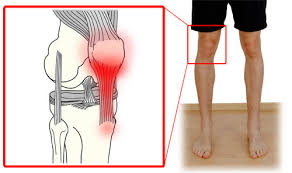
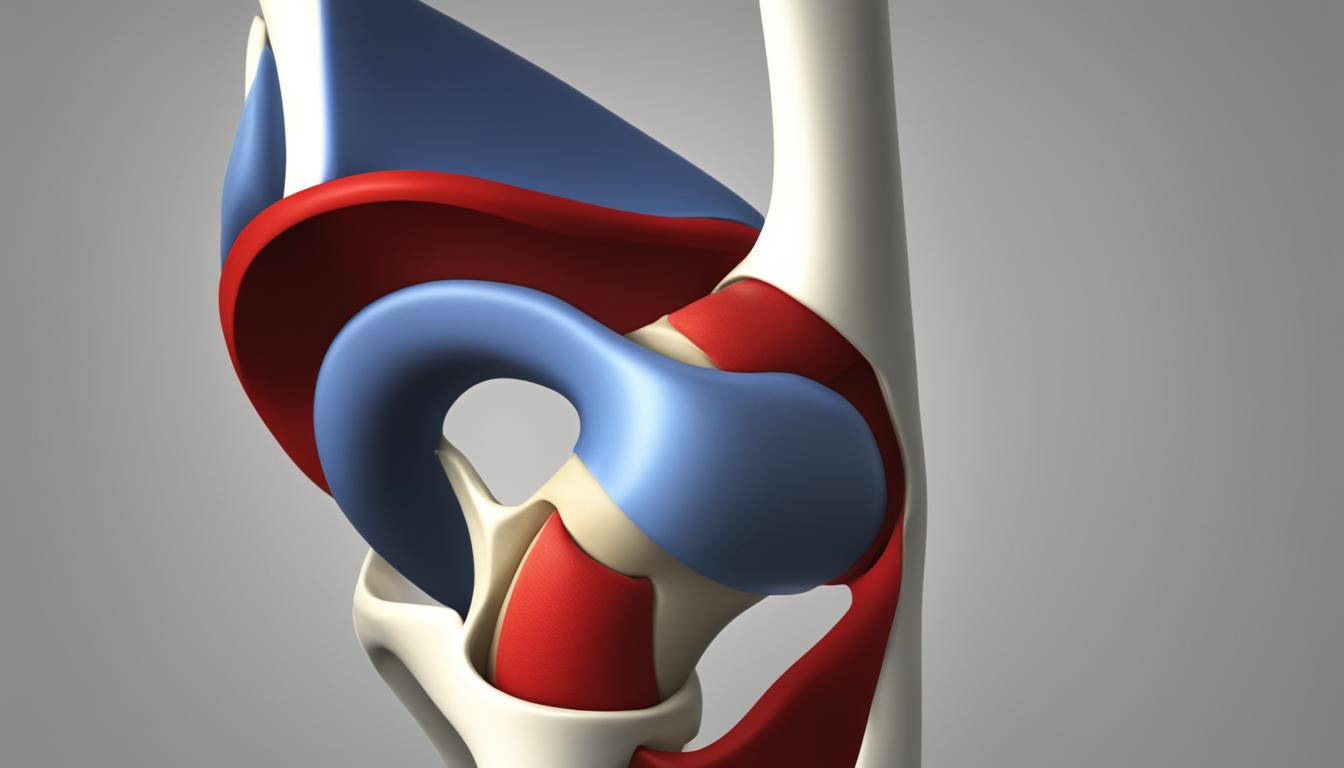
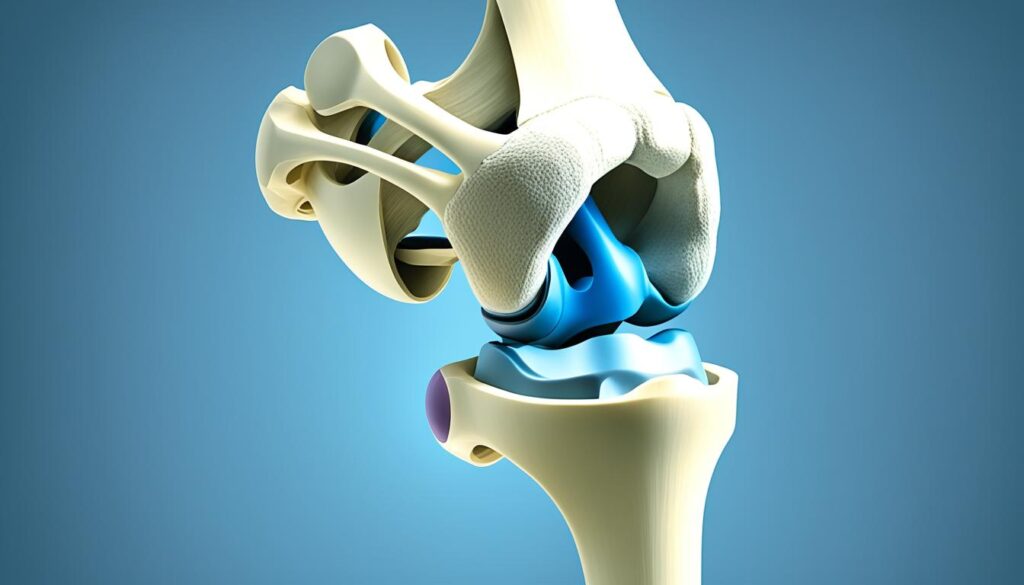
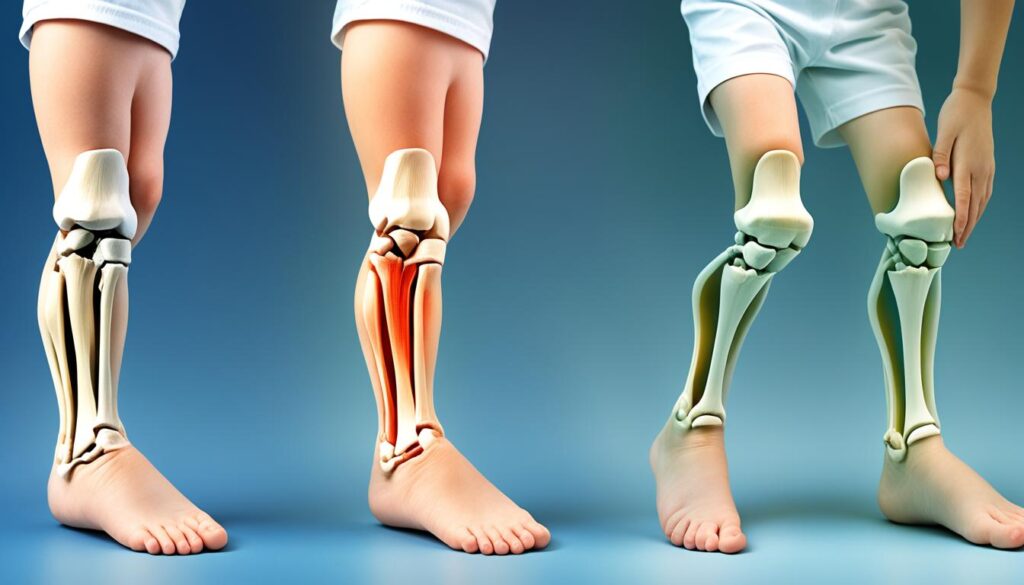
Did you know that the patella tendon, also known as the patellar ligament, is a strong cord of fibrous tissue that connects the bottom of the kneecap (patella) to the top of the shinbone (tibia)? This small but mighty tendon plays a crucial role in the functioning of our knees, allowing us to perform various movements such as walking, running, and jumping.
The anatomy of the patella tendon involves a complex network of fibers, which work together with the quadriceps muscles to extend the knee. It is responsible for transmitting the force generated by the quadriceps to the lower leg during leg extension, making it essential for everyday activities and sports performance.
Despite its importance, the patella tendon is prone to injuries such as tendinitis, tears, and fractures. These injuries can cause significant pain, swelling, and difficulty in walking, impacting our ability to lead an active lifestyle.
In this article, we will explore the functions of the patella tendon, common injuries, treatment options, and preventive measures to ensure the health and well-being of our knees. Whether you are an athlete or simply concerned about knee health, understanding the patella tendon is crucial for maintaining optimal performance and preventing injuries. Let’s dive in!
Functions of the Patellar Tendon
The patellar tendon, also known as the patellar ligament, plays a crucial role in the proper functioning of the knee joint. It serves several essential functions that are vital for lower extremity strength and power.
The primary function of the patellar tendon is to transmit the force generated by the quadriceps muscles to the lower leg, allowing for the extension of the knee. This transmission of force enables movements such as walking, running, jumping, and kicking. Without the patellar tendon, the knee would not be able to effectively straighten, significantly hampering these activities.
The patellar tendon acts as a rope-like structure, connecting the kneecap (patella) to the shinbone (tibia). It provides stability to the knee joint, preventing excessive movements during dynamic activities. This stability is crucial for maintaining balance and preventing injuries during movements that place stress on the knee.
Furthermore, the patellar tendon contributes to the overall alignment and tracking of the patella within the femoral groove. It helps to distribute forces evenly across the joint, reducing the chances of uneven wear and tear on the joint surfaces.
In summary, the patellar tendon functions as a transmitter of force, stabilizer of the knee joint, and contributor to the alignment and tracking of the patella. Its proper functioning is essential for the performance and integrity of the knee during activities that require lower extremity strength and power.

- Calmbach, W., & Hutchens, M. (2003). Evaluation of patients presenting with knee pain: Part I. History, physical examination, radiographs, and laboratory tests. American Family Physician, 68(5), 907-912. Retrieved from https://www.aafp.org/afp/2003/0901/p907.html
- Nielsen, R. (2016). Patellar Tendinopathy in Athletes: Current Diagnostic and Therapeutic Recommendations. Sports Medicine, 46(11), 1685-1696. doi: 10.1007/s40279-016-0538-8
Patellar Tendon Injuries and Treatment
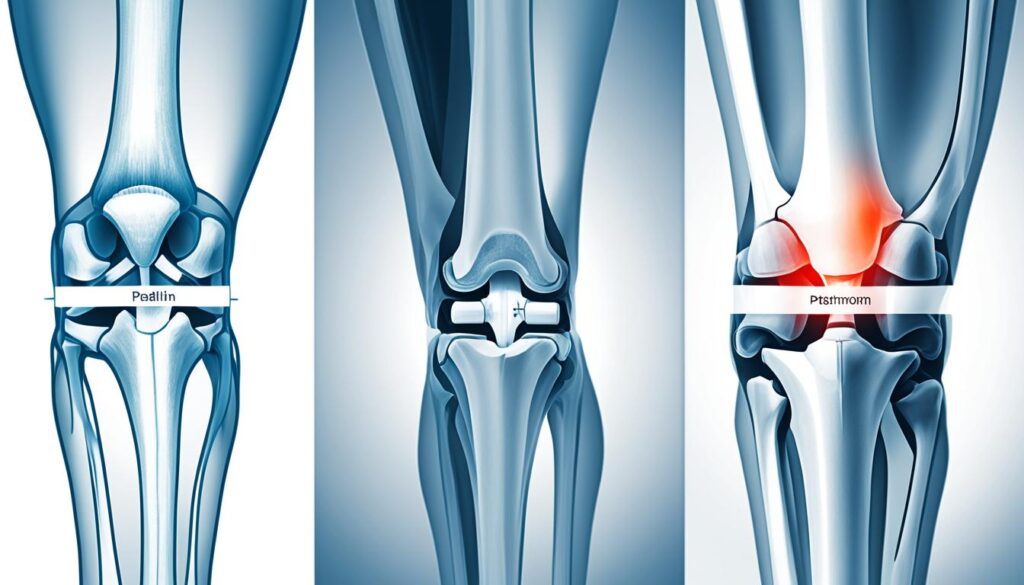
Patellar tendon injuries can range from minor tears and tendinitis to complete ruptures. When the patellar tendon becomes inflamed, it leads to a condition called patella tendonitis, which is characterized by pain, tenderness, and swelling in the front of the knee.
Conservative treatment options for patellar tendon injuries often involve rest, ice, physical therapy, and the use of braces or immobilizers to reduce pain and promote healing. Physical therapy plays a crucial role in patellar tendon rehabilitation, focusing on strengthening the surrounding muscles, improving flexibility, and restoring normal range of motion.
In some cases, conservative measures may not be sufficient, especially in severe injuries or when the tendon fails to respond to non-surgical interventions. In such cases, patellar tendon surgery may be necessary. Surgical options may include tendon repair, in which the torn or damaged portion of the tendon is sewn back together, or tendon reconstruction, in which a tendon graft is used to replace the damaged section.
The recovery timeframe for patellar tendon injuries can vary depending on the severity of the injury and the individual’s commitment to the rehabilitation process. Generally, it can take several weeks to months for full recovery after surgery, while non-surgical treatment may require a shorter recovery period.
“Patellar tendon injuries require a comprehensive approach that combines appropriate medical intervention and rehabilitation strategies. It is important to seek timely medical attention and adhere to prescribed treatments to ensure the best possible outcome.”
Risk Factors and Prevention of Patellar Tendon Injuries
When it comes to patellar tendon injuries, there are several factors that can increase the risk of developing this condition. Understanding these risk factors is essential for taking proactive measures to prevent patellar tendon injuries and maintain optimal knee health.
Risk Factors:
- Participating in activities that involve repetitive jumping, such as basketball or volleyball.
- Sudden increases in activity level without proper conditioning or training.
- Tight leg muscles, especially in the quadriceps and hamstrings.
- Muscular imbalances, where certain muscles overpower others, placing excessive strain on the patellar tendon.
- Chronic illnesses, such as kidney failure or diabetes, which can weaken the tendons and make them more prone to injury.
- The use of certain medications, such as fluoroquinolone antibiotics, which have been associated with an increased risk of tendon injuries.
Prevention:
- Gradually increase activity levels: When starting a new exercise program or engaging in high-impact activities, it’s important to gradually increase the intensity and duration to allow your body to adapt.
- Maintain proper muscle balance and flexibility: Incorporate stretching and strengthening exercises for the quadriceps, hamstrings, and calf muscles to improve overall muscle balance and flexibility.
- Warm up before exercise: Perform a dynamic warm-up routine that includes movements targeting the lower body, such as leg swings and knee lifts, to improve blood flow and prepare the muscles for activity.
- Use proper techniques: Practice proper form and technique when engaging in physical activities to minimize excessive stress on the patellar tendon. Seek guidance from a qualified trainer or coach if needed.
- Listen to your body’s warning signs: Pay attention to any pain or discomfort in the knee area during or after physical activity. If you experience persistent pain or notice any changes in the knee joint, consult a healthcare professional for a proper diagnosis and appropriate treatment.
“Prevention is key when it comes to protecting the patellar tendon.”
Conclusion
The patellar tendon, also known as the patellar ligament, is a critical structure that plays a vital role in knee joint function. Its primary function is to transmit the force generated by the quadriceps muscles, allowing for the extension of the knee. By connecting the kneecap to the shinbone, the patellar tendon provides stability during various activities such as walking, running, and jumping.
However, the patellar tendon is susceptible to injuries, ranging from tendinitis to complete tears. Symptoms of patellar tendon injury include pain, tenderness, and swelling in the front of the knee. Treatment options for patellar tendon injuries are dependent on the severity and may include physical therapy, bracing, or surgical intervention. Rehabilitation plays a crucial role in the recovery process, with exercises focusing on strengthening the surrounding muscles and gradually increasing the tendon’s load-bearing capacity.
Prevention is key in minimizing the risk of patellar tendon injuries. Incorporating proper warm-up routines, maintaining muscle balance and flexibility, and avoiding excessive stress on the tendon can significantly reduce injury occurrence. It is important to seek the guidance of a healthcare professional if you experience any symptoms or have concerns about your patellar tendon. Early diagnosis and appropriate treatment can help prevent further complications and aid in a faster recovery.
FAQ
What is the patella tendon?
The patella tendon, also known as the patellar ligament, is a strong cord of fibrous tissue that connects the bottom of the kneecap (patella) to the top of the shinbone (tibia).
What are the functions of the patellar tendon?
The primary function of the patellar tendon is to transmit the force generated by the quadriceps muscles to the lower leg, allowing for the extension of the knee. It acts as a rope-like structure, connecting the patella to the tibia and stabilizing the knee joint during movements such as walking, running, jumping, and kicking.
What are the symptoms of patella tendonitis?
Symptoms of patella tendonitis, which is inflammation of the patellar tendon, include pain, tenderness, and swelling in the front of the knee.
How are patellar tendon injuries treated?
Treatment options for patellar tendon injuries often involve rest, ice, physical therapy, and the use of braces or immobilizers. In severe cases or when conservative measures fail, surgical options such as tendon repair or reconstruction may be necessary.
How long does it take to recover from a patellar tendon injury?
The recovery timeframe for patellar tendon injuries varies depending on the severity of the injury and the individual’s adherence to rehabilitation protocols.
What are the risk factors for developing patellar tendon injuries?
Several factors can increase the risk of developing patellar tendon injuries, including participating in activities that involve repetitive jumping, sudden increases in activity level, tight leg muscles, muscular imbalances, chronic illnesses (such as kidney failure or diabetes), and the use of certain medications.
How can patellar tendon injuries be prevented?
To prevent patellar tendon injuries, it is important to gradually increase activity levels, maintain proper muscle balance and flexibility, warm up before exercise, use proper techniques, and listen to your body’s warning signs of pain and discomfort.
Why is understanding the patellar tendon important?
The patellar tendon is a crucial structure in the knee joint that plays a vital role in leg extension and stability. Understanding its functions, common injuries, and treatment options is important for maintaining optimal knee health and performance.