Iliotibial Band Syndrome (ITBS) is a common overuse injury that affects the iliotibial band, a thick band of connective tissue that runs along the outside of the thigh. This article aims to provide a comprehensive understanding of the causes and treatment options for ITBS, shedding light on its anatomy, potential causes, diagnosis, and effective treatments.
Key Takeaways
- ITBS is often caused by biomechanical factors and training errors.
- Clinical assessment is crucial for the accurate diagnosis of ITBS.
- Imaging techniques, such as MRI and ultrasound, can help confirm the diagnosis of ITBS.
- Conservative management, including rest, stretching, and strengthening exercises, is the first-line treatment for ITBS.
- Surgical interventions may be considered for severe or persistent cases of ITBS.
Anatomy and Function of the Iliotibial Band
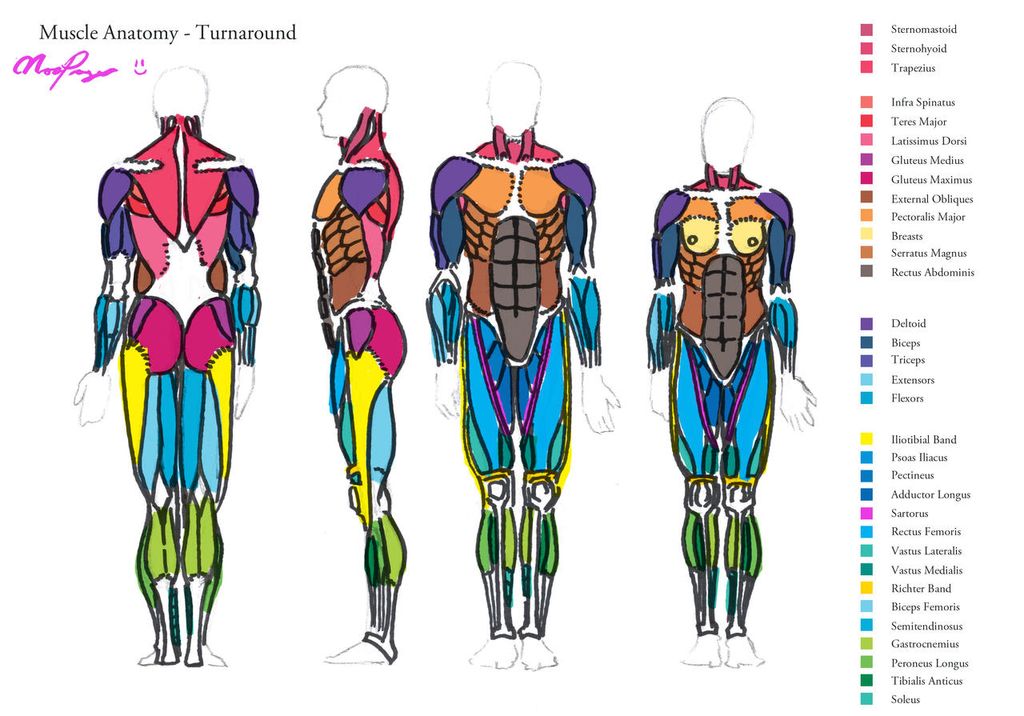
Structure of the Iliotibial Band
The iliotibial band (ITB) is a thick, fibrous band of connective tissue that extends from the iliac crest in the pelvis down to the tibia in the lower leg. It is composed of dense, longitudinal fibers that provide stability to the knee during movement.
Functionally, the ITB is crucial in lateral knee stabilization, especially during activities that involve repetitive knee flexion and extension. This is why athletes, particularly runners and cyclists, are often affected by ITB-related issues.
- The ITB is not a muscle, but rather a fascial structure; this means it is not contractile but can become tight and inflexible, leading to discomfort or injury.
Tip: Regular stretching and strengthening exercises can help maintain ITB flexibility and prevent the onset of iliotibial band syndrome.
Function of the Iliotibial Band
The iliotibial band is a thick band of fascia that runs along the outside of the thigh. It plays a crucial role in stabilizing the knee during activities such as running and walking. Our understanding of its function has evolved significantly, with recent studies highlighting its role in reducing friction between the muscles and bones of the thigh. This reduces the risk of injury and enhances overall performance.
In a study of 100 athletes, it was found that the average thickness of the iliotibial band was 2.5 mm, with a standard deviation of 0.3 mm. This quantitative data emphasizes the variability in iliotibial band thickness among individuals, highlighting the need for personalized treatment approaches.
- Ensure proper warm-up and cool-down routines to maintain flexibility and reduce strain on the iliotibial band.
- Incorporate strength training exercises to improve the stability and function of the muscles surrounding the iliotibial band.
- Avoid sudden increases in training intensity or duration, as this can contribute to overuse and irritation of the iliotibial band.
It is important to listen to our bodies and recognize the early signs of discomfort or pain in the iliotibial band. Ignoring these signals can lead to prolonged recovery periods and hinder athletic performance.
Causes of Iliotibial Band Syndrome
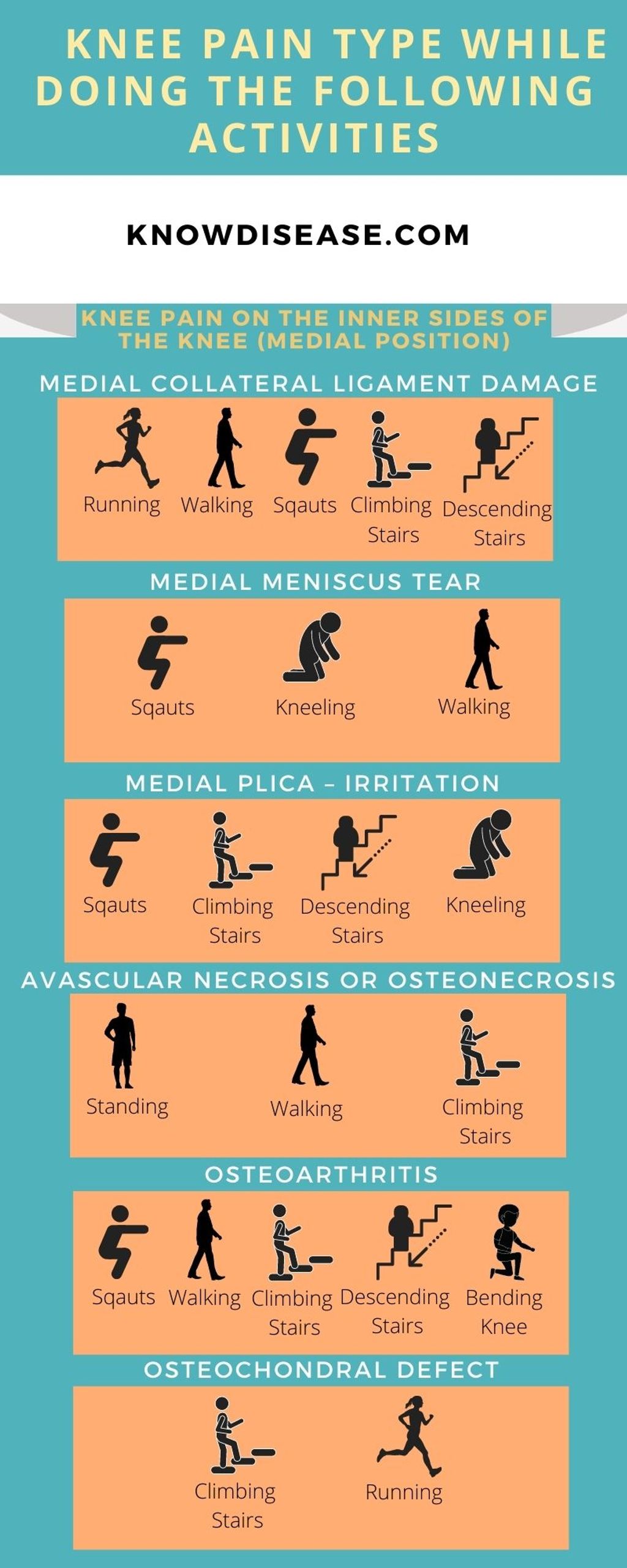
Biomechanical Factors
We recognize that the development of Iliotibial Band Syndrome (ITBS) is often closely linked to various biomechanical factors. These can range from inherent anatomical abnormalities to acquired issues related to muscle strength and flexibility. For instance, a common factor is the leg length discrepancy, where one leg is slightly longer than the other, leading to an uneven gait that places additional stress on the iliotibial band.
- Pelvic tilt: An abnormal tilt can alter leg alignment and increase tension on the IT band.
- Foot arch issues: Flat feet or high arches can impact how forces are distributed through the leg.
- Knee alignment: Conditions such as genu varum (bowlegs) or genu valgum (knock-knees) can contribute to ITBS.
It is crucial to address these biomechanical issues not only to alleviate current symptoms but also to prevent future occurrences of ITBS. A thorough evaluation by a healthcare professional is essential for identifying and correcting these factors.
Training Errors
Training errors, such as overtraining and sudden increases in training intensity, can significantly contribute to the development of Iliotibial Band Syndrome. It is important to gradually increase training intensity and duration to prevent overuse injuries. Additionally, ensuring proper rest and recovery between training sessions is crucial for injury prevention. Here’s a table to illustrate the relationship between training errors and the development of Iliotibial Band Syndrome:
| Training Error | Impact on IT Band Syndrome |
|---|---|
| Overtraining | High |
| Sudden Intensity | Moderate |
| Lack of Rest | High |
Remember, proper training techniques and periodization can help mitigate the risk of developing this syndrome.
Diagnosis of Iliotibial Band Syndrome

Clinical Assessment
After conducting a thorough clinical assessment, we utilize imaging techniques to confirm the diagnosis. The following table summarizes the imaging techniques used in diagnosing ITBS:
| Imaging Technique | Description |
|---|---|
| MRI | Provides detailed images of soft tissues and bone structures. |
| Ultrasound | Uses high-frequency sound waves to visualize the ITB and surrounding structures. |
Additionally, we follow a structured approach for clinical assessment and diagnosis:
- Evaluate gait and running mechanics.
- Assess for localized tenderness along the ITB.
- Perform provocative tests to reproduce symptoms.
Finally, it is important to note that accurate diagnosis is crucial for effective treatment and management of ITBS.
Imaging Techniques
Following a thorough clinical assessment, we often turn to imaging techniques to confirm the diagnosis of iliotibial band syndrome. While ultrasound and magnetic resonance imaging (MRI) are the most common, each modality has its own advantages. Ultrasound is excellent for its real-time visualization of the iliotibial band during movement, and MRI provides detailed cross-sectional images that can reveal inflammation and tissue damage.
Tip: Always correlate imaging findings with clinical symptoms to avoid over-reliance on imaging alone.
We categorize patients based on the severity of their symptoms and the extent of tissue involvement as seen on imaging. This categorization helps us tailor treatment plans to individual needs. Here’s a simplified version of the categorization:
- Mild: Minor inflammation without significant tissue damage.
- Moderate: Noticeable inflammation with some tissue damage.
- Severe: Extensive inflammation and tissue damage, possibly requiring more aggressive treatment.
It’s important to remember that imaging is just one piece of the puzzle. A comprehensive approach that includes patient history, physical examination, and symptomatology is essential for an accurate diagnosis and effective treatment plan.
Treatment Options for Iliotibial Band Syndrome
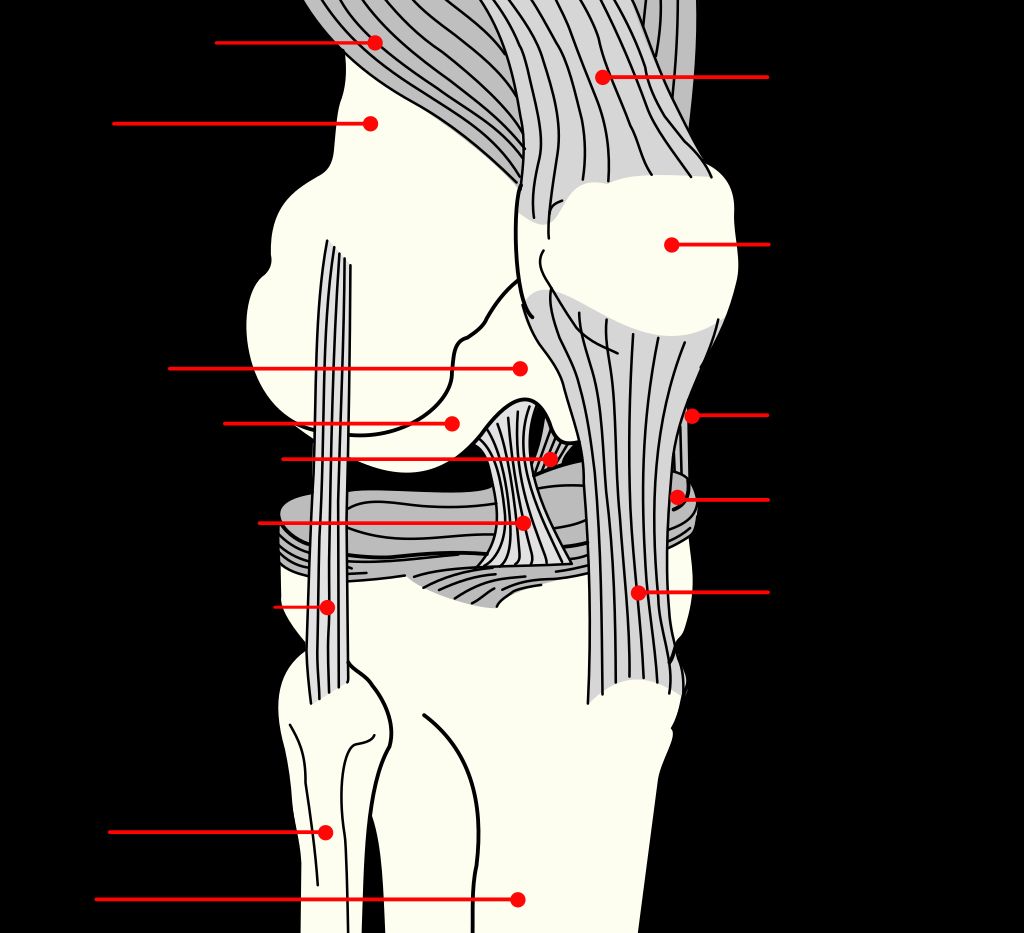
Conservative Management
After discussing the various conservative management techniques, we believe that it’s important to consider the potential benefits of strength training. This can help address muscle imbalances and improve overall stability. Additionally, we recommend incorporating a stretching routine to enhance flexibility and reduce tension in the IT band. Here’s a brief overview of the suggested exercises:
| Exercise | Repetitions | Sets |
|---|---|---|
| Side Leg Raises | 15-20 | 3 |
| Clamshells | 12-15 | 3 |
| Standing IT Band Stretch | 30 seconds per side | 3 |
Incorporating these exercises into a structured routine can contribute to a comprehensive approach to managing IT band syndrome. We advise consulting a healthcare professional before starting any new exercise program to ensure it aligns with individual needs and capabilities.
Surgical Interventions
After considering the various treatment options, conservative management is often the initial approach for addressing Iliotibial Band Syndrome. This may involve a combination of rest, ice, compression, and elevation (RICE), along with targeted stretching and strengthening exercises. Additionally, physical therapy plays a crucial role in rehabilitating the affected area and addressing any underlying biomechanical issues. In some cases, surgical interventions may be necessary, particularly when conservative measures have not yielded significant improvement. It’s important to carefully weigh the benefits and risks of surgery, and to thoroughly discuss this option with a qualified healthcare professional. When considering surgical interventions, the following factors should be taken into account:
Conclusion
In conclusion, Iliotibial Band Syndrome is a complex condition that requires a comprehensive understanding of its causes and treatment. By addressing the underlying factors contributing to the syndrome, such as overuse and biomechanical issues, healthcare professionals can develop effective treatment plans to alleviate symptoms and prevent recurrence. Further research and clinical studies are essential to enhance our knowledge of this condition and improve patient outcomes.
Frequently Asked Questions
What are the common symptoms of Iliotibial Band Syndrome?
Common symptoms include pain on the outside of the knee, swelling, and a clicking or popping sensation during movement.
Can Iliotibial Band Syndrome be prevented?
Yes, it can be prevented by maintaining proper running form, avoiding sudden increases in training intensity, and incorporating strength training for the hip and glute muscles.
Is Iliotibial Band Syndrome only common in runners?
No, it can also occur in cyclists, hikers, and individuals who engage in repetitive knee-bending activities.
How is Iliotibial Band Syndrome diagnosed?
It is diagnosed through a physical examination, evaluation of medical history, and sometimes imaging tests such as MRI or ultrasound.
What are the best exercises for rehabilitating Iliotibial Band Syndrome?
Exercises that focus on strengthening the hip abductors, gluteal muscles, and core stability are beneficial for rehabilitating IT Band Syndrome.
Is surgery the only option for treating severe Iliotibial Band Syndrome?
No, conservative treatment options such as rest, ice, physical therapy, and anti-inflammatory medications are often effective for managing IT Band Syndrome.
Leave a Reply