Torn Meniscus Risk: Can It Cause Knee Collapse?
Did you know that a torn meniscus can significantly increase the risk of knee collapse?
When we hear about knee injuries, we often think of sprains or strains. However, a torn meniscus is a common knee injury that can have a profound impact on your knee stability and overall function.
Whether it’s a sudden twist while playing sports or wear and tear from repetitive movements, a torn meniscus can cause debilitating symptoms like pain, swelling, and limited range of motion. But it’s not just the immediate effects that make a torn meniscus concerning.
In fact, untreated or improperly managed torn meniscus can lead to long-term knee instability. This means that your knee may give out or buckle unexpectedly, potentially causing falls and further damage. The fear of losing control of your knee can be both physically and emotionally challenging.
In this article, we will explore the relationship between a torn meniscus and knee collapse. We’ll delve into the role of the meniscus in knee stability, discuss the symptoms, diagnosis, and treatment options for a torn meniscus, and provide essential information to help you understand and manage this condition effectively.
Understanding the Meniscus and Its Role in Knee Stability
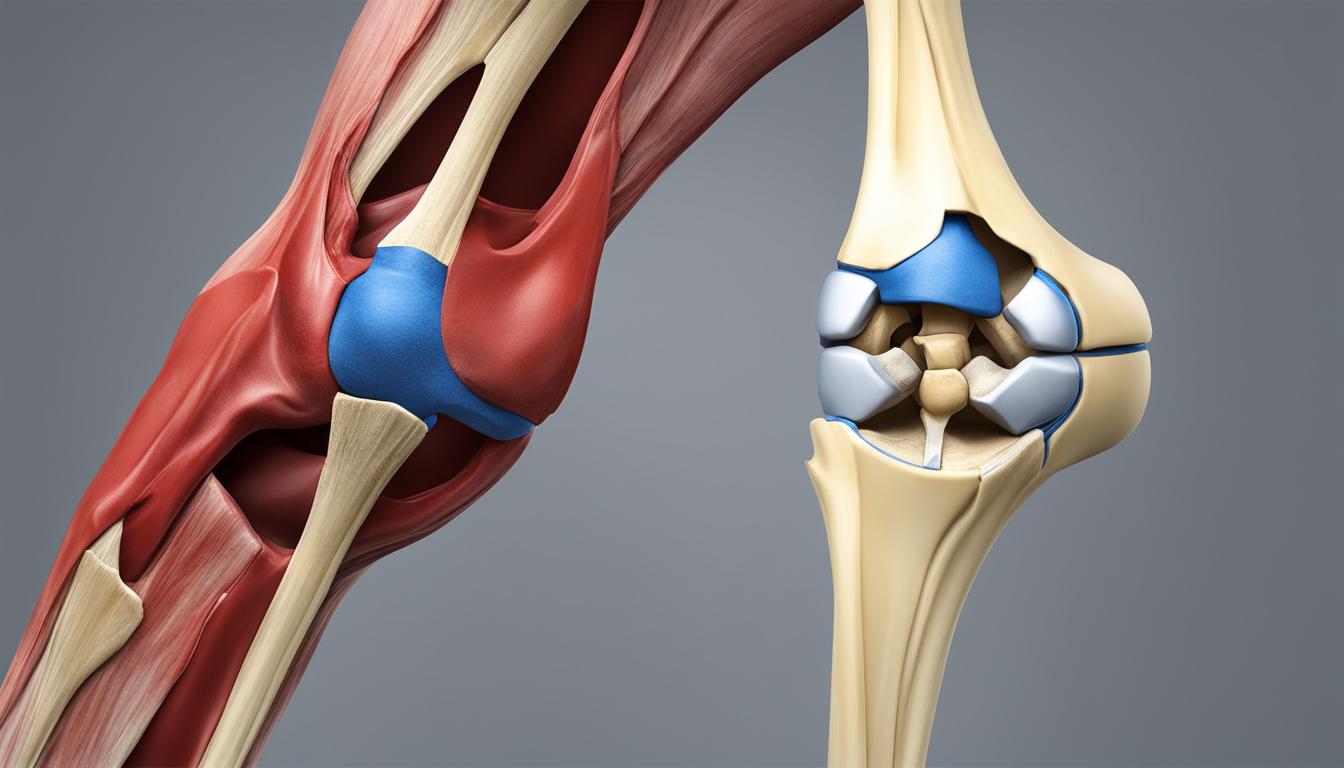
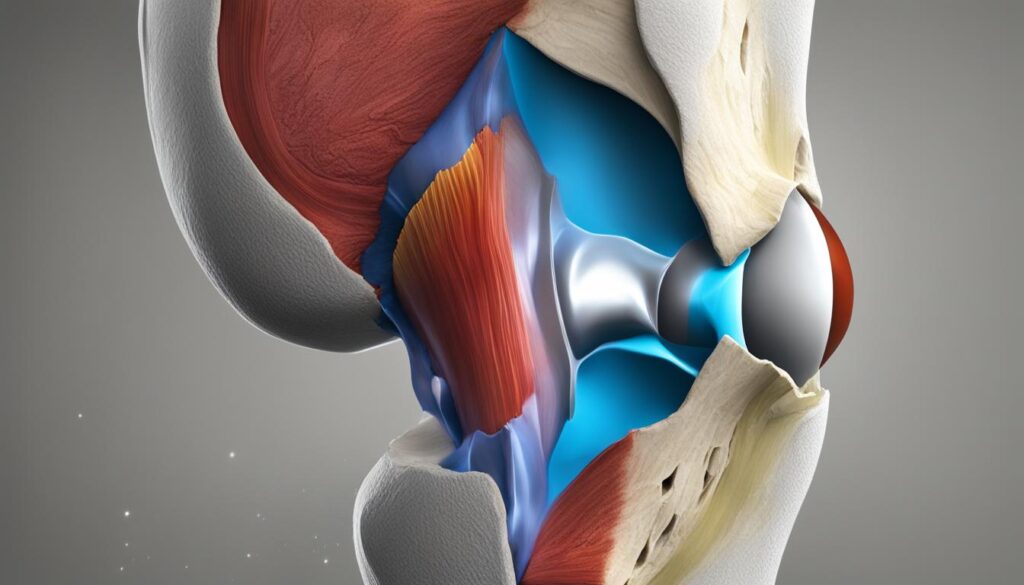
The meniscus is a crucial component of the knee joint, playing a significant role in providing stability and support. Positioned between the bones of the knee, the meniscus is a crescent-shaped disk made of strong connective tissue.
Functioning as a shock absorber, the meniscus cushions the lower part of the leg from the weight of the body, distributing the forces experienced during activities such as walking, running, or jumping. It helps to minimize the impact on the bones and cartilage in the knee.
When a meniscus tear occurs, this important shock absorber is damaged, affecting the knee’s ability to function normally. The tear creates an imbalance in the knee joint, leading to knee instability. As a result, individuals may experience symptoms such as weakness, buckling of the knee, and a sensation of the knee giving way.
It is crucial to understand that knee instability and a torn meniscus are closely interlinked. A meniscus tear can directly contribute to knee instability, making it essential to address the torn meniscus promptly to restore stability and prevent further complications.
“A torn meniscus can significantly impact knee stability, leading to symptoms such as weakness, buckling, and a sensation of the knee giving way.”
Symptoms, Diagnosis, and Treatment of a Torn Meniscus
If you suspect a torn meniscus, it is crucial to be aware of the symptoms associated with this condition. Common signs of a torn meniscus include:
- Pain in the knee
- Swelling and inflammation
- Stiffness or limited range of motion
- A catching or locking sensation in the knee
If you experience any of these symptoms or notice that your knee feels weak or unstable, it is important to seek medical attention promptly. Your doctor will perform a thorough physical examination and may recommend additional diagnostic tests to confirm the presence of a torn meniscus.
Diagnostic methods for a torn meniscus typically involve X-rays, magnetic resonance imaging (MRI), or arthroscopy. X-rays help rule out other potential causes of knee pain, while an MRI can provide detailed images of the meniscus to determine the extent and location of the tear. Arthroscopy is a minimally invasive surgical procedure that can not only diagnose a torn meniscus but also treat the condition.
Once a torn meniscus is confirmed, the appropriate treatment plan can be determined based on the severity of the tear. Treatment options may include:
- Ice therapy to reduce swelling and inflammation
- Medications such as nonsteroidal anti-inflammatory drugs (NSAIDs) to manage pain
- Physical therapy exercises to strengthen the surrounding muscles and improve knee stability
- Surgery, such as arthroscopic meniscus repair or meniscectomy, depending on the location and severity of the tear
It is essential to follow your doctor’s recommendations and undergo the prescribed treatment to ensure proper healing and reduce the risk of further knee instability. With early detection and appropriate interventions, individuals with a torn meniscus can expect to regain stability and resume their normal activities.
Case Study: John’s Experience with a Torn Meniscus
“I first noticed something was wrong with my knee when it started giving out, making it difficult for me to walk or engage in physical activities. The pain and swelling were unbearable at times. After consulting with my doctor, I learned that I had a torn meniscus. Through arthroscopy and post-surgical rehabilitation, I was able to regain the stability in my knee and get back to doing the things I love.”
Conclusion
A torn meniscus can have a significant impact on knee stability, causing symptoms such as weakness, buckling, and a sense of the knee giving way. If you experience these symptoms or suspect a torn meniscus, it is crucial to seek medical attention promptly.
Early diagnosis and appropriate treatment are essential in managing a torn meniscus and preventing further complications. Treatment options may include exercises, medication, and in some cases, surgery. By addressing a torn meniscus promptly, you can improve overall knee function and minimize the risk of long-term knee instability.
Remember, if you are dealing with knee instability or suspect a torn meniscus, don’t delay in seeking professional medical advice. By taking proactive steps and working with your healthcare provider, you can find the most suitable treatment approach and regain stability in your knee.
FAQ
Can a torn meniscus cause your knee to give out?
Yes, a torn meniscus can potentially cause knee instability, leading to symptoms such as weakness, buckling, and a sensation of the knee giving way.
Can a meniscus tear make your knee give way?
Yes, a meniscus tear can cause knee instability, resulting in a feeling of the knee giving way.
What are the symptoms of a torn meniscus?
Symptoms of a torn meniscus may include pain, swelling, stiffness, and a catching or locking sensation in the knee.
How is a torn meniscus diagnosed?
Diagnosis of a torn meniscus may involve a physical examination, X-ray, MRI, or arthroscopy.
What are the treatment options for a torn meniscus?
Treatment options for a torn meniscus can vary depending on the severity of the tear and may include icing, medication, exercises, or surgery.
How can I prevent knee instability from a torn meniscus?
Early diagnosis and appropriate treatment of a torn meniscus can help prevent knee instability and improve overall knee function.
Source Links
- https://www.hss.edu/condition-list_torn-meniscus.asp
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2758243/
- https://www.uwmedicine.org/conditions-symptoms/bone-joint-muscle/torn-meniscus