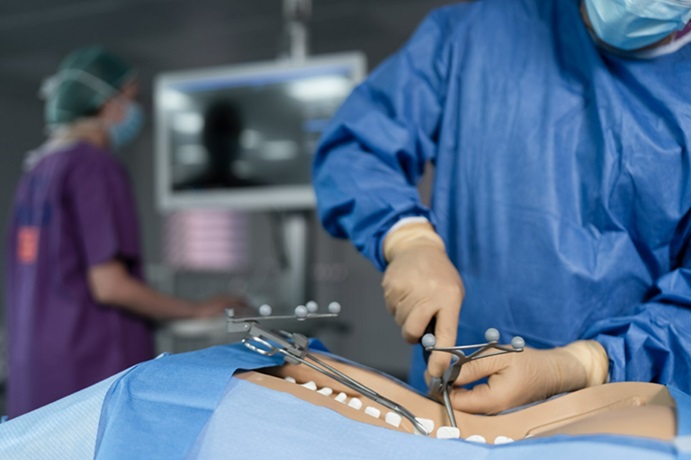
The PathKeeper 3D optical navigation system is used to improve the clinical experience, increase surgical accuracy and eliminate radiation exposure during spine surgery.
KFAR SABA, Israel, Nov. 16, 2023 /PRNewswire/ — PathKeeper Surgical, a privately held, Israel-based medical technology company, is committed to improving the health of people around the world suffering from all spinal problems requiring surgery. As PathKeeper Surgical celebrates the first use of the PathKeeper 3D optical navigation system during spinal fusion surgery at Southcoast Health’s St. Luke’s Hospital in New Bedford, Massachusetts, PathKeeper Surgical is committed to making navigation-guided surgery available to every patient in all operating rooms.
The PathKeeper system was used to create a comprehensive surgical plan and accurately navigate the single-level lumbar degenerative spinal fusion surgery at Southcoast Health’s St. Luke’s Hospital.
“The PathKeeper system addresses many of the complexities of spine surgery and adapts to the patient’s individual needs with a high degree of accuracy and without radiation during a critical part of the surgical procedure,” said Matthew Philips, MD, chief of Brain & Spine Services, Southcoast Health Neurosurgery, Dartmouth, MA. “We have already experienced the clinical benefits of integrating the PathKeeper system into our spinal fusion surgeries at St. Luke’s Hospital.”
The PathKeeper system is designed to replace traditional navigation technology with a 3D optical navigation system that provides comprehensive surgical planning; active, independent submillimeter registration and tracking of patient anatomy and surgical instruments; establish precise accuracy of device implantation; more efficient surgical workflow; elimination of radiation exposure during the surgical procedure; and a more affordable price point so that both hospital operating rooms and ambulatory surgical center operating rooms can integrate this new technology.
“We are very pleased with the adoption of the PathKeeper system at Southcoast Health, which continues our expansion of the PathKeeper system to hospitals and surgery centers across the United States,” said Ryan LeBlanc, Chief Commercial Officer of PathKeeper Surgical. “The PathKeeper system is a game changer in driving improved clinical outcomes and economic value for patients and healthcare providers.”
PathKeeper Surgical received FDA 510k clearance for the PathKeeper System earlier this year. The name PathKeeper effectively describes the essence of the system: a 3D optical navigation system that ‘keeps’ the surgical ‘path’ on course throughout the operation.
About PathKeeper Surgical
PathKeeper Surgical is an Israel-based medical technology company that has developed a solution to combat the high failure rates in spine surgery. PathKeeper was founded in 2018 by Erez Lampert, a top expert in medical 3D imaging with more than 20 years of experience in the healthcare and aerospace industries, and a proven track record in 3D imaging. Erez previously served as R&D leader for the Itero Element Intraoral Scanner for Align Technology (Invisalign), the world’s leading 3D dental scanner. Josh Schroeder, MD, director of Spinal Deformities at Hadassah Medical Center and an HSS fellow, has been on board as a clinical advisor since the company’s founding. Erez and Josh’s combined knowledge enabled the company to develop an innovative navigation system that outperforms existing solutions. More information can be found at path-keeper.com.
About Southcoast Health
For more than 25 years, Southcoast Health has served communities in southeastern Massachusetts and Rhode Island as the region’s largest provider of primary and specialty care. The nonprofit charity system includes three acute care hospitals – Charlton Memorial in Fall River, St. Luke’s in New Bedford (a Level II Trauma Center) and Tobey in Wareham – as well as a network of more than 700 physicians, hospitalists and mid-level practitioners.
Southcoast Health has established six urgent care centers, two cancer centers, a Visiting Nurse Association and numerous outpatient facilities that ensure convenient access to services for 725,000 residents in 33 communities covering 900 square miles. Additionally, the system has partnered with Acadia Healthcare to provide expanded resources at Southcoast Behavioral Health in Dartmouth.
Southcoast Health has been consecutively recognized as a Newsweeks World’s Best Hospital of 2019-2023, in addition to being ranked as a High Performing Hospital for Maternity Care during the calendar years 2021-2022 and 2022-2023 by American news and world report.
With more than 7,500 employees, Southcoast Health is the largest employer in southeastern Massachusetts and one of the largest employers in the Commonwealth, according to the Boston Business Journal. More information is available online at www.southcoast.org.
US Media Contact:
Ryan LeBlanc
head of marketing
ryan.leblanc@path-keeper.com
Photo – https://mma.prnewswire.com/media/2279117/PathKeeper.jpg
SOURCE PathKeeper