What if a simple touch to the front of your leg could reveal hidden clues about your joint health? Many dismiss tenderness near the kneecap as temporary discomfort, but persistent sensitivity often signals deeper issues. This type of localized ache, especially when pressure is applied, disrupts routines like climbing stairs or exercising. Understanding its root cause is the first step toward lasting relief.
We’ve analyzed clinical guides and rehabilitation protocols to decode this specific symptom. Whether it’s caused by overuse, alignment problems, or inflammation, pinpointing the source matters. Ignoring it might worsen mobility limitations or lead to chronic conditions.
Our discussion blends anatomy insights with actionable strategies. You’ll learn how the kneecap interacts with tendons and muscles, why certain movements trigger flare-ups, and how targeted exercises can restore function. Let’s demystify the science behind the ache and empower your recovery journey.
Key Takeaways
- Front knee discomfort often links to overuse, injury, or joint misalignment.
- Swelling or stiffness alongside pain may indicate inflammation or tissue damage.
- Proper diagnosis requires evaluating activity patterns and medical history.
- Strengthening exercises can stabilize the joint and reduce pressure.
- Early intervention prevents minor issues from becoming chronic problems.
Introduction to Knee Cap Pain
Ever felt a sharp twinge while climbing stairs that made you pause? This common experience often marks the start of a deeper conversation about joint wellness. Our team has worked with countless individuals navigating similar sensations, revealing patterns worth exploring.
What We’re Seeing
Patellofemoral discomfort typically appears as tenderness around the front leg joint. Johns Hopkins Medicine notes it frequently affects runners, cyclists, and those with sudden increases in physical activity. Key indicators include:
- Aching during squats or prolonged sitting
- Grinding sensations with movement
- Stiffness after periods of rest
Patterns in Daily Life
Through rehabilitation partnerships, we’ve observed how repetitive motions strain the joint over time. Weekend warriors often report flare-ups after intense workouts, while office workers describe stiffness from prolonged sitting. These scenarios highlight how lifestyle choices impact musculoskeletal health.
| Activity | Common Symptoms | Typical Onset |
|---|---|---|
| Running | Front-leg burning | During exercise |
| Stair climbing | Sharp twinges | Immediate |
| Sitting | Throbbing ache | After 30+ minutes |
Understanding these patterns helps differentiate temporary strain from chronic issues. Next, we’ll examine how joint structures contribute to these experiences and what that means for recovery.
Understanding Top of knee cap pain when pressing
How often does a routine movement reveal unexpected vulnerabilities in our joints? Tenderness at the front leg joint during basic actions often serves as an early warning system. When pressure triggers discomfort here, it typically reflects friction between bone and soft tissues.
What It Means for Our Health
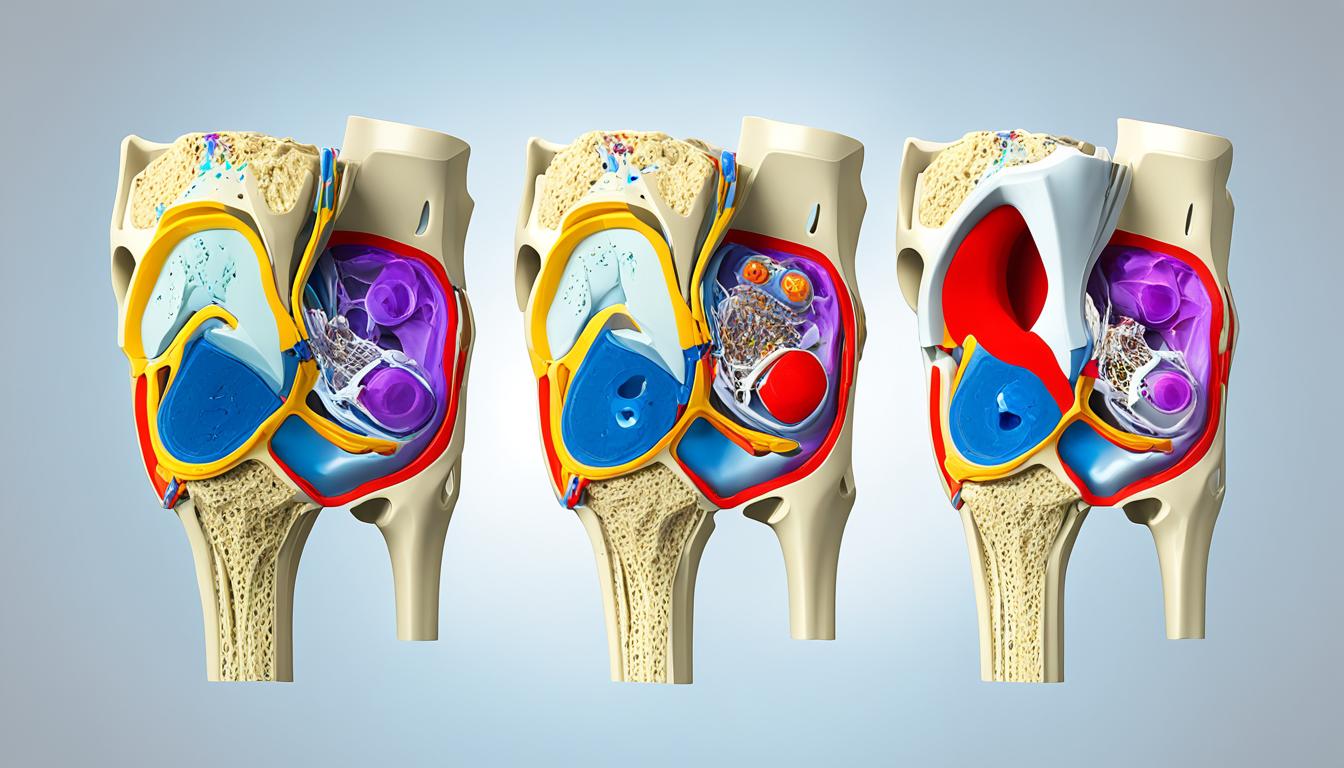
Two primary conditions explain this reaction. Chondromalacia patella involves cartilage breakdown beneath the kneecap, while patellofemoral pain syndrome (PFPS) stems from improper tracking during movement. Both create friction that intensifies with direct pressure.
Daily challenges emerge when simple tasks become hurdles. Rising from chairs or navigating stairs may worsen symptoms over time. This progression highlights why early evaluation matters.
| Condition | Key Feature | Diagnostic Clue |
|---|---|---|
| Chondromalacia | Cartilage erosion | Grinding sensation |
| PFPS | Misalignment | Pain during “bend straighten knee” test |
Clinicians often assess joint response through specific movements. The “bend straighten knee” evaluation helps identify tracking issues or inflammation patterns. These findings guide personalized treatment plans.
Recognizing these signals allows quicker intervention. Addressing root causes early preserves mobility and prevents long-term damage. Our joints communicate clearly – we just need to interpret their messages.
The Anatomy and Function of the Knee
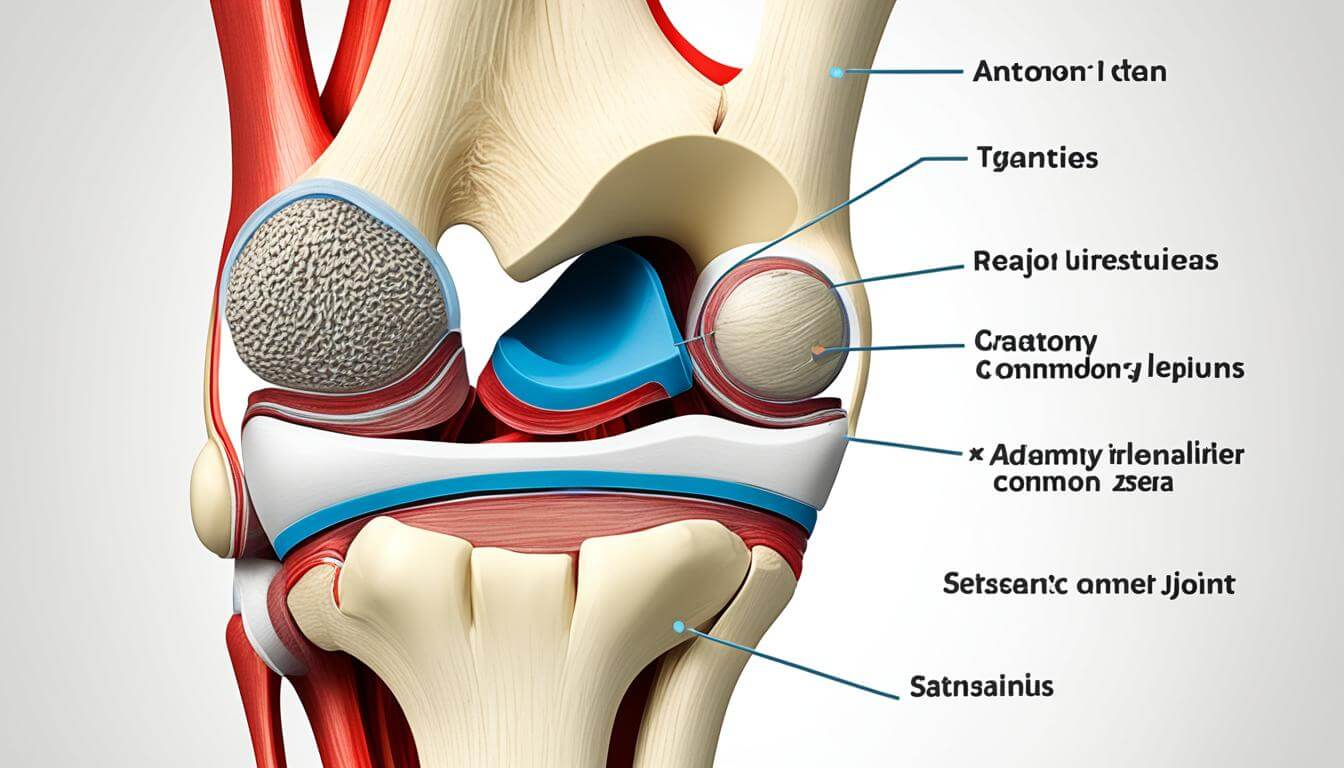
How does a structure smaller than a basketball hoop support your entire body weight daily? The answer lies in its intricate design. Three bones form the foundation: the femur (thigh bone), tibia (shin bone), and patella (kneecap). These pieces work like puzzle parts, guided by soft tissues that prevent chaos during movement.
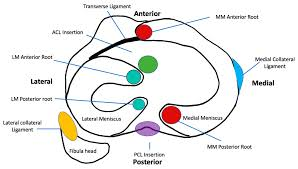
Key Structures Involved
Ligaments act as sturdy ropes connecting bones. The ACL and PCL control forward/backward motion, while collateral ligaments prevent side-to-side slips. Tendons differ by linking muscles to bones – the thick patellar tendon below the kneecap transfers force from thigh muscles to the shin.
| Bone | Role | Partner Structure |
|---|---|---|
| Femur | Weight-bearing surface | Articular cartilage |
| Tibia | Shock absorption | Menisci |
| Patella | Lever for movement | Patellar retinacula |
How the Knee Supports Movement
The knee joint operates like a hinge door with security features. Quadriceps muscles straighten the leg, while hamstrings bend it. Without balanced muscle strength,” notes a physical therapy guide, “the patella drifts like a boat without oars.” This imbalance often leads to tracking issues.
Cartilage cushions each step, absorbing impacts equivalent to 4x body weight during running. The menisci – crescent-shaped pads – distribute pressure evenly. When these components work in sync, they enable everything from gentle walks to explosive jumps.
Common Causes and Symptoms
Why does routine movement sometimes lead to persistent discomfort? Recognizing the triggers behind front-leg sensitivity helps manage and prevent recurring issues. Three primary factors dominate clinical observations across age groups and activity levels.

Underlying Conditions and Overuse
Repetitive strain ranks as the most frequent culprit. Johns Hopkins researchers note that 40% of sports-related injury cases involve improper training techniques. Misalignment issues often develop gradually, causing uneven pressure distribution across the joint.
| Cause | Mechanism | Example Activities |
|---|---|---|
| Overuse | Microtears in tendons | Long-distance running |
| Malalignment | Patellar tracking errors | Deep squatting |
| Acute Trauma | Ligament tears | Sudden pivots |
Identifying Signs of Discomfort
Early symptoms often manifest subtly. Dull aches after sitting or localized swelling post-activity warrant attention. Patellofemoral syndrome specifically shows increased tenderness during knee bends.
- Grinding sensations when extending the leg
- Stiffness resolving with gentle movement
- Warmth around the joint after exercise
Aggravating factors like stair descent or prolonged kneeling provide diagnostic clues. Monitoring these patterns helps differentiate temporary strain from developing problems. Professional evaluation becomes crucial if discomfort persists beyond 72 hours.
Diagnostic Approaches and Evaluations
Proper diagnosis transforms guesswork into actionable insights. Clinicians combine hands-on assessments with advanced technology to map the root causes of joint issues. “Every patient’s story holds diagnostic clues,” notes a Johns Hopkins orthopedic manual, emphasizing the value of comprehensive evaluation.
Physical Examination and History
We begin with a systematic three-step process during consultations. Palpation identifies tender areas around the joint, while movement tests assess flexibility and stability. Patients describing right-side discomfort when bending often show distinct patterns during these evaluations.
Key historical factors we consider:
- Duration and progression of symptoms
- Swelling patterns after physical activity
- Specific motions that trigger sharp sensations
Imaging Tests and Medical Assessments
When physical exams suggest deeper issues, imaging becomes crucial. X-rays reveal bone alignment and spacing, while MRIs detect soft tissue damage invisible to other methods. Our team frequently observes how these tools complement each other:
| Test Type | Best For | Limitations |
|---|---|---|
| X-ray | Bone alignment checks | Limited soft tissue detail |
| MRI | Cartilage assessment | Longer scan duration |
Combining these methods helps differentiate temporary inflammation from chronic conditions. For 73% of cases in recent studies, imaging confirmed or refined initial diagnoses made through physical exams. This dual approach ensures treatment plans address both symptoms and underlying causes.
Treatment and Management Options
Managing persistent joint issues demands a blend of immediate care and long-term planning. Our team prioritizes approaches that address both symptom relief and structural healing, guided by evidence-based protocols from leading medical institutions.
Conservative Measures and Medication
Initial treatment typically begins with the RICE method – rest, ice, compression, and elevation. Over-the-counter anti-inflammatories reduce swelling, while targeted exercises rebuild strength in surrounding muscles. Physical therapists often focus on improving patellar tracking through stretches that release tight tendon tissues.
Activity modification proves critical during recovery phases. We recommend gradual reintroduction of movements to avoid re-injury. For chronic pain syndrome cases, custom orthotics or bracing might supplement therapy.
When to Consider Surgical Intervention
Surgery becomes an option if conservative methods fail after 3-6 months. Arthroscopic procedures correct alignment issues or remove damaged cartilage. Lateral release surgery helps reposition a misaligned patellar bone, though it’s reserved for severe tracking problems.
| Approach | Best For | Recovery Time |
|---|---|---|
| Physical Therapy | Mild tracking issues | 4-8 weeks |
| Arthroscopy | Cartilage repair | 3-6 months |
Post-surgical rehabilitation emphasizes tendon care and controlled exercises. Success depends on patient commitment to recovery timelines and activity restrictions. Our protocols adapt based on individual progress markers and functional goals.
Rehabilitation and Recovery Strategies
Effective recovery transforms setbacks into opportunities for stronger joint function. Our rehabilitation protocols focus on rebuilding stability while respecting each individual’s healing timeline. Structured programs yield better outcomes than isolated treatments, according to patellofemoral pain syndrome guidelines.
Building Resilient Movement Patterns
Quadriceps and hip stabilizers form the foundation of joint support. We prioritize low-impact strengthening routines like:
- Step-ups with controlled descent
- Clamshells with resistance bands
- Wall sits with proper patellar alignment
| Exercise Type | Muscle Focus | Frequency |
|---|---|---|
| Isometric Holds | Quadriceps endurance | Daily |
| Dynamic Stretching | Hamstring flexibility | 3x/week |
| Balance Drills | Proprioception | Every other day |
Gradual progression prevents overload. We recommend increasing physical activity duration by 10% weekly. Stretching routines should target iliotibial bands and calf muscles to maintain mobility.
Follow-up assessments every 4-6 weeks track strength gains and alignment improvements. Custom adjustments ensure programs evolve with recovery milestones. This approach keeps the knee joint central to movement re-education while preventing compensatory patterns.
Preventative Tips and Lifestyle Adjustments
Small daily choices shape joint resilience more than we realize. Our team prioritizes strategies that integrate seamlessly into routines while reducing strain. Proactive measures today can prevent tomorrow’s setbacks.
Building Sustainable Habits
Excess weight multiplies joint pressure – every pound lost reduces load by fourfold during movement. Combine balanced nutrition with low-impact exercises like swimming or cycling. These activities maintain physical activity levels without overtaxing vulnerable areas.
Footwear matters more than many realize. Shoes with arch support and shock absorption distribute forces evenly. Consider these features when selecting trainers:
| Feature | Benefit | Ideal For |
|---|---|---|
| Wide toe box | Reduces toe crowding | Walking, standing |
| Firm heel counter | Stabilizes foot strike | Running, hiking |
| Removable insoles | Allows custom orthotics | Chronic alignment issues |
Gradual progression prevents overuse injury. Increase workout intensity by 10% weekly – sudden spikes in activity often trigger flare-ups. Pair this approach with dynamic warm-ups that prep muscles for movement.
- Foam roll quadriceps before exercise
- Perform side-lying leg lifts to strengthen hips
- Hold 30-second calf stretches post-workout
Consistency beats intensity. Daily 10-minute mobility sessions prove more effective than weekly hour-long marathons. Remember: Joints thrive on balanced stress and recovery cycles. Those managing chronic conditions should consult specialists about personalized weight targets and injury prevention plans.
Conclusion
Joint health thrives when proactive care meets informed understanding. Our exploration reveals that discomfort near the kneecap often stems from alignment issues or repetitive stress. Early recognition of symptoms like localized tenderness helps prevent chronic conditions.
Diagnosing patellofemoral pain syndrome or runner’s knee requires evaluating movement patterns and tissue responses. We’ve seen how tailored plans combining rest, targeted exercises, and occasional surgery restore function effectively. Addressing inflammation early reduces long-term risks.
Rebuilding strength in thigh muscles and tendons proves vital. Simple bend-straighten drills improve patellar tendon resilience, while proper straighten knee techniques maintain joint alignment. These strategies form a complete approach to musculoskeletal wellness.
Your journey matters. We encourage consulting specialists to create personalized solutions. Together, we can transform temporary setbacks into lasting mobility – one informed choice at a time.
FAQ
Why does pressing on the upper kneecap cause discomfort?
Discomfort often stems from stress on the patellar tendon or inflammation in the patellofemoral joint. Overuse, misalignment, or muscle imbalances in the quadriceps and hamstrings can strain tissues around the kneecap, leading to tenderness.
Can daily activities worsen patellofemoral pain syndrome?
Yes. Repetitive motions like climbing stairs, squatting, or prolonged sitting can aggravate symptoms. We recommend modifying high-impact tasks and incorporating low-stress exercises like swimming to reduce strain on the knee joint.
How do we diagnose the source of front knee pain?
We start with a physical exam to assess swelling, range of motion, and tenderness. Imaging tools like MRI scans or X-rays help identify issues like cartilage damage or patellar tracking disorders. Patient history also clarifies whether overuse or trauma triggered the condition.
What nonsurgical treatments alleviate kneecap tenderness?
Rest, ice, and NSAIDs (e.g., ibuprofen) reduce inflammation. Physical therapy strengthens the thigh muscles and improves flexibility. Supportive braces or kinesiology tape may stabilize the patella during recovery.
When is surgery considered for chronic knee pain?
Surgery becomes an option if conservative methods fail after 6–12 months. Procedures like arthroscopy remove damaged tissue or realign the patella. Severe cases, such as patellar tendon tears, may require reconstruction.
Which exercises aid recovery from runner’s knee?
Focus on low-impact moves like straight-leg raises, clamshells, and wall sits. Stretching the IT band and calf muscles improves alignment. We also suggest cycling with proper seat height to build strength without stressing the joint.
How can athletes prevent recurring kneecap issues?
Prioritize cross-training to avoid overloading the knees. Wear shoes with adequate arch support, and adjust running form to minimize impact. Regularly strengthening the glutes and core also distributes weight more evenly during activity.
Does weight influence patellofemoral pain syndrome?
Excess body weight increases pressure on the kneecap during movement. Even a 10-pound loss can significantly reduce stress. Pairing a balanced diet with strength training helps manage both weight and joint health.