Have you ever wondered why simple movements like climbing stairs or sitting too long suddenly cause discomfort? The answer lies in the delicate balance of our body’s most overworked joint. Your knees handle forces up to four times your body weight during routine activities, making them prone to wear even without intense exercise.
This complex hinge relies on ligaments, tendons, and cartilage working in harmony. When one component falters – whether from sudden twists, repetitive motions, or age-related changes – swelling and stiffness often follow. Over 25% of adults experience joint issues linked to daily habits, according to recent studies.
Our comprehensive guide to knee health reveals how minor adjustments can prevent major problems. From improper footwear to overlooked muscle imbalances, we’ll explore hidden culprits that turn ordinary actions into sources of lasting damage.
Key Takeaways
- The knee’s weight-bearing role makes it vulnerable to strain during daily tasks
- Cartilage wear and ligament tears account for most mobility complaints
- Swelling often signals underlying joint stress needing attention
- Early identification of triggers prevents chronic conditions
- Proper alignment during movement reduces injury risks
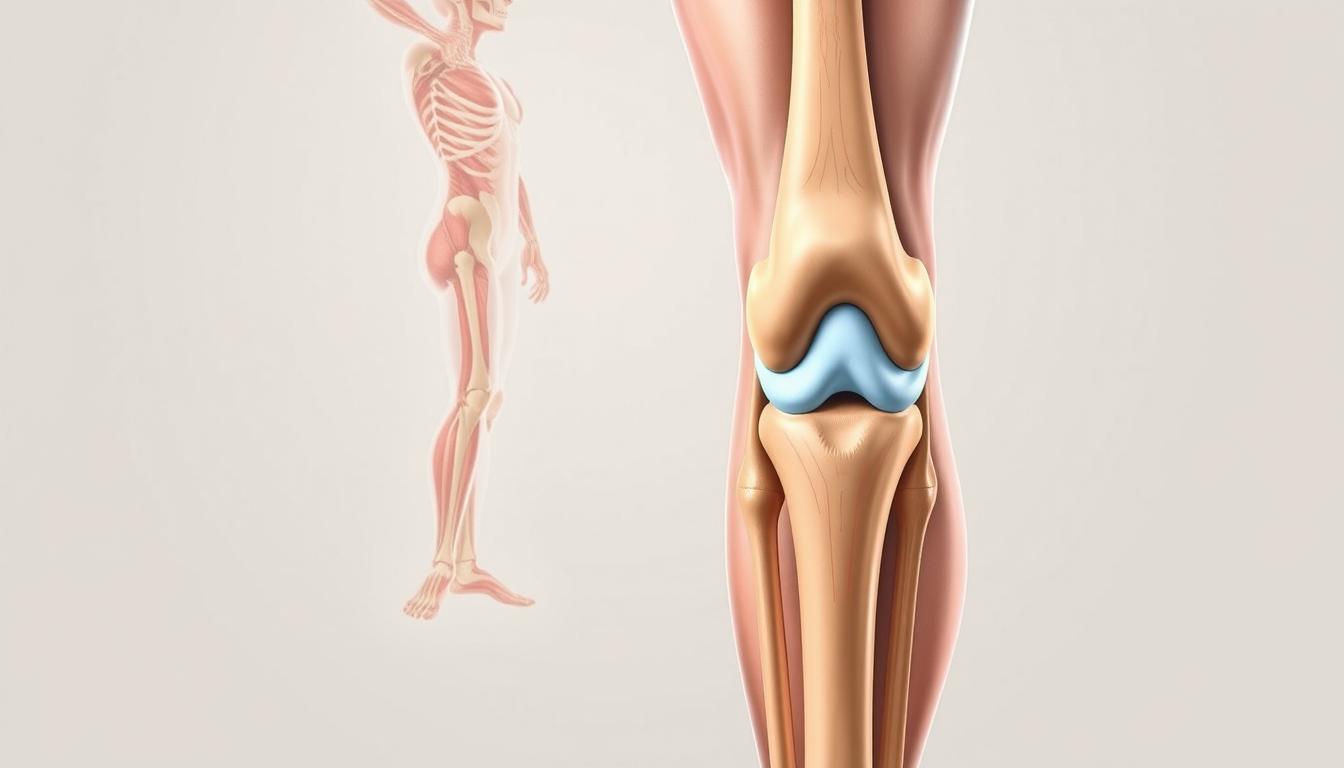
Understanding Knee Anatomy and Mechanics
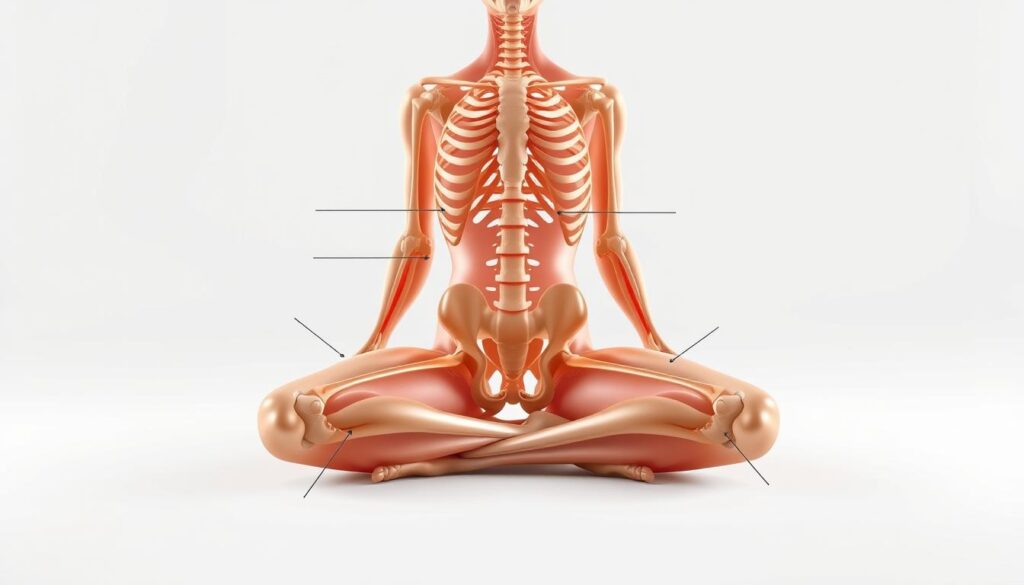
Every step we take relies on a complex system of bones and tissues working in precise harmony. The joint connecting thigh and shin bones functions like a living hinge, combining stability with remarkable flexibility.
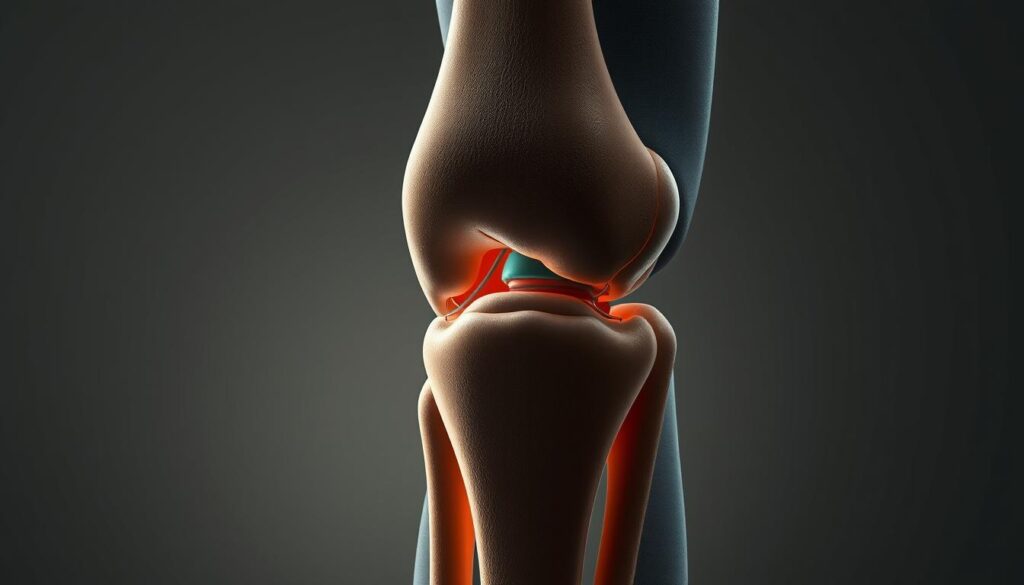
Building Blocks of Mobility
Three bones form this critical junction: femur, tibia, and patella. Between them lies cartilage – nature’s shock absorber preventing bone-on-bone contact. Ligaments act as sturdy ropes, connecting bones while allowing controlled movement.
Four primary bands maintain stability:
- ACL and PCL control forward/backward motion
- MCL and LCL prevent side-to-side slipping
Motion Creates Wear Patterns
Synovial fluid lubricates the joint during activity, much like oil in machinery. Repeated bending or twisting can thin this protective layer. When ligament fibers stretch beyond limits or cartilage develops uneven wear, grinding sensations often follow.
Research shows 30% of adults over 45 show early signs of arthritis in weight-bearing joints. Regular movement maintains circulation to these tissues, while excessive strain accelerates breakdown. Finding this balance proves crucial for long-term joint function.
What are Specific Knee Pain Triggers?
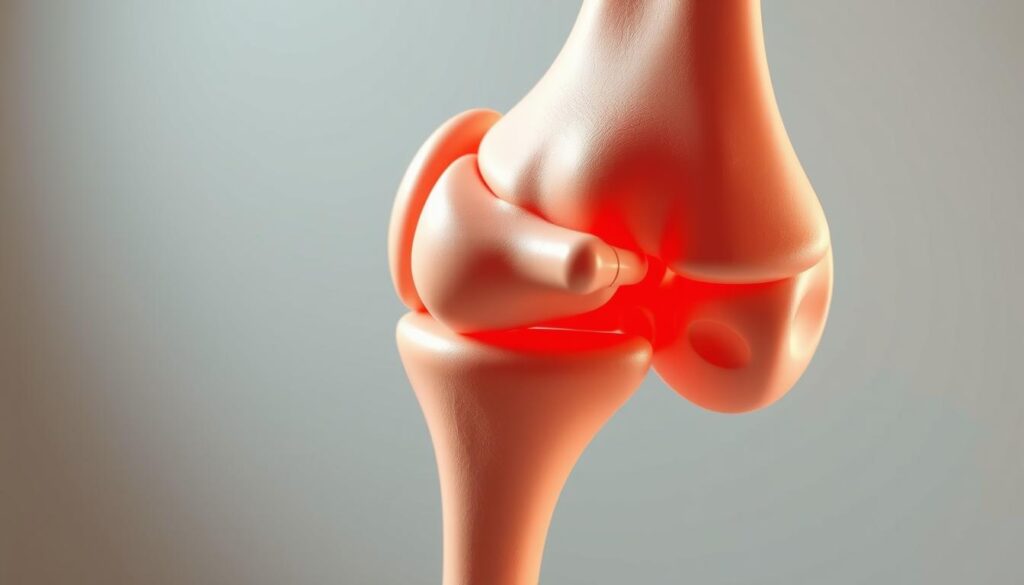
Why does bending down sometimes feel like a challenge? The answer often lies in hidden conditions that transform routine motions into sources of discomfort. Our joints communicate through swelling and stiffness when facing stressors – signals we shouldn’t ignore.
Hidden Culprits Behind Joint Stress
Repetitive motions like squatting or climbing stairs can gradually wear down tissues, creating micro-tears that accumulate over time. Rheumatoid arthritis exemplifies how autoimmune responses turn the body’s defenses against itself, attacking healthy joint linings. This leads to persistent swelling and reduced mobility.
Another common offender? Band syndrome, where connective tissues tighten abnormally during movement. Think of it like a guitar string pulled too taut – every motion creates friction. Combined with poor posture, this imbalance often cause knee strain during activities as simple as walking.
Persistent inflammation acts as the body’s flare gun, signaling underlying trouble. Whether from sudden injuries or chronic conditions, swollen joints demand attention before damage becomes irreversible. Recognizing these red flags early helps prevent long-term limitations.
Next, we’ll explore how acute injuries differ from gradual wear – and why your approach to care should too.
Common Causes: Injury, Overuse, and Disease
What transforms a minor ache into persistent joint trouble? Three primary factors – sudden damage, repetitive strain, and systemic illnesses – account for most mobility challenges. Let’s examine how these forces interact within our bodies.

When Trauma Meets Time
Acute damage often stems from impacts or twists. A soccer player’s ACL tear or a slip-related kneecap fracture demonstrates immediate trauma. These injuries typically cause sharp discomfort and visible swelling within hours.
Degenerative conditions operate differently. Years of wear thin cartilage, while autoimmune diseases like rheumatoid arthritis attack joint linings. “The difference between a sprain and arthritis? One shouts, the other whispers,” notes Dr. Ellen Torres, orthopedic specialist.
| Cause | Onset | Symptoms | Treatment Window |
|---|---|---|---|
| ACL tear | Sudden | Instability, swelling | Days |
| Osteoarthritis | Gradual | Morning stiffness | Months |
| Tendonitis | Progressive | Localized tenderness | Weeks |
Silent Aggravators
Connective tissues bear the brunt of overuse. Patellar tendonitis – often called “jumper’s knee” – develops when muscle imbalances strain the kneecap’s anchoring tendons. Similarly, iliotibial band syndrome plagues runners through repetitive friction.
Watch for these red flags:
- Persistent swelling after activity
- Clicking sounds during movement
- Difficulty bearing weight
Early intervention prevents 68% of chronic cases, according to Johns Hopkins research. Whether addressing a fresh injury or managing arthritis, timely care preserves mobility better than delayed reactions.
Impact of Age, Weight, and Activity Levels on Knee Health
Our bodies keep score in ways we often overlook. Years of movement patterns and physical demands leave lasting marks on joint structures. The relationship between lifestyle choices and joint durability becomes clearer as decades pass.
Time’s Toll on Joint Integrity
Cartilage loses elasticity with age – think of tire treads wearing thin. The meniscus, a crucial shock absorber between thigh and shin bones, develops frayed edges over time. This natural breakdown reduces the joint’s ability to handle impacts smoothly.
Research shows osteoarthritis affects 1 in 3 adults over 60. Synovial fluid production slows, leaving joints less lubricated during motion. These changes explain why morning stiffness becomes common as we accumulate birthdays.
Weight’s Multiplier Effect
Carrying extra pounds multiplies pressure on weight-bearing joints. Every 10 lbs of body weight adds 30-40 lbs of force during walking. For those with obesity, this strain accelerates meniscus degeneration and bones reshaping.
A 2024 analysis revealed maintaining ideal weight reduces arthritis risk by 52%. Simple swaps – taking stairs instead of elevators or choosing water over sugary drinks – create lasting protective effects.
While time remains unstoppable, proactive care preserves mobility. Low-impact exercises strengthen supporting muscles without stressing vulnerable tissues. Understanding these connections helps us make choices that honor our body’s changing needs through the years.
Managing Knee Pain with Home Remedies and Medical Treatments
When joint discomfort strikes, smart responses can prevent temporary issues from becoming chronic. Over 40% of mobility problems improve significantly with early intervention, according to Johns Hopkins rehabilitation data. Let’s explore practical strategies that address both immediate relief and long-term healing.
Effective self-care: Rest, ice, compression, and elevation
The RICE method remains gold-standard care for acute flare-ups. Rest prevents further tissue strain, while ice applied for 15-minute intervals reduces swelling. Compression sleeves stabilize vulnerable areas, and elevation drains excess fluid from inflamed joints.
For chronic bursitis, heat therapy often works better than ice. Warm compresses increase blood flow to stiff tissues. A 2023 Arthritis Foundation study found alternating heat and ice improved mobility in 72% of participants with persistent syndrome-related stiffness.
Consider these red flags requiring professional evaluation:
- Difficulty bearing weight for over 48 hours
- Visible deformity around joints
- Fever accompanying swelling
Alignment issues in the hip or pelvis frequently manifest as knee strain. Physical therapists often assess adjacent joints when treating persistent problems. “You can’t fix a door hinge without checking the frame,” explains Dr. Miriam Cole, sports medicine specialist.
| Care Type | Best For | Timeline |
|---|---|---|
| Home Remedies | Mild swelling, recent injuries | 3-7 days |
| Prescription Treatments | Bursitis, IT band syndrome | 2-6 weeks |
| Surgical Options | Severe cartilage damage | 6+ months |
Remember: Persistent syndrome management requires tailored approaches. What soothes bursitis might aggravate other conditions. Tracking symptom patterns helps identify the right type of care – and when to seek expert guidance for unresolved problems.
Diagnostic Approaches and Imaging Techniques
Unlocking the mystery behind joint discomfort requires detective-level precision. Modern medicine combines hands-on evaluations with advanced technology to map out treatment paths. We start by analyzing movement patterns and tenderness points before reaching for imaging tools.
Connecting Symptoms to Solutions
Physical exams often reveal what scans can’t. Doctors assess how activities like squatting or lunging cause knee pain during movement tests. The Ober maneuver, for example, helps identify iliotibial band tightness by measuring hip abduction range.
“Targeted movements during exams act like live video replays,” explains Dr. Alicia Hernandez, sports medicine specialist. Bursa inflammation becomes evident when pressure applied below the kneecap triggers sharp discomfort. These findings guide which imaging tests deliver the clearest answers.
| Test Type | Best For | Details |
|---|---|---|
| X-ray | Bone alignment | Detects fractures, arthritis |
| MRI | Soft tissue damage | Reveals ligament tears |
| Ultrasound | Bursa evaluation | Checks fluid accumulation |
Imaging confirms suspicions raised during physical assessments. MRIs excel at showing iliotibial band syndrome inflammation near the thigh’s outer edge. Ultrasound dynamically captures irritated bursa sacs during motion – something static scans miss.
When activities consistently cause knee pain, doctors might order gait analysis. This tracks pressure distribution across joints during walking or running. Combining these methods creates a 360-degree view of what’s disrupting mobility – and how to fix it.
Prevention Strategies: Lifestyle Modifications and Exercises
Protecting joint health starts with proactive habits that build resilience. We’ve curated science-backed methods to maintain mobility while reducing strain on vulnerable tissues. These approaches address both immediate risks and long-term durability.
Strengthening and Stretching Routines
Targeted exercises fortify muscles supporting the joint. Wall sits and step-ups strengthen quadriceps without heavy impact. For flexibility, try hamstring stretches with a resistance band – hold for 30 seconds to improve range of motion.
Yoga poses like Warrior II enhance balance while stretching iliotibial bands. “Consistent routines prevent 60% of soft tissue injuries,” notes physical therapist Marco Silva. Pair these with foam rolling to release tension in calf muscles – a common contributor to meniscus tear risks.
Smart Movement Patterns
Adjust daily habits to minimize wear:
- Use ergonomic stools during prolonged sitting
- Wear supportive footwear with arch cushioning
- Avoid sudden pivots during sports
Low-impact activities like swimming maintain fitness without pounding joints. A 2023 Journal of Orthopedic Research study found cyclists experience 40% fewer baker cyst cases than runners. Track activity duration – exceeding 90 minutes of continuous motion often causes knee overuse issues.
Early intervention matters. If pain swelling persists after rest, consult a specialist. Simple tweaks to exercise form and recovery routines can stop minor irritation from becoming chronic damage. Remember: Prevention isn’t about avoiding movement – it’s about moving smarter.
Conclusion
Maintaining healthy knee joints requires understanding their delicate balance. Our bodies rely on these complex hinges to handle forces from walking to twisting. Recognizing how daily motions impact joint structures helps prevent avoidable damage.
Early action proves critical. Tracking swelling patterns or stiffness allows timely interventions before minor irritation escalates. Proper alignment during movement and targeted strengthening exercises reduce strain on vulnerable tissues.
Professional guidance matters when symptoms persist. Physical therapists and orthopedic specialists offer customized solutions for unique needs. Don’t wait until discomfort limits daily activities – proactive care preserves mobility better than delayed treatments.
Ultimately, healthy knee joints depend on informed choices. From footwear selection to activity modifications, small changes create lasting protection. Prioritize joint health today to maintain an active, unrestricted lifestyle tomorrow.
FAQ
What conditions commonly cause swelling and discomfort in the knee joint?
Issues like arthritis, ligament tears, bursitis, or meniscus damage often lead to swelling and pain. Rheumatoid arthritis and osteoarthritis break down cartilage, while injuries like ACL tears or iliotibial band syndrome strain tissues around the joint.
How do acute injuries differ from chronic conditions like osteoarthritis?
Acute injuries—such as ligament sprains or fractures—happen suddenly from trauma or overexertion. Degenerative diseases like osteoarthritis develop slowly, wearing down cartilage over time due to age, repetitive stress, or excess body weight.
Why does aging increase the risk of joint pain?
Over time, cartilage thins, muscles weaken, and ligaments lose flexibility. Reduced shock absorption and joint stability make older adults more prone to inflammation, arthritis flare-ups, or overuse injuries like patellar tendinitis.
Can home remedies effectively manage mild knee discomfort?
Yes. Resting, applying ice packs, using compression sleeves, and elevating the leg reduce swelling. Low-impact exercises and anti-inflammatory medications like ibuprofen also help ease symptoms linked to iliotibial band syndrome or minor strains.
How do doctors diagnose the root cause of persistent knee issues?
Physical exams check for tenderness, range of motion, and instability. Imaging tools like X-rays spot bone spurs or fractures, while MRIs reveal soft tissue damage—meniscus tears, tendon injuries, or Baker’s cysts—to guide treatment plans.
What exercises strengthen muscles around the knees?
Squats, lunges, and leg raises build quadriceps and hamstrings. Stretching the iliotibial band, calves, and hips improves flexibility. Low-impact activities like swimming or cycling also reduce strain on joints while maintaining mobility.
How does excess weight contribute to knee problems?
Extra pounds add pressure on joints during walking or climbing stairs. Over time, this accelerates cartilage breakdown, raising the risk of osteoarthritis. Weight loss of just 10% can significantly lower inflammation and pain levels.