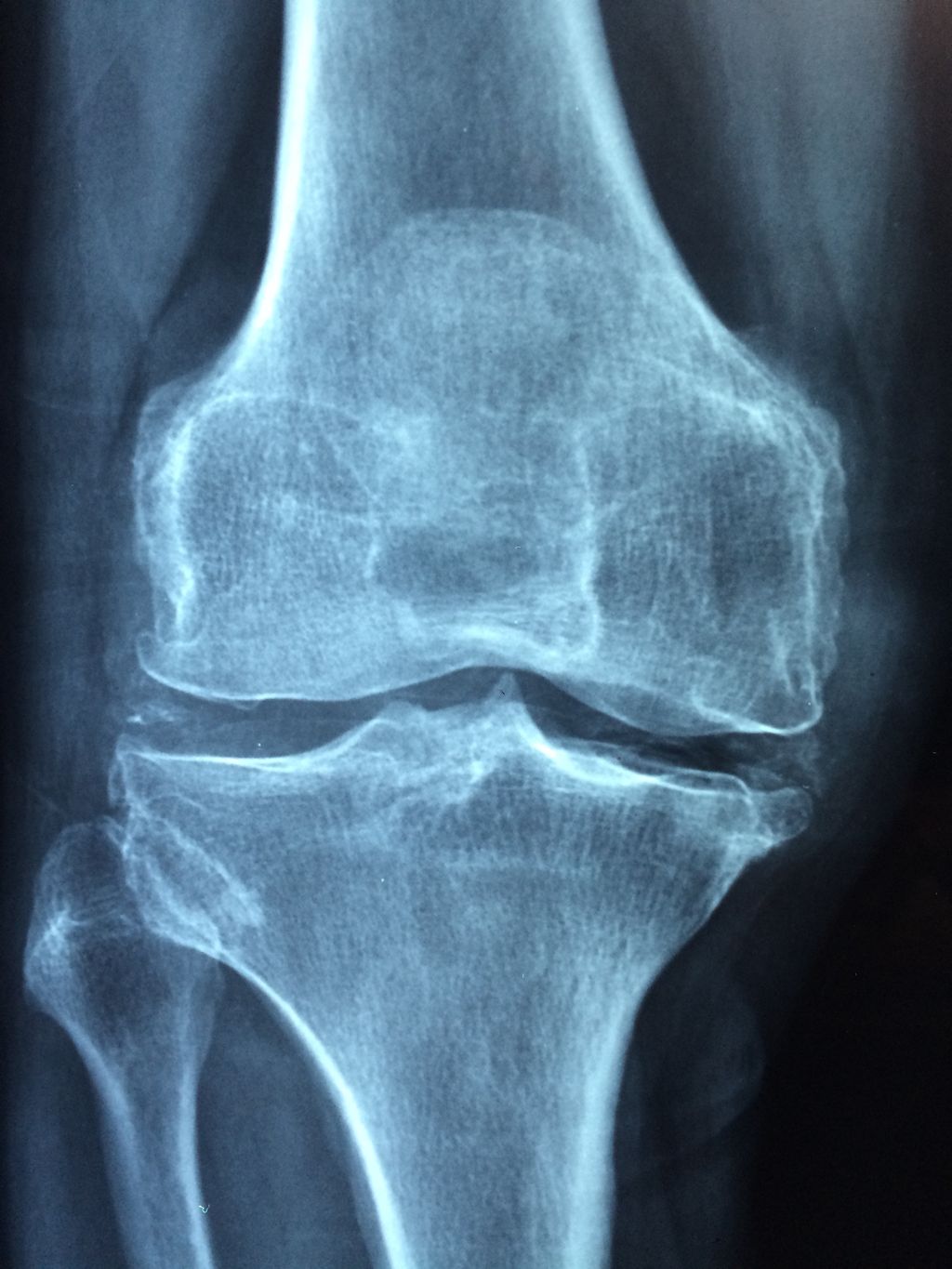
Inflammatory Conditions
We often encounter patients who suffer from unilateral knee and hip pain due to various inflammatory conditions. These ailments can range from autoimmune disorders like rheumatoid arthritis to more localized issues such as bursitis or tendinitis. The inflammation can lead to significant discomfort and impair mobility, making early diagnosis and management crucial.
Inflammatory conditions typically present with symptoms such as swelling, redness, warmth, and pain that is often worse in the morning or after periods of inactivity. To better understand these conditions, let’s consider the following list of common inflammatory diseases that can affect the knee and hip joints:
- Rheumatoid arthritis
- Psoriatic arthritis
- Ankylosing spondylitis
- Septic arthritis
- Bursitis
- Tendinitis
Tip: It’s essential to distinguish between the various inflammatory conditions, as each requires a unique treatment approach. For instance, managing an autoimmune disorder may involve immunosuppressive medications, whereas treating an infection would require antibiotics.
Our approach to managing these conditions involves a combination of medication, lifestyle modifications, and sometimes physical therapy. The goal is to reduce inflammation, alleviate pain, and prevent further joint damage. It’s important to note that while some inflammatory conditions can be managed effectively with conservative measures, others may progress and necessitate more aggressive treatment strategies.
Degenerative Joint Diseases
Degenerative joint diseases, such as osteoarthritis, are characterized by the gradual breakdown of cartilage and the formation of bone spurs. Inflammation and pain are common symptoms, often leading to limited mobility and reduced quality of life. Conservative management is often the first line of treatment, including weight management and physical therapy. In some cases, surgical interventions may be necessary to address severe joint damage. It’s important to consider the long-term implications of these diseases on overall joint health and function.
Traumatic Injuries
Traumatic injuries to the knee and hip joints can result in significant pain and functional impairment. Acute trauma, such as a sports-related injury or a fall, can lead to sudden and severe pain, swelling, and limited range of motion. It is important to promptly assess and manage traumatic injuries to prevent long-term complications. In some cases, surgical intervention may be necessary to repair damaged structures and restore joint function. Rehabilitation following traumatic injuries is crucial for optimizing recovery and regaining strength and mobility. It involves a comprehensive program of exercises, physical therapy, and gradual return to activities. Consistent adherence to the rehabilitation plan is essential for achieving the best outcomes and reducing the risk of recurrent injuries.
Diagnosis and Assessment
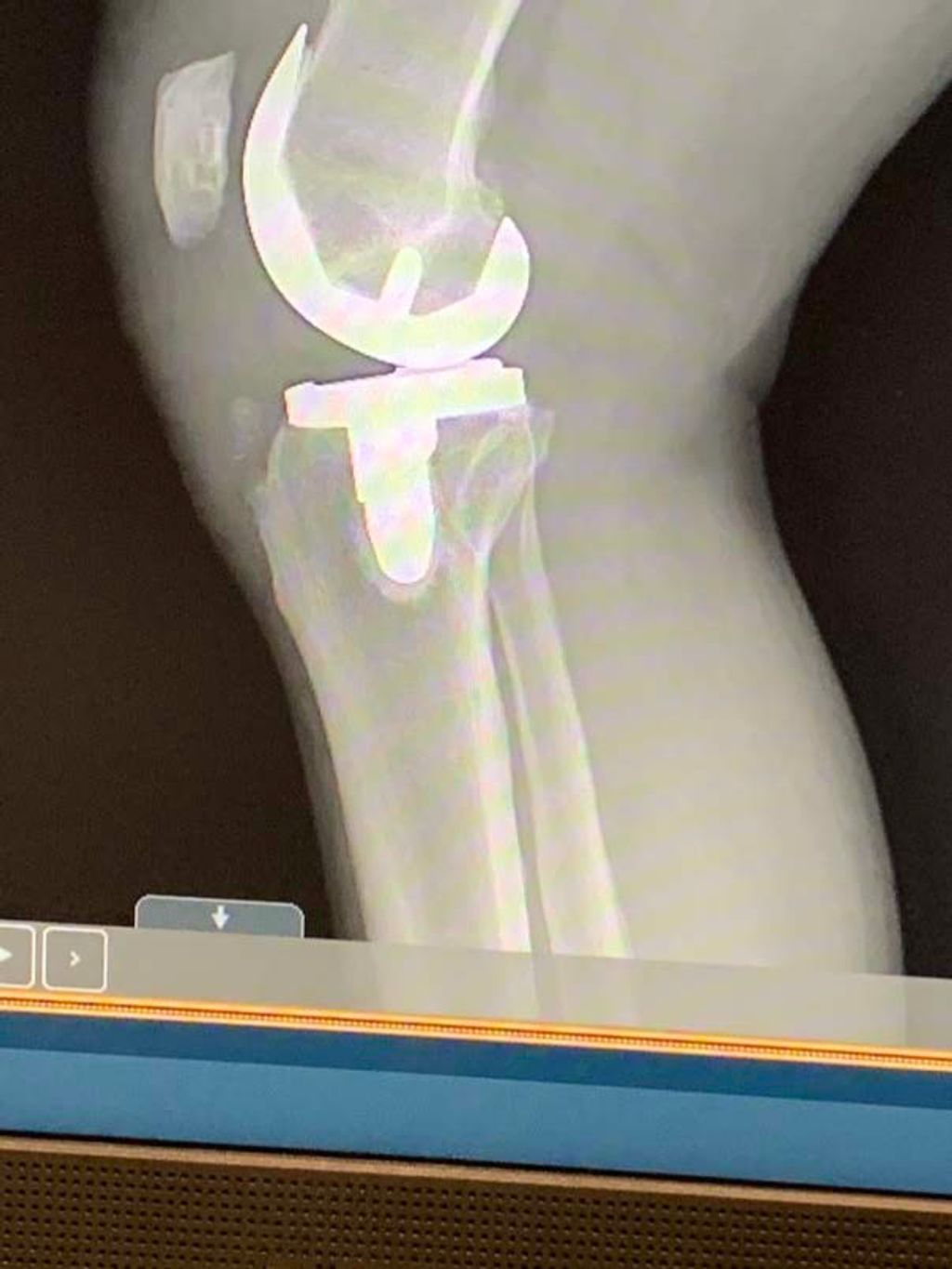
Physical Examination
In the process of diagnosing unilateral knee and hip pain, physical examination plays a crucial role in evaluating the range of motion, joint stability, and signs of inflammation. Additionally, imaging studies such as X-rays and MRI scans provide detailed insights into the structural integrity of the affected joints. These assessments aid in formulating a comprehensive differential diagnosis, considering various musculoskeletal and neurological conditions. It is important to interpret the findings of these assessments in conjunction with the patient’s medical history and clinical presentation to establish an accurate diagnosis and guide the subsequent treatment plan.
Imaging Studies
Following a thorough physical examination, we often turn to imaging studies to gain a deeper understanding of the underlying causes of unilateral knee and hip pain. These diagnostic tools provide us with detailed images of the internal structures, allowing for a more accurate assessment.
The most common imaging modalities we utilize include X-rays, which are quick and useful for detecting bone abnormalities, and Magnetic Resonance Imaging (MRI) scans, which offer a more comprehensive view of both bone and soft tissues. Ultrasound and Computerized Tomography (CT) scans also play a role in certain cases, particularly when we suspect soft tissue injuries or require a cross-sectional view of the joint.
It is crucial to select the most appropriate imaging study based on the patient’s symptoms and the findings from the physical examination to ensure a precise diagnosis.
The choice of imaging technique is guided by the suspected condition, as each modality has its strengths. For instance, MRI is particularly beneficial in diagnosing ligament tears or cartilage damage, while X-rays are the first line of investigation for fractures or osteoarthritis.
Differential Diagnosis
In the process of diagnosing unilateral knee and hip pain, physical examination plays a crucial role in identifying specific signs and symptoms. Additionally, imaging studies such as X-rays and MRI scans provide valuable insights into the structural integrity of the affected joints. These assessments aid in formulating a comprehensive differential diagnosis to distinguish between various underlying conditions. It is important to note that the differential diagnosis may include but is not limited to:
Treatment Options
Conservative Management
In our approach to conservative management, we prioritize non-invasive interventions such as physical therapy, exercise, and lifestyle modifications. These methods aim to reduce pain, improve function, and enhance overall quality of life for individuals experiencing unilateral knee and hip pain. Our team emphasizes the importance of personalized care and tailored treatment plans to address the unique needs of each patient. We believe in the power of holistic care that encompasses both physical and emotional well-being.
Surgical Interventions
When conservative management fails to alleviate knee and hip pain on one side, we often consider surgical interventions. These procedures are tailored to the individual’s condition and may range from minimally invasive arthroscopic surgery to total joint replacement. It’s crucial to understand that surgery is not a one-size-fits-all solution and the choice of procedure depends on factors such as the severity of the disease, age, and overall health of the patient.
- Postoperative care is essential for a successful outcome. Patients must adhere to a structured rehabilitation program to restore joint function and mobility. This typically includes physical therapy, pain management, and gradual return to activities. It’s important to note that recovery times can vary significantly among individuals.
Overcoming setbacks with the right strategies is key to a successful recovery. It is not uncommon for patients to experience challenges, such as the one mentioned at week 10 post-surgery. Being prepared and having a supportive care team can make a significant difference in the recovery process.
The following list outlines common surgical interventions for unilateral knee and hip pain:
- Arthroscopic debridement or repair
- Osteotomy to correct joint alignment
- Partial or total knee replacement
- Hip resurfacing or total hip replacement
- Ligament reconstruction or repair
Rehabilitation Strategies
After addressing the immediate concerns through conservative management or surgical interventions, we turn our focus to rehabilitation strategies. These strategies are crucial for restoring function, improving mobility, and reducing the risk of future injury. A comprehensive rehabilitation program is tailored to each individual’s needs, taking into account the severity of their condition and their overall health status.
Our approach to rehabilitation typically includes a combination of physical therapy exercises, pain management techniques, and education on body mechanics. We emphasize the importance of patient involvement and commitment to the rehabilitation process, as active participation is key to a successful recovery.
Physical therapy exercises are designed to strengthen the muscles around the knee and hip joints, improve flexibility, and increase range of motion. Here’s a simplified outline of a typical rehabilitation regimen:
- Initial assessment to determine specific needs
- Development of a personalized exercise program
- Regular progress evaluations and adjustments to the program
- Education on proper body mechanics to prevent re-injury
Tip: Consistency in performing prescribed exercises and attending therapy sessions is vital for optimal recovery.
It’s important to note that rehabilitation is a journey, often requiring patience and perseverance. We work closely with our patients to set realistic goals and provide support throughout their recovery.
Conclusion
In conclusion, this article has provided a comprehensive overview of the factors contributing to knee and hip pain on one side. By examining the asymmetry in musculoskeletal function and the role of posture in pain development, we have gained valuable insights into the complexities of unilateral joint discomfort. Further research and clinical investigation are necessary to deepen our understanding and develop effective interventions for individuals experiencing these challenging conditions.
Frequently Asked Questions
What are the common symptoms of unilateral knee and hip pain?
Common symptoms include pain, swelling, stiffness, and difficulty with movement.
Can unilateral knee and hip pain be caused by overuse or repetitive strain?
Yes, overuse or repetitive strain can lead to knee and hip pain on one side due to wear and tear on the joints.
Is it necessary to seek medical attention for unilateral knee and hip pain?
It is advisable to seek medical attention to determine the underlying cause and receive appropriate treatment.
What imaging studies are commonly used to diagnose knee and hip problems?
X-rays, MRI, and CT scans are commonly used to diagnose knee and hip issues and assess the extent of damage.
Are there non-surgical treatment options for unilateral knee and hip pain?
Yes, non-surgical options such as physical therapy, medication, and lifestyle modifications can be effective in managing knee and hip pain.
What is the typical recovery time after surgical intervention for knee and hip problems?
Recovery time varies depending on the type of surgery, but it may range from several weeks to several months.