Pseudogout Knee: Symptoms, Diagnosis, and Treatment for Knee Pain and Knee Hurt
Pseudogout knee can look like other knee problems, but the flare pattern and the underlying crystal cause make it a distinct type of inflammatory knee pain and knee hurt. In 2026, we are also seeing more attention to better ways of tracking CPPD (the condition behind pseudogout) because many people live with recurrent episodes they do not recognize early.
Key Takeaways
| What to know | Why it matters for your knee |
|---|---|
| Pseudogout knee is driven by CPPD crystal deposits | It can cause sudden inflammation, often mistaken for infection or gout. |
| Diagnosis often requires synovial fluid testing | This helps confirm CPPD and guides safe treatment. |
| Knee hurt and knee pain can mimic meniscus or ligament injury | We encourage readers to compare symptoms and timing, not just location. |
| Metabolic factors may influence knee chondrocalcinosis | Managing underlying risks can support long-term knee health. |
| Exercise and bracing can be part of flare prevention | For knee pain patterns tied to instability or altered mechanics, support may help. |
- Ask early if your knee pain comes on suddenly, becomes very warm, or swells quickly, because pseudogout knee may need timely anti-inflammatory treatment.
- Review common causes of knee pain and how to describe symptoms clearly in our guide to knee pain.
- If your knee pain started after trauma, compare with traumatic knee scenarios to avoid missing a crystal flare that begins near an injury.
- For knee hurt that follows instability, we often discuss support options in relation to injuries like ligament knee injury.
What Is Pseudogout Knee, and Why Does It Cause Knee Pain?
Pseudogout knee is a form of CPPD (calcium pyrophosphate deposition) that affects the knee joint. Instead of uric acid crystals (the classic cause of gout), CPPD involves calcium-based crystals that can irritate the joint lining and trigger inflammation.
When CPPD crystals provoke an inflammatory response, many people notice a rapid shift from baseline knee discomfort to acute knee pain and marked knee hurt. Swelling, warmth, and limited range of motion are common during a flare, and some episodes can feel intense.
In 2026, patient education increasingly emphasizes that crystal-driven knee pain is not “just osteoarthritis.” If your knee pain has a flare pattern (sudden onset, then partial settling), it is worth discussing pseudogout knee specifically with a clinician, especially if imaging shows joint calcifications.
Common Symptoms of a Pseudogout Knee Flare
Pseudogout knee flares vary, but there are recurring patterns that help distinguish them from gradual wear-and-tear. When inflammation spikes, your knee may feel more than “tender,” it may feel hot, swollen, and functionally restricted.
- Sudden knee pain that can intensify over hours
- Knee hurt that makes walking, stairs, or standing difficult
- Swelling around the joint
- Warmth and sometimes redness over the knee
- Reduced range of motion because of pain and swelling
Because these symptoms can overlap with infection, we strongly recommend prompt medical evaluation when a flare is severe. This is especially important if you have fever, rapidly worsening swelling, or feel generally unwell.
How Pseudogout Knee Is Diagnosed (and How It Differs From Injury)
People often assume knee pain is from damage like a torn meniscus or a ligament injury. Those causes can absolutely happen, but pseudogout knee has its own confirmation pathway, and accurate diagnosis matters for safe treatment.
In clinical practice, diagnosis frequently combines history, physical exam, imaging, and sometimes joint fluid testing. Joint aspiration (sampling synovial fluid) helps identify CPPD crystals and also helps rule out infection in cases that could look similar.
To help you compare possibilities, below is a practical way we describe “timing” and “mechanism” when evaluating knee pain:
| Pattern you notice | What it may suggest |
|---|---|
| Sudden, intense flare with warmth and swelling | Pseudogout knee flare or other inflammatory process |
| Pain after twisting or a feeling of locking | Possible meniscus involvement, see torn meniscus |
| Pain after a direct blow or instability | Possible trauma patterns, see traumatic knee |
| Pain linked to weakness, giving way, or abnormal tracking | Possible ligament or patellofemoral issues, see chondromalacia patella knees |
Even if you suspect an injury, it is still reasonable to ask whether pseudogout knee could be part of the picture, especially if you have a prior history of crystal flares or imaging evidence of calcifications.
Treatment Options for Pseudogout Knee in 2026
Treatment for pseudogout knee aims to reduce acute inflammation during a flare and prevent future episodes when possible. In 2026, clinicians continue refining patient education around safe medication use, dosing, and the importance of ruling out infection before aggressive anti-inflammatory strategies.
Common treatment categories include:
- Anti-inflammatory medicines to calm the flare (as determined by your medical history)
- Joint aspiration in selected cases, which can reduce pressure and improve comfort
- Targeted long-term strategies when flares recur, based on clinician assessment
- Supportive care like rest during the worst of the flare, then gradual return to movement
Because knee pain can overlap with other conditions, we advise readers not to self-diagnose based on symptoms alone. If your knee pain is severe, rapidly worsening, or you have fever, get urgent evaluation.
Practical tip: When you go in for evaluation, bring a simple flare timeline (when symptoms started, how fast they worsened, and what helped). Clear timing often improves the quality of the knee pain conversation.
When Knee Hurt Might Be Something Else: Overlap With Injury and Other Knee Conditions
Knee hurt often leads people to focus on structural injury. However, pseudogout knee can coexist with degenerative changes, and it can also be confused with injuries such as ligament sprains or meniscus tears.
Here are common “overlap” situations we see in knee pain discussions:
- After ACL-related instability or surgery: swelling and pain can be mistaken for mechanical issues. If you want a framework for injury-focused thinking, see anterior cruciate ligament (ACL) injury knee brace.
- After PCL-related injury: persistent discomfort after trauma can be confused with inflammatory flares. See posterior cruciate ligament (PCL) knee injury.
- With patellofemoral pain patterns: kneecap tracking problems can create chronic knee pain, which may mask or complicate flare symptoms. See chondromalacia patella knees.
- With a history of torn meniscus: locking or catching can be injury-driven, but swelling episodes may still have multiple contributors. See torn meniscus.
We do not use this to “dismiss” injury. Instead, we encourage a combined perspective, because treatment differs when the main driver is CPPD inflammation versus structural damage.
Prevention and Self-Management for Knee Pain and Knee Hurt
There is no single prevention method that guarantees you will never experience pseudogout knee flares, but self-management can reduce the burden of knee pain and help you respond faster when symptoms begin.
In 2026, many care plans place emphasis on two goals: (1) earlier flare recognition and (2) smarter joint protection between flares. We recommend:
- Track flare triggers: notice what preceded knee pain episodes (illness, dehydration, dietary changes, or major activity spikes).
- Keep movement consistent: during calm periods, gentle range-of-motion and strengthening can support joint function.
- Use supportive measures if swelling and tenderness affect walking or stairs. This is especially relevant for people whose knee pain flares on top of prior injury mechanics.
- Work on overall risk factors: metabolic health and glycemic control can matter for knee chondrocalcinosis risk, according to community cohort findings.
When you are building a self-management approach, it helps to start with a broader knee pain plan. We often send readers to understanding, managing, and overcoming knee pain so the pseudogout knee flare strategy fits into a full, realistic routine.
This matters because it explains why two people with similar pseudogout knee symptoms can have different experiences tracking response to care. We encourage you to measure what you can reliably feel, like knee pain intensity, walking tolerance, and flare frequency.
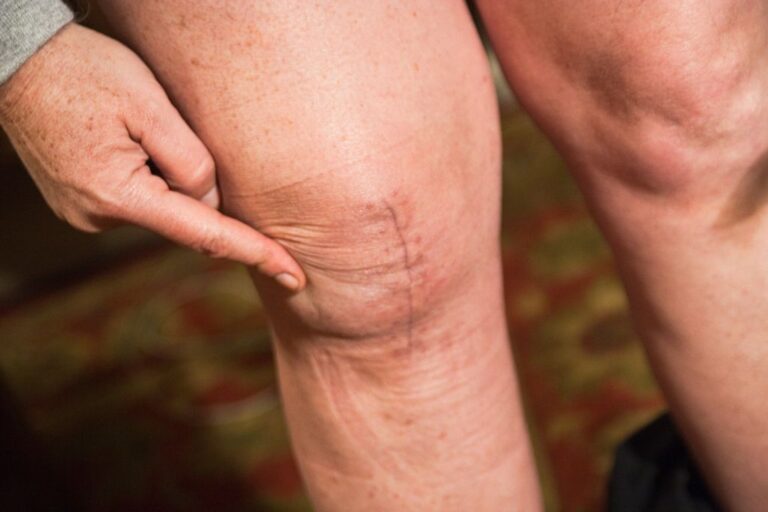
Illustrations: What Knee Problems Can Look Like Before Diagnosis
Because pseudogout knee can resemble other knee issues, images and explanations help readers understand why a “best guess” is not enough. Below, we include visuals to support common knee pain discussions and help you recognize what clinicians often describe during exams.
If your knee hurt feels “inflammatory” (hot, swollen, and sudden), that is one reason we urge early clinical assessment rather than waiting out symptoms.
These visuals should not replace medical evaluation, but they can help you describe knee pain in a way that supports faster, safer decision-making.
Pseudogout Knee and Long-Term Joint Health: What to Expect Over Time
Some people experience pseudogout knee flares that recur, while others have fewer episodes. Long-term joint health often depends on how quickly flares are treated, whether underlying risk factors are addressed, and how well joint function is supported between episodes.
In 2026, many clinicians and physical therapists also work on practical joint strategies, such as pacing activity, strengthening supporting muscles, and addressing movement patterns that increase knee pain. Even when the cause is CPPD inflammation, the knee still needs mechanical support to tolerate daily life.
If you have persistent knee pain outside of flare periods, that can indicate additional processes in the knee. That is one reason we recommend comparing symptoms and function across time, not only during the worst day of knee hurt.
Conclusion
Pseudogout knee is a crystal-driven cause of knee pain and knee hurt that can flare suddenly, often looking similar to other knee conditions. In 2026, the focus is increasingly on getting the right diagnosis early, choosing flare treatments safely, and building a realistic knee care routine that supports long-term joint health.
If your knee pain is hot, swollen, and rapidly worsening, do not wait. We encourage you to seek evaluation promptly and ask specifically whether pseudogout knee could explain your symptoms.
Frequently Asked Questions
Is pseudogout knee the same as gout?
No. Pseudogout knee is caused by CPPD crystal deposits, while gout is driven by uric acid crystals. Both can cause knee pain and knee hurt that feel sudden, but diagnosis matters for the right treatment plan.
How do doctors confirm pseudogout knee?
Doctors typically use your symptoms, exam findings, imaging, and sometimes synovial fluid testing. Identifying CPPD crystals helps confirm pseudogout knee and also helps rule out other urgent causes of intense knee pain.
What does pseudogout knee pain feel like during a flare?
Pseudogout knee flares often create sharp or intense knee pain, with noticeable swelling and warmth. Many people describe knee hurt that limits walking and daily movement within hours.
Can pseudogout knee cause swelling and warmth without an injury?
Yes. Pseudogout knee can trigger inflammatory episodes even when there was no twist, fall, or direct blow. That is why sudden knee pain with swelling and warmth should be medically assessed.
What should I do in 2026 if my knee pain keeps coming back?
If your knee pain keeps flaring, we recommend tracking flare timing, triggers, and what helps, then discussing pseudogout knee with a clinician. Because outcome-measurement tools for CPPD can be inconsistent, your own symptom tracking is especially useful in 2026.
Is pseudogout knee linked to chondrocalcinosis?
Often, yes. CPPD-related crystal deposition can be associated with knee chondrocalcinosis, which can contribute to ongoing knee pain patterns. Managing relevant health factors may support longer-term joint outcomes.
When should I seek urgent care for pseudogout knee?
Seek urgent care if your knee is severely swollen and warm, pain is rapidly worsening, or you have fever or feel unwell. These situations require prompt evaluation because other conditions can mimic pseudogout knee and need different treatment.