Patellofemoral pain syndrome
That dull, aching, throbbing, sometimes sharp pain around the knee or kneecap that comes and goes based on activity may be a condition known as Patellofemoral Pain Syndrome. Sometimes associated with cracking and popping, patellofemoral pain can range from not so bad to disabling discomfort causing people of all ages to avoid activities such as walking, jogging or participating in a sport.
What causes patellofemoral pain?
With patellofemoral pain syndrome, discomfort in or around the front of the knee is often due to irritation of the cartilage that lines the underside of the kneecap in the joint. Stress on the knee can cause the cartilage to become inflamed, which can ultimately lead to thinning and fraying of the tissue over time. In some cases, athletes begin to notice symptoms after years of competition and training, even without immediate injury. In other cases, people only report this pain days, weeks, or months after an increase or change in activity. If the causes of patellofemoral pain syndrome are not treated, they can eventually lead to tissue degeneration in the knee, such as osteoarthritis.
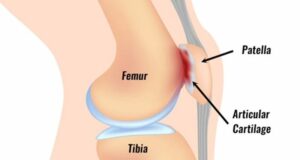
The patella, or kneecap, is a floating bone connected to the femur and shin bone by tendons and ligaments. The bottom, or back part, of the patella is covered with a layer of cartilage, which helps it slide smoothly over the thigh bone when you bend and straighten your knee. There should be sufficient joint space between the patella and the underlying femur, although this joint space sometimes narrows, increasing the chance of contact or friction between the bony surfaces.
A variety of factors including anatomy, soft tissue mobility, biomechanics (movement quality), and physical activity may contribute to a higher risk of patellofemoral syndrome. For example…
- The anatomical resting position of the patella may be slightly higher than normal, also called ‘patella alta’, which can make the patella more sensitive to gradual wear.
- A patella that is hypermobile or has too much mobility can bump and rub against the underlying bone, irritating the cartilage and causing pain. Conversely, a patella that is hypomobile or limited in mobility may become painful due to too much force being placed on a particular part of the patella.
- In terms of movement, the patella moves over the femur, but the femur also moves under the patella. The biomechanics of the entire leg must be addressed to understand what is happening at the knee. The hip and foot play an important role in what the knee experiences. For example, someone with overpronated feet or weakness in the hip muscles may experience knee pain due to altered mechanics and resulting pressure on the cartilage lining of the patella. Abnormal biomechanics can be corrected through exercises prescribed by a physical therapist.
- Physical activity also contributes to patellofemoral pain. The intensity or load of the activity can place more force on the knees than the body can safely tolerate. Activity modification may be necessary to control symptoms. For example, exercises such as running can be avoided for a while to calm symptoms such as swelling and pain.
If the contributing factors are not addressed, the friction and friction between the surfaces can worsen, leading to thinning and fraying of the cartilage, wear and tear of the joint, and ultimately bone-on-bone osteoarthritis.
What is the best treatment for patellofemoral pain syndrome?
The recommended treatment for patellofemoral pain generally focuses on strengthening the muscles of the leg, from the hip and trunk to the foot, along with maintaining or increasing flexibility to reduce stress on the patella. Normalizing strength, flexibility and biomechanics through the limbs will help reduce pressure on specific areas of the cartilage that have become irritated and painful, allowing activity and exercise to be comfortable again.
In addition to strengthening, ice and anti-inflammatory medications, such as ibuprofen, are often recommended to reduce swelling and relieve pain during the acute phase. Reducing painful activities such as climbing stairs can be helpful in recovering from patellofemoral pain syndrome. Although you limit painful exercises, you can still be active by incorporating alternative, non-painful exercises that will strengthen the knee around the knee and reduce irritation to the cartilage and other structures that support the patella. For example, a runner with patellofemoral pain can substitute swimming a few times a week to stay active without aggravating the knee.
Have I waited too long? Is it too late for me?
No matter how long you have been suffering from knee pain, it is never too late to build strength. Focusing on correcting your mechanics during exercise and exercise can help reduce your pain over time. Strengthening the muscles around the knees allows you to move with better control and precision, which also improves performance. Increasing body control provides more stability in the patellofemoral joint, which can take pressure off the patella and reduce the risk of further cartilage breakdown.
Can it be cured?
Patellofemoral pain syndrome is one of the most common causes of knee pain and one of the most common conditions resolved with physical therapy. A supervised exercise program to address the underlying causes is the best treatment strategy to relieve patellofemoral pain.
Our courses at ACL Strong are designed and programmed by physiotherapists to give you complete confidence that the exercises you perform are both safe and effective.
Many of our members experience an unexpected benefit when they enroll in an ACL Strong course… their patellofemoral pain improved because they trained smarter and reduced the strain on their knees.
“I can’t believe I’m skiing without pain for the first time in years!”
“The knee pain I used to have while playing football is no longer there!”
“One of the biggest benefits we have seen in our athletes through ACL Strong is that it helps them resolve old injuries that have been bothering them.”
When you take part in the ACL Strong Snow Course or Classic Course, you will learn how to care for your knees in the long term, so you can be as active or competitive as you want, and for as long as you want.
👉 Start strengthening and training smarter today!










