Show Image
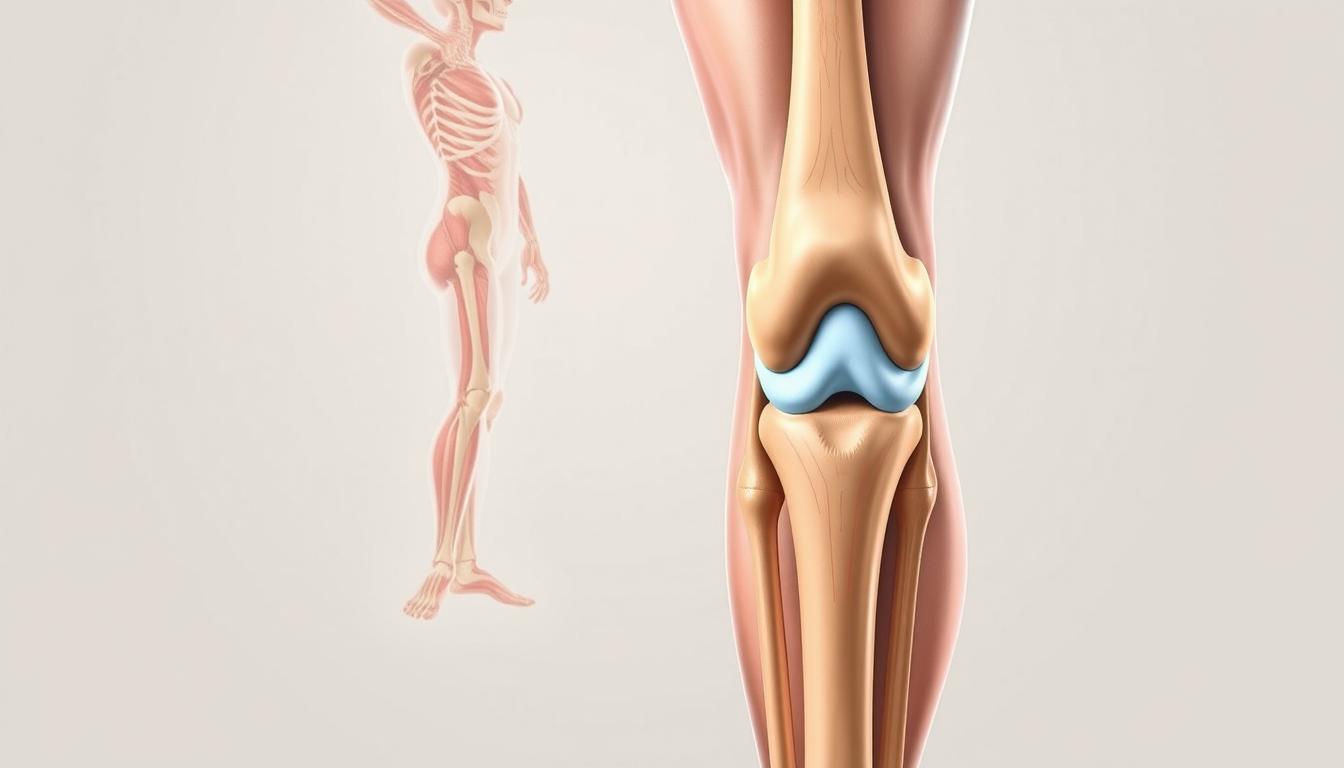
Knee pain is a pervasive issue that affects individuals across all age groups, whether stemming from injury, arthritis, or overuse. By comprehending the underlying causes of knee pain, you can more effectively manage symptoms and make informed decisions about treatment options. This comprehensive guide will delve into the intricacies of knee pain, providing you with valuable insights and practical solutions to improve your quality of life.
Common Causes of Knee Pain
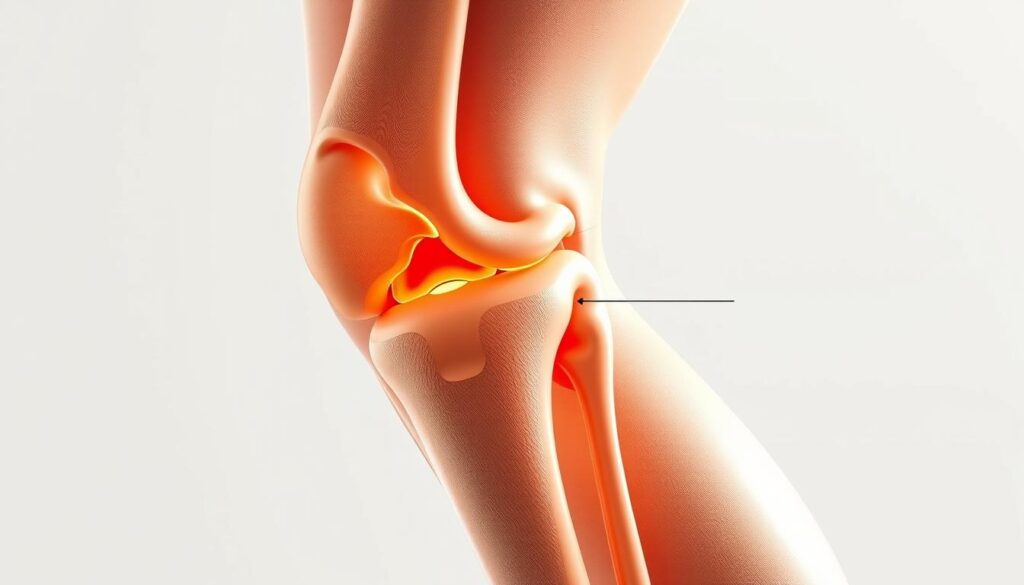
Knee pain can originate from various sources, each with its unique characteristics and implications. Let’s explore some of the most prevalent causes:
Injuries
Injuries are among the most frequent culprits of knee pain, particularly in athletes and physically active individuals. These can include:
- Fractures: Breaks in the bones that form the knee joint, often resulting from high-impact trauma.
- Sprains: Overstretching or tearing of ligaments, commonly affecting the anterior cruciate ligament (ACL) or medial collateral ligament (MCL).
- Torn ligaments: Complete ruptures of ligaments, such as the ACL, which can severely compromise knee stability.
Such injuries typically occur due to accidents, falls, or participation in high-impact sports like football, basketball, or skiing.
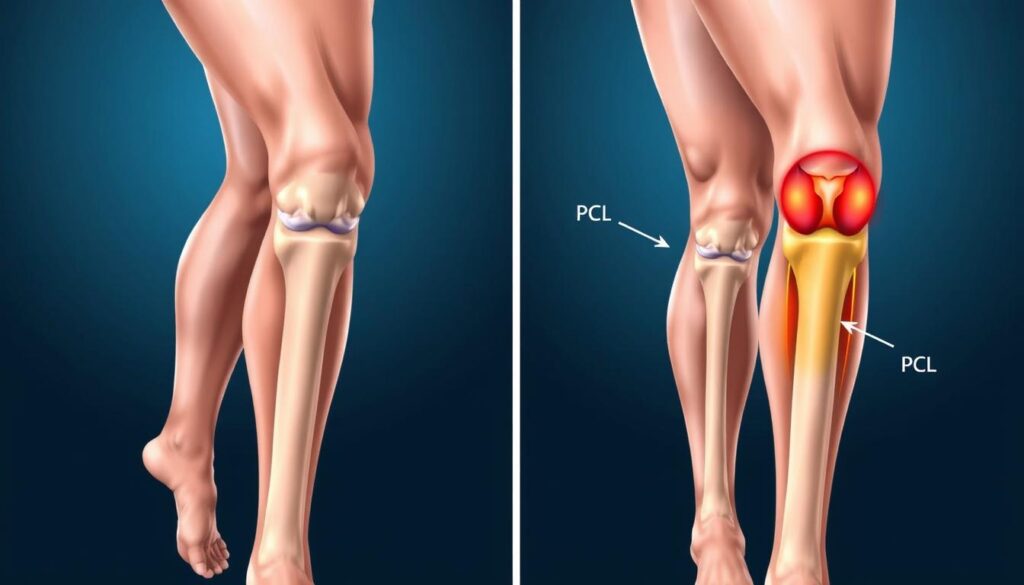
Arthritis
Arthritis is a broad term encompassing various conditions that cause joint inflammation. The two most common types affecting the knee are:
- Osteoarthritis (OA): A degenerative condition that gradually wears down the cartilage cushioning the joint surfaces. OA is often associated with aging and repetitive stress on the joint.
- Rheumatoid Arthritis (RA): An autoimmune disorder where the body’s immune system mistakenly attacks the joint tissues, leading to inflammation, pain, and potential joint deformity.
Show Image
Overuse and Tendonitis
Repetitive stress on the knee joint can lead to overuse injuries and conditions such as tendonitis. Common examples include:
- Runner’s knee: Pain around the kneecap (patella) often experienced by runners and cyclists.
- Jumper’s knee: Inflammation of the patellar tendon, frequently seen in athletes involved in jumping sports.
- Iliotibial (IT) band syndrome: Irritation of the IT band, a thick tissue that runs from the hip to the knee, common in long-distance runners.
Symptoms of Knee Pain
Knee pain manifests in various ways, depending on the underlying cause. Recognizing these symptoms is crucial for proper diagnosis and treatment. Here are the most common signs to watch for:
Swelling and Stiffness
Inflammation around the knee joint can lead to noticeable swelling and stiffness. This can make it challenging to bend or straighten the knee fully. Swelling may be localized to a specific area or affect the entire knee joint.
Redness and Warmth
In cases of acute inflammation or infection, the knee may appear red and feel warm to the touch. This is often accompanied by increased pain and tenderness.
Instability or Weakness
A sensation of the knee “giving out” or feeling unstable is often associated with ligament injuries or advanced stages of arthritis. This instability can significantly impact your ability to walk, climb stairs, or engage in physical activities.
Pain Patterns
The nature and location of knee pain can provide valuable clues about its underlying cause:
- Sharp, localized pain: Often indicative of a meniscus tear or ligament injury.
- Dull, aching pain: Commonly associated with osteoarthritis or overuse injuries.
- Pain behind the kneecap: Typically seen in cases of patellofemoral pain syndrome or chondromalacia patella.
- Pain when climbing stairs: Often experienced by individuals with osteoarthritis or patellar tendonitis.
Show Image
Treatment Options for Knee Pain
The approach to treating knee pain varies depending on the severity and underlying cause of the condition. Here are some effective treatment strategies:
Conservative Treatments
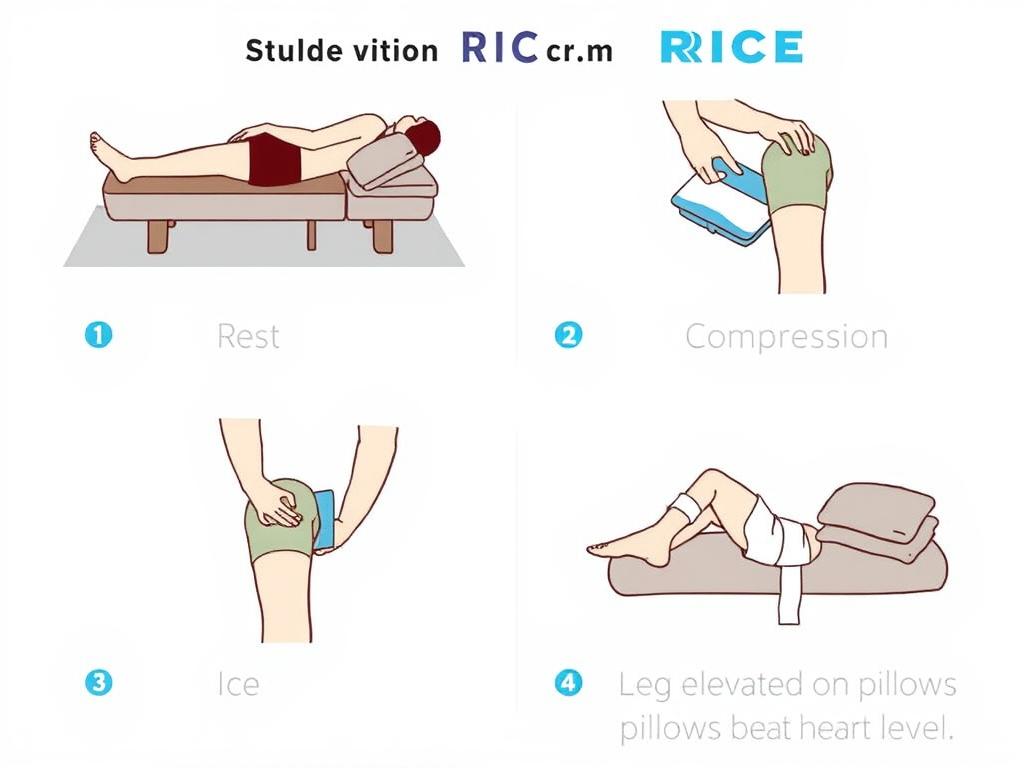
Rest, Ice, Compression, and Elevation (RICE)
For mild injuries or cases of overuse, the RICE method can be highly effective in alleviating pain and reducing swelling:
- Rest: Avoid activities that exacerbate the pain and give your knee time to heal.
- Ice: Apply cold packs to the affected area for 15-20 minutes at a time, several times a day.
- Compression: Use an elastic bandage to provide support and reduce swelling.
- Elevation: Keep your leg elevated above heart level when resting to minimize fluid accumulation.
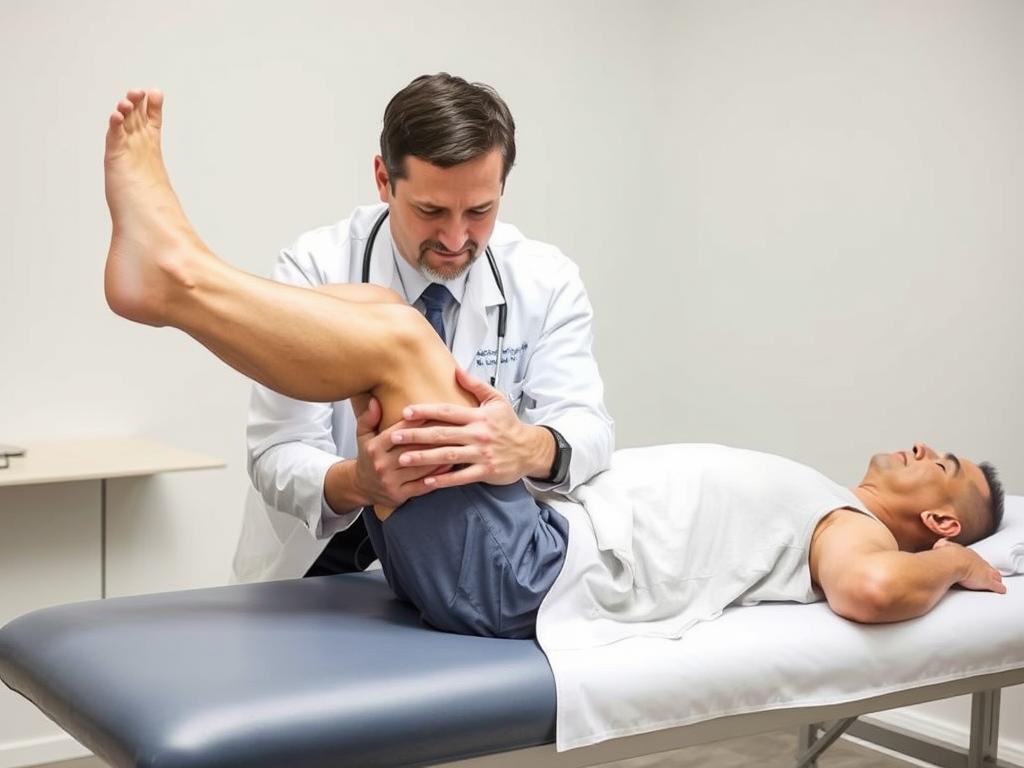
Physical Therapy
Physical therapy plays a crucial role in managing chronic knee pain and recovering from injuries. A tailored exercise program can:
- Strengthen the muscles supporting the knee joint, particularly the quadriceps and hamstrings.
- Improve flexibility and range of motion.
- Enhance overall knee stability and function.
- Reduce pressure on the joint through proper biomechanics.
Medications
Various medications can help manage knee pain and inflammation:
- Over-the-counter pain relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen can reduce pain and inflammation.
- Acetaminophen: Effective for pain relief without addressing inflammation.
- Topical medications: Creams or gels containing NSAIDs or capsaicin can provide localized pain relief.
For more severe cases, prescription medications may be necessary:
- Stronger NSAIDs
- Corticosteroid injections for rapid inflammation reduction
- Hyaluronic acid injections to improve joint lubrication in osteoarthritis cases
Surgical Interventions
When conservative treatments fail to provide adequate relief, surgical options may be considered:
- Arthroscopy: A minimally invasive procedure to diagnose and treat various knee conditions.
- Partial or total knee replacement: For severe cases of osteoarthritis or significant joint damage.
- Ligament reconstruction: To repair or replace damaged ligaments, such as in ACL tears.
Show Image
Preventing Knee Pain
Prevention is key to maintaining healthy knees and avoiding future problems. Here are some essential tips:
- Maintain a healthy weight: Excess weight puts additional stress on your knee joints, increasing the risk of osteoarthritis and other knee problems.
- Strengthen your leg muscles: Focus on exercises that target your quadriceps, hamstrings, and calf muscles to provide better support for your knees.
- Wear proper footwear: Choose shoes that provide adequate support and cushioning, especially during physical activities.
- Warm up and cool down: Before and after exercise, perform gentle stretches to improve flexibility and reduce the risk of injury.
- Use proper technique: When engaging in sports or physical activities, ensure you’re using correct form to minimize stress on your knees.
- Cross-train: Vary your exercise routine to avoid overuse injuries and strengthen different muscle groups.
- Listen to your body: If you experience persistent knee pain, don’t ignore it. Seek medical advice to prevent the condition from worsening.
Effectiveness of Treatment Options
To help you understand the potential benefits of various treatment approaches, we’ve compiled two tables comparing their effectiveness:
Table 1: Conservative Treatment Options
TreatmentPain ReliefInflammation ReductionImproved FunctionLong-term BenefitsRICE⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐Physical Therapy⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐OTC Medications⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐Prescription Medications⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐
Table 2: Surgical Treatment Options
Surgery TypePain ReliefFunctional ImprovementRecovery TimeLong-term OutcomeArthroscopy⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐Partial Knee Replacement⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐Total Knee Replacement⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐Ligament Reconstruction⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐⭐
Take Control of Your Knee Health Today!
Knee pain doesn’t have to dictate your life. Whether you’re dealing with a minor sprain or chronic arthritis, there are solutions available to help you regain your mobility and enjoy a pain-free life. Remember, early intervention is key to preventing long-term complications and achieving the best possible outcomes.
By understanding the causes of knee pain, recognizing its symptoms, and exploring various treatment options, you’re taking the first step towards better knee health. Don’t let knee pain hold you back from the activities you love or impact your quality of life.
Ready to Say Goodbye to Knee Pain?
The journey to a pain-free life starts with a single step. Don’t wait any longer to reclaim your mobility and well-being. Whether your goal is to return to your favorite sport, enjoy leisurely walks, or simply move through your day without discomfort, now is the time to act.
Take charge of your knee health by scheduling a consultation with a healthcare provider or physical therapist. They can assess your specific condition, provide an accurate diagnosis, and develop a personalized treatment plan tailored to your needs and goals.
Remember, every journey begins with a single step. Make that step today towards a future free from knee pain. Your knees have supported you throughout your life – now it’s time to give them the care and attention they deserve.
Act now, and open the door to a world of improved mobility, reduced pain, and enhanced quality of life. Your knees – and your future self – will thank you!