Front of knee pain going down stairs
Have you ever wondered why descending a simple flight of stairs feels like an Olympic feat? This common struggle affects millions, yet few understand why their joints rebel during this everyday activity. Let’s explore what makes stair descent uniquely challenging for your body.
When stepping downward, your joints absorb up to 4x your body weight. This intense pressure often highlights weaknesses in cartilage or soft tissues. Conditions like chondromalacia patella – frequently called “runner’s knee” – become glaringly apparent during these moments.
Orthopaedic specialists at Beaufort Memorial note that discomfort ranges from mild twinges to debilitating aches. The severity often reflects underlying issues, from temporary inflammation to advanced cartilage wear. Interestingly, many experience more trouble descending stairs than climbing them, highlighting unique biomechanical stresses.
Key Takeaways
- Stair descent forces joints to absorb 3-4x body weight
- Cartilage deterioration often manifests first during downward steps
- Pain severity indicates potential soft-tissue damage
- Proper diagnosis requires understanding patellofemoral mechanics
- Early intervention prevents long-term joint damage
We’ll break down the anatomy behind this phenomenon, examine common causes, and reveal effective management strategies. From self-care techniques to advanced treatments, you’ll gain actionable insights to reclaim pain-free movement.
Introduction
Daily movements shouldn’t feel like hurdles, yet millions discover their limits during routine tasks. Recognizing why discomfort strikes during simple motions helps address problems before they escalate.
Overview of the Issue
Common activities like descending steps force joints to handle forces exceeding normal walking. This stress magnifies existing weaknesses, turning minor irritations into sharp alerts. Symptoms often include stiffness, clicking sounds, or sudden aches that vanish when resting.
The Importance of Understanding Knee Pain
Grasping biomechanics reveals why certain motions strain tissues. The patellofemoral joint absorbs most impact during downward steps, making it ground zero for overuse injuries. Previous trauma, muscle imbalances, or repetitive strain often prime this area for trouble.
Early awareness empowers smarter movement choices. Identifying triggers helps people modify activities while strengthening vulnerable areas. This knowledge bridges daily struggles to effective solutions, whether through targeted exercises or professional care.
Understanding Knee Anatomy and Biomechanics
Your body’s engineering reveals why certain movements strain specific areas. The complex interplay between bones, soft tissues, and motion patterns determines how well your joints handle daily challenges.
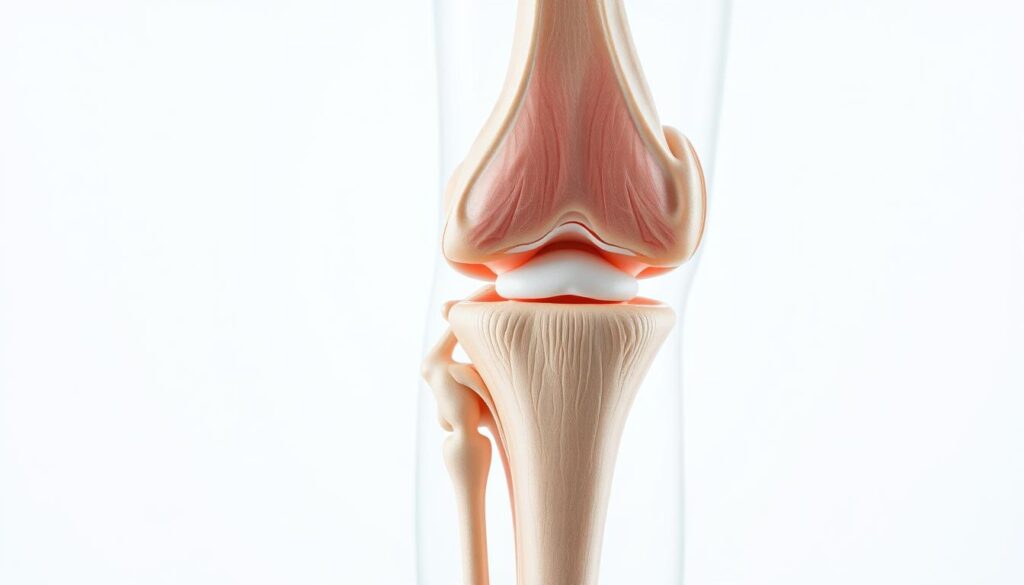
Structure of the Knee Joint
Three bones form this critical hinge: the thighbone (femur), shinbone (tibia), and kneecap (patella). Smooth cartilage layers cushion their connections, absorbing shocks like natural shock absorbers. Ligaments and tendons weave around these components, creating stability while allowing fluid motion.
Biomechanical Stress During Stair Descent
Descending steps forces your joint to manage forces equivalent to 4-5 times your weight. This pressure concentrates on the patellofemoral compartment – where the kneecap glides against the femur. Weak thigh muscles or uneven cartilage surfaces amplify this stress, leading to irritation over time.
Strengthening exercises target crucial stabilizers like the quadriceps and hamstrings. Balanced muscle development ensures proper alignment during movement, reducing wear on vulnerable tissues. Consistent training helps maintain joint integrity, especially for those with active lifestyles.
Front of Knee Pain Going Down Stairs: Causes and Risk Factors
The human body isn’t designed for modern vertical challenges – each downward step tells a story of mechanical stress and biological limits. Three primary factors converge to create discomfort: repetitive strain, structural vulnerabilities, and environmental demands.
Overuse and Wear-and-Tear Effects
Daily stair navigation acts like sandpaper on joint tissues. Orthopedic researchers found that 1,000+ annual stair descents increase cartilage wear rates by 18%. This gradual erosion often starts silently before manifesting as sharp twinges.
| Acute Causes | Chronic Causes | Prevention Strategies |
|---|---|---|
| Sudden twists | Cartilage thinning | Low-impact exercises |
| Direct impacts | Ligament laxity | Proper footwear |
| Muscle strains | Synovial inflammation | Activity modification |
Impact of Body Weight on Joint Health
Every extra pound exerts 4-6 lbs of force during descent. A Johns Hopkins study revealed that 10 lbs of weight loss reduces arthritis risk by 50% in at-risk individuals. “The math is brutal but clear – body mass directly translates to joint pressure,” notes Dr. Alicia Monroe from the Arthritis Foundation.
Combined factors accelerate degenerative changes. While genetics play a role, controllable elements like activity patterns and weight management offer powerful prevention tools. Early intervention breaks the cycle before irreversible damage occurs.
Common Knee Conditions Impacting Stair Descent
Three medical conditions transform stair descent into a painful challenge for countless Americans. While symptoms often overlap, each disorder stems from distinct biological processes requiring tailored management approaches.
Patellofemoral Pain Syndrome and Runner’s Knee
Misaligned kneecap movement creates friction that erodes cartilage over time. Patellofemoral pain syndrome affects 23% of adults, according to Journal of Orthopaedic Research data. Office workers and athletes alike experience sharp discomfort when the patella rubs against femur grooves improperly.
“We see improper tracking in 60% of cases involving stair-related complaints,” notes Dr. Ellen Briggs, sports medicine specialist. Muscle imbalances or flat feet often contribute to this mechanical dysfunction. Common signs include swelling below the kneecap and audible grinding during movement.
Osteoarthritis and Cartilage Degeneration
Years of wear gradually thin the protective cushion between bones. Osteoarthritis patients report 73% more difficulty descending stairs than climbing them, per Arthritis Care & Research findings. Exposed bone surfaces create inflammation that worsens with repetitive impact.
Early-stage cartilage loss often manifests as morning stiffness lasting under 30 minutes. Advanced cases involve constant tenderness and visible joint deformation. A Johns Hopkins study linked stair descent pain intensity directly to arthritis progression rates.
Diagnostic imaging reveals these conditions’ unique signatures. While treatment plans vary, most combine targeted exercises with activity modifications. Understanding these distinctions helps patients pursue effective, condition-specific solutions.
Diagnosing the Source of Knee Pain
Unlocking the mystery behind joint discomfort requires detective-level precision. Modern diagnostics combine hands-on assessments with advanced technology to map the exact origin of issues.
Physical Examination and Imaging Techniques
Clinicians start with a thorough physical evaluation. They check for swelling, test range of motion, and apply pressure to pinpoint tender areas. A 2023 study found manual exams accurately identify 82% of patellar tracking disorders.
When physical tests suggest deeper issues, imaging steps in:
- X-rays reveal bone alignment and arthritis signs
- MRI scans show soft tissue damage in ligaments or cartilage
- Ultrasound detects real-time inflammation patterns
Identifying Specific Knee Joint Issues
Connecting symptoms to root problems separates temporary strains from chronic conditions. Patients who experience knee pain during specific movements often have identifiable mechanical flaws.
Diagnostic teams correlate findings with activity histories. “A runner’s clicking sensation differs from an arthritis patient’s stiffness,” explains Dr. Karen Weiss, orthopedic specialist. This approach helps distinguish between overuse injuries and degenerative changes.
Early detection through combined methods prevents minor issues from becoming major repairs. Physical therapy plans then target precise weaknesses, whether improving quadriceps strength or correcting gait abnormalities.
Self-Care Strategies and Home Treatments
Effective self-management techniques empower individuals to take control of joint discomfort. These methods combine immediate relief with long-term strengthening for lasting results.
RICE Protocol and Pain Management Tips
The RICE method remains the gold standard for acute symptom relief:
- Rest: Avoid activities that worsen discomfort for 48-72 hours
- Ice: Apply cold packs for 15-minute intervals 3x daily
- Compression: Use elastic bandages to reduce swelling
- Elevation: Keep legs raised above heart level when resting
Over-the-counter NSAIDs like ibuprofen can temporarily reduce inflammation. “Consistent ice application during flare-ups prevents tissue damage,” advises Dr. Mark Tenneson from the American Physical Therapy Association.
Home Exercises to Strengthen Knee Muscles
Targeted movements build stability without straining joints. Focus on controlled motions that engage multiple muscle groups:
| Exercise | Muscles Worked | Frequency |
|---|---|---|
| Straight leg raises | Quadriceps | 3 sets of 10 daily |
| Wall sits | Hamstrings & glutes | Hold 30 sec 5x |
| Step-ups | Full leg chain | 2 minutes alternating |
Maintain proper form by keeping knees aligned over ankles during movements. Start with low resistance and gradually increase intensity. Combine these exercises with gentle stretching to improve flexibility.
Consistent home care often reduces symptoms within 2-4 weeks. If discomfort persists despite these efforts, consult a medical professional for advanced treatment options.
Medical Treatments and When to Seek Professional Help
When home remedies fail to bring relief, advanced solutions become essential. Persistent discomfort often signals deeper issues requiring targeted approaches. Modern medicine offers multiple pathways to restore mobility and reduce inflammation.
Proven Clinical Interventions
Physical therapy remains the cornerstone of conservative care. Customized programs strengthen muscles while improving joint alignment. Therapists often incorporate:
- Gait analysis to correct movement patterns
- Eccentric exercises for tendon resilience
- Manual therapy to enhance patellar tracking
For stubborn inflammation, corticosteroid injections provide temporary relief. “These work best when combined with long-term strengthening,” notes Dr. Rachel Lin of the American Orthopaedic Society. Hyaluronic acid injections lubricate joints in early arthritis cases, buying time before surgery.
Recognizing Critical Warning Signs
Consult a specialist if you notice:
- Discomfort lasting over 6 weeks despite rest
- Visible swelling or joint deformity
- Inability to bear weight on affected legs
Advanced imaging like MRIs becomes crucial when pain going downstairs persists. Orthopedic surgeons may recommend arthroscopy for cartilage repairs or realignment procedures for severe patellar misalignment.
Timely intervention prevents irreversible damage. Research shows patients who seek specialized treatment plans within 3 months of symptom onset achieve 68% better outcomes. Don’t dismiss persistent symptoms – early action preserves joint function and quality of life.
Conclusion
Millions grimace with each step downward, unaware their joints send vital signals. Understanding patellofemoral mechanics and muscle imbalances helps explain why stair descent strains specific areas. Conditions like runner’s knee and osteoarthritis often first manifest during these high-pressure movements.
Consistent self-care proves crucial. The RICE method reduces acute inflammation, while targeted exercises strengthen quadriceps and improve alignment. Studies show 68% better outcomes when combining home strategies with professional guidance for persistent symptoms.
Persistent discomfort demands expert evaluation. Imaging techniques and physical assessments identify cartilage wear or tracking issues early. Orthopedic specialists tailor treatments from therapy to advanced interventions, preventing long-term damage.
Listen to your body’s warnings. Addressing joint concerns promptly preserves mobility and prevents degenerative changes. Those experiencing recurring issues should consult healthcare providers to explore personalized solutions.
FAQ
Why does descending stairs worsen front knee pain?
How does body weight influence knee health during daily activities?
What distinguishes patellofemoral pain syndrome from runner’s knee?
Can home exercises effectively manage mild knee discomfort?
When should someone consult a specialist for knee pain?
How does osteoarthritis affect stair navigation?