As we age, our joints start to wear down, and we become more susceptible to developing arthritis. Knee arthritis, specifically, is a common condition that affects millions of people worldwide. Osteoarthritis and rheumatoid arthritis are the two most common types of knee arthritis, and they both cause joint pain, stiffness, and limited movement.

Fortunately, there are several ways to prevent knee arthritis and maintain healthy joints. First and foremost, it’s essential to stay physically active. Regular exercise helps strengthen the muscles that provide support to the knees, relieve pain and stiffness, and reduce weight gain that puts excess stress on the knees. Additionally, maintaining a healthy weight and eating a balanced diet can also help prevent knee arthritis.
Understanding Arthritis in the Knee
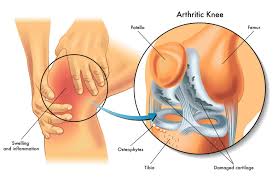
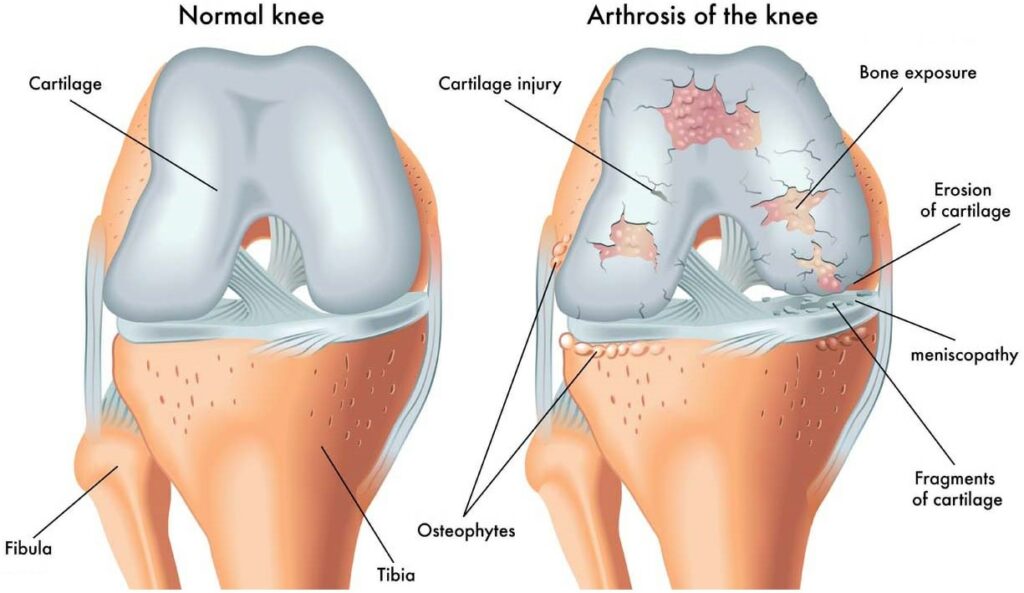
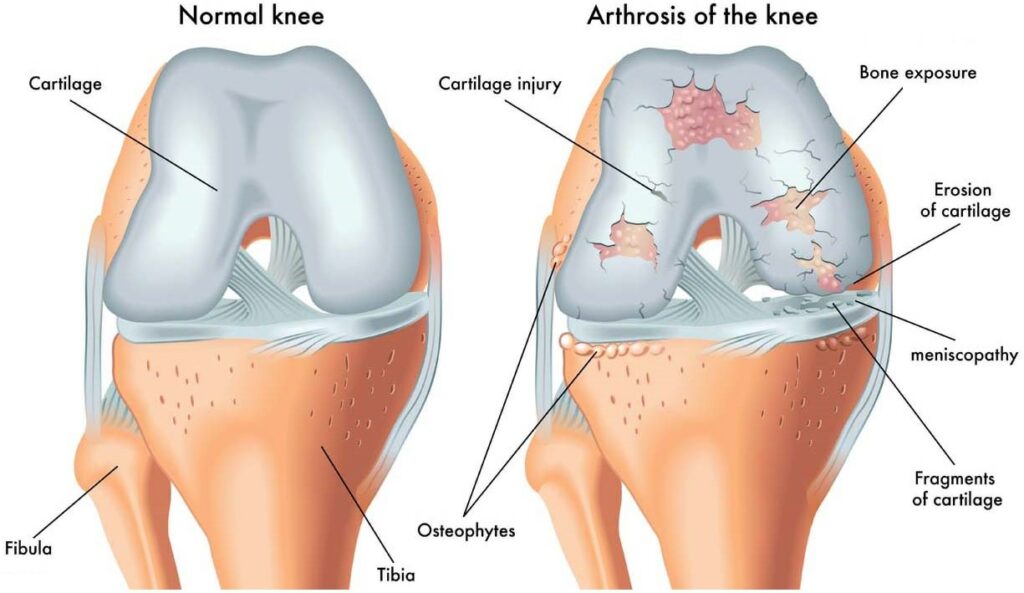
When it comes to preventing arthritis in the knee, it is important to first understand what arthritis is and how it affects the knee joint. Arthritis is a disease that causes inflammation in the joints, leading to pain, stiffness, and swelling. There are different types of arthritis, but the most common type that affects the knee joint is osteoarthritis.
Identifying Types and Symptoms
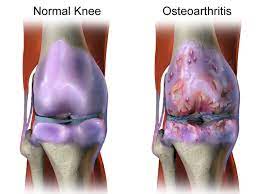
Osteoarthritis is a degenerative disease that occurs when the cartilage in the knee joint starts to wear away, causing the bones to rub against each other. This can lead to pain, stiffness, and swelling in the knee joint. Rheumatoid arthritis, on the other hand, is an autoimmune disease that can also affect the knee joint, causing inflammation and damage to the cartilage and bone. Symptoms of arthritis in the knee can include pain, swelling, stiffness, and limited range of motion.
Risk Factors and Causes
There are several risk factors that can increase the likelihood of developing arthritis in the knee. These include age, gender (men are more likely to develop knee arthritis than women), injury to the knee joint, obesity or excess weight, genetics, and overuse of the knee joint.
Diagnostic Procedures
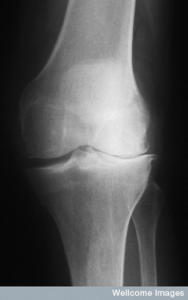
If you are experiencing symptoms of arthritis in the knee, it is important to seek medical attention. Your doctor may perform a physical exam to check for swelling, tenderness, and range of motion in the knee joint. They may also order diagnostic tests such as X-rays, MRI, CT scans, or blood tests to help confirm a diagnosis of arthritis in the knee.
In summary, understanding the different types of arthritis, its symptoms, and risk factors can help in preventing arthritis in the knee. Seeking medical attention and undergoing diagnostic procedures can also help in early detection and treatment of knee arthritis.
Prevention and Management Strategies

Arthritis in the knee can be a painful and debilitating condition that can affect your mobility and quality of life. Fortunately, there are several prevention and management strategies that can help you reduce the risk of developing arthritis in your knee or manage the symptoms if you already have the condition.
Lifestyle Modifications
One of the most effective ways to prevent arthritis in the knee is to adopt a healthy lifestyle. Maintaining a healthy weight through regular exercise and a healthy diet is essential as excess weight can put extra pressure on your knee joints. A Mediterranean-style diet rich in fruits, vegetables, whole grains, lean protein, and healthy fats can help reduce inflammation and promote joint health.
Smoking is also a risk factor for developing arthritis, so quitting smoking can also help reduce the risk. Reducing stress levels through relaxation techniques such as deep breathing, meditation, and yoga can also help reduce inflammation and promote joint health.
Medical Interventions
If you are experiencing knee pain or stiffness, it is important to seek medical attention promptly. Your doctor may prescribe medication or injections to help manage the pain and inflammation associated with arthritis.
In severe cases, surgery may be necessary to repair or replace damaged knee joints. Total knee replacement is a common surgical procedure that involves replacing the damaged joint with an artificial one.
Home Remedies and Supportive Care
In addition to medical interventions, there are several home remedies and supportive care strategies that can help manage the symptoms of arthritis in the knee. Rest, ice, compression, and elevation (RICE) can help reduce pain and swelling. Heat therapy can also help reduce pain and stiffness by increasing blood flow to the affected area.
Wearing a knee brace or using a cane or walker can help reduce pressure on the knee joint and improve mobility. Stretching and strengthening exercises can also help improve flexibility, range of motion, and joint health.
In conclusion, there are several prevention and management strategies that can help reduce the risk of developing arthritis in the knee or manage the symptoms if you already have the condition. By adopting a healthy lifestyle, seeking medical attention promptly, and practicing home remedies and supportive care, we can improve our joint health and reduce the impact of arthritis on our lives.
Frequently Asked Questions

What are the early symptoms of knee arthritis to look out for?
The early symptoms of knee arthritis may include pain, stiffness, swelling, and a reduced range of motion in the affected joint. If you experience any of these symptoms, it is best to consult a doctor for a proper diagnosis and treatment plan.
What natural methods are effective in avoiding arthritis?
There are several natural methods that can be effective in avoiding arthritis, such as maintaining a healthy weight, eating a balanced diet rich in anti-inflammatory foods, and getting regular exercise. Additionally, some dietary supplements like glucosamine and chondroitin may also be helpful in preventing arthritis.
What are the primary causes of arthritis and how can it be prevented?
The primary causes of arthritis include age, genetics, and wear and tear on the joints. While some factors like age and genetics cannot be changed, there are steps you can take to prevent arthritis or slow its progression. These include maintaining a healthy weight, getting regular exercise, and avoiding injury to the joints.
How can regular exercise contribute to preventing arthritis?
Regular exercise can help prevent arthritis by strengthening the muscles and bones around the joints, improving flexibility and range of motion, and reducing inflammation in the body. Exercise can also help maintain a healthy weight, which can reduce the stress on the joints.
Which dietary supplements are recommended for arthritis prevention?
Some dietary supplements that may be helpful in preventing arthritis include glucosamine, chondroitin, omega-3 fatty acids, and vitamin D. However, it is important to speak with a doctor before taking any supplements, as they may interact with other medications or have side effects.
What are the latest advancements in treating osteoarthritis of the knee?
There are several new treatments for osteoarthritis of the knee, including platelet-rich plasma (PRP) therapy, stem cell therapy, and hyaluronic acid injections. However, more research is needed to determine the long-term effectiveness of these treatments, and they may not be covered by insurance.