Medial tibial stress syndrome is one of the most common athletic injuries, especially among those who participate in high-impact activities. However, there are other risk factors for shin splints, and not all patients who complain of the characteristic pain along the shin are athletes.
MTSS is a condition that often resolves on its own. Physical therapy can help relieve the pain and prevent it from returning.
What causes shin splints?
There are several muscles in the leg that attach to the shin bone, including the anterior and posterior tibialis muscles, the flexor digitorum longus muscle, and the soleus muscle. These muscles and their connective tissue can pull on the periosteum, a layer of tissue that covers the bone and allows the muscles to attach.
Repeated stress can cause the periosteum to become inflamed, resulting in the pain of shin splints. There are several risk factors that can contribute to MTSS.

1. Physical activity
Athletes who do a lot of running and jumping, such as gymnasts, basketball players, dancers, tennis players and sprinters, are at particular risk for shin splints. An estimated 35% of these athletes eventually develop MTSS.
Due to frequent marching and other physically demanding tasks, soldiers are at risk of developing shin splints, with a incidence rate that can be as high as 35%.
2. Weak bones
MTSS may be more likely in people with underlying medical conditions that weaken the bones, such as osteoporosis or osteopenia. Other underlying medical conditions that can affect bone health and increase the risk of shin splints include eating disorders, vitamin D deficiencies, or hormonal changes in women that can also result in a loss of normal menstruation.
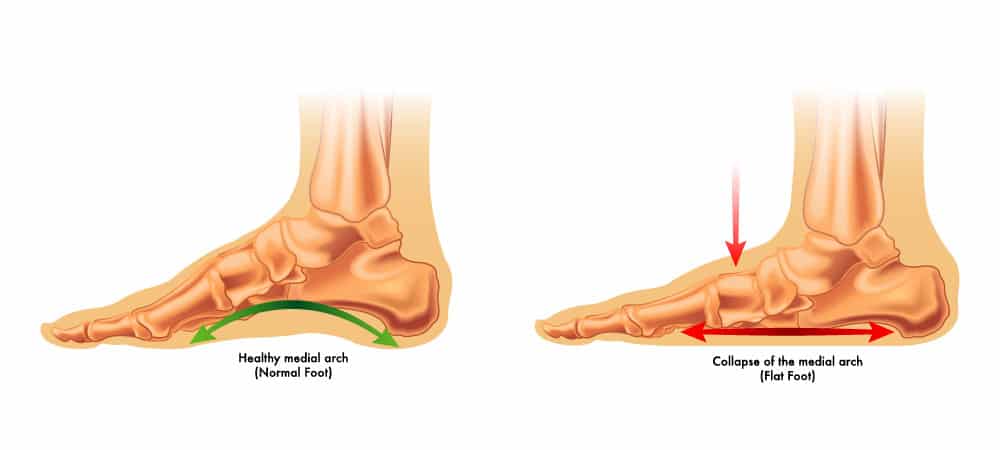
3. Flat feet
Overpronation occurs when the arch of the foot collapses due to the impact of a step. This is colloquially known as having flat feet. If you often walk or run with flat feet, this can strain the tibial periosteum and lead to shin splints. You can also develop MTSS if your arches are stiff or high. Exercising or playing sports in shoes that do not provide adequate arch support can contribute to overpronation and increase the risk of shin splints.
4. Overweight
Carrying extra weight puts more strain on the lower extremities and increases the risk of shin splints. Maintaining a healthy weight is important for shin splint prevention and overall health, but you should begin an exercise program gradually. Demanding too much of the body at once can also contribute to shin splints.
How can shin splints be prevented?
Chances are you will develop MTSS at the start of your athletic season or a new training regimen. In your eagerness to get started, you may try to do too much too quickly, putting too much pressure on your lower legs.
Starting with a gentle exercise program and progressing slowly is therefore important to prevent shin splints. Limiting activity increases to 10% per week helps prevent sudden changes that can trigger MTSS.
If your muscles are not properly warmed up before physical activity, they can put pressure on your shin. Be sure to stretch your entire body, especially your legs, before beginning any exercise or athletic event.
Supportive footwear helps prevent overpronation, so be sure to replace the shoes you use for exercise before they wear out. If you are a runner, replace your running shoes every 300 miles. If your shoes do not provide enough support, you can use arch supports that are specially designed to prevent overpronation.
Try cross-training with low-impact exercises, such as cycling or swimming, to give your lower legs a chance to rest and recover. When participating in high-impact activities, try to avoid uneven, hilly terrain and hard surfaces.
How can physical therapy help treat shin splints?
The prognosis for shin splints is usually very good and most people recover completely. The key is to relieve pressure on the inflamed tissues so they have a chance to heal. There are several physiotherapy techniques that can help relieve stress in the superficial tissues:
- Foam rolling
- Massage
- Tool-assisted therapy
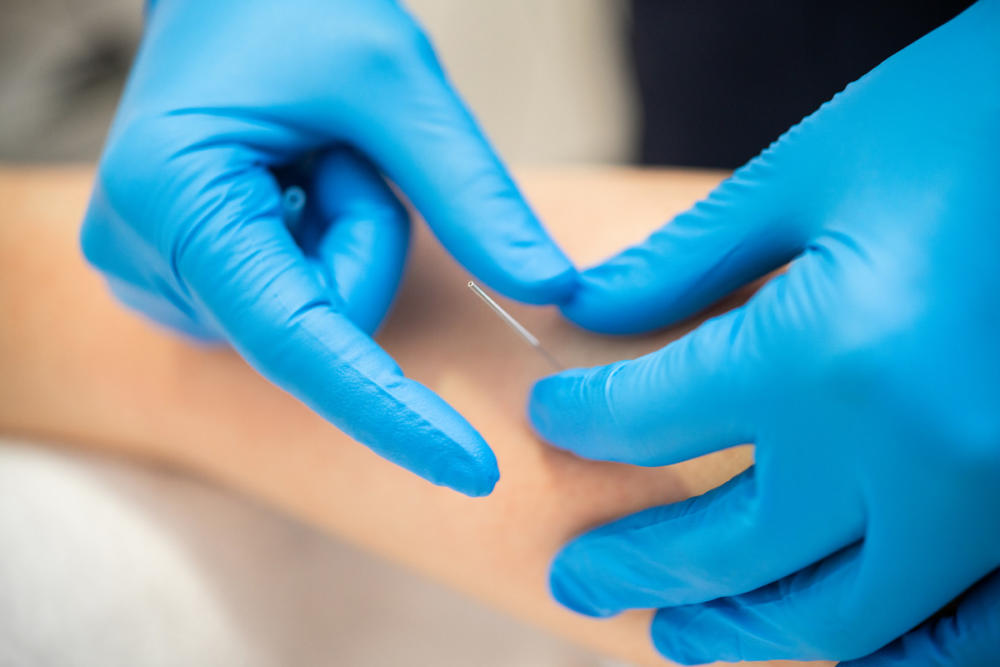
If the tension is in the deeper tissues of the muscle, these techniques may not be enough to relieve it. However, trigger point dry needling is another technique that can reach beyond the superficial tissues to relieve tension in the fibers in the muscle belly. The goal is for the muscle fibers that are better equipped for the task to absorb the stress instead of the periosteum.
In addition to helping relieve the pain of MTSS, physical therapy can also help prevent symptoms from coming back. You can learn exercises to prevent overpronation by strengthening the arch of your foot. Although it may seem counterintuitive at first, strengthening the muscles that control hip movement can help reduce tension in the lower leg.
Your physical therapist may also suggest shoes that provide better support and adjustments to your activities to reduce stress on your lower leg and prevent shin splints from coming back.
As you progress through therapy and eventually return to your previous activities, use pain as a guide and stop when it starts to hurt. Trying to push through the pain of shin splints only makes the problem worse. make an appointment today with a Foothills physical therapist.